What Should I Ask My Doctor
If you have ulcerative colitis, you may want to ask your healthcare provider:
- How much of my large intestine is affected?
- What risks or side effects can I expect from the medication?
- Should I change my diet?
- Will ulcerative colitis affect my ability to get pregnant?
- What can I do at home to manage my symptoms?
- What are my surgical options?
What Is The Outlook For Someone With Ulcerative Colitis
Ulcerative colitis can be managed with treatment. It generally wont alter the life expectancy of most people.
Most people with UC experience acute flares of symptoms during their lifetime. But with treatment, the disease can enter remission, during which symptoms go away.
Remission may last for weeks or even years. The longer the period of remission, the better a persons general health becomes.
Dr. Saurabh Sethi is a board certified physician specializing in gastroenterology, hepatology, and advanced interventional endoscopy. In 2014, Dr. Sethi completed his gastroenterology and hepatology fellowship at Beth Israel Deaconess Medical Center at Harvard Medical School. Soon after, he completed his advanced endoscopy fellowship at Stanford University in 2015. Dr. Sethi has been involved with multiple books and research publications, including over 30 peer-reviewed publications. Dr. Sethis interests include reading, blogging, traveling, and public health advocacy.
Why Patients Stop Uc Treatment
People stop taking their ulcerative colitis medications for a number of reasons, says Phanijphand.
One of the leading reasons is the steep cost of the drugs. The out-of-pocket cost for prescription medicines can run over $2,000 per year, while the cost of UC care in general can run from roughly $15,000 to $25,000 per year, according to a study published in Inflammatory Bowel Diseases in January 2020.
The study also found that patients using biologics had the highest costs. Treating UC with corticosteroids had higher costs than with nonsteroidal anti-inflammatory drugs, but the latter groups costs rose more over time.
Also, when a person feels better, they may decide they no longer need UC medicine.
âSome patients think that once their symptoms are gone, they can stop taking their meds,â Phanijphand says. âThey believe theyâre cured or that they may have been misdiagnosed.â
Also Check: Reasons For Low Energy And Fatigue
Also Check: How Can You Get Rid Of Ulcers
Symptoms Of Ulcerative Colitis
Mika, Facty Staff
Ulcerative colitis is a condition that mainly affects the colon, causing inflammation as well as ulcers. It also affects the rectum, and symptoms can be far-ranging, affecting many parts of the body. The main symptoms include bloody stool, pain, and inflammation. Ulcerative colitis may cause flare-ups, during which symptoms can be especially difficult to manage. Different treatment options are ranging from dietary modifications to medication.
How Common Is Fatigue In Inflammatory Bowel Disease
Fatigue affects many people with IBD, and it occurs more frequently among people with Crohns disease. Approximately 54% of people with Crohns disease and 33% of those with ulcerative colitis report experiencing fatigue.2 Fatigue also seems to worsen with more aggressive disease, with the people with the most aggressive Crohns disease most likely to report fatigue.9 Up to 86% report feeling fatigue during moderate-to-severely active Crohns disease.3 Even during remission, about 40% to 50% of patients with IBD disease report fatigue.3,9
Recommended Reading: What To Eat To Heal An Ulcer
Can Acid Reflux Cause Nerve Pain
Acid reflux symptoms can be typical or atypical in nature. Tingling limbs and nerve pain are considered rare and atypical acid reflux symptoms.
Dr. Mark Babyatsky, a former department chairman at Mount Sinai School of Medicine in New York, explained that inflammation from acid reflux can reach the lungs and trigger pneumonia.
As a result, the diaphragm can become inflamed, affecting the phrenic nerve, which is a nerve connecting the neck, lung, heart, and diaphragm. In this scenario, a patient can feel referred pain in the limbs, specifically the arms and shoulders.
Alternatively, nerve-related issues may be caused by pre-existing neuropathic conditions, leading to acid reflux. An example of this is gastroparesis. Gastroparesis is a form of diabetic peripheral neuropathy characterized by slow digestion. This leads to bloating, heartburn, and vomiting of undigested food.
If youre experiencing acid reflux symptoms with nerve pain, theres a high chance that your nerve pain is not reflux-related, especially if you are experiencing temporary reflux. Get in touch with a medical professional to find a separate diagnosis concerning your nerve pain.
