What Are The Types Of Ibd
Crohns disease and ulcerative colitis are the main types of IBD. Types include:
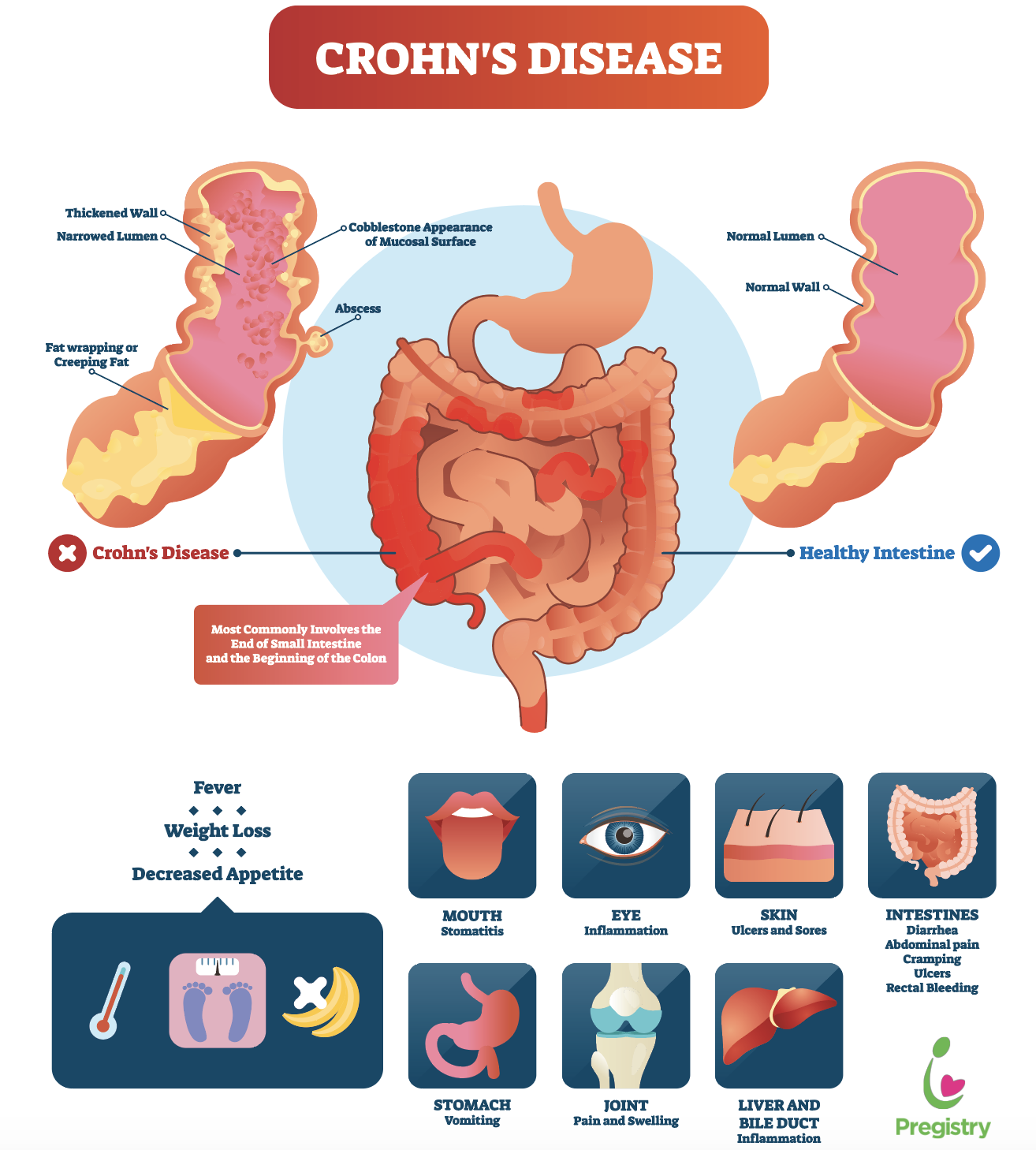
- Crohns disease causes pain and swelling in the digestive tract. It can affect any part from the mouth to the anus. It most commonly affects the small intestine and upper part of the large intestine.
