Surgery For Ulcerative Colitis
Despite drug therapies, approximately one-third of people with ulcerative colitis will need surgery to treat the inflammation, prevent or treat cancer, or to treat a complication such as rupture of the colon. Surgery in which the entire colon is removed cures the person of their ulcerative colitis. In the past they were left with ileostomies, external bags into which the small intestine emptied. Surgical techniques have been developed, however, that now allow the colon to be removed without the need for an ileostomy.
Also Check: Prevention Of Diabetic Foot Ulcer
Inflammation In Other Areas
Some people with IBD have painful inflammation in other areas of the body, including:
- joints of the fingers, hands, feet, ankles and knees
- joints of the spine, including vertebrae and sacroiliac joints
Two specific skin problems that can occur as a result of IBD are:
- pyoderma gangrenosum small, sunken ulcers on the skin
- erythema nodosum painful, small, reddened nodules on the skin .
Poor Growth And Development
Ulcerative colitis, and some of the treatments for it, can affect growth and delay puberty.
Children and young people with ulcerative colitis should have their height and body weight measured regularly by healthcare professionals.
This should be checked against average measurements for their age.
If there are problems with your child’s growth or development, they may be referred to a paediatrician .
Read Also: Colitis Vs Ulcerative Colitis Symptoms
Not All Ibd Medications Linked To Increased Kidney Disease Risk
Azathioprine is linked to a slightly higher eGFR for patients with inflammatory bowel disease.
Ravy K. Vajravelu, MD
While the association between inflammatory bowel disease and chronic kidney disease is well known, how IBD medications increases the risk of CKD is not known.
A team of investigators from the Perelman School of Medicine at University of Pennsylvania, led by Ravy K. Vajravelu, MD, Division of Gastroenterology and Department of Medicine, determined whether IBD medications are linked to changes in estimated glomerular filtration rate , a key indicator of kidney function.
The investigators performed a retrospective cohort study of the data from The Health Improvement Network. A total of 17,807 patients with inflammatory bowel disease were included and matched for age, sex, and practice with 63,466 individuals without IBD.
The team used a Cox proportional hazards model adjusted for common chronic kidney disease risk factors calculate the relative hazard of chronic kidney disease for stages 3 through 5D in patients with inflammatory bowel disease.
They also evaluated the association of 5-aminosalicylates , azathioprine, and methotrexate with change in eGFR using a longitudinal model.
After controlling for the risk factors associated with chronic kidney disease, the investigators discovered inflammatory bowel disease is associated with the development of chronic kidney disease in patients between 16-77 years old.
How Does Ulcerative Colitis Increase The Risk Of Colorectal Cancer
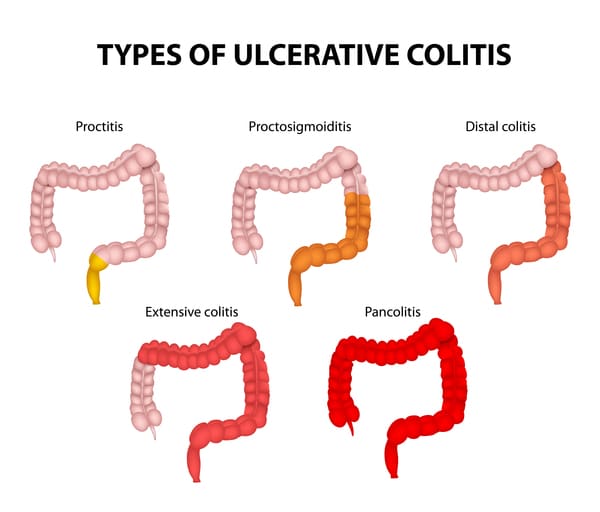
If you have ulcerative colitis, your risk of developing colon cancer is higher if you have the following conditions:
- An ulcerative colitis diagnosis at a young age
- Had ulcerative colitis for more than eight years
- Ulcerative colitis that affects most of your colon
- Uncontrolled inflammation
- Damage to your livers bile duct from inflammation or scarring
- Family history of ulcerative colitis
You May Like: What To Eat To Cure Ulcer
Crohns Disease And Ulcerative Colitis
A serious but rare complication of these forms of inflammatory bowel disease is fulminant or toxic colitis, formerly called toxic megacolon.
