What Are The Signs And Symptoms Of Colorectal Cancer
Unfortunately, some colorectal cancers might be present without any signs or symptoms. For this reason, it is very important to have regular colorectal screenings to detect problems early. The best screening evaluation is a colonoscopy. Other screening options include fecal occult blood tests, fecal DNA tests, flexible sigmoidoscopy, barium enema, and CT colonography . The age at which such screening tests begin depends upon your risk factors, especially a family history of colon and rectal cancers.
Even if you do not have a family history of colorectal cancer or polyps, tell your doctor if you have any of the signs that could indicate a colorectal cancer, no matter what your age. Common signs of colorectal cancer include the following:
If you experience any of these signs or symptoms, it is important to see your doctor for evaluation. For a patient with colorectal cancer, early diagnosis and treatment can be life-saving.
How To Reduce Your Risk
Here are a few other things you can do to lower your chances of developing colorectal cancer and improve your odds of finding it early if you develop it:
- Ask your doctor about taking medications such as sulfasalazine , vedolizumab , or mesalamine . These drugs help manage UC, and they may help lower your risk for colorectal cancer.
- Take your medications as your doctor prescribed to keep your UC inflammation well managed.
- See your gastroenterologist for check-ups at least once a year.
- Let your doctor know if any of your family members had colorectal cancer or have recently been diagnosed.
- Eat more fruits, vegetables, and whole grains such as brown rice or wheat bread.
- Limit red meat, such as burgers, steaks, and pork. Also limit processed meats, such as hot dogs, bacon, and sausage. Theyve been linked to colorectal cancer risk.
- Avoid alcohol or limit yourself to no more than one drink a day.
- Try to walk, ride a bike, or do other exercises on most days of the week.
Along with getting regular screenings, look for these symptoms of colorectal cancer and report them to your doctor right away:
- a change in your bowel movements
- blood in your stool
Manage Your Ibd Manage Your Colorectal Cancer Risk
To lower your risk of colorectal cancer, the main thing is to control the IBD and inflammation, says Fayez Abboud, MD, gastroenterologist with Premier Gastroenterology Specialists. He explains that inflamed tissue over time can irritate cells and change them into abnormal cells called dysplasia. And dysplasia cells can, in turn, change into cancer cells.
Dr. Abboud stresses the importance of taking the medicine your doctor prescribes to reduce symptoms and inflammation.
Theres a wide range of severity with these diseases, Dr. Abboud says. More serious symptoms may require modifying your immune system with biologics, such as Humira® or Remicaid®. Some people may require steroids to temporarily control inflammation.
Dr. Abboud says if you are in remission, reducing inflammation is likely to lower your risk of developing precancerous changes or cancer in your colon or rectum.
A colonoscopy is critically important for detecting dysplasia early, as well as removing polyps. These fleshy bumps can be the precursor to cancer.
The main thing is to control the IBD and inflammation
If you have had IBD more than eight years and a third or more of your colon is involved, general guidelines suggest you should have a colonoscopy every one to two years. If your IBD is more recent or not as severe, your doctor may recommend a colonoscopy less frequently.
You May Like: Compression Therapy For Venous Leg Ulcers
What Chemotherapy Agents Are Used To Treat Colorectal Cancer
5-Fluorouracil, or 5-FU , has been the first-line chemotherapy drug, along with the vitamin leucovorin, for advanced colorectal cancers for many years. 5-FU is often given intravenously but is also available in an oral form as capecitabine .
Two other intravenous chemotherapy drugs irinotecan and oxaliplatin also are used for the treatment of advanced colorectal cancers. Oxaliplatin is given, along with 5-FU and leucovorin, for advanced colorectal cancers, while irinotecan is used alone or in combination with 5-FU/leucovorin for patients with metastatic colorectal cancer .
Newer treatments for metastatic colorectal cancer include monoclonal antibodies and immunotherapy.
Monoclonal antibodies are created in a lab to find and destroy a particular target in this case, colorectal cancer cells. Because of their precision, the idea is that treating a tumor with a monoclonal antibody will be more specific than chemotherapy drugs, and therefore have fewer side effects.
