Key Points About Ulcerative Colitis In Children
-
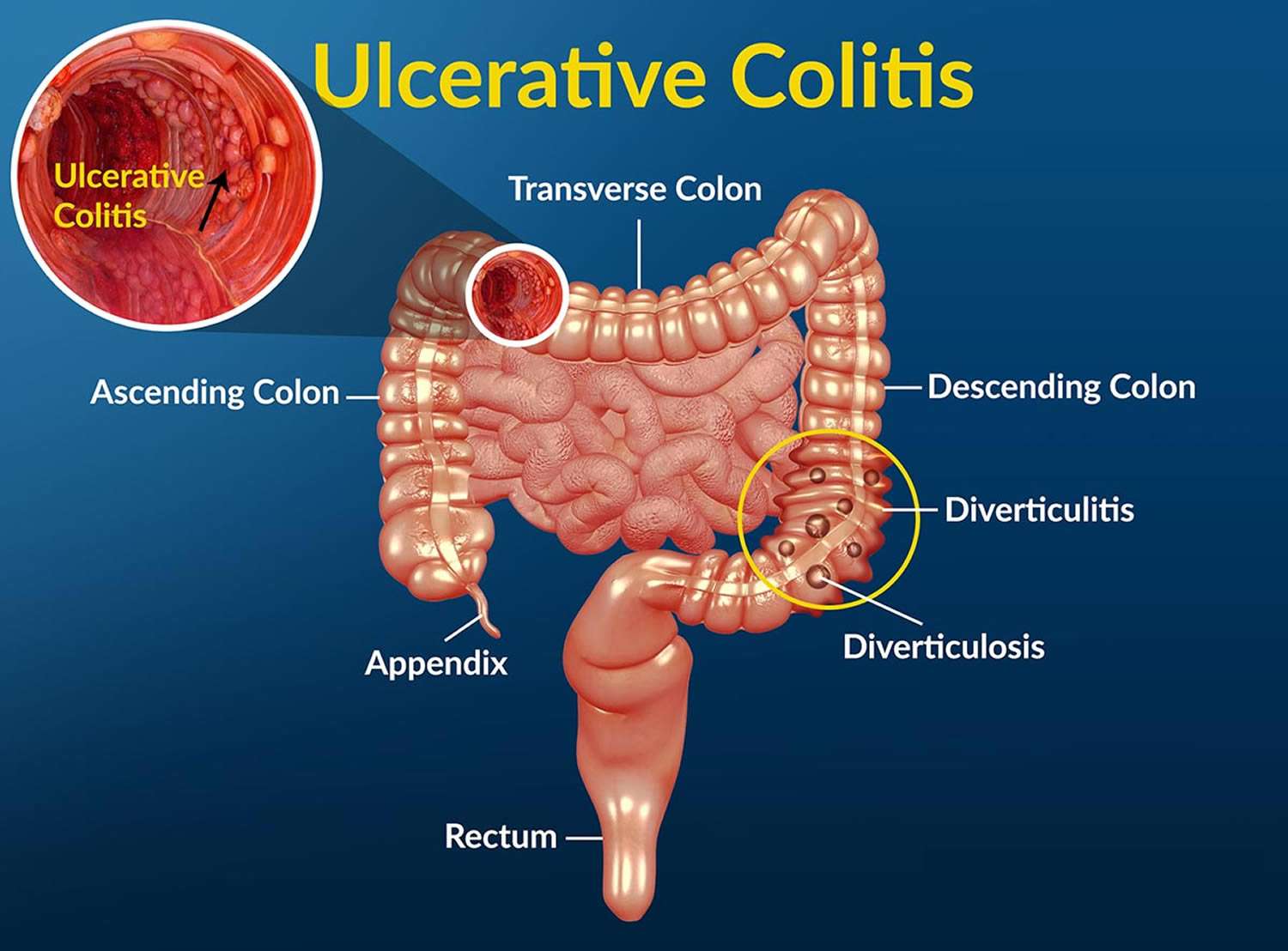
Ulcerative colitis is an inflammatory bowel disease. In this condition, the inner lining of your childs large intestine and rectum gets inflamed.
-
This inflammation causes diarrhea or frequent emptying of the colon. Your child may also have stomach pain and diarrhea.
