Can Pentasa Be Crushed Split Or Chewed
Pentasa capsules should be swallowed whole. Do not crush, split, or chew Pentasa capsules.
If you cannot swallow the whole capsule, you can open it and sprinkle its contents onto applesauce or yogurt. Be sure to take the applesauce or yogurt right away and avoid chewing it.
If you have problems taking Pentasa, talk with your doctor. You can also see this article.
Does Ulcerative Colitis Make You Immunocompromised
Ulcerative colitis doesnt make you immunocompromised. Some of the medicines that treat it may change the way your immune system responds. This change is different for each medication. Some of these changes may increase the risk of certain infections or other issues. A discussion with your health care team before starting a medication is the best way to understand these risks and ways to prevent them.
How Does Pediatric Ulcerative Colitis Affect My Childs Mental/emotional Health
Like many conditions, ulcerative colitis can have a negative psychological effect, especially on children. They can experience physical, emotional, social and family problems. Because of the medications and/or general stress from the situation, your child may experience:
- Mood swings.
- Worry about appearance and physical stamina.
- Vulnerability because their body doesnt function normally.
- Poor concentration.
- Misunderstandings with friends and family.
Children need mutual support from all family members. Its helpful for the entire family to learn about the disease and try to be empathetic. Seek out a psychiatrist and therapist to help your child manage such challenges of their ulcerative colitis.
Don’t Miss: How Do You Know You Have A Stomach Ulcer
Who Gets Ulcerative Colitis
Anyone at any age, including young children, can get ulcerative colitis. Your chance of getting it is slightly higher if you:
- Have a close relative with inflammatory bowel disease .
- Are between 15 and 30 years old, or older than 60.
- Are Jewish.
- Use frequent nonsteroidal anti-inflammatory drugs like ibuprofen .
More Drugs That Work On Your Immune System
Other types of medicines for ulcerative colitis target your immune system, too. Your doctor may call these immunomodulators. They may be good options if 5-ASAs and corticosteroids havenât worked well for you.
The most common ones are azathioprine , mercaptopurine , and cyclosporine . Due to the risk of side effects, doctors usually save cyclosporine for people who donât have success with other meds. They may also try methotrexate paired with folic acid.
Ozanimod is an oral medication and is the first sphingosine 1-phosphate receptor modulator approved for patients with moderately to severely active UC.
The goal is to lower inflammation in your colon.
These drugs can have side effects. They can damage your liver and make you more likely to get skin cancers, lymphoma, and infections. If you take them, your doctor will test your blood and check you for skin cancer regularly.
Cyclosporine is especially strong, but it works fast. Your doctor might prescribe it to get a severe flare under control, and then give you 6-MP or azathioprine afterward. The drug may cause kidney problems, gout, infections, and high blood pressure.
It can take several months for some of these drugs to work. So your doctor may give you a faster-acting medicine, like a low dose of a corticosteroid, to help in the meantime.
Don’t Miss: How Do You Treat A Peptic Ulcer
Side Effects And Interactions
The more common side effects of biologics can include:
- headache
Biologic drugs may interact with other drugs and biologic agents, including:
- natalizumab , which can be used to treat Crohns disease or multiple sclerosis
- tocilizumab , anakinra , abatacept , which are primarily used to treat arthritis
- warfarin
- theophylline , an asthma medication
- live vaccines such as the varicella zoster vaccine
How Do Doctors Treat Ulcerative Colitis
Doctors treat ulcerative colitis with medicines and surgery. Each person experiences ulcerative colitis differently, and doctors recommend treatments based on how severe ulcerative colitis is and how much of the large intestine is affected. Doctors most often treat severe and fulminant ulcerative colitis in a hospital.
Also Check: Do Enemas Help Ulcerative Colitis
I’ve Been Taking Corticosteroids With Great Success But My Doctor Wants Me To Stop Because Of Potential Side Effects What Are They
Corticosteroids, also known simply as steroids, are often effective at helping people achieve remission. But they shouldn’t be taken long-term because they can cause harsh side effects. These side effects include , , , facial hair, , and an increased risk of infection. Once steroids control the disease inflammation, they are usually phased out and replaced with other medications to maintain remission.
Accessible Labels And Containers
If your prescription label is hard to read, talk with your doctor or pharmacist. Some pharmacies offer labels that have large print, braille, or a code you scan with a smartphone to convert text to speech. If your local pharmacy doesnt have these options, your doctor or pharmacist may be able to direct you to one that does.
If you have trouble opening medication bottles, ask your pharmacist if they can put Pentasa in an easy-open container. They also may be able to recommend tools that can make it simpler to open lids.