Also Check: Horse Stomach Ulcers Natural Remedies
Can I Stop Taking My Meds In Deep Remission
In a word: no. The key to remaining in remission is sticking to your recommended treatment plan. A study published in PLoS One found that people in remission who stopped taking their meds were five times more likely to relapse. Treatments that may help achieve or maintain UC remission include aminosalicylates, drugs that reduce inflammation in the lining of the colon, and immunomodulators, meds that modify the immune system in order to decrease the bodys inflammatory response. All treatments come with potential side effects, and it can take time to find the one that works best for you.
Also Check: Best Treatment For Stage 2 Pressure Ulcer
Plan Your Day Carefully
If youre experiencing an ulcerative colitis flare, you have only a limited amount of energy to spare. If you usually feel more energetic in the morning, plan to tackle your most demanding tasks at that time. Don’t overcommit when it comes to your social calendar. “Be realistic with yourself and know your limits,” says Parris. She suggests picking one or two events a week and planning for them. For example, if you have an upcoming dinner on a Saturday night, she says, spend that morning and afternoon relaxing instead of running errands.
What To Eat For Acid Reflux
Whether its a chronic condition or a newfound symptom of stressful days, heartburn happens! Avoiding spicy, acidic and fried foods as well as cutting back on alcohol and chocolate can help douse the flames and there are some foods you should gravitate towards to help reduce the discomfort. Heres what you can eat to help keep heartburn symptoms from being too upsetting.
You May Like: Ulcers In Small Bowel Crohn’s
How Often Do I Need A Colonoscopy
Especially when you have symptoms or are just starting or changing medications, your doctor may want to periodically look at the inside of the rectum and colon to make sure the treatments are working and the lining is healing. How often this is needed is different for each person.
Ulcerative colitis also increases your chance of developing colon cancer. To look for early cancer signs, your healthcare provider may have you come in for a colonoscopy every one to three years.
Get Help From A Qualified Dietitian Nutritionist
If you are experiencing IBD fatigue, there is help. Contact a registered and licensed dietitian nutritionist for personalized support and guidance in creating an eating plan that will work for you. With the right tools in your toolbox, you can start to feel better and have more energy to enjoy life again.
You May Like: Diabetic Ulcer On Big Toe
Sleep Disturbance And Fatigue
Sleep disturbances have been implicated as the cause of worsening symptoms including pain and fatigue in chronic inflammatory diseases. Poor sleep has become a keen area of research interest because it is thought to be an environmental factor that is closely linked to worsening IBD symptoms, specifically fatigue . Significant fatigue has been shown to be strongly correlated with poor sleep quality and daytime sleepiness . Population-based sleep quality studies estimate that 32% of adults report poor sleep. Sleep deficiency is an even more common issue among patients with IBD with numerous authors including Graff et al. suggesting rates of problematic sleep in individuals with both active and inactive IBD to be greater than 50% .
Ulcerative Colitis And Colorectal Cancer
Ulcerative colitis increases the risk of colorectal cancer. Colorectal cancer often begins as small growths on the inside of the large intestine. The risk of colorectal cancer increases based on:
- the length of time a person has had ulcerative colitis
- how much of the colon is affected by ulcerative colitis
People with ulcerative colitis should have more frequent tests for polyps and colorectal cancer than people at average risk. The gold standard screening test is a colonoscopy. Polyps can be removed during a colonoscopy. This reduces the risk of colorectal cancer. Ask your doctor how often you should be checked for colorectal cancer.
Surgery to remove the entire colon eliminates the risk of colon cancer.
Also Check: Best Vitamins For Ulcerative Colitis
Should You Stop Taking Your Ibd Medication
First of all, do not make any changes to your medication regimen without first talking to your doctor.
According to the ACG, keeping IBD well-controlled or in remission may help protect you from contracting COVID-19.
Right now the real hotspots for spread of this infection are in health care settings, says Dr. Ungaro. If your condition is well-controlled and you stop taking your usual medications, you risk having a flare. We do not want patients to have a flare in the midst of this pandemic and end up in the ER where they could be exposed .
