Signs You May Have An Ulcer
Did you know that stomach ulcers also called peptic ulcers affect at least 1 in 10 Americans over the course of their lives? And while stomach ulcers can be treated easily when caught early, lack of medical care can lead to serious complications.
Understanding the signs of stomach ulcers is important in helping you get the treatment you need. At Prima Medicine in Fairfax and South Riding, Virginia, our care team has the experience and knowledge to diagnose and treat stomach ulcers. Weve curated this guide to help you recognize the warning signs of an ulcer and understand what you can do about it.
Burning Pain In The Abdomen
Persistent burning pain in the abdomen is one of the first signs of a stomach ulcer. The sensation of pain occurs when juices in the stomach, which help in digestion, come into contact with an open sore in the stomach lining.
In most cases, the pain is felt from the breast bone to the navel, and it often worsens during the night. If you skip meals, particularly breakfast, you may also experience this burning sensation in the stomach during the daytime.
If the dull and burning ache of the ulcer often turns into a sharp, stabbing pain, it is a sign that your ulcer is acting up and you need medical help. It could mean that the ulcer has caused a more critical problem like a perforation in the wall of your stomach or intestine, or a blockage in your digestive tract, and it is triggering intense pain.
Can You Prevent A Peptic Ulcer
While stress and spicy foods can make symptoms of a peptic ulcer worse, they donât seem to make you more likely to have one. But a few other things can raise your chances.
Be careful when you take pain relievers. Some people who have arthritis or other conditions that cause chronic pain take nonsteroidal anti-inflammatory drugs for weeks or months at a time to ease pain and swelling. These medicines can affect the mucus that protects your stomach against acid and make you more likely to have peptic ulcers.
These pain relievers include:
You’re more likely to get an ulcer while taking one of these if you:
- Are over age 65
- Are infected with H. pylori bacteria
- Take more than one NSAID at a time
- Have had a peptic ulcer in the past
- Also take a steroid drug or selective serotonin reuptake inhibitor
To lower your chances for peptic ulcers while you take NSAIDs:
- Use the lowest possible dose to control your symptoms, and stop taking them as soon as you no longer need them.
- Take your medicine with food.
- Don’t drink alcohol while youâre taking these medicines.
While you’re on NSAIDs, you can take medicine to lower the amount of acid your stomach makes. Drugs that can do that include:
- H2 blockers such as cimetidine , famotidine , and nizatidine
You can also take the drug misoprostol to boost the amount of protective mucus your stomach makes. But that can cause side effects like diarrhea and stomach cramps.
- Dairy products that have live cultures, like yogurt, kefir, and aged cheeses
Also Check: Does Ulcerative Colitis Cause Fatigue
What Questions Should I Ask My Doctor
If you have stomach ulcers, you may want to ask your doctor:
- What pain reliever can I use instead of an NSAID?
- How will I know if the H. pylori infection is gone?
- How do we find out if the ulcer has healed?
- What can I do relieve symptoms at home during treatment?
A note from Cleveland Clinic
Contrary to commonly held beliefs, ulcers arent caused by stress or foods you eat. Most of time, bacteria causes them. Doctors can treat the bacteria with antibiotics and other medications.
If youve been popping a lot of antacids lately, youre constantly snacking to get rid of a gnawing pain in your stomach or you have any other signs of an ulcer, the best thing you can do for your health is talk to your provider. Treatment can heal an ulcer in a matter of weeks.
