How Do You Get Colitis
According to the Mayo Clinic, the exact cause of ulcerative colitis is still unknown. In most cases, this disease develops over a long period of time, instead of suddenly.
Ulcerative colitis is thought to be the result of the interaction of different risk factors. However, these risk factors dont cause the disease directly they simply increase your likelihood of developing UC at some point in your life.
People with UC have an overactive immune system that malfunctions and attacks their own intestinal tissue. This irregular immune response causes the immune system to harm the cells in your digestive tract instead of fighting off possible health threats, such as bacteria and viruses. It has been theorized that infections can trigger the development of UC, or that an unbalanced gut microbiota may be involved. However, more research is still needed on this topic.
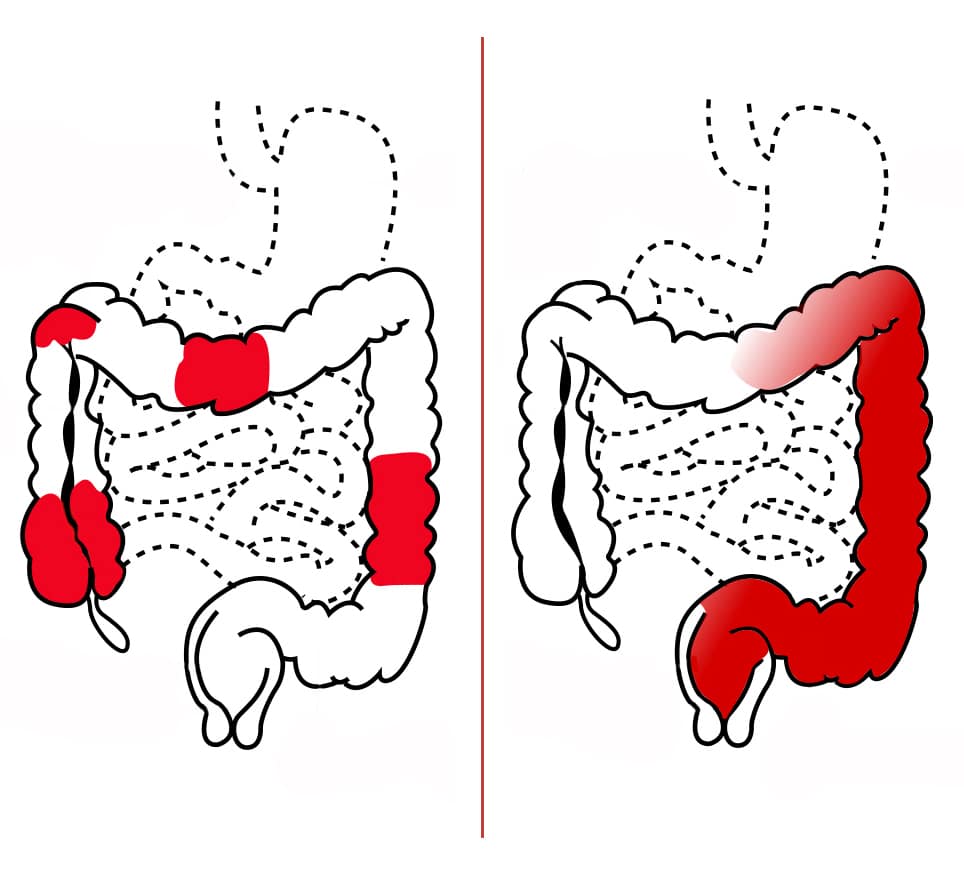
According to UCLA Health, there are four different types of ulcerative colitis, including:
- Ulcerative proctitis: this type of UC only affects the rectum, and its typically milder than other forms of the disease.
- Proctosigmoiditis: this condition affects the rectum and sigmoid colon, which is the terminal part of the large intestine right before the rectum starts.
- Left-sided or distal colitis: this is a form of descending colon colitis which affects the rectum and large intestine up to the splenic flexure.
- Pancolitis: in this type of UC, the entire colon is affected by the disease.
What Can I Expect If I Have A Diagnosis Of Ulcerative Colitis
Ulcerative colitis is a lifelong condition that can have mild to severe symptoms. For most people, the symptoms come and go. Some people have just one episode and recover. A few others develop a nonstop form that rapidly advances. In up to 30% of people, the disease spreads from the rectum to the colon. When both the rectum and colon are affected, ulcerative symptoms can be worse and happen more often.