Recommended Reading: How Effective Is Humira For Ulcerative Colitis
Ulcerative Colitis Treatment: Medication
The most common medication option is anti-inflammatory drugs. These can be used orally or topically to reduce inflammation of the colon and rectum.
Treating ulcerative colitis is a highly individualized process. At Johns Hopkins, we tailor your treatment to your specific needs and alter the medication as necessary. Your specific medication regimen will depend largely on the severity of your condition.
Other medications include:
-
Immunosuppressive medications: These drugs slow your immune system to stop the immune response that is causing the colon and rectum to swell.
-
Biologics: Like immunosuppressive medications, biologics target the immune system, but biologics act on specific immune system proteins that encourage inflammation.
Factors Associated With Uc
Smokers have lower than average rates of UC . In fact, it has been reported that some patients with UC had disorders after they gave up smoking, and many studies have stressed the association between smoking and protection against UC. This information is certainly no encouragement to smoke. Rather, patients should ask their physician about trials using nicotine replacement aids. Breast feeding also appears to be associated with lower risk of UC. Left-handed people have a significantly higher risk for both IBDs and other diseases associated with immune abnormalities. A 2001 study reported that patients with UC were more likely to have a history of depression or anxiety than those without IBD. Some researchers suggested that depression might alter the immune system and make people more susceptible to UC.
Also Check: What Is Moderate Ulcerative Colitis
Talk With Your Doctor
Many drugs can help reduce your UC symptoms.
Your doctor will suggest medications based on factors such as your overall health and the severity of your condition. You may need to try a few medications before you find a treatment plan that works for you.
If taking one medication doesnt reduce your symptoms enough, your doctor may add a second medication that makes the first one more effective.
It may take some time, but your doctor will work with you to find the right medications to help relieve your UC symptoms.
What Are The Prescription Medications For Uc
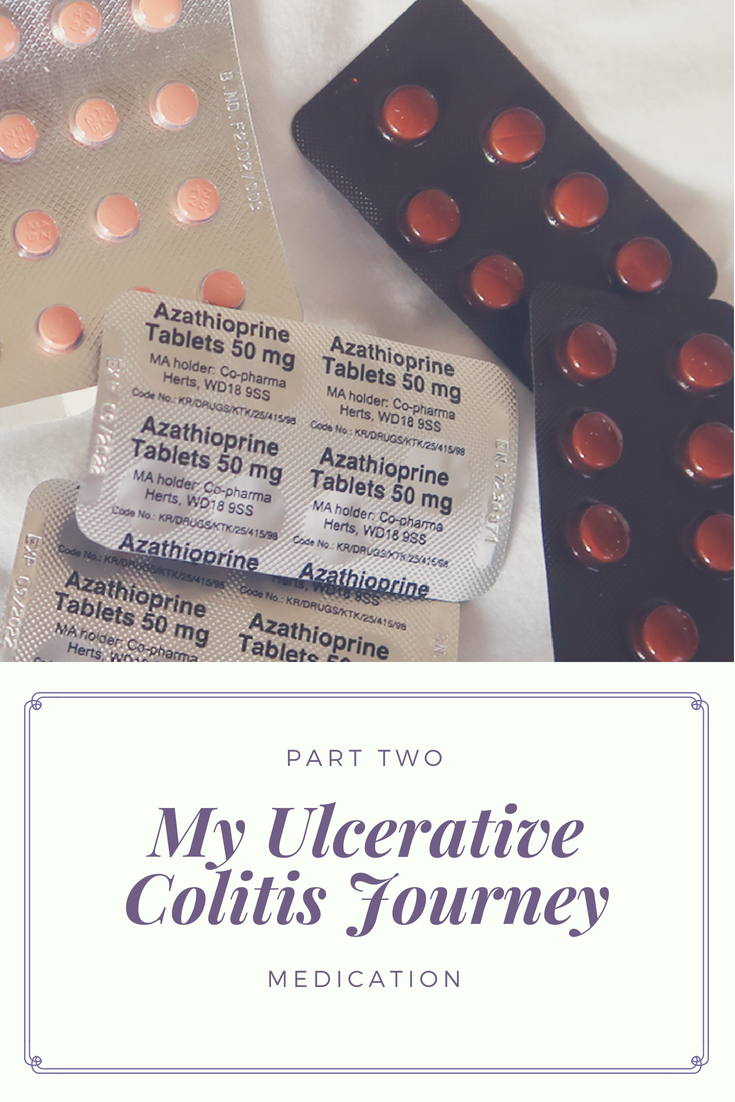
Medication for UC is designed to suppress your immune systems abnormal inflammatory responsewhich is causing symptoms. When inflammation is suppressed, it offers relief from common symptoms .
