How Can I Tell If I Have Ulcerative Colitis Or Crohns Disease
Its important that you, your healthcare provider, and a GI specialist work together closely to figure out whats causing your symptoms. This is especially important since the symptoms of Crohns disease and ulcerative colitis can be similar. Your providers may check blood work and a stool sample. To get an accurate diagnosis, your GI specialist may do a colonoscopy, where a camera is pushed into the colon. Your provider will look at the inside of the colon and take tissue samples, which are important for making the right diagnosis. Your providers might get a CT scan or an MRI of your abdomen to check for complications related to your condition.
Diagnosis Of Ulcerative Colitis And Crohns Disease
The right diagnosis is important as both diseases have similar symptoms. Different ways for doctors to diagnose it correctly include:
- X-rays or Contrast X-rays that show which parts of the intestine have been affected
- CT scans and MRIs to ensure its inflammatory bowel disease and rule out other diseases with similar symptoms
- Endoscopy, a procedure in which a tiny camera is inserted into your digestive system to get a clear look
- Scientists are also trying to improve several blood tests to make it better at diagnosing Ulcerative Colitis and Crohns Disease
Complications Caused By Nutritional Deficiencies
Some of the complications of malnutrition include:
- Dehydration diarrhoea causes your body to lose fluid, which can lead to dehydration. Severe dehydration can damage your kidneys.
- Anaemia reduced iron in the diet combined with losing blood from the bowel can lead to anaemia .
- Weight loss reduced appetite and poor absorption of food nutrients can cause weight loss.
- Reduced growth inadequate nutrition during childhood and adolescence can impair a childs growth and physical development.
Don’t Miss: Ulcerative Colitis And Liver Function Tests
Inflammation In Other Areas
Some people with IBD have painful inflammation in other areas of the body, including:
- joints of the fingers, hands, feet, ankles and knees
- joints of the spine, including vertebrae and sacroiliac joints
Two specific skin problems that can occur as a result of IBD are:
- pyoderma gangrenosum small, sunken ulcers on the skin
- erythema nodosum painful, small, reddened nodules on the skin .
Smoking And Crohns Disease
The initial observation that smoking is associated with an increased risk of Crohns disease was made shortly after the link between ulcerative colitis and smoking was established,subsequent studies have shown a greater risk of Crohns disease in current smokers than non-smokers. Logan summarised the relative risk of Crohns disease in patients, relative to never smokers at diagnosis, as 2.7 for current smokers, 1.5 for ex-smokers, and 2.4 for those who had ever smoked during their life. A meta-analysis on seven suitable studies of Crohns disease confirmed a pooled odds ratio and a 95% confidence interval of 2.0 for current smokers compared with life time non-smokers, and 1.83 for former smokers compared with life time non-smokers. In this non-smoking group the risk was greatest for those who had quit smoking within four years of developing Crohns disease, and least for those who had been non-smokers for more than 10 years. The relative risk associated with smoking for women may be greater than for men: one study demonstrated a threefold difference. The site of Crohns disease has been linked with the duration of smoking habit and number of cigarettes smoked, suggesting that small bowel and ileocolonic disease are more common in heavy smokers.
Don’t Miss: What Does A Colon Ulcer Feel Like
Pemeriksaan Untuk Menunjang Diagnosis
Dokter dapat memeriksa sampel tinja untuk melihat tanda-tanda lendir atau darah, yang dapat mengindikasikan colitis. Sampel feses juga dapat membantu dokter menyingkirkan masalah lain, seperti patogen atau bakteri.
Standar terbaik untuk mendiagnosis penyakit inflamasi pada usus adalah melalui kolonoskopi. Pelaksanaannya menggunakan kamera kecil yang terpasang pada tabung tipis, selanjutnya dokter akan memasukkan kamera tersebut ke dalam usus besar.
Prosedur ini memungkinkan dokter untuk melihat seluruh usus besar dan melakukan biopsi. Jika dokter melihat bahwa peradangan terjadi pada rektum dan bergerak terus menerus ke atas usus besar dan kemudian berhenti, ini bisa menjadi tanda kolitis.