- Ulcerative colitis causes swelling and sores in the large intestine .
- Microscopic colitis causes intestinal inflammation thats only detectable with a microscope.
What Is The Outlook For People With Inflammatory Bowel Disease
Because of the nature of its symptoms and the fact that people with the condition often eventually require one or more surgeries, people with IBD may experience a poorer quality of life than their healthier peers.
As far as life expectancy, this varies depending on which condition a person has. Those with Crohns disease may have a somewhat shorter lifespan, due to complications from the disease. People with ulcerative colitis may have a normal life expectancy, in part because of advancements in treatment in recent years.
Will I Need Surgery For Crohn’s Disease
Maybe. More than half of people with Crohn’s disease need surgery within 20 years of being diagnosed.16 Surgery can relieve your symptoms, but it cannot cure the disease.
Surgeries for Crohn’s disease include:15
- Bowel resection. In this surgery, your doctor removes the damaged part of your small or large intestine and sews the two healthy ends together.
- Removal of your large intestine, including your rectum. After this procedure, your body can no longer get rid of solid waste on its own. Your doctor will make a small opening in the front of your abdominal wall. Then your doctor will bring the end of your small intestine through the hole. This allows waste to drain out of your body. A pouch is worn over the opening to collect waste. You will need to empty the pouch several times a day.
- Fistula surgery. Some patients develop a collection of pus or drainage of pus from an opening around the anus. Surgery may be required to drain the pus and put in a small wire to keep the pus from recollecting.
Read Also: What Should I Eat With Ulcerative Colitis
Other Forms Of Respiratory Involvement
Exudative pleuritis, usually eosinophilic, may accompany other lung pathologies . Exudative pericarditis with possible life-threatening tamponade may also be present in these patients . Pachypleuritis with extensive pleural fibrosis was described in a CD patient . Good responses to steroids have been reported in all cases of pleuritis or pleuropericarditis. Pneumothorax is a rare complication, and was described in a patient suffering from CD-related granulomatous lung disease . An air-leak syndrome associated with organizing pneumonia pattern was described as an unusual presentation of UC-related bronchopulmonary involvement .
Patients with IBD are at increased risk of pulmonary embolism. The risk of thromboembolic complications is 34 times higher compared to the general population therefore thromboembolism should always be considered in cases of acute and unexplained pulmonary symptoms in IBD patients.
What Is The Best Diet For Ulcerative Colitis
Theres no single diet that works best for ulcerative colitis. If the disease damages the lining of the colon, your body might not absorb enough nutrients from food. Your healthcare provider may recommend supplemental nutrition or vitamins. Its best to work with your provider and nutritionist to come up with a personalized diet plan.
You May Like: How To Treat A Diabetic Foot Ulcer On The Sole
What Are Surgical Treatments For Ulcerative Colitis
After 30+ years of living with ulcerative colitis, about 1 in 3 people need surgery.
A surgeon:
- Removes the colon or the colon and rectum .
- Connects the small intestine and anus.
- Creates an ileal pouch that collects stool, which then exits through the anus.
Rarely, you may need an ileostomy instead of an ileal pouch. An ileostomy bag attaches outside of the belly to collect stool.
A proctocolectomy is curative. Symptoms wont return after surgery to remove the colon and rectum. However, you may have problems with the ileostomy or ileal pouch, such as pouchitis .
What Side Effects Of Ibd Can Cause Malnutrition
There are several reasons why people with IBD may be at risk for malnutrition. The following list includes some side effects that contribute to malnutrition.
- Inadequate food/fluid intake may by caused by nausea, abdominal pain, loss of appetite or altered taste sensation
- Increased losses â intestinal inflammation during acute flares results in increased protein losses, losses from fistula fluids, diarrhea and bleeding
- Increased nutritional needs â inflammation or infection increases metabolic requirements
- Malabsorption with Crohn’s disease may be caused by severe intestinal inflammation, resection of small intestine and medications, such as prednisone and sulfasalazine
You May Like: What Does A Colon Ulcer Feel Like
Is Cannabis Effective For Ulcerative Colitis And Crohns Disease
IBD is a chronic condition that can seriously impact your quality of life depending on your symptoms. Scientists still dont know the exact cause of IBD, but they believe genetics, diet, and environmental influences may all be factors.