-
Treatment may include avoiding foods that cause symptoms, taking medicine, and having surgery.
-
Children with this condition need long-term care. Your child may have times when symptoms go away. But symptoms usually come back.
Can I Get Surgery For My Ulcerative Colitis
Surgery is an option if medications arent working or you have complications, such as bleeding or abnormal growths. You might develop precancerous lesions, or growths that can turn into colorectal cancer. A doctor can remove these lesions with surgery or during a colonoscopy.
Research shows that about 30% of people with ulcerative colitis need surgery sometime during their life. About 20% of children with ulcerative colitis will need surgery during their childhood years.
There are two kinds of surgery for ulcerative colitis:
Proctocolectomy and ileoanal pouch
The proctocolectomy and ileoanal pouch is the most common procedure for ulcerative colitis. This procedure typically requires more than one surgery, and there are several ways to do it. First, your surgeon does a proctocolectomy a procedure that removes your colon and rectum. Then the surgeon forms an ileoanal pouch to create a new rectum. While your body and newly made pouch is healing, your surgeon may perform a temporary ileostomy at the same time. This creates an opening in your lower belly. Your small intestines attach to the stoma, which looks like a small piece of pink skin on your belly.
After you heal, waste from your small intestines comes out through the stoma and into an attached bag called an ostomy bag. The small bag lies flat on the outside of your body, below your beltline. Youll need to wear the bag at all times to collect waste. Youll have to change the bag frequently throughout the day.
How Can I Prevent Ulcers
You may be able to prevent ulcers from forming if you:
- Talk to your doctor about alternatives to NSAID medications to relieve pain.
- Discuss protective measures with your doctor, if you cant stop taking an NSAID.
- Opt for the lowest effective dose of NSAID and take it with a meal.
- Quit smoking.
Recommended Reading: Bland Diet Recipes For Ulcers
Don’t Miss: Hand Foot And Mouth Ulcers
Can The Colon Repair Itself
The intestine is the most highly regenerative organ in the human body, regenerating its lining, called the epithelium, every five to seven days. Continual cell renewal allows the epithelium to withstand the constant wear and tear it suffers while breaking down food, absorbing nutrients, and eliminating waste.
Symptoms Of Crohn’s Disease
The most common symptoms of Crohn’s disease are abdominal pain and diarrhea. Other signs of inflammation are often present, including fever and abdominal tenderness. Because symptoms can be worsened by eating, the intake of food is reduced, and this leads to loss of weight, and, less commonly, nutritional deficiencies. Slow, continuous loss of blood into the intestine that may not even be recognizable in the stool can lead to iron deficiency anemia.
Recommended Reading: Symptoms Of A Bleeding Ulcer In Your Stomach
How Are Peptic Ulcers Treated
Treatment will depend on the type of ulcer you have. Your healthcare provider will create a care plan for you based on what is causing your ulcer.
Treatment can include making lifestyle changes, taking medicines, or in some cases having surgery.
Lifestyle changes may include:
- Not eating certain foods. Avoid any foods that make your symptoms worse.
- Quitting smoking. Smoking can keep your ulcer from healing. It is also linked to ulcers coming back after treatment.
- Limiting alcohol and caffeine. They can make your symptoms worse.
- Not using NSAIDs . These include aspirin and ibuprofen.
Medicines to treat ulcers may include:
- Antibiotics. These bacteria-fighting medicines are used to kill the H. pylori bacteria. Often a mix of antibiotics and other medicines is used to cure the ulcer and get rid of the infection.
- H2-blockers . These reduce the amount of acid your stomach makes by blocking the hormone histamine. Histamine helps to make acid.
- Proton pump inhibitors or PPIs. These lower stomach acid levels and protect the lining of your stomach and duodenum.
- Mucosal protective agents. These medicines protect the stomach’s mucus lining from acid damage so that it can heal.
- Antacids. These quickly weaken or neutralize stomach acid to ease your symptoms.
In most cases, medicines can heal ulcers quickly. Once the H. pylori bacteria is removed, most ulcers do not come back.