There are 5 main categories of medications used to treat inflammatory bowel disease like UC.
Given either orally or rectally, these drugs work to decrease inflammation in the lining of the intestines and are usually used to treat mild to moderate UC symptoms. Sulfasalazine and mesalamine are examples of 5-ASA medications.
Metronidazole, ciprofloxacin, and other antibiotics may be used when infections occur, or to treat complications of ulcerative colitis.
These suppress the immune system to reduce inflammation by targeting a specific pathway. Certain biologics work by targeting specific inflammatory proteins that play a role in inflammation called cytokines. Others work by preventing certain white blood cells from getting into inflamed tissues.
Prednisone, prednisolone, and budesonide are included in this type of medication. They affect the bodys ability to initiate and maintain an inflammatory processkeeping the immune system in check. While effective for short-term flare-ups, theyre not recommended for long-term use.
These modify the bodys immune system activity to stop it from causing ongoing inflammation. These drugs , and methotrexate) are usually used to maintain remission or for people who have only responded to steroids.
Don’t Miss: Remicade Vs Entyvio For Ulcerative Colitis
What Is The Latest Treatment For Ulcerative Colitis
Some doctors and researchers believe that ulcerative colitis flare-ups are due to an imbalance of good vs bad bacteria in the gut. Lactobacillus and E. coli probiotics have been shown in some studies to be effective at preventing flare-ups. For this reason, the newest therapy in clinical trials is fecal microbiota transplantation . A solution of fecal matter taken from a healthy family member or centralized stool bank is injected into the patients colon during a colonoscopy. The goal is to recolonize the gut with healthy bacteria. Early case reports show real promise in achieving remission, but more work needs to be done to see how long the positive effects last.
Side Effects Of Ulcerative Colitis
Side effects are based on the biologic medication that youre receiving. While some are minor, others may be life-threatening. You should talk to your doctor before receiving infusion therapy to ensure that you are getting the best option for your UC. The most common side effects include:
- Serious allergic reactions
- Lymphoma and other cancers including skin and cervical cancer
- Heart problems including failure
- Psoriasis
Also Check: How Do I Get Rid Of A Stomach Ulcer
How Can I Make My Treatment Plan More Effective
You play a key role in the treatment of your disease. By taking the right steps, you can ensure the greatest chance of achievingand stayingin remission:
- Always take your medication exactly as prescribed.
- Talk with your doctor about any side effects you experience.
- If your treatment plan requires close monitoring, make sure you complete blood work or schedule follow-up visits as requested.
- Never stop taking your medications without talking with your doctor.
- Tell your doctor about all medications you take, including over-the-counter relievers and vitamins/minerals.
What Causes Ulcerative Colitis Flareups
When youre in remission from ulcerative colitis, youll want to do everything you can to prevent a flareup. Things that may cause a flareup include:
- Emotional stress: Get at least seven hours of sleep a night, exercise regularly and find healthy ways to relieve stress, such as meditation.
- NSAID use: For pain relief or a fever, use acetaminophen instead of NSAIDs like Motrin® and Advil®.
- Antibiotics: Let your healthcare provider know if antibiotics trigger your symptoms.
Don’t Miss: Side Effects Of Ulcerative Colitis
Are Biosimilars Effective At Treating Ibd
As noted above, biosimilars arent exact copies of the drugs theyre modeled after. When a compound has extremely large molecules that are created through a biological process, its impossible to re-create that compound exactly. If the FDA adopted such a standard for the approval of biosimilars, it would never be met.
So instead of showing that theyre identical to the original drug on a molecular level, which is required for generic drugs, manufacturers of biosimilars must prove that theyre similar enough to the originals to have no clinically meaningful difference. This is done through clinical trials for safety and effectiveness, which account for a large share of the cost of bringing a biosimilar to market.
But according to the FDAs rules, biosimilars are required to be tested for only one indication disease or health condition that the originator drug is approved for. If the drug is shown to be safe and effective for this use, the FDA extrapolates that its safe and effective for all approved uses of the originator drug.
For example, if a biologic drug is approved for treating rheumatoid arthritis, plaque psoriasis, UC, and Crohns disease, and a biosimilar version is shown to be safe and effective for rheumatoid arthritis, then the FDA will approve the biosimilar for all the other conditions as well, without testing the drug in those patient populations.
When Is Surgery For Uc Necessary
Medication is often the first treatment option. But there are cases when people with UC might require surgery.