Berbeda dengan colitis, Crohn terkadang menciptakan kelompok sel kekebalan yang bernama granuloma. Granuloma merupakan hasil dari upaya tubuh untuk membuang bahan asing, dan sel-selnya terlihat saat menggunakan mikroskop. Dokter mungkin akan merekomendasikan pengidap untuk melakukan pemeriksaan pencitraan apabila mencurigai adanya keterlibatan usu kecil.
Tes ini termasuk CT scan dan MRI untuk mendapatkan gambaran yang lebih baik. Jika bagian dari saluran pencernaan bagian atas terlibat, misalnya lambung, dokter mungkin melakukan endoskopi bagian atas untuk menentukan letak peradangannya.
Referensi:
Does Ibs Get Worse With Age
IBS is long-term disorder of the gut and is an inevitable part of aging. It comes and goes over time. The sensitivity of the gut nerves may elevate with age and the symptoms overlap is possible. Different signs and symptoms related to IBS may show up with age. However, there are some ways like exercise, avoidance of foods that irritate the digestive system etc. that help to help reduce the overall risk of IBS and aid in reducing the symptoms.
Don’t Miss: Lunch Ideas For Ulcerative Colitis
Symptoms Associated With Crohns Disease
Most of the time, CD affects the upper section of the large intestine and the ileum . Nonetheless, Crohns disease can affect any part of the GI tract.
CD may have patches of inflammation with healthy sections in between.
Inflammation can penetrate the deeper layers of the bowel wall.
Crohns disease can recur even after surgical removal of the affected section of bowel.
Getting To A Diagnosis
Theres no doubt that IBD can significantly decrease quality of life, between uncomfortable symptoms and frequent bathroom visits. IBD can even lead to scar tissue and increase the risk of colon cancer.
If you experience any unusual symptoms, its important to call your doctor. You may be referred to a gastroenterologist for IBD testing, such as a colonoscopy, sigmoidoscopy, or a CT scan. Your doctor may also order blood and fecal testing. Diagnosing the specific form of IBD will lead to more effective therapies.
Commitment to daily treatment and lifestyle changes can help minimize symptoms, achieve remission, and avoid complications.
Regardless of your diagnosis, Healthlines free app, IBD Healthline, can connect you with people who understand. Meet others living with Crohns and ulcerative colitis through one-on-one messaging and live group discussions. Plus, youll have expert-approved information on managing IBD at your fingertips. Download the app for iPhone or Android.