The signs and symptoms of this condition can include bloody diarrhea along with fever, racing heartbeat , low blood pressure , metabolic acidosis , low urine output , and acute kidney failure.
Toxic colitis is more common with ulcerative colitis than it is with Crohns disease.
Effects Of Crohns Disease And Ulcerative Colitis
Every person responds differently to IBD. The severity of symptoms will vary from time to time and from person to person. IBD is not a progressive disease . Rather, flare-ups can range from mild to severe and back to mild again. Some people will experience periods of relief from symptoms in between flare-ups.We cannot predict how long a person will stay free from symptoms, or when their next flare-up will occur. Some flare-ups settle down quite quickly with treatment. Other times, it may take months for a persons symptoms to respond to treatment.IBD interferes with a persons normal body functions. Signs and symptoms can include:
- pain in the abdomen
In addition to the above prevention methods, women can also:
- Avoid contraceptive methods that contain spermicide
- Avoid using a diaphragm as a birth control method
- Avoid the use of feminine products on genital regions, such as deodorant sprays and douches, which have the potential to irritate the urethra
- Receive vaccination against certain E. coli strains
You May Like: Treatment For Stomach Ulcers In Humans
Baseline Characteristics Of The Study Population
From January 2010 to December 2013, a total of 38812 patients with IBD were enrolled in the IBD cohort . Of these, 16606 patients were included in the IBD incidence group. The IBD cohort comprised 12585 patients with CD and 26227 patients with UC. The control group comprised 116436 age- and sex-matched subjects without IBD. Compared to the control group, the IBD cohort had significantly lower proportions of rural residents and individuals with incomes in the bottom 20% . Moreover, compared to controls, the IBD cohort had significantly lower prevalences of DM , hypertension , and dyslipidemia , and higher prevalences of congestive heart failure , ischemic heart disease , and gout and hyperuricemia . The CD and UC groups were not significantly different from controls in the trends of covariates, except for DM and dyslipidemia. Among the medications prescribed for IBD, 5-ASA, corticosteroids, immunomodulators, and anti-TNF- agents were prescribed to 36288 , 22284 , 10356 , and 2103 patients with IBD, respectively. The immunomodulators and anti-TNF- agents were used more frequently by patients with CD than by patients with UC .
Ibd And Changing Your Diet
Some dietary changes that may help a person with IBD include:
- Low-fibre diet when IBD is active, most people find a bland , low-fibre diet helps to ease diarrhoea and abdominal cramping. People with Crohns disease who have a narrowed small intestine may need to eat a low-fibre diet most of the time.
- Low-fat diet people with Crohns disease who experience steatorrhoea may benefit from a low-fat diet.
- Low-lactose diet the milk sugar lactose is broken down by the enzyme lactase, commonly found in the lining of the small intestine. Some people with Crohns disease lack this enzyme, so should avoid milk and other dairy products. Lactose intolerance can be diagnosed with a simple test ask your doctor.
- Liquid diet a person with severe Crohns disease may need a nutritionally balanced liquid diet.
- Plenty of water people with IBD need to drink plenty of fluids to prevent dehydration.
Don’t Miss: What Can I Do To Relieve Ulcer Pain
Can Ulcerative Colitis Cause Urinary Problems
Patients with inflammatory bowel disease and irritable bowel syndrome often show evidence of bladder hypersensitivity such as detrusor instability, nocturia, frequency and some forms of urinary urge incontinence, back pain and, in women, dyspareunia, leading to significant problems in diagnosis and
You May Like: Do Kidney Stones Pass Through The Bladder
When To Get Treatment
An increase in inflammation causes a flare, and the nature of inflammation means that you should treat it as quickly as you can. Inflammation grows exponentially, because inflammation itself causes an increase in inflammation. The longer you leave it untreated, the worse it will get. In addition, untreated inflammation not only leads to the symptoms associated with ulcerative colitis, it can also increase your risk of developing complications such as colorectal cancer down the line. Pay attention to your symptoms, and visit your physician if you notice that they change or increase even a small amount.
Don’t Miss: Hind Gut Ulcers In Horses Treatment
E Coli Infections Can Be Mild To Life
The strain of E. coli that most commonly causes hemorrhagic colitis is E. coli 0157:H7. Other strains of E. coli may also cause the infection, but they are hard to identify.