Dietary And Lifestyle Modifications
Physicians often recommend lifestyle and dietary changes for those with ulcers in addition to medications until the ulcers completely heal. It is best to avoid certain foods and beverages such as chocolate, coffee, alcohol, fatty foods, peppermint, citrus fruits and juices, tomato products, pepper, mustard, and vinegar during healing. Eating smaller meals more frequently may also control symptoms better. Smoking cessation is important, as smoking inhibits ulcer healing. You should also not take NSAIDs, such as aspirin, ibuprofen, or naproxen because they can cause further damage to stomach tissue. Your physician will probably lift any dietary restrictions once your ulcers have healed.
Read Also: How To Ease Mouth Ulcer Pain
What Are Ulcerative Colitis Medications
Since ulcerative colitis cannot be cured by medication, the goals of treatment with medication are to 1) induce remissions, 2) maintain remissions, 3) minimize side effects of treatment, 4) improve the quality of life, and 5) minimize risk of cancer. Treatment of ulcerative colitis with medications is similar, though not always identical, to treatment of Crohn’s disease.
Medications for treating ulcerative colitis include 1) anti-inflammatory agents such as 5-ASA compounds, systemic corticosteroids, topical corticosteroids, and 2) immunomodulators.
Anti-inflammatory medications that decrease intestinal inflammation are analogous to arthritis medications that decrease joint inflammation . The anti-inflammatory medications that are used in the treatment of ulcerative colitis are:
- Topical 5-ASA compounds such as sulfasalazine , olsalazine , and mesalamine that need direct contact with the inflamed tissue in order to be effective.
- Systemic anti-inflammatory medications such as corticosteroids that decrease inflammation throughout the body without direct contact with the inflamed tissue. Systemic corticosteroids have predictable side effects with long term use.
It has long been observed that the risk of ulcerative colitis appears to be higher in nonsmokers and in ex-smokers. In certain circumstances, patients improve when treated with nicotine.
Diet And Nutrition In Crohn’s Disease
MMaintaining good nutrition with Crohn’s disease can be a challenge. Some foods may provoke your symptoms, and others may ease them. But no single meal plan will work for every person with Crohn’s. Weight loss as well as specific vitamin and mineral deficiencies may occur. Patients whose inflammation is still active do not have much of an appetite, so their intake of food is reduced or the types of foods they eat are restricted. Eating can also make symptoms worse, so people with this disease may eat less. Finally, if a substantial portion of the small intestine is inflamed, the inflamed intestine may not absorb nutrients normally. Good nutrition depends on the control of inflammation, but when that is not achievable, it depends on supplemental vitamins, minerals, and calories.
Don’t Miss: Ulcerative Colitis Abdominal Pain Relief
Stomach Ulcer Diagnosis And Conventional Treatment
If you suspect you have a stomach ulcer, see your doctor to first rule out other causes of your pain. In order to diagnose a stomach ulcer, your doctor may perform an endoscopy, which allows the doctor to view the inside lining of the esophagus, stomach and small intestine. Once a diagnosis is verified, treatment options can begin.
Your doctor will likely take your medical history and perform a physical exam along with a blood test, plus ask you about your past use of medications and possibly do an X-ray to locate a stomach ulcer. Testing the blood for H. pylori, plus doing a urea breath test and/or stool test to look for the presence of H. pylori antigens, are common ways to diagnose an ulcer.
The goal of stomach ulcer treatments is to help reduce pain and inflammation in the digestive tract, boost the immune system to fight H. pylori bacteria, prevent complications, and lower the chance for future ulcers from forming or returning.