Can Colitis Be Caused By Stress
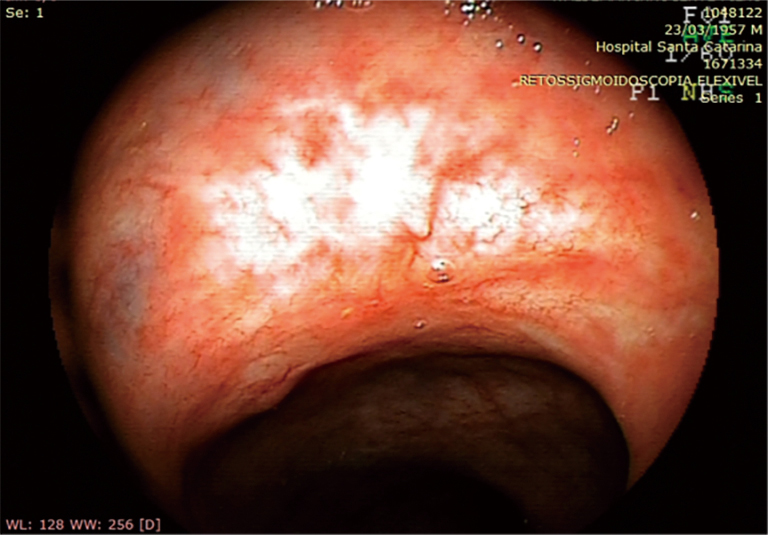
Although stress can be responsible for triggering a flare-up of symptoms, stress is currently not thought to cause ulcerative colitis. Instead, researchers think stress exacerbates it. The exact cause of ulcerative colitis is unknown, but some people have a greater risk for developing this condition.
Read Also: Can You Donate Blood If You Have Ulcerative Colitis
What If I Have A Family History Of Colorectal Cancer
Your doctor may recommend earlier screening for colorectal cancer if you have a family history of the condition. To determine the appropriate age to start screening, your doctor will discuss all of your risk factors with you. These risk factors can include a family or personal history of polyps, a history of cancer in the abdomen, and a history of inflammatory bowel disease.
Some studies have found that having a first-degree relative with colorectal cancer puts you at a risk that is 2-3 times higher than someone without a first-degree relative with colorectal cancer. A first-degree relative is defined as your mother, your father, your brother or sister, and your child. Your risk can also be higher if you have other people in your family with colorectal cancer, even if they are not first-degree relatives. They could be grandparents, aunts, uncles, cousins, nieces and nephews, even grandchildren.
The age at which any relative is diagnosed is also important. The risk to you is more significant when the relative is diagnosed before age 45.
About 75% of people who do get colorectal cancer do not get it because of genetics. About 10% to 30% do have a family history of the disease.
Reducing The Risk Of Cancer
People with UC are at greater risk of developing colorectal cancer, so it is important to take steps to manage this risk.
People with UC should see their doctor at least once per year for annual checkups and scans. At these appointments, they can discuss their condition and overall state of health.
Doctors may be able to help manage the risk of colorectal cancer in people with UC.
You May Like: Diabetic Foot Ulcer Treatment Guidelines
Does Ulcerative Colitis Affect Your Cancer Risk
Having ulcerative colitis doesnt mean you will get colorectal cancer, but it does increase your risk.
Ulcerative colitis is a chronic inflammatory bowel disease that affects the lining of the rectum and colon. It can be limited to the rectum or extend throughout the colon. Ulcerative colitis that affects the entire colon is called pancolitis.
The most common symptoms of ulcerative colitis are diarrhea and blood in your stool. Some patients may have abdominal pain. In severe cases, it can cause fever. Experts arent sure what causes the disease.
We talked to Yinghong Wang, M.D., about the link between ulcerative colitis, cancer and cancer treatment.
How does ulcerative colitis affect cancer risk?
If you have ulcerative colitis, your immune system recognizes the lining of your colon as a foreign body and attacks it. Over time, this damages the colon. As your body tries to repair the damage, the inflammation and constant cell replacement can result in a mutation that leads to cancer.
The more extensive your colitis and the longer you have it, the greater your risk of colorectal cancer. Males are at higher risk. And if you have both primary sclerosing cholangitis, which is inflammation of the bile duct, that puts you at even greater risk for colorectal cancer.
What should I do to reduce my cancer risk if I have ulcerative colitis?
Surgery is a cure. Because your colon is gone, the disease is gone, too.
What should cancer patients with ulcerative colitis know?
What Are Colon Cancer Risk Factors And Causes
Health care professionals are certain that colorectal cancer is not contagious . Some people are more likely to develop colorectal cancer than others. Factors that increase a person’s risk of colorectal cancer include increasing age, African-American race, high fat intake, a family history of colorectal cancer and polyps, the presence of polyps in the large intestine, and inflammatory bowel diseases, primarily chronic ulcerative colitis.
