Southern Cross Medical Library
The purpose of the Southern Cross Medical Library is to provide information of a general nature to help you better understand certain medical conditions. Always seek specific medical advice for treatment appropriate to you. This information is not intended to relate specifically to insurance or healthcare services provided by Southern Cross. For more articles go to the Medical Library index page.
More Tips To Ease Ulcerative Colitis Symptoms
The best way to shorten a flare, of course, is to get treated by your doctor. But there are steps you can take at home too.
When you have a flare, try to follow a low-residue diet for several weeks, Damas says. The goal is to let the colon rest by avoiding fiber. That means staying away from seeds, nuts, fresh fruit, dried fruit, raw vegetables, whole grain bread and cereal, and tough meat.
Were learning more now about the influence that diet can have on control of inflammation, Damas notes. When patients are having an acute flare, its important in the short term to have a low-fiber diet. Many times, for a short period of time, until the flare-up is controlled, we recommend whats called a low FODMAP diet. However, this diet is not recommended long term, because it has no impact on inflammation itself and only on control of symptoms.
Indeed, once youre in remission, Damas says your doctor will likely recommend reintroducing fruits and vegetables as tolerated. Its better to cook vegetables without the skin and consume no more than 2 cups of milk a day.
If youre lactose intolerant, be sure you choose lactose-free dairy products. Its also a good idea to cut down on fat during this time to prevent bulky stools. Avoid other potential triggers, too, such as spicy foods.
Additionally, we recommend patients avoid eating processed foods, as well as those high in fat and animal protein, as these have been associated with inflammation in some studies, Damas says.
What Are The Treatments Complications And Risk Of Cancer For Diverticular Disease Vs Ulcerative Colitis
Diverticular Disease Treatment
A high-fiber diet is the mainstay of diverticulosis and diverticulitis prevention.
- Start a high-fiber diet because it will decrease the risk of complications and the accompanying symptoms however, will not make the diverticula a person has gone away. Foods high in fiber include:
- Whole-grain cereals and bread
- Vegetables
- Beans, peas, and lentils.
In the past patients with diverticulosis/diverticulitis were told that foods to avoid included seeds, corn, and nuts because it was thought fragments of these foods would get stuck in the diverticula and cause inflammation. However, current research has not found this to be the case, and the fiber content of such foods may benefit individuals with diverticulosis/diverticulitis. Discuss your diet or potential diet changes with your doctor.
Treatment for diverticulitis depends on the severity of the condition.
Treatment consists of IV or oral antibiotics, bowel rest, and possibly surgery.
If diverticulitis attacks are frequent or severe, the doctor may suggest surgery to remove a part of the patients colon.
- As with any surgery, there are risks the patient should discuss with his or her doctor.
- Sometimes the operation requires at least two separate surgeries on different occasions.
You May Like: Foam Dressings For Pressure Ulcer Prevention
Ulcerative Colitis Questions To Ask Your Doctor
Whether youâre worried your symptoms are UC, or you already have the condition and want more information, here are questions to ask your doctor:
- Are my symptoms a sign of ulcerative colitis or another condition?
- Are there different kinds of UC? Do they have different symptoms?
- What tests will I need?
- If I have ulcerative colitis, what will my treatment plan be?
- Will changing my diet or lifestyle help ease my symptoms?
- How serious is my ulcerative colitis?
- If I take medication for ulcerative colitis, will there be side effects?
- Should I take nutritional supplements like probiotics?
- How often will I need to come in for checkups?
- What should I do if my symptoms suddenly get worse?
- How do I know if my ulcerative colitis is getting worse?
- How do I know if I should change my ulcerative colitis medication?
- Should I consider surgery? What does surgery involve?
- What is my risk of getting colon cancer?
Feeling Comfortable With Your Doctor
Its not always easy to talk about your bowel habits. Talking about poop can be embarrassing, and many people may not be ready to open up to their doctor about it.
Others may ignore the changes to their stool or think that nothing is wrong. However, ignoring symptoms will only make things worse.
Your doctor has studied the gastrointestinal tract along with all that it does and produces. They have seen and heard it all. Nothing you say about your bowel symptoms is going to offend or shock them.
Its part of their job to know about any changes in your symptoms. Your doctor is there to help you, not to judge you.
You dont have to know any fancy medical terms when talking with your doctor about your symptoms. Share your concerns and any changes in your bowel habits you have noticed. Talking with them about changes in your stool can only help get you closer to resolving the problem.