Current treatments available for IBD arent always effective at managing UC and CD symptoms long-term, particularly if you have severe symptoms such as diarrhea with bloody stools, and abdominal pain. This is why scientists are searching for new therapies to better manage these chronic conditions to improve peoples long-term outlook.
found in cannabis plant varieties with many different effects. There are still a lot of questions about their use for IBD treatment.
Some important questions include:
- Which types may be beneficial ?
- How do they work for IBD symptoms?
- Which forms and dosage are best?
- What is known about the safety and risks of long-term use?
For example, a 2020 review of studies of cannabis for IBD found insufficient evidence for the effectiveness and safety of cannabis for managing UC and CD symptoms. More research is needed to understand if cannabis has benefits for UC or CD symptoms and if the long-term complications outweigh the benefits.
Symptoms Of Inflammatory Bowel Disease
Inflammatory bowel disease affects your bodys digestive system. The main symptom of ulcerative colitis is diarrhea with blood and mucus, with or without abdominal pain.
Crohns disease has more varied symptoms, with the most common symptoms listed first:
- abdominal pain and cramps
- lack or loss of appetite
- weight loss
- arthritis
- slowing of growth
These symptoms can make everyday activities difficult or impossible. They can also lead to serious health problems.
Don’t Miss: What Do You Do For An Ulcer In Your Stomach
Ulcerative Colitis And Crohns Disease
Inflammatory bowel disease includes a number of conditions in which the immune system mistakenly attacks the intestines and triggers inflammation of the tissues. There are two main kinds of IBD: ulcerative colitis and Crohns disease. Today many medications are available to successfully treat IBD. These therapies work to calm inflammation, reduce and even alleviate symptoms, decrease flare-ups, and help you better cope with your condition. This report provides insight into the possible causes and complications of IBD, how you are diagnosed, and the steps you can take for better care so you can live your best life.
How Is Ulcerative Colitis Diagnosed
To diagnose ulcerative colitis in children, teenagers and adults, your healthcare provider has to rule out other illnesses. After a physical exam, your provider may order:
- Blood tests: Your blood can show signs of infection or anemia. Anemia is a low level of iron in your blood. It can mean you have bleeding in the colon or rectum.
- Stool samples: Signs of infection, parasites , and inflammation can show up in your poop.
- Imaging tests: Your healthcare provider may need a picture of your colon and rectum. You may have tests including a magnetic resonance imaging scan or computed tomography scan.
- Endoscopic tests: An endoscope is a thin, flexible tube with a tiny camera. Specialized doctors can slide the endoscope in through the anus to check the health of the rectum and colon. Common endoscopic tests include colonoscopy and sigmoidoscopy.
Read Also: Sand Beds For Pressure Ulcers
Does Ulcerative Colitis Make You Immunocompromised
Ulcerative colitis doesnt make you immunocompromised. Some of the medicines that treat it may change the way your immune system responds. This change is different for each medication. Some of these changes may increase the risk of certain infections or other issues. A discussion with your health care team before starting a medication is the best way to understand these risks and ways to prevent them.