If youre using steroids: Topical steroids, which are taken via suppositories or enemas, are unlikely to cause problems. Systemic steroids, however, are another story. If youre on oral steroids, now is a good time to start tapering off them if you can, says Dr. Ungaro, but do not stop taking steroids cold turkey. Call your gastroenterologist, discuss whether it is a good idea for you to start decreasing your dose, and find out how to do so slowly and safely.
If youre using aminosalicylates, biologics, or immunomodulators: If youre doing well on a drug in one of these classes, stick with it, says Dr. Morganstern. If you stop, youre at risk of flaring.
One exception, however, may be for patients who are stable and taking both an immunomodulator and a biologic. If someone is in remission on combination therapy, I might try removing the immunomodulator and keeping the biologic, says Dr. Morganstern.
Fatigue In Children With Ulcerative Colitis
In a 2019 study , researchers looked at how children with ulcerative colitis experienced fatigue.
They found that, like adults, children with the condition can experience high levels of fatigue. They noted the following potential reasons for this:
- disease activity level
According to the Crohns and Colitis Foundation, fatigue is a common issue among people with IBD. It affects 80% of people with active IBD and 50% of people in clinical remission.
Despite the frequency of fatigue in IBD, researchers have indicated that it is often underreported and undertreated. They have noted that doctors often do not treat fatigue because of the subjective nature of the condition.
People with fatigue should talk with a doctor and make sure that they understand how much fatigue affects their life. The more information a person can provide about their symptoms, the more likely the doctor is to understand fatigue as a serious symptom and make recommendations for treatment.
In addition to taking steps to manage and treat ulcerative colitis, a person can make certain lifestyle changes to help reduce fatigue.
Some potential ways for a person to improve fatigue and boost energy levels include:
In one 2020 study , researchers found that the best way to treat fatigue is to treat its underlying causes.
Don’t Miss: Can You Get Ulcerative Colitis At Any Age
Warning Disclaimer Use For Publication
WARNING: Please DO NOT STOP MEDICATIONS without first consulting a physician since doing so could be hazardous to your health.
DISCLAIMER: All material available on eHealthMe.com is for informational purposes only, and is not a substitute for medical advice, diagnosis, or treatment provided by a qualified healthcare provider. All information is observation-only. Our phase IV clinical studies alone cannot establish cause-effect relationship. Different individuals may respond to medication in different ways. Every effort has been made to ensure that all information is accurate, up-to-date, and complete, but no guarantee is made to that effect. The use of the eHealthMe site and its content is at your own risk.
If you use this eHealthMe study on publication, please acknowledge it with a citation: study title, URL, accessed date.
Fatigue Is Common Among All People With Uc
Remember, its not just older folks or one biological gender who experience fatigue with ulcerative colitis. Recent research published in the Journal of Crohns and Colitis found more than 60% of people diagnosed with IBDs reported significant fatigue. In another study, lack of energy was the most burdensome symptom reported, even more than gastrointestinal complaints including diarrheawhich is often triggered by inflammation in the large intestine in people with UC. Though fatigue seems to impact more women than men with UC, it can occur in all ages and both sexes, per Advances in Therapy.
Also Check: What Is Acute Ulcerative Colitis
Get Checked For Nutrient Deficiencies
Having IBD puts you at risk for nutritional deficiencies.
This can be from inflammation in the intestine preventing nutrients from being absorbed properly or from diarrhea and vomiting preventing proper nutrient absorption.
Your doctor can order a basic blood draw to check for nutrients. Some nutrients to check for in particular are:
If needed, you can take supplements of any nutrients youâre deficient in or focus on eating more foods that the nutrient is found in. Work with your doctor or a practitioner versed in supplementation and make sure the supplements wonât interfere with any medication youâre on.
Eat For Maximum Energy
Diet may play a role in causing UC fatigueespecially if youre not eating a balanced and broad diet, says Dr. Ananthakrishnan . Consuming low FODMAP foods can also help so, too, can avoiding seeds, whole wheats, and lactose foods. While there are several specialized diets that may be helpful for some, no one plan has been proven to prevent or control UC, per the Crohns & Colitis Foundation. Your medical team may recommend a particular diet based on your symptoms and what foods youre best able to tolerate.