You May Like: What Are Leg Ulcers Caused By
How Does Pediatric Ulcerative Colitis Affect My Childs Mental/emotional Health
Like many conditions, ulcerative colitis can have a negative psychological effect, especially on children. They can experience physical, emotional, social and family problems. Because of the medications and/or general stress from the situation, your child may experience:
- Mood swings.
- Worry about appearance and physical stamina.
- Vulnerability because their body doesnt function normally.
- Poor concentration.
- Misunderstandings with friends and family.
Children need mutual support from all family members. Its helpful for the entire family to learn about the disease and try to be empathetic. Seek out a psychiatrist and therapist to help your child manage such challenges of their ulcerative colitis.
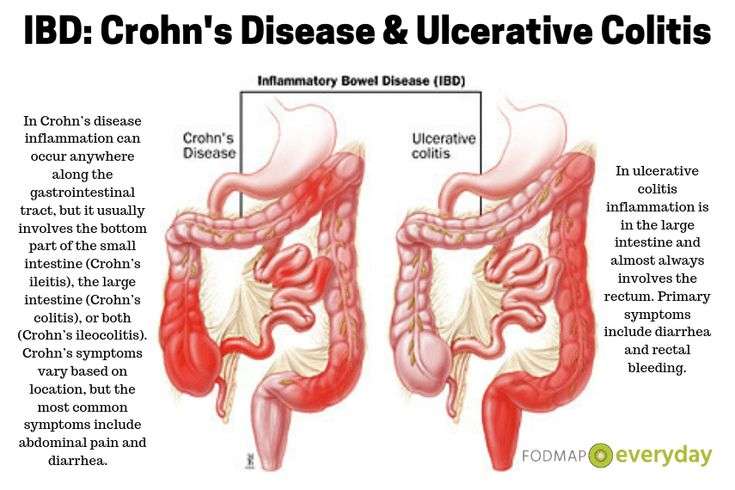
Ulcerative Colitis Vs Crohns Disease Vs Irritable Bowel
Other gut diseases can have some of the same symptoms.
- Ulcerative colitis affects only your large intestine and its lining.
- Crohnâs disease causes inflammation, but it affects other places in your digestive tract.
- Irritable bowel syndrome has some of the same symptoms as UC, but it doesnât cause inflammation or ulcers. Instead, itâs a problem with the muscles in your intestines.
You May Like: Ulcerative Colitis Bad Smelling Gas
First Symptoms Of Ulcerative Colitis Causes & Treatment
Ulcerative colitis is a chronic condition in which the large intestine becomes inflamed with ulcers that cause diarrhea and bleeding. Ulcerative colitis generally affects the lower part of the colon and the rectum, though can affect the entire colon.
Ulcerative colitis is a type of inflammatory bowel disease . Another type of IBD is Crohns disease, which can affect any part of the gastrointestinal tract from the mouth to the anus.
Symptoms of ulcerative colitis vary and mild symptoms occur in about half of all patients. The first symptoms of ulcerative colitis may include:
- Loose and urgent bowel movements
- Frequent need to empty the bowels
- Bloody stool
- Persistent diarrhea accompanied by abdominal pain and blood, mucus, or pus in the stool
Other symptoms of ulcerative colitis may include:
Patients with ulcerative colitis often have relapses, when inflammation and symptoms worsen , followed by periods of remission, that can last months to years when symptoms subside.
Complementary And Alternative Remedies
Alternative treatments such as acupuncture may help to reduce and regulate bowel inflammation, reducing UC pain.
Another form of alternative treatment called moxibustion may also have a positive effect on UC symptoms. Moxibustion is a type of heat therapy. It uses dried plant materials burned in a tube to warm the skin, often in the same areas targeted by acupuncture.
Recommended Reading: Does Stomach Ulcer Cause Pain
What Imaging Tests And Procedures Diagnose Colitis
Colonoscopy: The length of the colon can be directly viewed by colonoscopy. A gastroenterologist uses a thin, flexible tube equipped with a fiberoptic camera to view the inside lining of the colon. The appearance of the colonic lining often allows the doctor to make the diagnosis and also provides the opportunity to look for tumors and polyps. Biopsies can be obtained from the mucosal lining during colonoscopy and evaluated under the microscope by a pathologist to determine the cause of colitis. A biopsy is the only way to diagnose microscopic colitis.
Computerized tomography and barium enema are tests that are sometimes ordered to help diagnose the potential cause of colitis. CT scan of the abdomen has become a more common test to evaluate patients with abdominal pain. However, it is important for the health care professional to balance the risk of radiation with the reward of the information that can be obtained. These tests usually are performed by a radiologist.
