Talking With Your Healthcare Team
Not every doctor and nurse will be aware of how serious fatigue can be for people with IBD. It may be hard to get them to understand that it is affecting your quality of life and that you need help managing it. Dont let anyone dismiss how you are feeling and lose your chance of getting help.
If youre looking for words that can describe how you are experiencing fatigue, try using overwhelming tiredness, brain fog or completely wiped out.
Fatigue is a symptom of IBD and should be treated like any other symptom that needs to be managed.
Tips For Managing Your Ulcerative Colitis Fatigue
The key to easing fatigue is not to ignore it. Fatigue is a sign that something requires attention, Katkov says. Consider the following steps.
Additional reporting by Ashley Welch.
How Does Pediatric Ulcerative Colitis Affect My Childs Mental/emotional Health
Like many conditions, ulcerative colitis can have a negative psychological effect, especially on children. They can experience physical, emotional, social and family problems. Because of the medications and/or general stress from the situation, your child may experience:
- Worry about appearance and physical stamina.
- Vulnerability because their body doesnt function normally.
- Poor concentration.
- Misunderstandings with friends and family.
Children need mutual support from all family members. Its helpful for the entire family to learn about the disease and try to be empathetic. Seek out a psychiatrist and therapist to help your child manage such challenges of their ulcerative colitis.
Read Also: Can Coffee Cause Extreme Fatigue
Read Also: Are All Ulcers Caused By H Pylori
Tips To Manage Your Fatigue With Ulcerative Colitis
Because fatigue can be debilitating and prevent you from carrying out your daily tasks, its important to be aware of the steps you can take to help combat fatigue experienced in ulcerative colitis. Here are some tips to manage your fatigue associated with ulcerative colitis.
- Control your ulcerative colitis: work with your doctor to develop a treatment plan to better manage your condition.
- Rule out other causes of fatigue: have yourself check for anemia, sleep disorders, mental health problems, and anything else that could be contributing to fatigue.
- Exercise regularly.
- Try to improve your sleep: aiming to get at least eight hours a night is a good goal for improving the quality of your sleep. Ensure your sleeping space is conductive for proper sleep.
- Supplement with vitamins: with sever colitis, absorbing vitamins and nutrients may be difficult, so your doctor may recommend mineral and vitamin supplementation to help boost your nutrition and combat fatigue.
- Plan ahead: if you have an upcoming event, plan ahead and get plenty of rest beforehand.
- Make adjustments to your work day, if possible: if the standard nine-to-five schedule isnt working for your fatigue, try to find ways to create a different schedule so you can be more productive.
- Reduce stress: stress can be taxing on the body, promoting and worsening your fatigue.
- Become aware of your triggers: knowing what prompts your fatigue can help you reduce it. A good example of a common fatigue trigger is poor sleep.
How Can Fatigue Affect People With Ibd

Key points
- When experiencing IBD fatigue, even simple everyday tasks can be hard to do.
- Fatigue can interfere with your relationships and social life. Speaking openly about your condition can make it easier for you and those you care about.
- Work and school life can be harder if youre experiencing IBD fatigue and you may need to make some changes.
Being too tired to do anything means that every part of your life can be affected. Even normal everyday tasks may take greater effort.
Each person will have a different experience of fatigue but there are some common areas of life that can be affected.
Physical activity Participating in sport may be very hard for those experiencing fatigue but some people will find it hard to do housework, drive or even move around the house.
Concentration Thinking and focusing can become difficult when experiencing fatigue. You may even start to stumble over your words.
Social life Because fatigue can come on without warning, it can be hard to make plans to see friends, travel or maintain your hobbies and interests.
Relationships It can be hard to explain IBD fatigue to friends and family, and their lack of understanding can affect your relationships negatively. Not being able to contribute fully can also make you feel guilty towards them when they have to do extra work.
Recommended Reading: What Foods To Eat When You Have A Stomach Ulcer
What Ulcerative Colitis Fatigue Feels Like
Fatigue is beyond just a passing feeling of being tired, explains Dr. Katkov. People with ulcerative colitis can experience malaise, a profound kind of fatigue that makes it difficult to carry out normal activities, he says.