Age
Increasing age is the main risk factor for colorectal cancer. Around 90% of colorectal cancers are diagnosed after age 50.
Race
Surgery is the most common initial medical treatment for colorectal cancer. During surgery, the tumor, a small margin of the surrounding healthy intestine, and adjacent lymph nodes are removed. The surgeon then reconnects the healthy sections of the bowel. In patients with rectal cancer, the rectum sometimes is permanently removed if cancer arises too low in the rectum. The surgeon then creates an opening on the abdominal wall through which solid waste from the colon is excreted. Specially trained nurses can help patients adjust to colostomies, and most patients with colostomies return to a normal lifestyle.
Treatment of stage IV colorectal cancer
If the first treatment is not effective, second- and third-line options are available that can confer a benefit to people living with colorectal cancer.
Read Also: What To Do When Ulcerative Colitis Flares
Studies Show Progress For People With Ibd
The Crohns & Colitis Foundation of America reports positive news from recent studies on the link between IBD and colorectal cancer:
- Evidence shows people with IBD have a lower risk of developing colon cancer when they undergo regular colonoscopies to remove precancerous tissue.
- Colon cancers occur less frequently in people with IBD than previous reports have suggested. This may be due to better IBD medicines, regular colonoscopies or factors not yet understood.
- A sharper picture with todays scopes and newer procedure methods provide better views of the colon’s surface. So doctors can successfully remove small, precancerous polyps and tissue.
To keep improving your odds, see your doctor once a year for a checkup, even if you feel your IBD is under control.
Strategies To Reduce Your Risk Of Colorectal Cancer
Having regular colonoscopies is one of the most important preventive measures people with ulcerative colitis can take to reduce the risk of colorectal cancer.
There are also other steps people with UC can take to minimize risk, including avoiding smoking, limiting alcohol intake, maintaining a healthy weight, and exercising regularly.
Other tactics that have been shown to reduce the risk of colorectal cancer include the following:
Don’t Miss: Tofacitinib Acute Severe Ulcerative Colitis
Difference Between Ulcer And Cancer
Categorized under Health | Difference Between Ulcer and Cancer
Ulcer vs Cancer
Ulcer and Cancer are medically classed as two different illnesses. However, it is possible for an internal ulcer to develop into cancerous cells.
The inside of your body is protected by a protective layer, medically known as the mucous membrane. If this membrane becomes broken or violated the area becomes known as an ulcerated disruption. Your body will ultimately try to mend the membrane, but other factors like bacterial infection often prevent your body from doing this naturally. An ulcer will cause irritation to the surrounding nerves when this occurs, the patient experiences an enormous amount of pain and discomfort. If the membrane lining of the stomach or intestine becomes torn, you will develop a painful and life threatening form of peritonitis.
The most common type of ulcer occurs in the lining of the stomach. The stomach produces a form of acid called hydrochloric an over production of this acid can damage the cell walls causing the membrane to develop an ulcer. Ulcers can also be found in the intestines, known as duodenal ulcer. Ulcers can even form on the outer layer of the skin.
Summary.
The inner lining of your body is covered in a mucous membrane. If the membrane becomes torn, this is when an ulcer forms.2.
An ulcer will cause an irritation to the surrounding nerve endings, causing the individual to become ill.3.
What Is Chemotherapy
Chemotherapy refers to drugs that kill cancer cells. Chemotherapy drugs can be given intravenously via an injection or a pump, or orally as a pill. Each drug works against a specific cancer and is delivered in specific doses and schedules. Chemotherapy may be recommended for advanced colorectal cancers, in which the cancer cells have spread to the lymph nodes or to other organs.
Chemotherapy is used in the following ways:
- Primary chemotherapy is used when the colorectal cancer has already metastasized to other organs, like the liver or lungs. In this situation, since surgery usually cannot eliminate the cancer, chemotherapy can possibly shrink the tumor nodules, relieve symptoms and prolong life.
- Neo-adjuvant chemotherapy is given before surgery for certain rectal cancers in order to shrink the tumor and allow the surgeon to better remove it. In this situation, the patient usually receives radiation along with the chemotherapy.