Read Also: Why Are Bedridden Patients At Risk For Developing Decubitus Ulcers
Tips For Managing Your Ulcerative Colitis Fatigue
The key to easing fatigue is not to ignore it. Fatigue is a sign that something requires attention, Katkov says. Consider the following steps.
Additional reporting by Ashley Welch.
What Causes Ulcerative Colitis
Ulcerative colitis is thought to be an autoimmune condition.
This means the immune system, the body’s defence against infection, goes wrong and attacks healthy tissue.
The most popular theory is that the immune system mistakes harmless bacteria inside the colon for a threat and attacks the tissues of the colon, causing it to become inflamed.
Exactly what causes the immune system to behave in this way is unclear.
Most experts think it’s a combination of genetic and environmental factors.
Also Check: Ulcerative Colitis And Back Pain
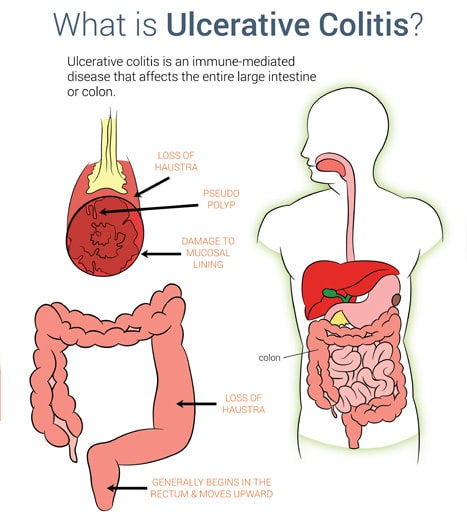
Types Of Ulcerative Colitis :
The different types of ulcerative colitis are classified according to the location, or affected site of inflammation. They are :
Ulcerative Proctitis:
It this inflammation is limited to the rectum. A person has suffered from rectal bleeding, rectal inflammation, pain, urgency , etc.
Proctosigmoiditis:
It involves inflammation of the rectum and the sigmoid colon . Symptoms include abdominal cramps, rectal bleeding, urgency, and tenesmus, diarrhea with blood, etc.
Left-Sided Colitis:
This type involves inflammation that starts at the rectum and extends up the left colon . A person may experience excess weight loss, dehydration, bloody diarrhea, left-sided abdominal pain, etc.
Universal Colitis:
This type is called universal colitis because it affects the entire colon . Symptoms may include fever, night sweating, diarrhea with mucus, weakness, loss of appetite, anemia, etc.
Fulminant colitis:
It is rare but severe form of universal colitis. Patients with this type of colitis are suffered with dehydration, abdominal cramps, diarrhea with bleeding, weakness, loss of appetite, and even shock. Those people are at the risk of developing toxic megacolon and colonic rupture .
You Begin Doing The Things You Used To Do
You will know the treatment and medication are working when you start doing the things you enjoyed doing before. For instance, going out or taking on extra activities. As long as you are maintaining your treatment plan and avoiding triggers, there should be no problem with doing the things you enjoyed doing before.
Don’t Miss: Compression Stockings For Leg Ulcers
Can I Get Surgery For My Ulcerative Colitis
Surgery is an option if medications arent working or you have complications, such as bleeding or abnormal growths. You might develop precancerous lesions, or growths that can turn into colorectal cancer. A doctor can remove these lesions with surgery or during a colonoscopy.
Research shows that about 30% of people with ulcerative colitis need surgery sometime during their life. About 20% of children with ulcerative colitis will need surgery during their childhood years.
There are two kinds of surgery for ulcerative colitis:
Proctocolectomy and ileoanal pouch
The proctocolectomy and ileoanal pouch is the most common procedure for ulcerative colitis. This procedure typically requires more than one surgery, and there are several ways to do it. First, your surgeon does a proctocolectomy a procedure that removes your colon and rectum. Then the surgeon forms an ileoanal pouch to create a new rectum. While your body and newly made pouch is healing, your surgeon may perform a temporary ileostomy at the same time. This creates an opening in your lower belly. Your small intestines attach to the stoma, which looks like a small piece of pink skin on your belly.
After you heal, waste from your small intestines comes out through the stoma and into an attached bag called an ostomy bag. The small bag lies flat on the outside of your body, below your beltline. Youll need to wear the bag at all times to collect waste. Youll have to change the bag frequently throughout the day.