What makes these E. coli different from harmless E. coli is that they produce a toxin that damages the lining of the colon, causing inflammation and bleeding, says Dr. LoSavio.
Toxins are substances made by bacteria that are poisonous to humans. The toxin made by E. coli 0157:H7 is called Shiga toxin. Shiga toxin allows the bacteria to cling to cells lining the colon and cause inflammation and cell damage.
Shiga toxin can also cause red blood cells to die. The dead cells can overwhelm the kidneys and cause a dangerous complication called hemolytic-uremic syndrome . Deadly cases of E. coli colitis are usually due to HUS and are more common in children and the elderly.
Its hard to know how common E. coli hemorrhagic colitis is because many cases never get diagnosed. The Centers for Disease Control and Prevention estimate there are about 73,000 cases every year in the United States.
Taking Care Of Yourself
Its natural that living with ulcerative colitis can make you feel stressed at times. Stress can sometimes trigger flare-ups so you may find it helpful to try some relaxation techniques. These may include deep breathing, meditation, yoga and mindfulness.
Regular exercise can also help to give you a boost and make you feel better. It can also improve your general health and help to keep your bones and muscles strong. This is important because some medicines for ulcerative colitis may affect your bone health.
You May Like: Is Coconut Milk Good For Ulcerative Colitis
Recommended Reading: Does Stress Affect Ulcerative Colitis
Strategies To Reduce Your Risk Of Colorectal Cancer
Having regular colonoscopies is one of the most important preventive measures people with ulcerative colitis can take to reduce the risk of colorectal cancer.
There are also other steps people with UC can take to minimize risk, including avoiding smoking, limiting alcohol intake, maintaining a healthy weight, and exercising regularly.
Other tactics that have been shown to reduce the risk of colorectal cancer include the following:
Acute Kidney Injury In The Context Of Inflammatory Bowel Disease
Joana Cristóvão Marques1*, Rui Barata1, Joana Lemos Garcia2, David Navarro1, Mário Góis1,3, Helena Sousa1,3, Patrícia Cotovio1, Francisco Ribeiro1 and Fernando Nolasco1
1Nephrology Department, Hospital Curry Cabral, Centro Hospitalar Universitário de Lisboa Central, Lisboa, Portugal
2Gastroenterology Department, Instituto Português de Oncologia, Lisboa, Portugal
3Laboratory of Renal Morphology, Nephrology Department, Hospital Curry Cabral, Centro Hospitalar Universitário de Lisboa Central, Lisboa, Portugal
Read Also: What Not To Eat With Bleeding Ulcers
Don’t Miss: What Is The Treatment For Ulcerative Colitis
Q: Does Having Inflammatory Bowel Disease Affect My Risk For Developing Colon Cancer
A: Yes. If you go back 20 years, the thinking was that just ulcerative colitis was associated with increased risk of colon cancer. But weve found more recently that inflammatory bowel disease does have a higher risk than the general population.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services.Policy
There are two things we think about here when it comes to risk. The first one is the length of time that someone has had IBD. The second is the degree to which the bowel is affected. So patients that have had it longer and have more of their colon affected are at a higher risk and thats for both patients with Crohns and ulcerative colitis.
In people without inflammatory bowel disease, the pathway to cancer is pretty clear-cut, where you get a polyp, the polyp becomes dysplastic, and then ultimately you get cancer. But the IBD pathway can be different. So not only is it important that we control these patients inflammation, but also that we follow up with them at more frequent intervals to make sure they dont have cancer.
Read Also: Relief Of Pain Of A Lower Leg Ulcer
Study Population And Patient Identification
This study included all patients with IBD in the NHI database that were assigned both the V code and the ICD-10 code, from January 2010 to December 2013. The NHI and RID databases included patients with CD and UC . The IBD cohort was divided into an incidence group and a prevalence group. The IBD incidence group included all patients who were newly identified through both the ICD-10 and V codes for CD and UC, from January 2010 to December 2013. These patients had no history of CD or UC from January 2005 until the inclusion date of the study. The IBD prevalence group included all patients who were formerly assigned IBD codes, from 2005 to index day, and received reimbursements for IBD during the 2010 to 2013 period.