Tina Haupert, a nutrition coach living in the South Shore of Massachusetts who was diagnosed with ulcerative colitis in 2011, agrees. Before addressing her UC fatigue with dietary changes and exercise, she pretty much always felt tired.
According to research by the British organization Crohns and Colitis UK, people with IBD often describe their tiredness with words such as: brain fog, zombie mode, feeling woozy or fuzzy, completely wiped out, and overwhelming heaviness.
The group also found that IBD fatigue tends to be unpredictable it can come on suddenly, without warning, and vary from day to day. It can also affect memory and concentration, interfere with work, make it harder to exercise and socialize, and take a hefty emotional toll, leading to reduced confidence and depression, they report.
Experts agree that making sure fatigue doesnt interfere with quality of life, the ability to work, and the capacity to have a normal social life is central to the goal of treating a chronic condition like ulcerative colitis. We dont want to settle for a lower quality of life than what can be achieved with aggressive treatment, Katkov says.
What Are The Types Of Crohns Disease
Crohns disease can affect different sections of the digestive tract. Types of Crohns disease include:
- Ileocolitis: Inflammation occurs in the small intestine and part of the large intestine, or colon. Ileocolitis is the most common type of Crohns disease.
- Ileitis: Swelling and inflammation develop in the small intestine .
- Gastroduodenal: Inflammation and irritation affect the stomach and the top of the small intestine .
- Jejunoileitis: Patchy areas of inflammation develop in the upper half of the small intestine .
Read Also: Treating Leg Ulcers With Sugar
Read Also: How To Treat Unstageable Pressure Ulcer
Can I Stop Taking My Meds In Deep Remission
In a word: no. The key to remaining in remission is sticking to your recommended treatment plan. A study published in PLoS One found that people in remission who stopped taking their meds were five times more likely to relapse. Treatments that may help achieve or maintain UC remission include aminosalicylates, drugs that reduce inflammation in the lining of the colon, and immunomodulators, meds that modify the immune system in order to decrease the bodys inflammatory response. All treatments come with potential side effects, and it can take time to find the one that works best for you.
Also Check: Best Treatment For Stage 2 Pressure Ulcer
Weight Loss And Loss Of Appetite
About half of individuals with ulcerative colitis experience weight loss.4 Loss of appetite is common, due to fear of eating and the symptoms that follow.4,13 Some people have very limited diets in order to manage their symptoms. Healing from inflammation or surgery can increase nutrient needs at a time when it is difficult to eat. Diarrhea can cause significant loss of fluid and blood.
One weight measurement is not enough for evaluating a persons nutritional status.13 It is important that your health care provider or dietitian tracks changes in your weight over time.
Recommended Reading: What Medicine To Take For Ulcer
What Is The Outlook For Someone With Ulcerative Colitis
Ulcerative colitis can be managed with treatment. It generally wont alter the life expectancy of most people.
Most people with UC experience acute flares of symptoms during their lifetime. But with treatment, the disease can enter remission, during which symptoms go away.
Remission may last for weeks or even years. The longer the period of remission, the better a persons general health becomes.
Dr. Saurabh Sethi is a board certified physician specializing in gastroenterology, hepatology, and advanced interventional endoscopy. In 2014, Dr. Sethi completed his gastroenterology and hepatology fellowship at Beth Israel Deaconess Medical Center at Harvard Medical School. Soon after, he completed his advanced endoscopy fellowship at Stanford University in 2015. Dr. Sethi has been involved with multiple books and research publications, including over 30 peer-reviewed publications. Dr. Sethis interests include reading, blogging, traveling, and public health advocacy.
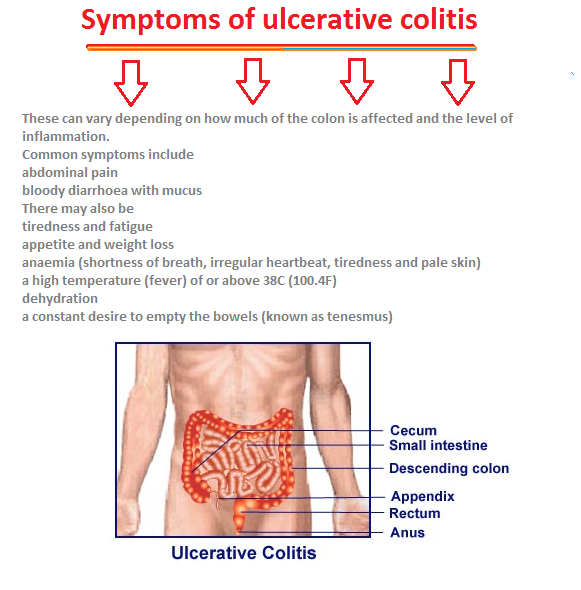
Most Symptoms Of Ulcerative Colitis Relate To Bowel Movements
The symptoms of ulcerative colitis can vary from person to person, based on where the disease is in the body and how bad the inflammation is.