What Role Does Diet And Nutrition Play In Ulcerative Colitis
Diet does not cause the development of ulcerative colitis nor can any special diet cure the disease. However, the foods you or your child eat may play a role in managing symptoms and lengthening the time between flareups.
Some foods may make symptoms worse and should be avoided, especially during flareups. Foods that trigger symptoms are different from person to person. To narrow down what foods affect you, keep track of what you eat each day and how you feel afterward .
Problem foods often include:
- High sugar foods and drinks.
- Carbonated beverages.
- High-fiber foods.
- Alcohol.
In addition to the problem foods listed above, infants, children and teenagers can also experience issues with:
- Salt.
- Dairy products.
Keep a careful eye on your childs diet and nutrition. Their appetite may decrease during a flareup and they might not eat enough to stay healthy, and grow. Also, the inflammation caused by ulcerative colitis may keep their digestive tract from absorbing enough nutrients. This can also affect your childs health. For these reasons, you may have to increase the amount of calories your child consumes.
Its best to work with your provider and nutritionist to come up with a personalized diet plan if you or your child has ulcerative colitis.
You May Like: How To Know You Have A Ulcer
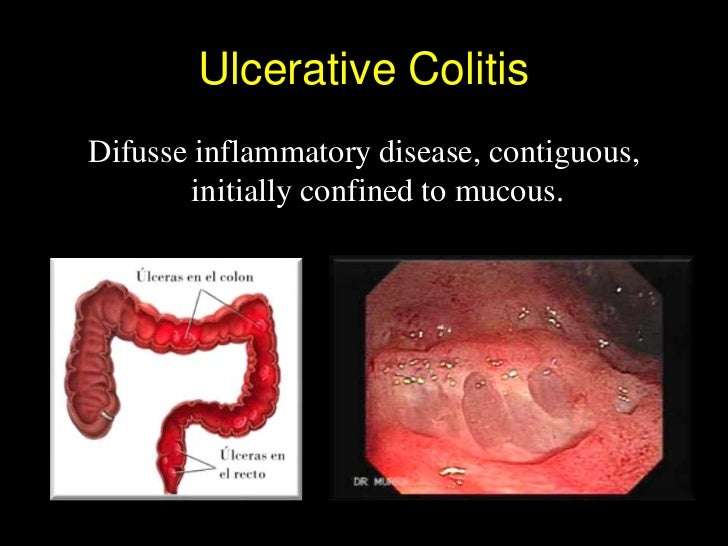
So What Exactly Is Ulcerative Colitis
Ulcerative colitis is an autoimmune disorder. It happens when your immune system turns on your own tissuesin this case, the lining or mucosa of your colonattacking with ferocity what ought to be reserved for invading pathogens. The immune assault creates open ulcers severe enough to bleed. And then theres a rush of white blood cells, which triggers inflammation.1
UC often starts in the rectum, the small section of your bowel that connects to your anus, but it can spread through the whole colon, according to the Cleveland Clinic. How the disease is classified depends on how much of the colon is inflamed. Heres what that means officially:
- Ulcerative proctitis means the problem is restricted to the rectum.
- Proctosigmoiditis means the sores and inflammation have spread to the sigmoid colon, or the last section of the bowel before you get to the rectum.
- Left side ulcerative colitis indicates that the descending segment of the colon is being affected. That part is just as it soundsthe part of the large intestine that curves downward, just above the sigmoid colon.
- Pancolitis is when the entire colon is under fire.
What To Know About Ulcerative Colitis Triggers And Flare
Once you have an ulcerative colitis diagnosis, its important to know that triggers and symptoms vary from one person to the next. A big part of your UC journey will be figuring out exactly what causes symptoms to flare up for you. Stress, loss of sleep, and the foods you eat can all play a role in triggering a flare, according to the Crohns and Colitis Foundation. Once a flare subsides, you could find yourself in a remission that lasts weeks, months, or years.
During flares, it could feel like déjà vu with a return to symptoms you noticed at the start of your journey, including:
- frequent trips to the bathroomsometimes a dozen or more a day
- bloody diarrhea
- fatigue, exhaustion, or physical weakness
- loss of appetite or weight loss
Flares can occur without a trigger, James East, M.D., colonoscopist and gastroenterology consultant at Mayo Clinic in London, tells SELF, although stress, infection, and running out of medication can all start a flare.
He recommends an at-home stool test to help you pinpoint when a flare is starting. This can help patients self-monitor their disease at home and pick up flares early so treatment can be initiated promptly.