Recommended Reading: Ulcerative Colitis And Mental Health
Are Bananas Good For Ulcerative Colitis
Bananas are high on the list of healthy foods if you’re in an ulcerative colitis flare. They’re easy to digest and rich in potassium . People with irritable bowel disorders, like ulcerative colitis, are often deficient in this mineral. Blend one cup of low fat milk with one cup of yogurt, a ripe banana, and ice.
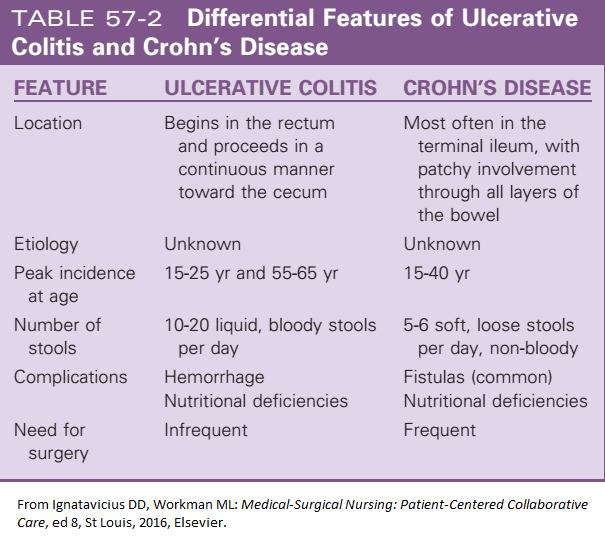
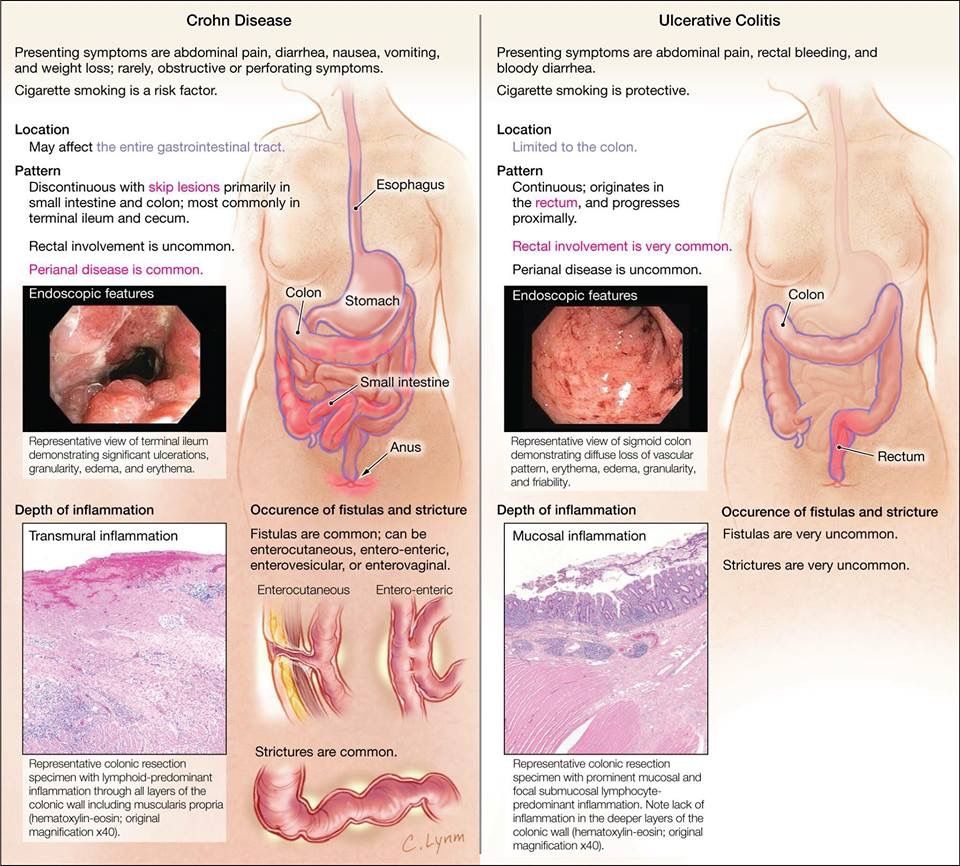
Crohns Disease Vs Ulcerative Colitis: Differences And Similarities
Ulcerative colitis and Crohns disease are both forms of inflammatory bowel disease. In both conditions, a persons intestinal tract regularly becomes inflamed.
These bouts of inflammation occur as a result of the bodys immune system reacting inappropriately to the bacteria that live in a persons gut.
However, there are some key differences involving where and how Crohns disease and ulcerative colitis affect a persons bowels.
This article looks at the key differences between ulcerative colitis and Crohns disease. It details their symptoms, describes the diagnostic criteria and treatment options, and considers the outlook for people with these conditions.
As one 2020 review explains, the main differences between ulcerative colitis and Crohns disease concern how they affect a persons bowels and which parts of the bowels they affect.
Ulcerative colitis causes inflammation of the colonic mucosa, the innermost part of a persons intestinal tract. By contrast, Crohns disease can affect any portion of the intestinal tract, including, but not limited to, the colonic mucosa.
Crohns disease typically affects a persons colon, or large intestine, as well as their terminal ileum. The terminal ileum is the part of the intestinal tract where the small and large intestines meet.
Doctors can classify ulcerative colitis in different ways, depending on which bowel parts the condition affects:
Recommended Reading: Prednisone For Ulcerative Colitis Reviews
Also Check: How To Help Ulcerative Colitis
Cd Affects Your Entire Gi Tract
- Bowel obstruction
The inflammation of CD can also cause your colon to narrow significantly, a complication known as the quill sign because your intestines may be no wider than a turkey quill in places. This narrowing obstructs your bowels and may make it difficult to pass feces.
