Herbal And Alternative Treatments
Cannabis research increasingly points to benefits for a range of chronic health conditions, but there is minimal evidence specific to ulcerative colitis at this time. Studies so far suggest the potential of cannabis to improve the quality of life for people with UC, likely due to its anti-inflammatory and antioxidant effects. More investigation is needed before recommendations can be made.
Other studies show that, compared to placebo, the treatments of aloe vera gel, wheatgrass juice, andrographis paniculata extract, and topical Xilei-san may all help alleviate UC symptoms. Before experimenting with any alternative treatments, you should always consult with your health care provider.
Talk With Others Who Understand
MyCrohnsAndColitisTeam is the social network for people with ulcerative colitis and their loved ones. On MyCrohnsAndColitisTeam, more than 138,000 members come together to ask questions, give advice, and share their stories with others who understand life with ulcerative colitis.
Are you living with ulcerative colitis pain? What has helped you to manage it? Share your experience in the comments below, or start a conversation by posting on your Activities page.
Where Does Ulcerative Colitis Pain Come From
Ulcerative colitis can be an unpredictable condition as the cause of it has yet to be uncovered. The illness is also associated with flare-ups, which can have unique triggers. Approximately 30% of people who are currently in remission will relapse in the next year.
It is believed that there is a genetic component that comes into play with this condition. Those with family members with ulcerative colitis are more likely to be afflicted by this condition. This disease can generally be found in any age group, but it is far more prevalent between the ages of 15 to 30, as well as 50 to 70. It is also believed that Caucasians are much more likely to develop this condition and the risk is even higher for those of Ashkenazi Jewish decent.
At one time, it was believed that ulcerative colitis was caused by stress and diet. Today, researchers believe these can be a trigger, but they no longer think it is a direct cause. Most studies are focused on searching the immune systems for a root cause for this condition. It is thought that the immune system might inadvertently attack the healthy cells in the GI tract when trying to fight off foreign invaders, which causes inflammation.
You May Like: Can Ulcerative Colitis Cause Body Aches
How Does The Severity Of Your Ulcerative Colitis Affect Treatment
Thereâs no cure for ulcerative colitis. But treatments can help ease your symptoms, inflammation, and treat underlying conditions. With any form of ulcerative colitis, the goal is to go into remission and stay there. Certain medications work well to ease mild-to-moderate symptoms. There are also treatment options for more severe ulcerative colitis.
To improve your quality of life, your doctor may suggest:
Aminosalicylates. If you have mild to moderate ulcerative colitis, sulfasalazine may help your symptoms. Make sure to let your doctor know if youâre allergic to sulfa. If you are, they can give you alternatives.
Youâll take these drugs in capsule form through your mouth. They also come in a rectal form , which means youâll put it in your bottom.
Corticosteroids. For severe cases of ulcerative colitis, your doctor might suggest prednisone or budesonide . These drugs have serious side effects though. Your health care team will only suggest them for short-term use. Theyâll give you other drugs to help keep you in remission.
You can take these medications through your mouth, bottom, or through an injection.
Biologics. These are good options for moderate to severe ulcerative colitis. They target parts of your immune system to ease symptoms. Some you might try are adalimumab , certolizumab pegol , golimumab , or others.
Your doctor will give these to you through an IV. You may be able to give yourself these medications if your doctor allows you to do so.