Read Also: Will Ulcers Cause Blood In Stool
Which Type Of Doctor Treats Colitis
- Gastroenterologists are the medical specialists that treat diseases of the gastrointestinal organs such as colitis.
- In some cases colitis may be managed by primary care specialists or internal medicine specialists.
- Depending on the type of colitis, other specialists may be involved in the treatment, including
- infectious disease specialists or surgeons.
- Pediatricians or pediatric gastroenterologists are involved in the care of infants, children, and teens with colitis.
When To See A Doctor If You Have Bowel Concerns
If youre having bloody diarrhea, dont wait to get help. Talk to a health professional sooner rather than later, so you can start working on a treatment plan that will get you out of the bathroom and back to normal.
Dr. Philpott also recommends keeping track of your symptoms. It can be hard to assess your response to treatment if you dont know where you started, Dr. Philpott notes. Document your symptoms down to the number of bowel movements you have. Life can be so hard with this condition that people sometimes have a hard time communicating. If you keep track of the symptoms objectively, its easier for your doctor to see how youre doing.
You dont have to just live with uncomfortable symptoms, even if youre already taking medications, Dr. East says, as adjustments to your treatment plan may be necessary. Long-term poorly controlled inflammation increases your bowel cancer risk and decreases your quality of life. New treatments could ease you into remission faster and keep you there longer.
Don’t Miss: Pediatric Ulcerative Colitis Treatment Guidelines
Symptoms Of Ulcerative Proctitis
The presenting symptoms of ulcerative proctitis all relate to the rectum. Blood in the stool occurs in almost everyone with the disease. Diarrhea is a common symptom, although constipation can also develop as the body struggles to maintain normal bowel function.
Inflammation of the rectum may cause a sense of urgency to have a bowel movement, discomfort after having a bowel movement, and a sensation of incomplete emptying of the bowels. Systemic symptoms such as fever, tiredness, nausea, and weight loss are rare.
Ulcerative proctitis has very few complications but with increased irritation to the anal and rectal area, hemorrhoids may occur. Only rarely do other complications occur, such as abscesses and extra-intestinal manifestations. Individuals with ulcerative proctitis are not at any greater risk for developing colorectal cancer than those without the disease.
What Should I Ask My Doctor
If you have ulcerative colitis, you may want to ask your healthcare provider:
- How much of my large intestine is affected?
- What risks or side effects can I expect from the medication?
- Should I change my diet?
- Will ulcerative colitis affect my ability to get pregnant?
- What can I do at home to manage my symptoms?
- What are my surgical options?
Don’t Miss: Remicade Dosing For Ulcerative Colitis
How Ulcerative Colitis Is Treated
Treatment for ulcerative colitis aims to relieve symptoms during a flare-up and prevent symptoms from returning .
In most people, this is achieved by taking medication such as:
- aminosalicylates
- corticosteroids
- immunosuppressants
Mild to moderate flare-ups can usually be treated at home. However, more severe flare-ups need to be treated in hospital to reduce the risk of serious complications, such as the colon becoming stretched and enlarged or developing large ulcers. Both of these can increase the risk of developing a hole in the bowel.
If medications aren’t effective at controlling your symptoms, or your quality of life is significantly affected by your condition, surgery to remove your colon may be an option.
During surgery, your small intestine will either be diverted out of an opening in your abdomen , or used to create an internal pouch that’s connected to your anus .
Read more about:
What Is The Best Diet For Ulcerative Colitis
Theres no single diet that works best for ulcerative colitis. If the disease damages the lining of the colon, your body might not absorb enough nutrients from food. Your healthcare provider may recommend supplemental nutrition or vitamins. Its best to work with your provider and nutritionist to come up with a personalized diet plan.
Also Check: Foods That Cure Ulcerative Colitis
Outlook For People With Ulcerative Colitis
If you have UC, a doctor will need to monitor your condition, and youll need to carefully follow your treatment plan throughout your life.
The only true cure for UC is removal of the entire colon and rectum. Your doctor will usually begin with medical therapy unless you have a severe complication that requires surgery. Some people will eventually require surgery, but most do well with nonsurgical therapy and care.
A Chronic Inflammatory Disease
Ulcerative colitis belongs to a larger group of illnesses called inflammatory bowel diseases that affect the large intestine in the gastrointestinal tract. It is a chronicor long-lastingdisease that can get worse over time if left untreated.
While the exact cause of UC is not fully understood, research shows that it could be the result of several factors, such as genetics, the environment, or an immune system malfunction.
What You Need to Know
Read Also: Why Do We Get Ulcers In Stomach