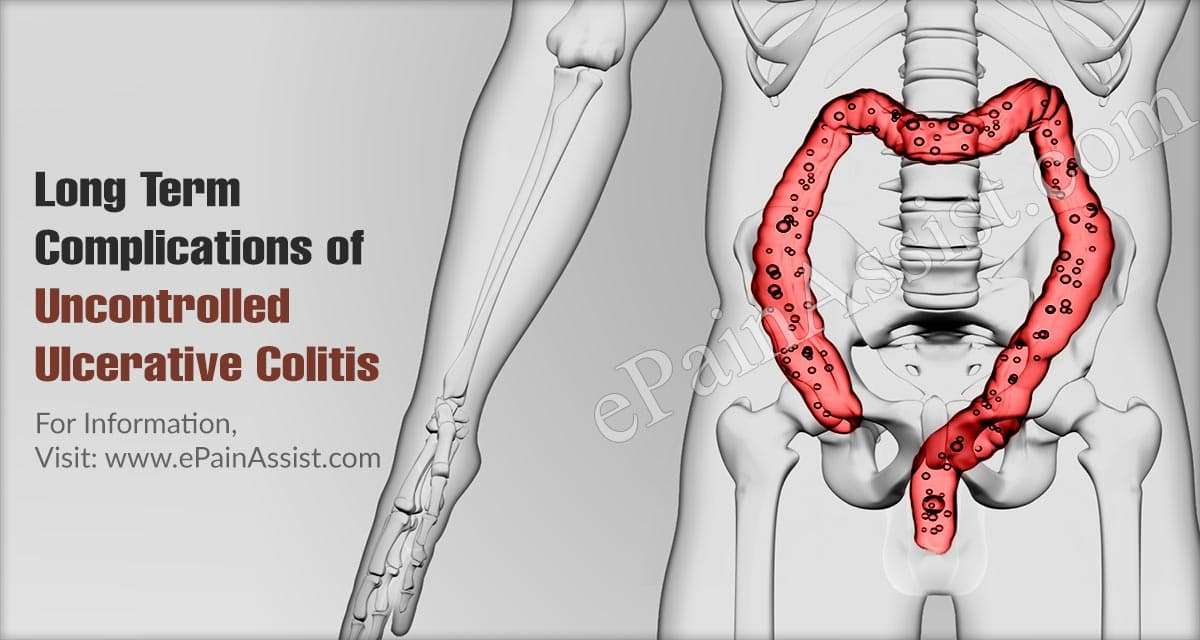
The Link Between Ulcerative Colitis And Joint Pain
UC is a type of inflammatory bowel disease . Arthritis is the most common non-GI complication of IBD. The reason for the link may lie in genes that make people with IBD more susceptible to arthritis.
Two types of conditions can affect the joints of people with UC. Arthritis is joint pain with inflammation . Arthralgia is pain in the joints without any inflammation.
Arthritis that occurs with UC is a bit different than regular arthritis. For one thing, it typically starts at a younger age.
In addition, arthritis in people with UC doesnt usually cause long-term joint damage. The joints swell up and become painful, but they return to normal once intestinal inflammation is under control.
A few types of arthritis can affect people with UC:
What Can I Expect If I Have A Diagnosis Of Ulcerative Colitis
Ulcerative colitis is a lifelong condition that can have mild to severe symptoms. For most people, the symptoms come and go. Some people have just one episode and recover. A few others develop a nonstop form that rapidly advances. In up to 30% of people, the disease spreads from the rectum to the colon. When both the rectum and colon are affected, ulcerative symptoms can be worse and happen more often.
You may be able to manage the disease with medications. But surgery to remove your colon and rectum is the only cure. About 30% of people with ulcerative colitis need surgery.
Reducing Your Arthritis Risk When You Have Ulcerative Colitis
Arthritis is the most common complication outside the gut for people with ulcerative colitis. These dos and donts will help you protect your joints.
As if gut pain from ulcerative colitis weren’t enough, as many as 30 percent of people with an inflammatory bowel disease , including ulcerative colitis, will develop problems with their joints, according to the Crohns and Colitis Foundation. Indeed, arthritis is the most common complication that occurs beyond the intestines.
Although it’s not fully understood, there seems to be a link between the gut and joints, says Harry D. Fischer, MD, the chief of rheumatology at Lenox Hill Hospital in New York City. For example, a bacterial infection in the digestive tract can cause a reactive type of arthritis, he notes. In addition, both arthritis and ulcerative colitis have a genetic component.