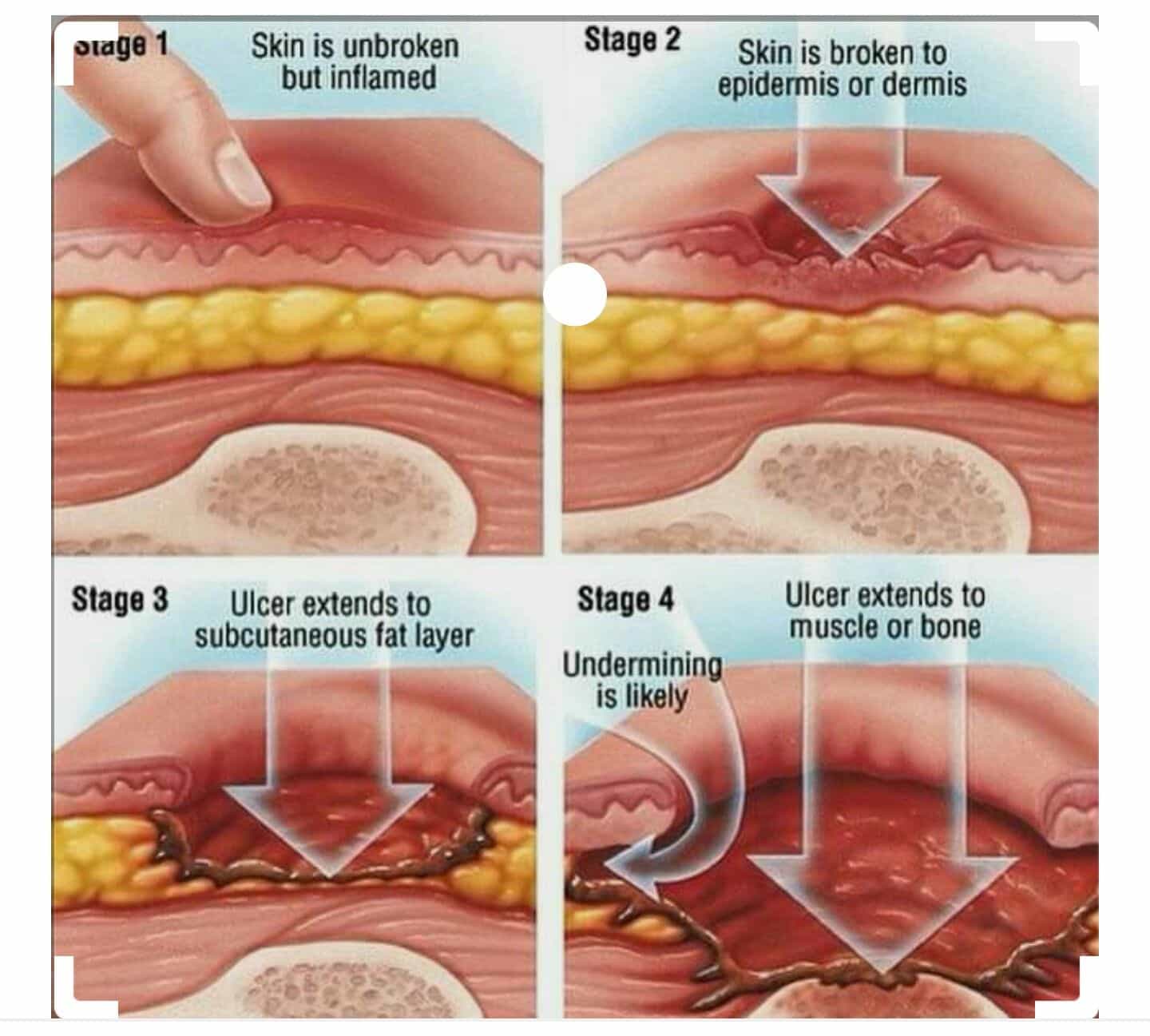
How Are Pressure Sores Caused
Pressure sores, also known as decubitus ulcers, have been called bed sores colloquially for a reason many times, they are caused by excessive pressure brought on from lying in a hospital bed for prolonged periods, without repositioning to relieve it. This may affect blood supply to the bony prominences below or skin surface. When too much pressure is placed on the skin , pressure sores will develop, often in the form of a blood filled blister. The key to preventing pressure sores is utilizing techniques and technology that relieve pressure, assess risk holistically and allow for a hospital environment in which pressure sore prevention is prioritized.