Most common symptoms:
- Diarrhea , which is often the first symptom.
- Blood in the stool.
- Urgency, or immediate need, to go to the bathroom.
- Increased number of bowel movements.
- Belly pain and cramping.
Ulcerative colitis can cause symptoms throughout your body.
You might have weight loss or other symptoms that affect the entire body. The inflammation of ulcerative colitis can also affect your joints or skin, leading to painful joints and skin rashes. During a flare-up, symptoms may go beyond those that affect the digestive system, including:
- Rashes or patches of red, swollen skin.
- Painful or swollen joints.
- Red, irritated eyes.
Keep of track of any symptoms, how often you have them, and how bad they are to talk about with your health care provider.
You May Like: What Is Crohn’s Disease And Ulcerative Colitis
Outcomes And Statistical Analysis
Patient demographics, clinical characteristics, disease activity and medication use were reported by the gastroenterologist, while current symptoms during the time of consultation , work productivity , EQ-5D and the Short Inflammatory Bowel Disease Questionnaire were reported by the patient. The WPAI generates four metrics: absenteeism, presenteeism, overall work impairment and activity impairment . The SIBDQ consists of ten items covering four dimensions: bowel, systemic, emotional and social it is scored on a seven-point scale with higher scores indicating a better HRQoL . Numeric rating scales were used to assess level of pain and sleep disturbance. For the other symptoms, patients indicated whether they were present or absent from a list of symptoms.
Disease activity was measured using the Mayo score for patients with UC and the Crohns Disease Activity Index for patients with CD . The components for the Mayo scores were collected and derived from PRF data and the score for all patients was calculated using the PRF. Similarly, the CDAI components were collected and derived based on the data from the PRF and PSC.
Assessment Of Concurrent Symptoms
In order to select an optimal treatment strategy, assessment of concurrent symptoms is mandatory. Many factors are known to contribute to fatigue, such as inflammation, pain, emotional distress, sleep disturbance, anaemia, alterations in nutrition and overall nutritional status, and a diminished activity level. The presence of any of these conditions should be treated in accordance with practice guidelines and with referral to other care professionals as appropriate. Furthermore, medication side effects as well as alcohol and/or drug abuse should be taken into account, as should other comorbidities.
2.2.1. Inflammation
During periods of active gut inflammation, fatigue rates understandably increase. Fatigue, on the other hand, is a highly reported symptom and a major concern in IBD patients and fatigue can be a concealed indication of active disease. Disease activity should be ascertained by the usual clinical, radiological and endoscopic assessments in order to optimize treatment.
2.2.2. Anaemia
2.2.3. Nutrition
2.2.4. Sleep disturbance
2.2.5. Emotional distress
2.2.6. Pain
2.2.7. Medication side effects
2.2.8. Activity level
2.2.9. Comorbidities
2.2.10. Substance abuse
Alcohol and/or drug abuse are associated with emotional distress, poor sleep quality and anxiety, and should always be assessed in the work-up of IBD-related fatigue.
Don’t Miss: Common Symptoms Of Stomach Ulcer
You Begin Doing The Things You Used To Do
You will know the treatment and medication are working when you start doing the things you enjoyed doing before. For instance, going out or taking on extra activities. As long as you are maintaining your treatment plan and avoiding triggers, there should be no problem with doing the things you enjoyed doing before.
Dont Miss: Compression Stockings For Leg Ulcers
Prevalence And Score Of Fatigue
The prevalence of fatigue in patients with UC, defined as a FSS score> 4, was 61.8% in the total study population. The prevalence of fatigue in patients with active disease was 68.2%, which was remarkably high compared with those in remission . The score of MFI showed a positive correlation with FSS score . The median FSS score of UC patients was 4.4. The median total score of MFI was 61 . The scores of different MFI domains were general fatigue: 13 physical fatigue 13 mental fatigue11 reduced activity 11 and reduced motivation 12 .