You may be able to manage the disease with medications. But surgery to remove your colon and rectum is the only cure. About 30% of people with ulcerative colitis need surgery.
Dont Miss: Ulcerative Colitis Iv Infusion Treatment
What Should I Eat
Its not always easy knowing what foods best fuel your body, especially when you have Crohns disease or ulcerative colitis. Your diet and nutrition are a major part of life with inflammatory bowel disease , yet there is no single diet that works for everyone.
Nutrition affects not just your IBD symptoms, but also your overall health and well-being. Without proper nutrients, thesymptoms of your Crohns disease or ulcerative colitis can cause serious complications, including nutrient deficiencies, weight loss, and malnutrition.
We have several tips for a healthy diet thats well-balanced and nutrient rich. These tips are for educational purposes only. You should work with your doctor or a dietitian specializing in IBD to help you develop a personalized meal plan.
Watch our with Emily Haller, registered dietitian at Michigan Medicine! Tune in to hear Emily review diet facts, debunk myths, speak about restrictions, and highlight ongoing research.
You May Like: How To Self Treat An Ulcer
Untreated Ulcerative Colitis: Risks And Can You Die
Ulcerative colitis is a type of inflammatory bowel disease. In people with ulcerative colitis, an overactive immune system attacks the lining of the colon, causing ulcers and inflammation. Symptoms typically include:
- frequent diarrhea
These symptoms can range from mild to severe, and they tend to come and go in cycles.
When a person has few or no symptoms, doctors refer to it as being in remission. When symptoms suddenly get worse, they call it a flare-up.
In this article, we discuss the potential consequences of people leaving ulcerative colitis untreated, and whether a person can die from this condition.
We also cover when to see a doctor and treatment options.
What To Eat During A Flare
All of the diets above are intended to be temporary and followed during a flare-up. Working with a dietitian can help prevent deficiencies in certain micronutrients, which is common with IBD.
During a flare its helpful to eat four to six small meals per day rather than fewer larger meals. Its also very important to drink fluids because diarrhea can occur with a flare and cause dehydration.
Dont Miss: Ulcerative Colitis Bad Smelling Gas
You May Like: What Foods Should I Avoid With A Stomach Ulcer
How Does Pediatric Ulcerative Colitis Affect My Childs Mental/emotional Health
Like many conditions, ulcerative colitis can have a negative psychological effect, especially on children. They can experience physical, emotional, social and family problems. Because of the medications and/or general stress from the situation, your child may experience:
- Worry about appearance and physical stamina.
- Vulnerability because their body doesnt function normally.
- Poor concentration.
- Misunderstandings with friends and family.
Children need mutual support from all family members. Its helpful for the entire family to learn about the disease and try to be empathetic. Seek out a psychiatrist and therapist to help your child manage such challenges of their ulcerative colitis.
Dont Miss: How Do You Know If Your Horse Has Ulcers
Research And Statistics: How Many People Have Ulcerative Colitis
People of European descent have a higher risk of developing ulcerative colitis than do those of African or Hispanic descent.
People of European Jewish descent have an especially high risk.
Ulcerative colitis tends to run in families, affecting men and women equally overall. But older men are more likely to develop it than older women, according to the Crohns and Colitis Foundation.
Recommended Reading: Does Ulcerative Colitis Cause Fatigue
How To Calm An Ulcerative Colitis Flare
This article was co-authored by Peter Gardner, MD. Peter W. Gardner, MD is a board certified physician who has practiced Gastroenterology and Hepatology for over 30 years. He specializes in diseases of the digestive system and liver. Dr. Gardner earned his Bachelors degree from the University of North Carolina and attended Georgetown Medical School. He completed his residency in Internal Medicine and then his fellowship in Gastroenterology at the University of Connecticut. He is a previous Chief of Gastroenterology at Stamford Hospital and remains on the staff. He is also on the staff of Greenwich Hospital and New York Presbyterian Hospital. Dr. Gardner is an Approved Consultant in Internal Medicine and Gastroenterology with the American Board of Internal Medicine.There are 8 references cited in this article, which can be found at the bottom of the page.wikiHow marks an article as reader-approved once it receives enough positive feedback. In this case, 100% of readers who voted found the article helpful, earning it our reader-approved status. This article has been viewed 14,663 times.
You May Like: What Is The Best Medicine For Mouth Ulcer
Is Ulcerative Colitis Serious
Unfortunately ulcerative colitis, or UC as its often referred to, does have the potential to be a serious illness due to some of the complications it can cause.