According to the Crohns and Colitis Foundation, people with ulcerative colitis tend to have one of three forms of arthritis:
- Peripheral arthritis , which affects large joints such as the knees, ankles, elbows, or wrists when IBD is properly treated and controlled, PA joint pain and symptoms typically improve
- Axial arthritis, which causes pain and stiffness in the spine and lower back
- Ankylosing spondylitis, a more severe type of arthritis that affects the spine and can lead to joint damage. Its an uncommon complication that affects between 2 and 3 percent of people with IBD.
Also Check: Signs And Symptoms Of Peptic Ulcer
Your Mental And Emotional Health Are Just As Important As Your Physical Health
People living with ulcerative colitis can absolutely lead a full life. But when the disease is active, its understandable that, because of UC-flare-ups or complications, there can be an impact on a persons quality of life. It can be difficult to cope with a serious and chronic illness. Some patients react to the unpredictable or severe nature of their symptoms. Those feelings can include:
Anger
Questions To Ask Your Doctor
- How will my inflammatory bowel disease be treated?
- Will I need surgery? Are there other options?
- What lifestyle changes can I make to help inflammatory bowel disease?
- What are some medicines used to treat inflammatory bowel disease and what are the possible side effects?
- Are my children at risk of inflammatory bowel disease?
You May Like: What To Do For Ulcer Pain
Inflammatory Bowel Disease Treatment Options
IBD is a lifelong disease, and at this point, people are rarely cured. However, thanks to advances in medication, gastroenterologists at CHI Health can help patients keep their condition in check and live an active, pain-free lifestyle.
The most common medications we prescribe include:
- Aminosalicylates: These treat mild to moderate Crohn’s disease by controlling inflammation in the lining of the gastrointestinal tract.
- Antibiotics: These treat symptoms and help heal infections.
- Biologics: These drugs treat people with moderate to severe disease, often if other drugs have not worked well. They don’t affect your whole immune system, so they tend to cause fewer side effects, although some side effects can be serious.
- Corticosteroids: These strong and fast-acting drugs can often relieve flares in moderate to severe Crohn’s within a few days. You usually take them in small doses for a short time because they can cause serious side effects.
- Immunomodulators: If you have moderate to severe Crohn’s, and you have not had luck with aminosalicylates or corticosteroids, your doctor may suggest one of these. They can help your body respond better to corticosteroids during a flare and help you stay flare-free longer.
Continuous Signs And Symptoms
Ulcerative colitis can cause signs and symptoms such as diarrhea, blood in the stool, nausea, fatigue, and abdominal pain. One of the goals of treatment is to stay on top of the inflammation that may contribute to these symptoms.
The symptoms of ulcerative colitis can lower a persons quality of life significantly, as well as affect personal relationships and the ability to have a rewarding and successful career. While it does take time and effort to develop a treatment plan, the result can be the cessation of the symptoms and an improvement in quality of life.
You May Like: Icd 10 Venous Stasis Ulcer Left Leg
Faqs About Ulcerative Colitis
What is ulcerative colitis?
Ulcerative colitis is an inflammatory bowel disease of unknown cause in which the gastrointestinal tract is unable to distinguish foreign from self-antigens. It is characterized by chronic inflammation of the colonic mucosa and submucosa, atrophy and possibly dysplasia limited to the colon. The extent of disease varies and may involve only the rectum , the left side of the colon to the splenic flexure or the entire colon .
What causes ulcerative colitis?
Hereditary factors seem to play a role in the etiology of ulcerative colitis. The most significant risk factor for the development of ulcerative colitis is a family history. Environmental factors are also involved, as evidenced by higher rates of this disease in urban locales.
What are the symptoms of ulcerative colitis?
The most common symptom of ulcerative colitis is diarrhea that is often bloody. Other symptoms include abdominal and/or rectal pain, fever and weight loss. Some patients complain of constipation and rectal spasm. Arthritis symptoms may occur in as many as 26 percent of patients with ulcerative colitis, dermatological changes in fewer patients and ocular manifestations in about 5 percent.
How is ulcerative colitis diagnosed?
Who is affected by ulcerative colitis?
Is there a relationship between smoking cigarettes and developing UC?
What is the treatment for ulcerative colitis?
Will I eventually need to have surgery for ulcerative colitis?
What is pouchitis?
Request an Appointment
Continue Learning About Ulcerative Colitis
Important: This content reflects information from various individuals and organizations and may offer alternative or opposing points of view. It should not be used for medical advice, diagnosis or treatment. As always, you should consult with your healthcare provider about your specific health needs.