Surgery in ulcerative colitis usually involves removal of the colon and rectum. This is called a proctocolectomy, which might include:
- Total proctocolectomy with end ileostomy: A total proctocolectomy is when the anus is surgically removed in addition to the colon and rectum. An ileostomy is a surgical procedure that creates a hole in the abdomen through which solid waste is emptied into a pouch.
- Proctocolectomy with ileal pouch-anal anastomosis : In this procedure, the colon and the rectum are removed, but the anus and anal sphincter muscles are preserved. The ileum is fashioned into a J-, S-, or W-shaped pouch. This eliminates the need to wear a permanent external bag.
Its important to keep in mind that UC can still cause symptoms after surgeryso it’s essential to continue to work with your doctor to keep up with the management of your disease. If you have treatment that works for you, its possible to achieve remission without surgery.
When it comes to people with ulcerative colitis, in a given year:
of people with ulcerative colitis have symptoms under control
experience mild disease activity
experience moderate disease activity
experience severe disease
The longer a person with UC maintains symptom control, the less likely he or she is to experience a relapse, or flare-up, in the following year.
Don’t Miss: New Meds For Ulcerative Colitis
What Are The Symptoms Of Ulcerative Colitis
Ulcerative colitis symptoms often get worse over time. In the beginning, you may notice:
- Diarrhea or urgent bowel movements.
- Abdominal cramping.
- Liver disease.
- Loss of fluids and nutrients.
Symptoms are similar in pediatric ulcerative colitis and may also include delayed or poor growth. Some ulcerative colitis symptoms in children can mimic other conditions, so it is important to report all symptoms to your pediatrician.
Related Resources For Ulcerative Colitis

* Prescription savings vary by prescription and by pharmacy, and may reach up to 80% off cash price.
Pharmacy names, logos, brands, and other trademarks are the property of their respective owners.
This article is not medical advice. It is intended for general informational purposes and is not meant to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. If you think you may have a medical emergency, immediately call your physician or dial 911.
Also Check: Over The Counter Medication For Ulcerative Colitis
My Doctor Prescribed 5
Aminosalicylates are a type of drug that contains 5-aminosalicylic acid . Common examples include sulfasalazine and mesalamine. They are often prescribed to people with mild to moderate UC as a first line of therapy. They may also be used to help people maintain remission.
Aminosalicylates decrease inflammation in the lining of the gastrointestinal tract. They are prescribed in topical or oral forms and relieve symptoms for many people. In fact, research shows that if taken as prescribed, they can control UC symptoms in up to 80 percent of people.
Common side effects include , joint pain, nausea, and .
Acute Severe Ulcerative Colitis
Patients with acute severe ulcerative colitis, defined as six or more bloody bowel movements per day and at least one of the following: pulse rate > 90 beats per min, temperature > 37.8°C, haemoglobin count < 10.5 g/dL, or ESR > 30 mm/h, should be admitted to a tertiary care centre. Acute severe ulcerative colitis is associated with significant morbidity and mortality of approximately 1%. Patients are initially treated with intravenous corticosteroids to which approximately 65% will respond. For patients not responding to intravenous corticosteroids within 3 to 5 days, rescue medical therapy with either ciclosporin or infliximab can be attempted. Both drugs are equally efficacious in acute severe ulcerative colitis., Delays in surgery can increase postoperative complications and mortality increases significantly after 7 days., If there is no response to one of these drugs, colectomy should be performed. Further discussion of acute severe ulcerative colitis is in the .
Also Check: Diet For Gerd And Ulcers
Ulcerative Colitis Treatment Options
Treatment of ulcerative colitis focuses on one of two goals: inducing remission during an active flare-up or maintaining remission. These goals are largely accomplished through medications that will be tailored to the severity and extent of the illness. Severe disease or complications may require surgical removal of part or all of the colon.
Lifestyle Changes For Ulcerative Colitis
Its also important to control stress, as it can worsen UC symptoms and may trigger ulcerative colitis flare-ups. Exercise, meditation, yoga and biofeedback, a stress-reduction technique designed to reduce muscle tension and slow heart rate via a feedback machine, are often recommended to help ulcerative colitis patients reduce stress levels.
You May Like: Ulcerative Colitis And Colon Cancer Statistics
Ulcerative Colitis Treatment: All You Need To Know
Elizabeth Oliver, PhD
Ulcerative colitis is an inflammatory bowel disease. It causes inflammation and ulcers in the inner lining of the large intestine . Ulcerative colitis is a chronic condition. The goal of treatment is to reduce the inflammation that causes symptoms in order to prevent flare-ups and maintain longer periods of remission.
Treatment options for ulcerative colitis usually include either medication or surgery, as well as a focus on diet and nutrition. Because the symptoms of ulcerative colitis vary from person to person there is no single treatment that works for everyone.