In addition, the inflammation associated with CD may affect other areas of your body. You may have:
- Painful, red eyes
Crohns Disease And Ulcerative Colitis And Digesting Food
Your mouth and stomach break down food by mechanical and chemical means. When the food has reached a pulp-like consistency, it is slowly released into the first part of the small intestine . The food is then massaged along the length of the small intestine. Organs like the pancreas and the gall bladder make digestive enzymes to further break down the food into its simpler components.
- Crohns disease an inflamed ileum impairs absorption of vitamin B12 and bile salts. Inflammation along the length of the small intestine impairs absorption of all food nutrients. Inflammation of the large bowel impairs water absorption, causing diarrhoea.
- Ulcerative colitis digestion and absorption are generally not affected. Inflammation of the large bowel impairs water absorption, causing diarrhoea.
Other factors that may affect your nutritional status include:
- Medication some medication used to treat IBD may lessen your appetite and interfere with the absorption of certain nutrients, such as folic acid.
- Inflammation your body needs greater amounts of nutrients in order to cope with inflammation and fever.
- Surgery some people with IBD need surgery to remove parts of their small intestine. This lessens nutrient absorption.
Don’t Miss: Could I Have An Ulcer
Effects Of Crohns Disease And Ulcerative Colitis
Every person responds differently to IBD. The severity of symptoms will vary from time to time and from person to person. IBD is not a progressive disease . Rather, flare-ups can range from mild to severe and back to mild again. Some people will experience periods of relief from symptoms in between flare-ups.We cannot predict how long a person will stay free from symptoms, or when their next flare-up will occur. Some flare-ups settle down quite quickly with treatment. Other times, it may take months for a persons symptoms to respond to treatment.IBD interferes with a persons normal body functions. Signs and symptoms can include:
- pain in the abdomen
- delayed or impaired growth in children.
Symptoms Associated With Ulcerative Colitis
During a UC flare up, the individual experiences continuous inflammation within the inner lining of the colon and rectum. This inflammation leads to the development of ulcers on the surface of the lining. These ulcers usually produce blood and mucus.
Inflammation typically starts in the lower section of the colon, including the rectum.
With ulcerative colitis, there are no healthy patches between the inflamed sections of colon.
Individuals with ulcerative colitis tend to experience pain in their lower abdominal area.
Also Check: Can You Take Imodium If You Have Ulcerative Colitis
Where To Find Help With All 3
Should you find yourself experiencing any of the symptoms laid out above, its imperative that you speak with a gastrointestinal specialist as soon as you can. At the Colorectal Clinic of Tampa Bay, your physician will do a deep dive with you on all of your symptoms, your daily habits, and your overall lifestyle to best understand which condition is truly to blame. We are well versed in treating Ulcerative Colitis, Crohns Disease, and Celiac Disease, having helped many patients throughout the Bay Area find relief. Schedule your first appointment with us now!
Nutritional Supplements For Crohns
Food is ultimately the best source of nutrients, but Crohns usually causes deficiencies. Supplements can complement a balanced diet to help resolve these nutritional deficiencies. A few common ones associated with Crohns disease are:
- Fat-soluble vitamins A, D, E, and K.
Your nutritionist or health care professional may recommend supplementing these. They may also suggest the following:
These supplements also help support overall health as they support gut health and lower inflammation.
Dont Miss: What Is Best Medicine For Ulcer
Recommended Reading: How To Stop A Bleeding Stomach Ulcer
Diagnosis Criteria & Disease Severity Assessment
To assess disease activity and severity of UC, we used Mayo disease activity score, which is a combined endoscopic and clinical score .
The Crohn’s Disease Activity Index was used to assess disease severity in patients with CD consisting of 8 factors of patients symptoms during previous seven days and clinical data that are adjusted with a weighting factor and then summed. The score ranges from 0 to 600 .
The disease was considered clinically active if the CDAI score was higher than 150 and Mayo Score was higher than 3 . All patients with UC had active disease, while only 86.7% of patients with CD had Active disease.
Cd3 And T Cells In Mucosal Compartments In Relation To Clinical And Histological Variables
Proximal colon has higher numbers of mucosal T and CD3 cells than distal colon
Comparing cell numbers between proximal and distal colon mucosal compartments across all groups showed more CD3 and T cells proximally. The difference was significant for CD3 IELs and subepithelially , but not in lamina propria . The difference was also significant for IELs and in lamina propria , and nearly for subepithelial T cells . The /CD3 ratios were similar in proximal and distal colon mucosa.