Recommended Reading: Home Remedies For Intestinal Ulcers
Axial Arthritis And Ulcerative Colitis
Although more common in people with Crohns disease, axial arthritis can also affect those with UC. Over time, axial arthritis causes pain and stiffness in the lower spine and sacroiliac joints, which connect the lower spine and pelvis.
The main symptoms of axial arthritis are stiffness and pain in the lower back, hips, and buttocks that persist for three or more months at a time. Flare-ups typically come on slowly, gradually worsening over a period of several weeks or months. Symptoms tend to be at their worst in the morning and wear off with time and exercise. Prolonged rest or inactivity can make joint pain worse.
I can’t bend or twist like I used to, wrote one MyCrohnsAndColitisTeam member. It hurts too bad. Being up and about helps, but getting up for those first few steps after sitting a while is so painful, and I can’t fully stand upright sometimes for a minute or so. It’s frustrating.
Does Ulcerative Colitis Make You Immunocompromised
Ulcerative colitis doesnt make you immunocompromised. Some of the medicines that treat it may change the way your immune system responds. This change is different for each medication. Some of these changes may increase the risk of certain infections or other issues. A discussion with your health care team before starting a medication is the best way to understand these risks and ways to prevent them.
Recommended Reading: Best Foods To Eat If You Have An Ulcer
Ways To Reduce Complications
Early intervention and frequent surveillance of ailments is key to reducing complications and improving outcomes. It’s important to maintain proper nutrition and avoid emotional stress, though neither stress nor sensitivity to certain foods causes the disease. Avoiding steroids can also be helpful if you and your doctor have an alternative way of treating UC flares.
While the cure for UC has yet to be found, when the disease is treated properly, some complications may disappear altogether. Work with your doctor and other members of your healthcare team to get optimal control of the disease as soon as possible.
Additional reporting by Jordan M. Davidson.
Can I Treat Ibd If I Am Pregnant Or Breastfeeding
Yes, but your doctor may change the type or amount of the medicine you take. Some medicines, such as methotrexate and thalidomide, cause birth defects and other health problems and should not be taken while you are pregnant or breastfeeding.31
Before you get pregnant, make a plan with your obstetrician and gastroenterologist about the medicines you will take during and after pregnancy. Take your medicines as your doctor tells you to. If you stop taking your medicines and your symptoms come back , it may be difficult to get them back under control.31
Talk with your doctor about your medicines and breastfeeding before you give birth. You can search for your medicine in the LactMed database to find out if your medicine passes through your breastmilk and, if so, if it has any possible side effects for your nursing baby.
Also Check: How Do You Stop A Stomach Ulcer From Hurting
Back Pain And Ulcerative Colitis
Research indicates that nearly 25 percent of people with inflammatory bowel disease including ulcerative colitis and Crohns disease experience chronic lower back pain. Ankylosing spondylitis and axial arthritis both of which can cause back pain are two common causes of back pain in people with UC.
That said, a doctor may not suspect that a person with back pain has UC unless they also experience gastrointestinal symptoms. If you do experience back pain, its important to let your doctor know even if you dont suspect that its related to UC. They will be able to determine the cause of your pain and work with you to find the best way of managing it.
Ulcerative Colitis Symptoms You Should Never Ignore
Ulcerative colitis is an autoimmune disease in which the immune system attacks the colon and causes a range of symptoms, both in the GI tract and around the body.
Symptoms of ulcerative colitis, a type of inflammatory bowel disease , can vary widely depending on how much inflammation a person has and where the inflammation is located.
Abdominal pain and bloody diarrhea are the most common warning signs of UC, and can range from mild and intermittent to severe and chronic. The pain of UC is quite common and can significantly impact quality of life. Ulcerative colitis symptoms tend to come and go, often with extended periods of time in between flares. These are called remission periods.
The disease tends to develop gradually over time, so you might not automatically think of ulcerative colitis or IBD if you have occasional abdominal pain or digestive distress.
Ongoing inflammation along with ulcers and abscesses in the intestines are additional common causes of pain. Scarring in the lining of the intestinal tract can lead to painful obstructions. Pain may occur in different areas such as the abdomen or rectal area, depending where the inflammation is located. For example, people may experience moderate to severe pain on the left side of the abdomen if the UC affects the rectum and the lower segment of colon.
UC symptoms might ebb and flow, but they wont go away unless you see a gastroenterologist and start treatment.