Today, conventional treatment options for stomach ulcers include:
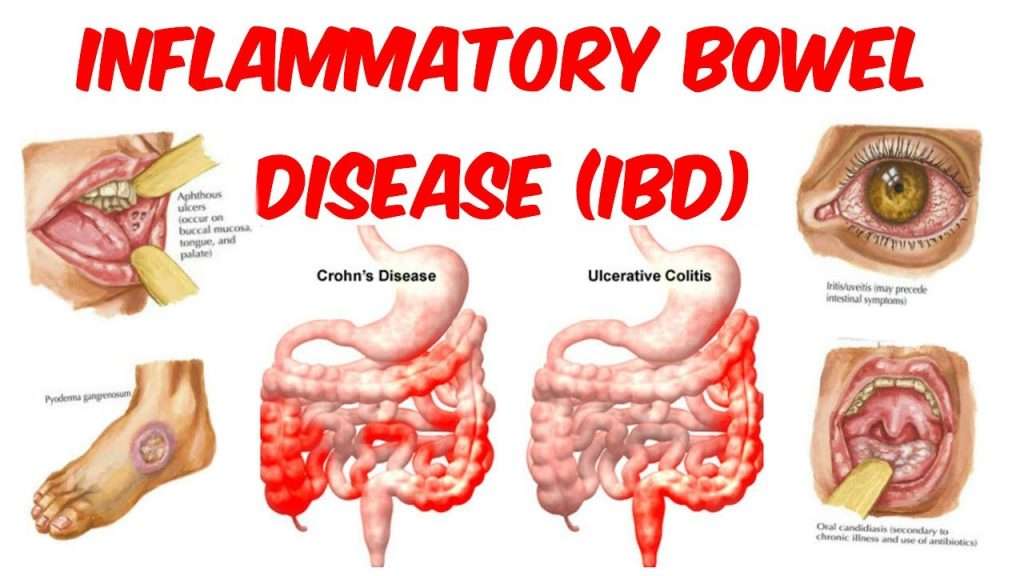
Inflammatory Bowel Disease Treatment
The goal of treatment is to get rid of the inflammation that causes your symptoms. Many types of medicine can help reduce inflammation. Talk to your doctor about anti-inflammatory drugs and drugs that suppress the immune system. Some medicines are needed only during flare-ups. You may need long-term medicines to suppress your immune system. Depending on your symptoms, your doctor may also recommend these medicines and supplements:
- Antibiotic
- Pain reliever
- Vitamin supplements
In severe cases of inflammatory bowel disease, you may need to go to the hospital for intravenous fluids or surgery.
During your treatment, you will most likely be treated by a team of doctors. This team may include your family physician, a gastroenterologist , and, possibly, a surgeon.
Read Also: Can Stomach Ulcers Be Cancerous
Can Inflammatory Bowel Disease Be Prevented Or Avoided
IBD cannot be prevented, but there are lifestyle changes you can make to minimize symptoms. The best thing you can do is to take good care of yourself. Its important to eat a healthy diet. Depending on your symptoms, your doctor may ask you to reduce the amount of fiber or dairy products in your diet. It also may be necessary to limit or avoid caffeine, alcohol, and carbonated beverages. In addition to eating well, you need to get enough rest and exercise regularly. Its also important that you learn to manage the stress in your life. When you become overly upset by things that happen at home or at work, your intestinal problems can get worse.
Symptoms Of A Duodenal Ulcer
If you have a duodenal ulcer, you might:
- have pain in the stomach or abdomen
- have indigestion
Very occasionally, an ulcer can cause serious complications. Go to the emergency department if:
- you have a sharp pain in your stomach that doesnt go away
- your vomit or stools look bloody or a black colour
If you are concerned about symptoms, you can use healthdirects online Symptom Checker to get advice on the next appropriate healthcare steps and when to seek medical attention.
You May Like: Do Ulcers Cause Weight Loss
Don’t Miss: Ulcerated Nodular Basal Cell Carcinoma
When Should I Call My Healthcare Provider
See your healthcare provider right away if you have any of these symptoms:
- Vomiting blood or dark material that looks like coffee grounds
- Extreme weakness or dizziness
- Blood in your stools
- Nausea or vomiting that doesnt get better, or gets worse
- A sudden, severe pain that may spread to your back
- Losing weight without even trying
Untreated peptic ulcers may cause other health problems. Sometimes they bleed. If they become too deep, they can break through your stomach.
Ulcers can also keep food from going through your stomach.
Is It Important To Treat A Flare Early Or Is It Ok To Wait A Bit
Inflammation typically does not resolve without treatment and early intervention has a better outcome than waiting to treat. At an early stage of a flare, a more optimal baseline treatment is often enough to get the inflammation under control. If you wait, there is a greater risk that you might need drugs with greater side effects, such as oral steroids. By waiting, you will have to manage longer with your symptoms before getting relief. Living with constant or longer periods of inflammation might increase your risk for future complications, as inflammation might cause damage to the gut wall that accumulates in severity with each flare.