To assess the diagnostic accuracy of IBD defined with the V code and ICD-10 codes, the medical records of all patients with IBD were reviewed retrospectively at Seoul National University Hospital , a tertiary referral hospital in Korea. A total of 830 patients with IBD were enrolled at SNUH, based on both ICD-10 code and V code assignments, from January 2010 to December 2013. The diagnostic sensitivities for CD and UC were 94.5% and 96.4% , respectively. Age- and sex-matched individuals without IBD were randomly selected and included in the study at a ratio of 3 controls for each patient with IBD .
You May Like: Cranberry Juice And Ulcerative Colitis
Who Can And Cannot Take Tolterodine
Tolterodine can be taken by most adults. It can also be taken by children aged 2 years and over, on the advice of their specialist.
Tolterodine is not suitable for some people. To make sure its safe for you, tell your doctor or pharmacist before starting tolterodine if you:
- have ever had an allergic reaction to tolterodine or any other medicine
- have kidney or liver problems
- have myasthenia gravis, a condition that causes muscle weakness
Recommended Reading: Gastric Ulcer Treatment At Home
Vitamin And Mineral Supplements For Ibd
A person with IBD who eats a healthy, varied diet does not usually need to take vitamin supplements. But if they have a dietary deficiency, they may need tablets or occasional vitamin B12 injections. For example, a person on a low-fibre diet may need extra vitamin C and folic acid because they dont eat enough fruit and vegetables.A person with Crohns disease who experiences steatorrhoea may need calcium and magnesium supplements. Most children with IBD should take supplements to help them grow and develop normally.
Also Check: First Signs Of Ulcerative Colitis
Ulcerative Colitis Risk Factors
Most people with UC dont have a family history of the condition. However, about 12 percent of people with UC do have a family member with IBD, according to research from 2014.
UC can develop in a person of any race, but its more common in white people. If youre of Ashkenazi Jewish descent, you have a greater chance of developing the condition than most other groups.
Young people with IBD may also be dealing with acne at the same time. Some older studies have suggested a possible link between the use of the cystic acne medication isotretinoin and UC. However, newer research has yet to find a definitive causal relationship.
Theres no solid evidence indicating that your diet affects whether you develop UC. You may find that certain foods and drinks aggravate your symptoms when you have a flare-up, though.
Practices that may help include:
- drinking small amounts of water throughout the day
- eating smaller meals throughout the day
- limiting your intake of high fiber foods
- avoiding fatty foods
- lowering your intake of milk if youre lactose intolerant
Also, ask a doctor if you should take a multivitamin.
Mixing Tolterodine With Herbal Remedies And Supplements
There might be a problem using herbal remedies and supplements while taking tolterodine.
Some herbal medicines can make you feel sleepy, cause a dry mouth, or make it difficult to pee. Their effect is similar to tolterodine. This can increase your risk of getting side effects or make your side effects worse.
You May Like: Can Ulcers In The Esophagus Cause Cancer
Recommended Reading: How Do Stomach Ulcers Heal
Have A Uti It Could Be Related To Your Ibd Treatment
Many women will experience at least one urinary tract infection in their lifetime and men can experience UTIs, too. In fact, UTIs are the reason over 8.1 million people visit their doctor each year.1 But did you know that UTIs can be related to biologics for inflammatory bowel disease ?
While upper respiratory infections are a common side effect of biologics for IBD, most people dont know that UTIs are another type of infection that can be related to your IBD treatment, explains Faten N. Aberra, MD, MSCE, associate professor of medicine in the division of gastroenterology at the University of Pennsylvania in Philadelphia.
Why the increased risk? Biologics suppress your immune system increasing your risk of an infection like a UTI.
Read Also: Air Mattress For Decubitus Ulcers
Can Stomach Bloating Be A Sign Of Kidney Failure
My husband was diagnosed in October with stage 3 chronic kidney disease and has not yet been seen by kidney doctor I was not aware of his chronic kidney disease because his doctor never discussed it with me he went to his doctor on March the 20th and I didnt realize he had chronic kidney disease until around March the 27th when I called about his blood work and thats when they told me he was diagnosed in October we went on April the 20th 2018 for blood work at the kidney doctor he has an appointment on May 3rd for the results of his blood work but he keeps talking about hurting it in his stomach both sides underneath his rib cage he had a colonoscopy done
Read Also: Can Hemorrhoids Cause Abdominal Pain And Bloating
Don’t Miss: Wound Care For Venous Leg Ulcers