Recommended Reading: Can Ulcerative Colitis Cause Blood In Urine
Signs And Symptoms Of Ulcerative Colitis
Recognizing the symptoms of ulcerative colitis is your first step toward knowing when your disease is in a flare and when to seek medical attention.
The symptoms of ulcerative colitis vary from person to person and about half of all ulcerative colitis patients experience mild symptoms. If you experience any of these symptoms, consult your healthcare provider.
-
Loose and urgent bowel movements
-
Bloody stool
-
Persistent diarrhea accompanied by abdominal pain and blood in the stool
Research And New Developments
Previous research has shown that ankylosing spondylitis has a strong genetic component and were currently funding several research projects to further understand this. Previously, we part funded research that identified a specific gene, called IL23R, thats linked to the condition. Were now funding a follow-on project to investigate how changes in this gene lead to the development of ankylosing spondylitis.
Were also supporting a study thats investigating a gene called RUNX3. Researchers are investigating whether this molecule can be targeted with drugs. Results from this research may lead to the development of new and more effective drug treatments.
Were funding a project investigating the protein HLA-B27. This protein is found in over 90% of people with ankylosing spondylitis. Its thought that HLA-B27 proteins tend to fold incorrectly inside cells, which may lead to the immune system releasing chemicals that cause inflammation. This research aims to generate HLA-B27 specific treatments that overcome the problems associated with current treatment options.
Don’t Miss: Herbal Medicine For Stomach Ulcer
Etiology Of Ulcerative Colitis
The exact cause of ulcerative colitis is unknown. The most accepted theory about its etiology is that ulcerative colitis is an autoimmune disorder. Also, genetic and environmental factors play a role.
Unlike Crohns disease, smoking doesnt represent a risk factor in ulcerative colitis. The incidence of ulcerative colitis is lower among smokers 80% of the patients are nonsmokers.
Page 2 of 18
Recommended Reading: Advil Or Ibuprofen For Back Pain
Stay Strong Ulcerative Colitis And Lower Back Pain
As soon as your lower neck and back pain has actually declined, you can aid avoid future episodes of pain in the back by functioning the muscular tissues that support your lower back, consisting of the back extensor muscles. They aid you keep the appropriate posture as well as alignment of your spine. Having solid hip, pelvic, and abdominal muscles additionally provides you extra back support. Avoid stomach crunches, because they can really put even more stress on your back.
Read Also: How Do They Treat Ulcerative Colitis
Painful And Strenuous Defecation
With colitis, dogs will strain while passing stool. This will cause pain. These are usually displayed when the dog squats to defecate. It will do so with a sense of urgency and display signs of discomfort and pain, unlike times when it is okay.
Flatulence, pronounced squatting and hunching, weight loss and disinterest in food are additional symptoms.
Ulcerative colitis can make life hard to predict. A flare-up of symptoms is stressful and can leave you worn out for days, weeks, or even months. Even in remission, you might get tired a lot or have a hard time meeting friends or going to work. Itâs easy to see why living with this long-term inflammatory disease can affect your mental health.
Theres no evidence that stress actually causes inflammatory bowel disease , which includes UC and Crohnâs disease. But stress can definitely bring on a flare-up. And youre more likely to feel anxious and depressed than your friends without UC. Your chances are even higher if you are a woman. Even rats with IBD in lab studies show signs of mood problems.
But there are steps you can take to lift your mood, even when your symptoms get you down.
Complications Caused By Nutritional Deficiencies
Some of the complications of malnutrition include:
- Dehydration diarrhoea causes your body to lose fluid, which can lead to dehydration. Severe dehydration can damage your kidneys.
- Anaemia reduced iron in the diet combined with losing blood from the bowel can lead to anaemia .
- Weight loss reduced appetite and poor absorption of food nutrients can cause weight loss.
- Reduced growth inadequate nutrition during childhood and adolescence can impair a childs growth and physical development.
You May Like: Remicade Infusion For Ulcerative Colitis
Don’t Miss: Where Is Stomach Ulcer Pain
What Are The Complications Of Ulcerative Colitis
UC can also lead to complications, especially if left untreated or if you dont follow the directions for your medications to a T . Common complications of UC include:
-
Rectal bleeding, which can lead to iron-deficiency anemia
-
A rupture of the bowel
-
Increased risk of colon cancer
-
Deficiencies in vitamins and minerals, which can lead to bone loss in the form of osteopenia or osteoporosis
-
Inflammation throughout the body, such as the eyes, skin, and joints
If youve had surgery for UC, keep in mind there may be surgical complications as well. Talk with your doctor about any warning signs to watch for.