If you are experiencing worsening symptoms, you have probably already had the flare for some time without symptoms. Evidence shows that a stool test for inflammation in the colon, called fecal calprotectin, is often elevated for two to three months before any symptoms appear. Your colon might also start to show visual evidence of inflammation before you have symptoms, or at least indicate an increased risk for a flare.
You May Like: Foods You Can Eat With An Ulcer
Purpose Of Stomach Ulcer Surgery
Peptic ulcers can cause pain, stomach discomfort, abdominal cramps, decreased appetite, hematemesis, gastrointestinal bleeding, iron deficiency anemia , and malnutrition.
Generally, the condition can be effectively treated with medication and lifestyle changes, rather than with surgical intervention. Smoking and alcohol use can contribute to stomach ulcers, and stopping these habits can help an ulcer heal. Sometimes dietary modifications, like avoiding spicy foods, can help control symptoms.
Treatments for gastric ulcers include proton pump inhibitors and antibiotics to eradicateHelicobacter pylori, a bacteria that is commonly associated with stomach ulcers.
Surgical management may be needed for complications of peptic ulcer disease or for treatment of a stomach ulcer that doesnt improve despite conservative management.
Issues that may warrant surgical intervention for the treatment of peptic ulcer disease include:
These issues can cause persistent and serious health problems. Stomach ulcer surgery would be done to alleviate your symptoms and prevent consequences to your overall health.
Should You Try Probiotics For Crohn’s
People with Crohn’s and other forms of irritable bowel disease lack some of the gut microbes found in other people. Some of these microbes include anti-inflammatory bacteria. Probiotics are thought to improve gut health by providing living microorganisms that can help repopulate your insides in health-promoting ways. As with any treatment, it is important to discuss probiotics with your doctor before attempting to increase them in your diet. Some probiotics sources include:
- Yogurt
- Probiotic supplements
Also Check: Icd 10 Venous Stasis Ulcer Left Leg
What Are The Signs & Symptoms Of Ulcerative Colitis
The most common symptoms of ulcerative colitis are cramping belly pain and diarrhea. Other symptoms include:
- blood in the toilet, on toilet paper, or in the stool
- urgent need to poop
- low energy
- weight loss
Ulcerative coliits can cause other problems, such as rashes, eye problems, joint pain and arthritis, and liver disease. Kids with ulcerative colitis may not grow well as well as other kids their age and puberty may happen later than normal.
What Causes Colon Ulcers
Colon ulcers have many causes. Where the ulcers are located in your colon may help diagnose the cause.
Crohnâs disease and ulcerative colitis . Both Crohnâs and UC are types of inflammatory bowel disease , an inflammation of your colon. These diseases can cause erosions or ulcers in your colon tissue. In Crohnâs, ulcers affect patchy areas of the colon. They can appear in any part of your intestine. UC inflammation affects only the inner lining of your large intestine. It never causes ulcers in your small intestine.
Colon ulcers are often the first sign of Crohnâs. Ulcers caused by Crohnâs disease often crop up on the side of your colon near the mesentery, the tissue that holds your intestines to the inner wall of your abdomen.
After surgery. Erosions and ulcers are a rare possible complication of gastric band surgery to treat obesity. The band can slip and travel to your colon, where it causes an erosion. Your doctor can diagnose this with an image test like a colonoscopy, which uses a camera on the end of a long, flexible tube to examine your colon.
Diverticulitis. As many as 60% of older adults develop diverticulitis, an inflammation of sac-like bulges in your colon wall. If digested food gets stuck in the sac, it can cause pressure to build up and can lead to an erosion.
You can also get colon erosions from infection with cytomegalovirus .
Gastrointestinal Endoscopy: âAphthous Ulcers in Terminal Ileum Encountered During Colonoscopy: Are They Significant?â
You May Like: What Is Ulcer Pain Like
Crohns Disease In Children & Teens
Crohns disease most commonly affects children in their late teens and young adults in their 20s and 30s. Nevertheless, it can affect infants and young children as well. Crohns disease is not rare 100,000 teens and preteens in the U.S. have Crohns disease. For children, the social problems created by the symptoms of Crohns disease are difficult to deal with since the disease can restrict activities. The chronic inflammation can also add to the social difficulties with stunted growth and delayed puberty. Emotional and psychological factors always must be considered in young people with Crohns disease.