Show Sources
What To Look For When You Have Ulcerative Colitis Pain
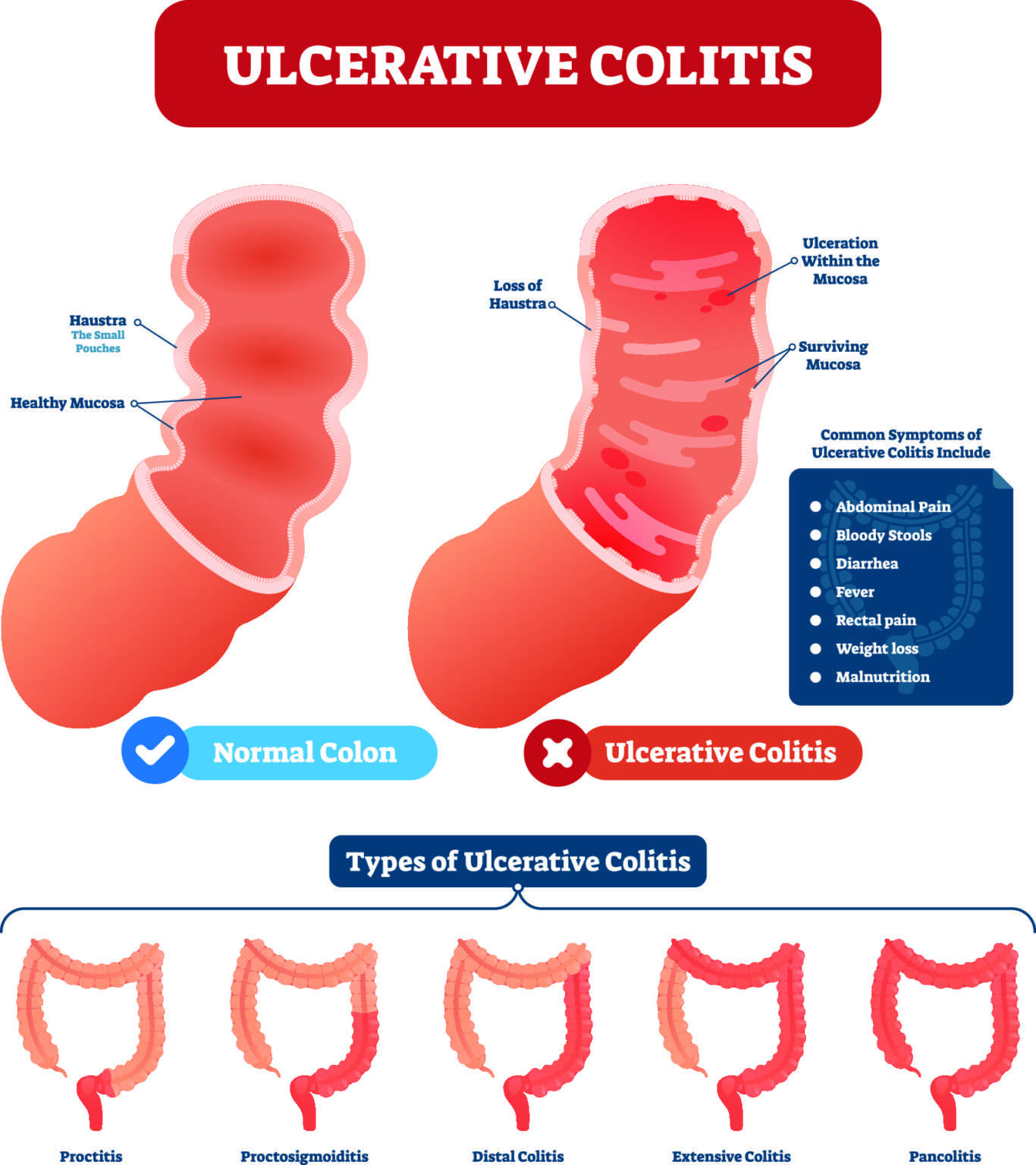
Attacks from this condition vary greatly depending on the person, so it is important to know what a flare-up is to you. It can also affected by the severity of the inflammation as well as where in the large intestine it is.
Ulcerative colitis symptoms can be anywhere from mild to severe. They can slowly build or come on suddenly without warning. It is important to monitor this condition periodically as it can get worse over time even with treatment.
Some of the most common symptoms of ulcerative colitis are:
- Blood or pus in stool
- Fever
- Weight loss
- Frequent, uncontrollable bowel movements
There are other difficulties that can happen with this chronic condition. Some of these complications include rupture of the bowel, profuse bleeding, vitamin and mineral deficiencies, severe dehydration, and inflammation of the skin, joints, and eyes. The risk of colon cancer increases as well as the possibility for blood clots in veins and arteries.