Read Also: Signs Of Ulcers In Humans
What Triggers Stomach Ulcer Symptoms
Stomach ulcer symptoms are irritated by several triggers. They include:
- Stomach acid â some people notice it after they eat while others notice it more on an empty stomach
Our site is the source of information about the gastroenterology related conditions and procedures. This information is intended for patients looking to learn about our gastroenterology practice in New York and make an appointment to see one of our physicians. This information is only intended to provide guidance, not definitive medical advice. Please consult a doctor or GI specialist about your specific condition. Only a trained physician can determine an accurate diagnosis and proper treatment. Terms and conditions are subject to change.
Can Stomach Ulcers Be Treated
Yes, stomach ulcers can heal well with a medication regimen. The type of treatment will depend on what caused your ulcer.
If your stomach ulcer was caused by a H. pylori bacterial infection, youll likely receive antibiotics and a proton pump inhibitor medication. The antibiotics could include:
The PPIs that you will also be prescribed will block the production of stomach acid. There are both prescription and over-the-counter PPI medications, including:
You may also end up taking histamine blockers, or H-2 blockers, that reduce the stomach acid released into your digestive tract. The reduction of stomach acid can promote healing and lessens the pain you may be feeling. Your doctor may prescribe these or you could take over-the-counter medications such as:
Your doctor may also prescribe antacids to help with symptom relief. There are also medications called cytoprotective agents to protect the lining of your stomach, such as Carafate and Cytotec .
Recommended Reading: Side Effects Of Humira For Ulcerative Colitis
The Early Signs Of Leg Ulcers
Most leg ulcers, unless they are caused by injury or trauma, dont develop overnight. In fact, most venous leg ulcers take months, if not years, to develop into a giant, visible open sore.
Even though it takes months or years for ulcers to develop doesnt mean there arent signs or symptoms of them. There are numerous signs that could indicate you are developing an ulcer on the leg.
Some of the signs and symptoms that are often associated with venous ulcers include:
- Discolored skin, usually around the ankles, that appears reddish-brown or purple
- Skin that feels extremely dry
- Skin that has a very firm appearance
- Chronic swelling a doctor will run tests to determine the primary lymphedema causes that resulted in the swelling
- Noticeably swollen or enlarged veins
- Extremely heavy feeling in the legs
What Causes Peptic Ulcers
Ulcers form when digestive juices damage the walls of the stomach or small intestine. If the mucus layer gets too thin or your stomach makes too much acid, your gut will feel it. The two major causes are:
- Bacteria. Itâs called Helicobacter pylori , and as many as half of us carry it. Most people infected with H. pylori do not get ulcers. But in others, it can raise the amount of acid, break down the protective mucus layer, and irritate the digestive tract. Experts arenât sure how H. pylori infection spreads. They think it may pass from person to person through close contact, like kissing. You may also get it from unclean food and water.
- Certain pain relievers. If youâve been taking aspirin often and for a long time, youâre more likely to get a peptic ulcer. The same is true for other nonsteroidal anti-inflammatory drugs . They include ibuprofen and naproxen. NSAIDs block your body from making a chemical that helps protect the inner walls of your stomach and small intestine from stomach acid. Other types of pain meds, such as acetaminophen, wonât lead to peptic ulcers.
- Smoking cigarettes and drinking alcohol also can make you more likely to get ulcers. Stress and eating a lot of spicy food donât cause ulcers, as experts once thought. But they can make ulcers worse and harder to treat.
Don’t Miss: Cbd Oil For Stomach Ulcers
Warning Signs Of Ulcers
Ulcer is the result of an imbalance in your digestive fluids. It is considered to be a painful sore in the stomach lining or at the opening of the small intestine. Below are the 10 warning signs of ulcers you should know:
1. Abdominal pain: Experiencing a burning sensation or pain in the middle or upper part of the stomach after eating or at night.