How Are Ulcerative Colitis And Crohn’s Disease Similar
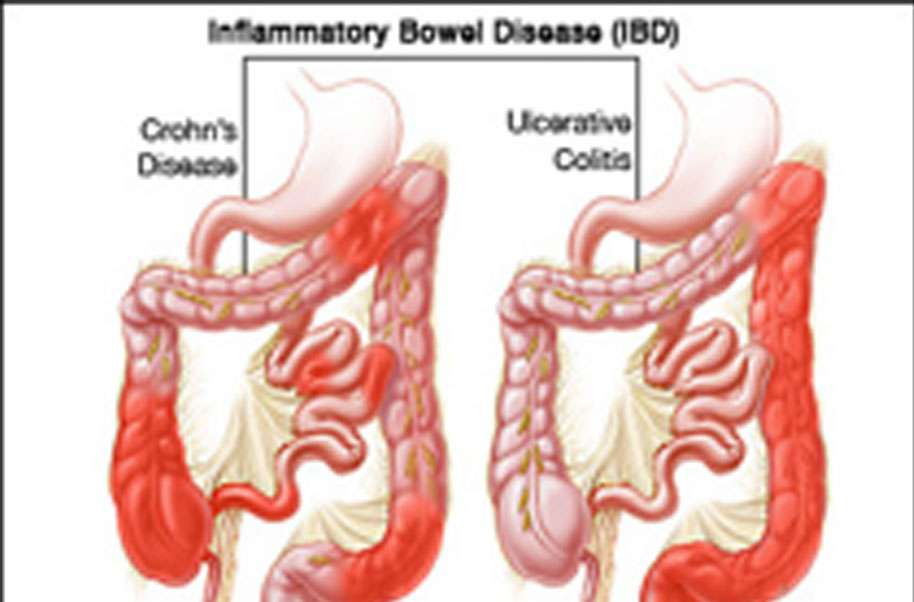
- Both diseases often develop in teenagers and young adults although the disease can occur at any age
- Ulcerative colitis and Crohn’s disease affect men and women equally
- The symptoms of ulcerative colitis and Crohn’s disease are very similar
-
The causes of both UC and Crohn’s disease are not known and both diseases have similar types of contributing factors such as environmental, genetic and an inappropriate response by the body’s immune system
Recommended Reading: How Do You Get Ulcers On Your Legs
Surgery A Last Resort
For patients with certain complications and those whose disease is not controlled with medication, surgery is an option.
For ulcerative colitis, the colon is removed. After the surgery, the disease will not recur. With Crohns, surgery to remove the diseased segment of the bowel may be necessary if a persons symptoms do not respond to medication, or if they develop an intestinal blockage, or a fistulaan ulcer that tunnels through the intestine and into the surrounding tissue, often around the anus and rectum. Other complications that may require surgery include excessive bleeding in the intestine or perforation of the bowel. The surgery does not cure Crohns but it can reduce symptoms and address complications that are not amenable to medical therapy.
If surgery is required for ulcerative colitis, the standard surgical procedure is removal of the colon and rectum, called proctocolectomy. In the past, patients who underwent this procedure had to wear a bag over a small hole in the abdomen to collect stool. Today, many patients undergo variations to the procedure that do not require wearing a permanent external bag.
Many patients with Crohns have surgery on their small bowel. urgery for Crohns removes the area that is most involved, leaving behind as much bowel as possible. In many cases, the surgeon removes the end of the small bowel and beginning of the colon and reconnects those areas.
Interview with Dr. Darrell S. Pardi, July 2017.
References
What Medicines Treat Ibd
Medicines used to treat IBD help reduce inflammation, relieve symptoms, and prevent future flare-ups. Your doctor may give you:10,15
- Medicines to control inflammation, such as:
- Aminosalicylates, which may also help prevent flare-ups. Most people with mild to moderate ulcerative colitis and some people with Crohn’s disease are treated with aminosalicylates.
- Biologic therapies, which block substances in your body that cause inflammation
- Antibiotics, which may help if you have an infection or overgrowth of bacteria
You may need to try several different medicines before you find what works best for you.
Recommended Reading: Over The Counter Remedies For Ulcers
Effects Of Crohns Disease And Ulcerative Colitis
Every person responds differently to IBD. The severity of symptoms will vary from time to time and from person to person. IBD is not a progressive disease . Rather, flare-ups can range from mild to severe and back to mild again. Some people will experience periods of relief from symptoms in between flare-ups.We cannot predict how long a person will stay free from symptoms, or when their next flare-up will occur. Some flare-ups settle down quite quickly with treatment. Other times, it may take months for a persons symptoms to respond to treatment.IBD interferes with a persons normal body functions. Signs and symptoms can include:
- pain in the abdomen
- delayed or impaired growth in children.
What Is Inflammatory Bowel Disease
Inflammatory Bowel Disease causes chronic inflammation of the intestines not due to infections or other identifiable causes. There are two main types of IBD: ulcerative colitis and Crohns disease. Ulcerative colitis affects only the lining of the large intestine , while Crohns disease can involve any part of the intestine, small or large, and irritate not only the lining, but also deeper layers.