Also Check: Is Smoking Good For Ulcerative Colitis
And Be Proactive About Probiotics
Youve probably heard about probiotics. Theyre the living microorganisms that help keep the healthful bacteria flourishing in your digestive tracthome to the largest part of your immune system. Your favorite yogurt is loaded with probiotics . According to one 2019 study, more than half of those who regularly consumed probiotics saw improvements in their general quality of life and in specific UC symptoms, including more regular bowel movements.
Deal With Iron Deficiencies Too
UCs painful, even gut-wrenching symptoms dont always make it fun to eat. And, people with this chronic condition may lose blood in their stool, as well as absorb dietary iron poorly due to inflammation, according to the Cleveland Clinic. Additionally, foods rich in iron, like red meat, often trigger flareups. Together, this can cause anemia, a condition characterized by a low red blood cell count. Its a common issue with the UC communityand must be controlled to battle fatigue. If you have UC and super-low energy, talk to your doctor about iron supplements.
You May Like: What To Eat With Gastric Ulcer
How To Manage Ulcerative Colitis Pain
Learning effective pain management strategies is a crucial aspect of living well with ulcerative colitis , a form of inflammatory bowel disease . Flare-ups can happen, even if you carefully manage your condition. Swelling of the intestine may cause bloating and painful cramping. You may experience bleeding due to skin irritation from persistent diarrhea.
During a flare-up, it’s not unusual to feel unwell all over. Fatigue, nausea, fever, and anxiety are common symptoms with UC. Progression of the disease can produce joint pain, skin rashes, mouth sores, and even make your eyes hurt.
UC pain can significantly impact quality of life. One MyCrohnsAndColitisTeam member wrote, Pain in my gut . So tired of being in pain. Another member posted, Woke up with the worst back pain I could ever imagine. I was in tears.
Fortunately, it’s possible to manage the pain associated with UC using a combination of at-home remedies, medical interventions, lifestyle changes, and alternative treatments.
Symptoms Of Ulcerative Proctitis
The presenting symptoms of ulcerative proctitis all relate to the rectum. Blood in the stool occurs in almost everyone with the disease. Diarrhea is a common symptom, although constipation can also develop as the body struggles to maintain normal bowel function.
Inflammation of the rectum may cause a sense of urgency to have a bowel movement, discomfort after having a bowel movement, and a sensation of incomplete emptying of the bowels. Systemic symptoms such as fever, tiredness, nausea, and weight loss are rare.
Ulcerative proctitis has very few complications but with increased irritation to the anal and rectal area, hemorrhoids may occur. Only rarely do other complications occur, such as abscesses and extra-intestinal manifestations. Individuals with ulcerative proctitis are not at any greater risk for developing colorectal cancer than those without the disease.
Recommended Reading: Best Anti Diarrhea Medicine For Ulcerative Colitis
Don’t Miss: Can I Take Imodium If I Have Ulcerative Colitis
What Kinds Of Pain Relievers Can Be Used By People With Ibd
The most common type of over-the-counter pain relievers are called NSAIDs , such as ibuprofen , aspirin, or naproxen. These medications are generally not recommended for people with inflammatory bowel disease because of the side effects that they can cause in the digestive tract. This means that taking NSAIDs for pain relief can cause the symptoms of IBD to get worse or trigger IBD flare-ups that can cause further damage to the digestive tract.1,2
Patients with IBD should consult their healthcare providers before taking any NSAID medications. In some cases, NSAIDs may be recommended for treating pain due to arthritis, but patients will be monitored closely for side effects. Instead of NSAIDs, people with IBD may be advised to try acetaminophen for pain relief.1,2
Opiates are a very strong type of medication that can be used to treat severe pain. They include morphine, hydrocodone with acetaminophen , oxycodone with acetaminophen , and codeine. While they can be very effective at treating severe pain in the short term, if they are taken long-term, opiates can cause serious side effects and can make a person physically dependent on them. For this reason, they should be taken only under close supervision from a healthcare provider.1,2
What Causes Ulcerative Colitis Plus How To Treat It
- Ulcerative colitis is a type of inflammatory bowel disease that develops when your colon or rectum become inflamed.