However, its important to remember that most people with ulcerative colitis dont experience some of the more serious complications that can occur due to receiving effective treatment. To help minimise your risk of complications you should follow the treatment prescribed by your doctor.
Some of the things that can cause serious complications include…
Read Also: Stage 2 Pressure Ulcer Icd 10
Recognizing The Signs Of A Person At Risk Of Suicide
According to the National Institutes of Health, signs someone is at risk for suicide include:
- Threatening to hurt or kill oneself or talking about wanting to hurt or kill oneself
- Looking for ways to kill oneself, such as seeking access to firearms, pills, or other means
- Withdrawing from family, friends, and society
- Feeling hopeless
Dont Miss: Foam Dressings For Pressure Ulcer Prevention
Whats A Good Plan To Manage Uc Cramping
Monitor your medications. Talk to your doctor about any prescription, over-the-counter, or herbal medications youre taking. Iron deficiency is common with UC, but oral iron supplements have been shown to increase the risk of inflammation and cramping. Some antibiotics and pain relievers, such as ibuprofen, may also increase flare-ups and cramping.
Review your diet.Keep a food diary and note the connection between the foods you eat and your UC symptoms. In general, its smart to stay away from processed foods and those high in saturated fat and sugar. High-fiber foods and dairy products can also cause UC cramping, but check with your doctor before eliminating foods from your diet, to ensure youre getting the nutrients you need.
Eat frequent, small meals. Instead of two or three large meals, eat four to six smaller meals spaced more closely throughout the day. Also, take your time while eating and chew thoroughly.
Skip caffeine and carbonated drinks. Caffeine can cause gas, intensifying abdominal cramping. It is also a stimulant, which can make cramping and diarrhea worse.
Drink enough water. People with UC may be at increased risk of dehydration, so be sure to drink plenty of H2O. A good rule of thumb, according to the Crohns and Colitis Foundation, is to aim for about 64 ounces or eight 8 oz glasses per day.
Don’t Miss: What Essential Oils Are Good For Ulcerative Colitis
How Do You Get Rid Of Colitis
The only way to cure ulcerative colitis is to get surgery to remove the diseased colon and rectum. You may also choose an operation if you want to cut your risk of colon cancer. Your chances of getting colon cancer go up if you have ulcerative colitis for 8 years or more or have a lot of colon damage.
Menstrual Cycle & Ulcerative Colitis

Women with UC, experience changes in their menstrual cycle and start to experience irregular periods or changes in their flow. The prostaglandins that cause uterine contractions and other menstrual symptoms also cause colon contraction, which in turn make the period pain more intense.
When women with UC menstruate they face an increased risk for anemia. The anemia risk is high for women with high flow. Losing a lot of blood during the flow can use up more red blood cells than the body can produce, thus reducing iron stores.
You May Like: Can An Ulcer Cause Stomach Pain
Your Immune System May Suffer
Inflammation can put constant stress on your body, which makes you vulnerable to infections and other illnesses. Your body is putting in so much energy to try to keep the inflammation under control that it really doesnt allow your body to do the normal housekeeping things its supposed to do, Bonthala explains. So people have a harder time fighting off illnesses and are more susceptible to catching other infections.
Outcome And Complications From Ileoanal Anastomosis
Complications are common with any intestinal operation. In a small percentage of IPAA procedures, complications occur that require conversion to an ileostomy.
Pouchitis
Inflammation of the pouch is the most common complication of the pouch procedures. Symptoms include rectal bleeding, cramps, and fever. It can usually be successfully treated with antibiotics such as metronidazole or ciprofloxacin .
Bowel obstruction
Bowel obstruction may occur although it is less common than pouchitis. With most people, this condition can be treated by avoiding food for several days and administering intravenous fluids. In some cases of bowel obstruction, surgery may need to be performed to remove the blockage.
Pouch failure
Pouch failure occurs in a small percentage of people. It requires permanent removal of the pouch and use of ileostomy.
Irritable Pouch Syndrome
Irritable pouch syndrome is a problem that includes frequent bowel movements, an urgent need to defecate, and abdominal pain. However, there are no signs of inflammation as there are with pouchitis. Stress and diet play a role in this condition, and it is usually relieved after a bowel movement.
Infertility
IPAA can cause infertility in women because the surgery can scar or block the fallopian tubes.
Read Also: Paleo Diet For Ulcerative Colitis
What To Expect After Your Surgery
Most people do very well after their surgery and are able to return to work and their normal daily activities after they recover.