It is estimated that about 3.1 million Americans suffer from IBD. Males and females are affected equally. Ulcerative colitis and Crohns disease may occur at any age, including young children but occur most often in young adults. Most cases of Ulcerative colitis and Crohns disease are diagnosed before age 30. Crohns disease tends to occur in families and in certain ethnic groups, such as Eastern European Jews. About 5 percent to 8 percent of patients may have a family member with IBD and about 20 percent to 25 percent of patients may have a close relative with the condition. However, it can occur in any ethnic group and in members of families where no one else has these diseases.
Treating Inflammatory Bowel Disease
Nationwide Children’s Hospital offers a team of experts focused on the treatment of children and teens with inflammatory bowel disease.
What is Inflammatory Bowel Disease or IBD?
Recommended Reading: Quantitative Research On Pressure Ulcer Prevention
How Is Ibd Diagnosed
Crohns disease and ulcerative colitis cause similar symptoms. No single test can diagnose either condition.
To make a diagnosis, your healthcare provider will ask about your symptoms. Your workup may start with a complete blood count and stool test to look for signs of intestinal inflammation.
You may also get one or more of these diagnostic tests:
- Colonoscopy to examine the large and small intestines.
- EUS to check the digestive tract for swelling and ulcers.
- Flexible sigmoidoscopy to examine the inside of the rectum and anus.
- Imaging scan, such as a CT scan or MRI, to check for signs of inflammation or an abscess.
- Upper endoscopy to examine the digestive tract from the mouth to the start of the small intestine.
- Capsule endoscopy using a small camera device that you swallow. The camera captures images as it travels through the digestive tract.
Treatment For Ulcerative Colitis
The treatment for ulcerative colitis is complex and may be different for every child, but the main goals are the same: to relieve symptoms, prevent flares, and achieve mucosal healing and remission. There is no one size fits all treatment for ulcerative colitis, and children respond to therapy differently. Using a combination of medication, nutritional therapy, and in more severe cases, surgery, we aim to promote each childs quality of life without limiting his or her goals or dreams. Primary treatment for ulcerative colitis includes medications. Those most often used in the treatment of ulcerative colitis are 5-aminosalicylates, corticosteroids, antibiotics, and medications that alter the immune system, called immunomodulators or biologics.
Read Also: Triderma Diabetic Ulcer Defense Healing Cream