- UC affects about 900,000 individuals in the U.S.
- The exact cause of ulcerative colitis is complex but experts believe it could be caused by an overactive immune system.
- Even though there is no cure, there are treatment options available that can help you manage the disease.
Do you need to take frequent trips to the bathroom? Perhaps youre suddenly feeling overly tired every day or experiencing unusual abdominal pain or cramping. If thats the case, you might be suffering from a type of inflammatory bowel disease known as ulcerative colitis.
Related Topics :
Roughly 900,000 individuals are living with ulcerative colitis in the United States. And while it often develops between the ages of 15 and 30, anyone can develop it at any age. Theres a lot more to know about it too. So, lets take a look at what ulcerative colitis is, what causes it, the signs to look out for, plus how to treat it.
You May Like: Psc Liver Disease Ulcerative Colitis
Knowing The Symptoms Of Ulcerative Colitis
Approximately 750,000 people in the US are living with ulcerative colitis. While relatively less common than other bowel diseases, you probably cant go very long without seeing an ad for medications that are designed to treat symptoms of UC. Perhaps you see these ads and realize that the symptoms they are talking about are ones you experience. Could you have ulcerative colitis? Fortunately, your gastroenterologist will be able to shed light on this issue.
Recommended Reading: Best Supplement For Gastric Ulcers In Horses
How Often Do I Need A Colonoscopy
Especially when you have symptoms or are just starting or changing medications, your doctor may want to periodically look at the inside of the rectum and colon to make sure the treatments are working and the lining is healing. How often this is needed is different for each person.
Ulcerative colitis also increases your chance of developing colon cancer. To look for early cancer signs, your healthcare provider may have you come in for a colonoscopy every one to three years.
Recommended Reading: Ulcerative Pancolitis With Rectal Bleeding
Five Tips For Dealing With Ulcerative Colitis Pain
There are ways to combat the pain that comes along with ulcerative colitis flare-ups. However, it is always best to get treatment from a doctor as they are most likely to efficiently and safely resolve your symptoms.
Here are five strategies you can use to help relieve symptoms and avoid a flare-up in the first place.
You May Like: How To Lose Weight With Stomach Ulcers
Work With Your Doctor
Youâll need to see your doctor regularly. It may be every 6 months while youâre in remission. Youâll have routine procedures like colonoscopies and bloodwork to check on your UC.
If youâre having a flare-up, make sure to check in with your doctor. UC isnât the only thing that causes digestive symptoms. They may need tests to rule out something else, like an infection. Or you may need your prescriptions adjusted.
Certain symptoms mean you need help right away. Call your doctor if you:
- Canât keep liquids down
- Have severe diarrhea
- Have a fever
Don’t Miss: Is Ulcerative Colitis A Gastrointestinal Disease
How Can People With Ibd Manage Their Pain
The first step in developing a pain management approach for a patient with IBD is to determine what is causing the pain. If active IBD is causing the pain, then the first strategy is generally for healthcare providers to change or increase the medication that the patient is taking to manage the disease, such as aminosalicylates, corticosteroids, antibiotics, immunosupressants, or biologics. In many cases, treating the disease and its symptoms can be effective in reducing pain.1
However, some people may continue to experience pain despite the change in medication, or they may have pain that is not due to active IBD but some other cause. In those cases, healthcare providers may recommend trying some kind of pain relievers.
What Should I Ask My Doctor
If you have ulcerative colitis, you may want to ask your healthcare provider:
- How much of my large intestine is affected?
- What risks or side effects can I expect from the medication?
- Should I change my diet?
- Will ulcerative colitis affect my ability to get pregnant?
- What can I do at home to manage my symptoms?