2. Flu-like symptoms: Flu like symptoms such as nausea, fever, fatigue and general malaise does not go away over the next few days.
3. Indigestion: Ulcer can cause gastrointestinal pain and terrible indigestion.
4. Loss of appetite: Individual with ulcer may experience appetite loss due to intense and sudden stomach pain.
5. Nausea: Imbalance of digestive juices often lead to nausea. You will likely experience mild to severe nausea with an ulcer.
6. Heavy abdomen: Abdominal heaviness is a common thing to feel as an ulcer develops. The feeling of heaviness in the belly is similar to the burdensome feeling you can get after drinking lots of water.
7. Unexplained hunger: It is also common for someone with ulcer to feel hunger pangs after only a couple of hours from eating a full meal. These are not hunger pangs, but rather ulcer pains, that are caused by increased digestive juices.
8. Sudden weight loss: Loss of appetite may cause sudden weight loss due to lack of eating.
What Are The Warning Signs Of A Venous Leg Ulcer
Unless your leg ulcer is the result of an injury or trauma, its unlikely to develop overnight. In general, venous leg ulcers take months and sometimes years to form into a noticeable, open sore.
The good news is that there are signs and symptoms youre at risk for developing a leg ulcer before a visible sore appears. Some of the warning signs most often associated with venous ulcers include:
- Discolored skin, usually around the ankles
- Skin that feels very dry
You May Like: How To Stop Ulcers From Hurting
How Are Stomach Ulcers Diagnosed
Diagnosis and treatment will depend on your symptoms and the severity of your ulcer. To diagnose a stomach ulcer, your doctor will review your medical history along with your symptoms and any prescription or over-the-counter medications youre taking.
To rule out H. pylori infection, a blood, stool, or breath test may be ordered. With a breath test, youll be instructed to drink a clear liquid and breathe into a bag, which is then sealed. If H. pylori is present, the breath sample will contain higher-than-normal levels of carbon dioxide.
Other tests and procedures used to diagnose stomach ulcers include:
- Barium swallow: You drink a thick white liquid that coats your upper gastrointestinal tract and helps your doctor see your stomach and small intestine on X-rays.
- Endoscopy : A thin, lighted tube is inserted through your mouth and into the stomach and the first part of the small intestine. This test is used to look for ulcers, bleeding, and any tissue that looks abnormal.
- Endoscopic biopsy: A piece of stomach tissue is removed so it can be analyzed in a lab.
What Kind Of Doctor Treats Peptic Ulcers
- If you suspect you may have a peptic ulcer, you may first be diagnosed by your family practitioner or internist.
- Children or teenagers may see a pediatrician.
- For further treatment you will likely be referred to a gastroenterologist, a specialist in disorders of the digestive tract.
- If you have an emergency such as vomiting or severe abdominal pain you will be seen by an emergency medicine specialist in an emergency room.
- In the rare case where surgery is needed, you may see a general surgeon.
Recommended Reading: How To Treat Oral Ulcers
Read Also: I Think I Have An Ulcer What Should I Do
Could I Have An Ulcer And Not Know It
5 min Read Time
Around 25 million people will have a stomach ulcer in their lifetime, according to the Centers for Disease Control and Prevention. Despite their prevalence, the symptoms of an ulcer can frequently be mistaken for other conditions, like heartburnand some people may not show any signs at all. Its also unlikely that stress or your diet is the culprit. If youre concerned that your stomach pain could be something more serious, read on to find out the causes, proper treatment and prevention methods for peptic ulcers.
Also Read Eating Disorders: When To See A Doctor
Abdominal ultrasound is not used for the diagnosis of stomach ulcer but it helps in ruling out other causes of abdominal pain or to help detect presence of fluid in the abdomen which may result from perforation of the stomach.
Other investigations that may be asked for may be used in getting the physiological condition of the individual or help rule out other disease conditions.