-
You should expect an adjustment period of up to one year to get used to the changes in your body after your proctocolectomy.
-
Some patients may still feel as if they need to have a bowel movement after their surgery, just as people who have lost a limb sometimes still feel as if the limb is still there. This called phantomrectum and it completely normal. It does not require any treatment and often subsides over time.
-
Your doctor may recommend a physical activity restriction for a minimum of six weeks, depending on what type of surgery you had.
-
Talk to your doctor about resuming normal sexual activity after your surgery. Some people find their sex life improves some time after surgery due to improvements in pain, inflammation, and other ulcerative colitis symptoms.
Open Up To Friends And Family
If youre feeling too tired to go to a relatives birthday party, for example, be honest about it. Parris says she hid her fatigue from family and friends for a long time because she was embarrassed. But after I shared what I was going through, they were really supportive, she says. Plus, it made me stop looking like a flake when I couldnt go out. They understood the real reason instead of me having to try and make up an excuse.Speaking up about her ulcerative colitis allowed Parris to help her friends and relatives better understand what she was going through so that they could be more supportive.
You May Like: How Do You Say Ulcerative Colitis
Ulcerative Colitis Treatment Options
The primary goal in treating ulcerative colitis is to help patients regulate their immune system better. While there is no known cure for ulcerative colitis and flare ups may recur, a combination of treatment options can help you stay in control of your disease and lead a full and rewarding life.
Treatment for ulcerative colitis is multifaceted and includes the use of medication, alterations in diet and nutrition, and sometimes surgical procedures to repair or remove affected portions of your GI tract.
It Helps To Have A Network Of People With Ulcerative Colitis
Hopefully, youll find yourself with a tight-knit group of friends and family members who are ready to support you through even your very worst days. But no matter how well-intentioned those loved ones are, the only people wholl really get what its like to live with ulcerative colitis are other people who have it.
Even my best friend and my boyfriend will never understand what Ive gone through like my friends that have ulcerative colitis do, Skomski says. Until you live it, you dont know what it feels like to go through all those years of people not believing you, having the worst pain in your life that you have no understanding of. For a really long time, when I was in my denial phase, I thought, I dont need to have those people in my life, its just gonna make me feel like the sick girl all the time. But to have people that have gone through the same thing changed my life. I dont think I would be so positive and would embrace it as much as I do if it werent for having those people in my life that have the same disease as me.
It can also be such a relief to save valuable energy by skipping a few steps in the explaining process. Im so used to having to go through the whole song and dance of This is what I went through, Skomski says. When I connect with people that have ulcerative colitis, I dont have to do that. Its like a weird bond that I didnt know that I wanted or needed, but I definitely do.
Read Also: Symptoms Of Crohn’s And Ulcerative Colitis
Can I Get Surgery For My Ulcerative Colitis
Surgery is an option if medications arent working or you have complications, such as bleeding or abnormal growths. You might develop precancerous lesions, or growths that can turn into colorectal cancer. A doctor can remove these lesions with surgery or during a colonoscopy.
Research shows that about 30% of people with ulcerative colitis need surgery sometime during their life. About 20% of children with ulcerative colitis will need surgery during their childhood years.
There are two kinds of surgery for ulcerative colitis:
Proctocolectomy and ileoanal pouch
The proctocolectomy and ileoanal pouch is the most common procedure for ulcerative colitis. This procedure typically requires more than one surgery, and there are several ways to do it. First, your surgeon does a proctocolectomy a procedure that removes your colon and rectum. Then the surgeon forms an ileoanal pouch to create a new rectum. While your body and newly made pouch is healing, your surgeon may perform a temporary ileostomy at the same time. This creates an opening in your lower belly. Your small intestines attach to the stoma, which looks like a small piece of pink skin on your belly.
After you heal, waste from your small intestines comes out through the stoma and into an attached bag called an ostomy bag. The small bag lies flat on the outside of your body, below your beltline. Youll need to wear the bag at all times to collect waste. Youll have to change the bag frequently throughout the day.
Urgency To Pass A Stool

Not only will the stool consistency change if you have ulcerative colitis, but the urge to pass could hit suddenly and strongly even though nothing comes out. If you have inflammation in the rectum, you have this sense of needing to get rid of something, even though its not there, says Dr. Englander.
Read Also: Ulcerative Colitis And Colon Cancer Statistics
Read Also: Fda Approved Drugs For Ulcerative Colitis