To avoid bias from changes caused by active disease, separate comparisons were made only for HC and inactive IBD. The number of samples was too low in the inactive CD and UC groups to draw conclusions. When merged into one inactive IBD group, we found significantly more T cells in proximal lamina propria, but this was not the case for CD3 cells. HC clearly had more CD3 and T cells within and beneath the epithelium proximally, while the numbers in lamina propria were similar .
Oral corticosteroids impact the number of T cells, but not CD3 cells, while age, gender, and disease duration have no impact
There is no correlation between the ratio of /CD3 T cells in peripheral blood and colon mucosa in HC or during inflammation in active IBD
Recommended Reading: Diabetic Foot Ulcer Healing Time
Nicotine And Ulcerative Colitis
Ulcerative colitis is largely referred to as a disease of non-smokers. Former smokers are at the highest risk for developing ulcerative colitis, while current smokers have the least risk. This tendency indicates that smoking cigarettes may prevent the onset of ulcerative colitis.
Researchers have discovered that it is the nicotine in tobacco cigarettes that have a positive influence on symptoms of ulcerative colitis. Nicotine is a naturally occurring substance in tobacco that has a complex effect on many organs and systems in the body. Nicotine is also highly addictive, and many people who smoke cigarettes have difficulty quitting despite serious health risks.
It is theorized that the nicotine in cigarettes affects the smooth muscle inside the colon. This effect may alter gut motility .
How Smoking Affects Ulcerative Colitis
Ulcerative colitis is an inflammatory bowel disease of the colon the large intestine. While smoking is harmful to overall health, research shows that smoking may help prevent or delay the development of UC. But the effect may only last while you continue to smoke: Symptoms of UC may be worse for smokers who have quit than for current smokers or people who have never smoked.
One MyCrohnsAndColitisTeam member shared, I used to smoke a pack a day for two years, but quit two months before being officially diagnosed. I definitely think my initial flare was so horrible because I was a smoker.
Despite the potential beneficial effects on UC, experts suggest that people quit smoking to avoid other negative effects from the practice, including heart disease and lung cancer.
You May Like: Pain Medicine For Ulcerative Colitis
Read Also: Humira Ulcerative Colitis Success Rate
Can You Drink Alcohol With Crohns Disease
- Drinking alcohol is not recommended for most people with Crohns disease.
- Alcohol may irritate the lining of the intestinal wall, causing or worsening symptoms such as vomiting, diarrhea, and bleeding.
- It also may contribute to malabsorption, further complicating nutritional deficiencies.
- Alcohol interacts with many medications, causing side effects that may be serious.
- Alcohol disrupts sleep cycles and can leave you feeling tired, and irritable the next day. However, if alcohol is well tolerated and not causing any complications, it can be consumed in moderation.
- Chronic diarrhea can lead to dehydration very easily.
- Dehydration makes you feel weak, tired, light-headed, or just blah.
- Alcohol can cause headaches, abdominal pain, and other symptoms. It also can place dangerous strain on your kidneys.
- Dehydration can be avoided by making a special effort to take in plenty of nonalcoholic fluids.
- You should take at least 8 full glasses of fluid every day.
- Try to stick to water, diluted fruit juice, sports drinks, decaffeinated beverages, and fruit and vegetable drinks.
- Avoid caffeinated beverages and sodas.
Effect Of Smoking Cessation Before Ibd Diagnosis
We explored the effect of smoking cessation and compared the differences in outcomes between past smokers and current smokers at diagnosis. Among 75 smokers with UC, 51% were past smokers, and 49% were current smokers. Among 63 smokers with CD, 30% were past smokers, and 70% were current smokers. When comparing the disease phenotypes and outcomes, we did not find any statistical difference between past and current smokers, although high proportions of current and past smokers with CD had strictures and inflammatory disease phenotypes, respectively . The small sample size and the follow-up period < 20 years might explain these results.
Don’t Miss: Does Gluten Affect Ulcerative Colitis