- When appropriate, adjuvant chemotherapy is given after the colorectal cancer is removed with surgery. The surgery may not eliminate all of the cancer cells, and some may remain in the lymph nodes or other organs. The adjuvant chemotherapy is used to kill any of these remaining cancer cells.
Your doctor will talk with you about the best treatment for your condition.
Recommended Reading: What Happens When You Have A Bleeding Ulcer
How Often To Screen
since your symptoms first appeared or you were diagnosed with UC.
People with UC are generally advised to have a colonoscopy . Some people may need to have this test more or less often based on factors such as:
- the age when they were diagnosed
- how much inflammation they have and how much of their colon it affects
- their family history of colorectal cancer
- whether they also have PSC
What If I Have Polyps
There are a variety of colorectal polyps, but cancer is thought to arise mainly from adenomas and sessile serrated lesions, which are precancerous polyps. If a polyp is found during a colonoscopy it is usually removed, if possible. Polyps removed during colonoscopies are then examined by a pathologist and evaluated to determine if they contain cancerous or precancerous cells. Based on the number, size, and type of precancerous polyps found during colonoscopy, your healthcare provider will recommend a future colonoscopy for monitoring .
Also Check: How To Stop Ulcerative Colitis Pain
What Causes Colon Ulcers
Colon ulcers have many causes. Where the ulcers are located in your colon may help diagnose the cause.
Crohnâs disease and ulcerative colitis . Both Crohnâs and UC are types of inflammatory bowel disease , an inflammation of your colon. These diseases can cause erosions or ulcers in your colon tissue. In Crohnâs, ulcers affect patchy areas of the colon. They can appear in any part of your intestine. UC inflammation affects only the inner lining of your large intestine. It never causes ulcers in your small intestine.
Colon ulcers are often the first sign of Crohnâs. Ulcers caused by Crohnâs disease often crop up on the side of your colon near the mesentery, the tissue that holds your intestines to the inner wall of your abdomen.
After surgery. Erosions and ulcers are a rare possible complication of gastric band surgery to treat obesity. The band can slip and travel to your colon, where it causes an erosion. Your doctor can diagnose this with an image test like a colonoscopy, which uses a camera on the end of a long, flexible tube to examine your colon.
Diverticulitis. As many as 60% of older adults develop diverticulitis, an inflammation of sac-like bulges in your colon wall. If digested food gets stuck in the sac, it can cause pressure to build up and can lead to an erosion.
You can also get colon erosions from infection with cytomegalovirus .
Gastrointestinal Endoscopy: âAphthous Ulcers in Terminal Ileum Encountered During Colonoscopy: Are They Significant?â
Who Is At Risk For Colorectal Cancer
Every one of us is at risk for colorectal cancer. Although the exact cause for the development of precancerous colon polyps that lead to colorectal cancer is not known, there are some factors that increase a person’s risk of developing colorectal polyps and cancer. These risk factors include:
- Age: The risk of developing colorectal polyps and cancer increases as we age. Colorectal cancer is more common in people over the age of 50, however, younger adults can also develop colorectal cancer.
- Other medical conditions: Medical conditions and inherited conditions can increase your chances of developing colorectal cancer.
- Lifestyle factors: You may be at increased risk for developing colorectal cancer if you drink alcohol, use tobacco, don’t get enough exercise, and/or if you are overweight. Smoking increases the risk of precancerous polyps and colorectal cancer. A diet high in fat and calories and low in fiber, fruits and vegetables has been linked to a greater risk of developing colorectal cancer. Many lifestyle factors that increase the risk of colorectal cancer can be modified to lessen that risk.
Don’t Miss: Bone Broth And Ulcerative Colitis
Other Ways To Reduce Risk
Having regular checkups is an important part of reducing colorectal cancer risk. People with UC should see their gastroenterologist at least once per year. It is important to discuss any changes to symptoms or treatment, and to be open about any concerns.
Anyone who feels unsatisfied with their treatment should visit more regularly to discuss and explore their options.
It is also important to stay healthy overall. Eating a healthful, balanced diet that is rich in fruits and vegetables and low in processed foods may help keep UC in check. It is also important to eliminate trigger foods and other irritants, such as alcohol or excess amounts of meat.
Exercise is an integral part of staying healthy. Try to find a way to exercise most days of the week, such as by jogging, swimming, or cycling.
For people with UC, reducing the risk of cancer will also involve undergoing regular endoscopies or colonoscopies. This can help catch any signs of colorectal cancer at the earliest possible stage.