How Does Crohn’s Disease Affect The Intestines
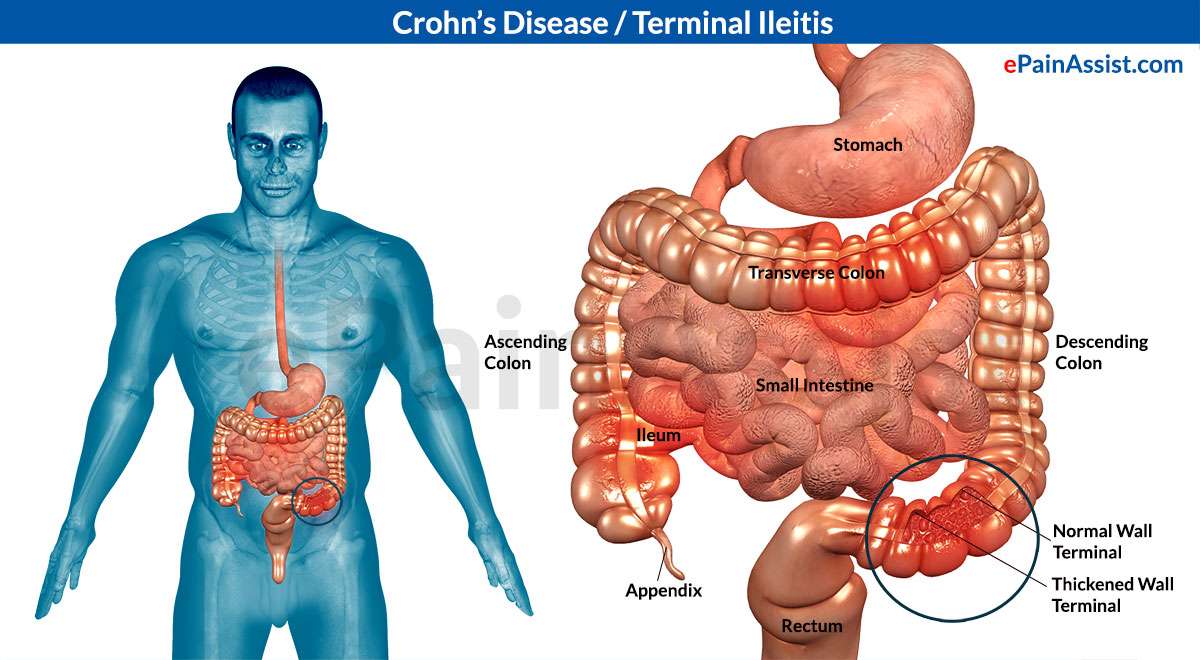
The first signs of Crohn’s disease are small ulcers, called aphthous ulcers, caused by breaks in the lining of the intestine due to inflammation. The ulcers become larger and deeper. With the expansion of the ulcers comes swelling of the tissue, and finally scarring of the intestine that causes stiffness and narrowing. Ultimately, the narrowing can obstruct the flow of food being digested in the intestines. The deepening ulcers can fully penetrate the intestinal wall and enter nearby structures such as the urinary bladder, vagina, and parts of the intestine. These penetrating tracts of inflammation are called fistulas.
You May Like: What’s The Signs Of An Ulcer
Ulcers Of The Small And Large Intestine
Solitary ulcers of the small intestine result from a wide variety of causes . Radiation injury is a known cause of small intestinal ulceration and is discussed in Chapter 39. Solitary ulcers beyond the duodenum that cannot be explained on the basis of any known etiology are referred to as nonspecific or idiopathic intestinal ulcers. Such solitary nonspecific ulcers are rare, with an incidence of 4 per 100,000.1
In a review of the Mayo Clinics experience with 59 cases of small intestinal ulcers over a 22-year period ending in 1979, Boydstun and associates1 showed that 53 patients had no identifiable cause of ulceration. Patients ranged in age from 17 to 77 years, with most presenting in the fifth and sixth decades of life no gender predominance was found. The most common presenting symptom was intermittent small bowel obstruction . Physical findings ranged from nonspecific abdominal tenderness and distention to an acute abdomen resulting from intestinal perforation. Laboratory evaluation was notable only for anemia in one half of the patients. Radiologic studies localized the ulcer in a minority of patients.