Read Also: Is Kimchi Good For Ulcerative Colitis
Read Also: Ulcerative Colitis Nausea In Morning
Acid Reflux Or Heartburn
Acid reflux happens when contents from the stomach move up into the esophagus. It is also called acid regurgitation or gastroesophageal reflux. This occurs when the lower esophageal sphincter is weakened or relaxes at the wrong time. This may cause stomach acid to back up into the esophagus.
The esophageal sphincter is the muscle that tightens to prevent food in the stomach from going back up. Ulcer sores cause disruption with how this muscle functions.
Heartburn is experienced when excessive amounts of acid reflux get into the esophagus. It is described as a feeling of burning discomfort behind the breastbone. The burning then moves up toward the neck and throat. A bitter or sour taste in the back of the throat is reported to be experienced by some people. The pain and pressure brought by heartburn can last for several hours and may worsen after eating.
How Are Ulcers Diagnosed
Your healthcare provider may be able to make the diagnosis just by talking with you about your symptoms. If you develop an ulcer and youre not taking NSAIDs, the cause is likely an H. pylori infection. To confirm the diagnosis, youll need one of these tests:
Endoscopy
If you have severe symptoms, your provider may recommend an upper endoscopy to determine if you have an ulcer. In this procedure, the doctor inserts an endoscope through your throat and into your stomach to look for abnormalities.
H. Pylori tests
Tests for H. pylori are now widely used and your provider will tailor treatment to reduce your symptoms and kill the bacteria. A breath test is the easiest way to discover H. pylori. Your provider can also look for it with a blood or stool test, or by taking a sample during an upper endoscopy.
Imaging tests
Less frequently, imaging tests such as X-rays and CT scans are used to detect ulcers. You have to drink a specific liquid that coats the digestive tract and makes ulcers more visible to the imaging machines.
Read Also: How Does An Ulcer Feel In Your Stomach
How Are Ulcers Treated
Some mild cases of ulcers may not need medical attention as they will heal on their own. However, not seeking proper medical treatment may result in these ulcers coming back.
Antibioticsare normally prescribed to eliminate the infection, and sometimes an acidreducer. They may be prescribed to be taken twice a day for 1 to 2 weeks.
If NSAIDs are causing the ulcers, a doctor may prescribe a protective medication to take along with it.
What Causes Ulcerative Colitis Flareups
When youre in remission from ulcerative colitis, youll want to do everything you can to prevent a flareup. Things that may cause a flareup include:
- Emotional stress: Get at least seven hours of sleep a night, exercise regularly and find healthy ways to relieve stress, such as meditation.
- NSAID use: For pain relief or a fever, use acetaminophen instead of NSAIDs like Motrin® and Advil®.
- Antibiotics: Let your healthcare provider know if antibiotics trigger your symptoms.
Read Also: How Do You Stop A Bleeding Ulcer
Enhancing Healthcare Team Outcomes
An evidence-based approach to peptic ulcer disease is recommended. PUD is a very common disorder that affects millions of people. When left untreated, it has significant morbidity. The majority of patients with PUD present to their primary caregiver, but others may present to the emergency department, urgent care clinic, or an outpatient clinic. Because the presentation of PUD is often vague, healthcare workers, including nurses, need to be aware of this diagnosis. The abdominal pain can mimic a number of other pathologies and consequently lead to a delay in treatment.
Once the diagnosis is made, the key is to educate the patient on lifestyle changes, which include discontinuation of smoking, abstaining from alcohol and caffeinated beverages, and avoid consumption of too many NSAIDs. Gastroenterology nurses monitor patients, provide education, and keep the team updated on the patient’s condition. The pharmacist should educate the patient on medication compliance to obtain symptom relief and a cure. A dietary consult should be sought as there is evidence that obesity may be a trigger factor for peptic ulcer disease. Only through a team approach can the morbidity of peptic ulcer disease be decreased. For most patients with PUD who are treated with the triple regimen or PPI, the outcomes are excellent, but recurrence of symptoms is not uncommon.