Fig. 1
Fatigue score in ulcerative colitis patients. A Correlation between FSS score and MFI score in patients with UC. Pearson r=0.687 P< 0.0001. B The fatigue score of different MFI domains
You May Like: Natural Herbs To Treat Stomach Ulcers
Treatments For Extreme Tiredness And Lack Of Energy In Inflammatory Bowel Disease
Review question
What are the effects of drug and non-drug treatments on fatigue in individuals with inflammatory bowel disease compared to no treatment, placebo or active comparator ?
Background
IBD is a life-long illness that causes inflammation and ulceration in the gut. Crohns disease and ulcerative colitis are the two main types of IBD. People living with IBD often experience fatigue, which can be burdensome and negatively impact on their quality of life. Different treatments, such as medications and exercise, may improve fatigue. However, it is unclear what the effects of such treatments on fatigue in IBD are. This review presents the available evidence of the effectiveness of treatments on fatigue in IBD.
Search date
Extensive searches were undertaken from inception up to July 2018. A top-up search was run in October 2019.
Study characteristics
Fourteen studies met the inclusion criteria. Nine different drug trials, four non-drug trials and one multimodular trial were included in the review. Thirty ongoing studies were also identified and five studies are awaiting classification. In only four trials was managing fatigue the aim of the intervention. In the remaining trials the interventions were aimed at managing other symptoms, including fatigue. Data on fatigue were not available for the fourteen trials, therefore, the findings of this review are based on 1344 participants in nine trials. Most studies were small in size and had low or very low quality of evidence.
Stomach And Back Pain At The Same Time
For most of us, its not uncommon to have an occasional stomachache or acute back pain. But what does it mean if both are happening at the same time? This could be a coincidence, but it may also be concerning to notice two disconnected symptoms. The combination of pains may make daily activities difficult or be distracting. If the pain reaches this level, it may be a good idea to visit an Atlanta MRI center to rule out any serious conditions that could cause both problems at the same time.
If your stomach ulcers caused by a Helicobacter pylori bacterial infection, youll be given:
- a course of antibiotics
- a medication called a proton pump inhibitor
This is also recommended if its thought your stomach ulcers caused by a combination of an H. pylori infection and non-steroidal anti-inflammatory drugs .
Read Also: What Can I Do For Mouth Ulcers
You May Like: Can A Heating Pad Help Ulcerative Colitis
Uc Fatigue Has Many Sources
When it comes to UC and fatigue, there are a number of contributing factors at play, says Ashwin Ananthakrishnan, M.D., an associate professor of medicine at Massachusetts General Hospital and Harvard Medical School in Boston. It is likely that different factors influence each other, so it may not be just one thing that is making you tired. In other words, UC can come at you at once from multiple fronts. Contributing factors may include inflammation inadequate nutrition status, including iron deficiency the role of depression stress impaired sleep and other factors, he explains.
Check If You Have Anaemia Or Nutrient Deficiencies
If your disease is under control, the next step may be to check your bloods for anaemia or low levels of nutrients. However, not all nutrients can be tested easily. Your doctor may check your iron, vitamin B12, folate, vitamin D, magnesium and calcium levels.
Try to ask your healthcare team what they are testing for. It may be helpful to keep a note of your results so you can compare them in the future. Even if all your bloods are ok, it may help to feel involved in your care and to know the numbers. You can use our appointments journal to help with this.
If you have iron deficiency anaemia then you may be given a top up either with tablets or through a drip, which often helps fatigue. However, people who do not have anaemia but do have low iron stores usually do not get benefit in fatigue levels after having iron replacement. Vitamin B12 and folate are also used to treat some types of anaemia. In more severe cases, a blood transfusion may be needed to treat your anaemia.
Topping up your vitamin D may help your fatigue, but there is not much evidence for this There is some evidence suggesting that high dose thiamine may help reduce fatigue in people with Crohns and Colitis. But more research is needed before this can become a routine treatment.
You May Like: How Do You Cure Ulcerative Colitis