- What are my surgical options?
Don’t Miss: How To Cure Skin Ulcer
Complementary And Alternative Remedies
Alternative treatments such as acupuncture may help to reduce and regulate bowel inflammation, reducing UC pain.
Another form of alternative treatment called moxibustion may also have a positive effect on UC symptoms. Moxibustion is a type of heat therapy. It uses dried plant materials burned in a tube to warm the skin, often in the same areas targeted by acupuncture.
Get Regular Exercise To Reduce Uc Inflammation
Snider says exercise is useful in managing many of the complications associated with ulcerative colitis, including decreased bone density, a weakened immune system, emotional health problems, stress, and weight gain.
“Try to engage in a moderate-intensity exercise like swimming or biking, three or four days per week,” he says. A review published in August 2016 in Pharmacological Reports noted that moderate exercise releases protective myokines such as irisin from working skeletal muscles, which promotes healing and helps with inflammatory bowel disease inflammation.
Snider also strongly recommends yoga as a natural treatment for ulcerative colitis, as it promotes relaxation and targets the digestive system, flooding the area with oxygen and nutrition for healing. Find what type and frequency of exercise works for you and take it slow: Too much exercise can cause mild systemic inflammation.
Research indicates that stress plays a role in inflammatory bowel diseases such as ulcerative colitis. Researchers analyzed data on 2,007 adults in a Swiss IBD study and found a relationship between depression and anxiety and disease symptoms. The results were published in June 2016 in Clinical Gastroenterology and Hepatology.
Counteract stress with relaxation techniques such as meditation, deep breathing, and progressive muscle relaxation to help your body relax.
You May Like: Stelara Indications For Ulcerative Colitis
How To Define Ulcerative Colitis Pain
To help your doctor figure out whats causing your abdominal pain and other symptoms, you need to be able to accurately describe the sensation. Before seeing your doctor, take stock of what youre feeling. It may be useful to keep a colitis symptom journal to write down what you are experiencing. Be ready to describe:
- How long youve had your pain
- Where you feel your pain
- How it feels, both in sensation and intensity
- The frequency and duration of your pain
- What seems to trigger your abdominal pain
- What seems to help ease the pain
- What time each pain occurred, including how long after eating, and how long it lasted
The more specific you can be about your pain, the better, Dr. Kane says.
Signs And Symptoms Of Ulcerative Colitis
The symptoms of ulcerative colitis can vary for each individual and they can even change over time. That said, some of the common early signs and symptoms to be on the lookout for include abdominal pain, diarrhea, an urgency to defecate, fatigue, nausea, weight loss, and anemia.
Over time, other symptoms can develop too. The Cleveland Clinic says this may include severe cramping, bloody stools, mucus or pus in the stool, fever, skin problems, mouth sores, joint pain, eye inflammation, loss of fluids and nutrients, and liver disease.
Children who develop ulcerative colitis can develop similar symptoms to adults but a symptom unique to them is delayed or poor growth. Symptoms can mimic other conditions, so its always important to have your child checked by their pediatrician for a proper diagnosis.
Recommended Reading: What’s The Signs Of An Ulcer
Treatments For Ulcerative Colitis
Treatments for ulcerative colitis wont cure the condition, but it can help to regulate the immune system and manage symptoms. Patients may use one type of treatment or a combination of them depending on their unique condition.
Certain medications can treat inflammation and symptoms such as diarrhea, bleeding, and abdominal pain. Medication may also be prescribed to lower the frequency of flare-ups. Alongside medication, it can be helpful for patients to alter their diet and nutrition.
Experts have found that certain foods can aggravate symptoms in UC patients. This includes spicy, high-fibers, or dairy foods. Instead, eating a healthy diet that involves softer and blander food can cause less discomfort.
In some cases, medicine and diet changes arent enough to treat UC. Surgery may be required to remove the colon and rectum completely with the creation of an ileostomy or external stoma. The type of surgical procedure for UC will greatly depend on the patients age, overall health, and symptoms.