Ulcerative Colitis And Joint Pain
When you have ulcerative colitis , its normal to have pain in your abdomen, along with diarrhea and other gastrointestinal symptoms.
Up to 30 percent of people with UC also have arthritis, which is characterized by swollen, painful joints.
Heres a look at the connection between UC and joint pain, as well as what you can do to protect your joints if you have UC.
What Is Ulcerative Colitis
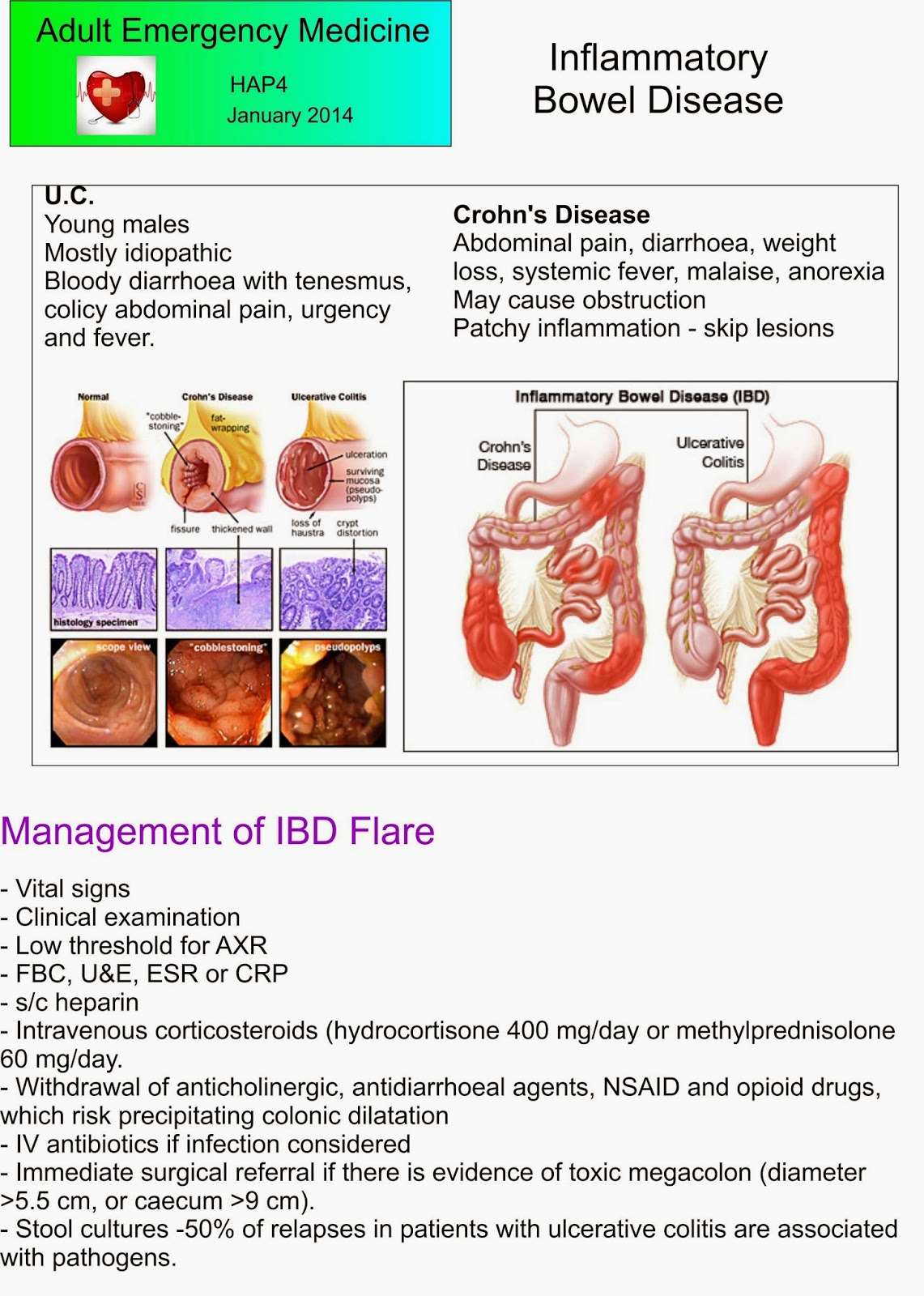
Ulcerative colitis causes irritation and ulcers in the large intestine . It belongs to a group of conditions called inflammatory bowel disease . It often causes diarrhea with blood, cramping and urgency. Sometimes these symptoms can wake a person up at night to go to the bathroom as well.
The inflammation in ulcerative colitis usually starts in the rectum, which is close to the anus . The inflammation can spread and affect a portion of, or the entire colon. When the inflammation occurs in the rectum and lower part of the colon it is called ulcerative proctitis. If the entire colon is affected it is called pancolitis. If only the left side of the colon is affected it is called limited or distal colitis.
The severity of UC depends on the amount of inflammation and the location. Everyone is a little different. You could have severe inflammation in the rectum or very mild inflammation in the entire colon .
If you have ulcerative colitis, you may notice a pattern of flare-ups , when symptoms are worse. During times of remission, you might have little to no symptoms. The goal with therapy is to remain in remission as long as possible .
You May Like: Bed To Prevent Pressure Ulcers
How Does Ibd Affect Pregnancy
IBD can affect your chances of getting pregnant and your symptoms during pregnancy. Pregnant women with IBD may have a high-risk pregnancy.
- Before you get pregnant: You may have more trouble getting pregnant during a flare-up . Also, if you have IBD, talk to your doctor about your risk of problems during pregnancy. If you have a flare-up during pregnancy, you have a slightly higher risk of premature birth, low birth weight, and cesarean delivery than women who do not have IBD.30
Your doctor may also change the type or amount of the medicine you take. Some medicines, such as methotrexate and thalidomide, cause birth defects and other health problems and should not be taken while you are pregnant or breastfeeding.31 If you might become pregnant, talk to your doctor about any medicines you take.
- During pregnancy: Some women say their symptoms get better during pregnancy, but others say they get worse. Women whose IBD is in remission before getting pregnant are more likely to stay symptom-free during pregnancy.31