How Are Skin Lesions Diagnosed
In order to diagnose a skin lesion, a dermatologist or doctor will conduct a full physical exam. This will include observing the skin lesion and asking for a full account of all symptoms.
To confirm a diagnosis, they make take skin samples, perform a biopsy of the affected area, or take a swab from the lesion to send to a lab.
If you dont already have a dermatologist, you can browse doctors in your area through the Healthline FindCare tool.
Treatment is based on the underlying cause or causes of the skin lesions. A doctor will take into account the type of lesion, your personal health history, and any treatments previously attempted.
Symptoms Of Leg Ulcers
- that they are commonly found on the lower leg and ankle
- a sunken, asymmetrically shaped wound
- the edges of the ulcer are clearly defined from the surrounding skin
- the surrounding skin is intact, but inflamed
- the surrounding skin may be pigmented, hardened or calloused
- yellowish-white exudate
- varicose veins in the leg.
Primary Vs Secondary Skin Lesions
Skin lesions are either primary or secondary. Primary skin lesions are either present from birth or develop during your lifetime.
Secondary skin lesions arise from primary skin lesions. This can happen when a primary skin lesion is:
- Changes over time
For example, if eczema is scratched, a crust may form. The crust is a secondary lesion.
Don’t Miss: Treatment Of Ulcerative Colitis In Child
Can Venous Leg Ulcers Be Prevented
There are several ways to help prevent developing a venous leg ulcer in people at risk.
These include:
- elevating your leg when possible
- stopping smoking if you smoke
These measures are particularly important if you previously had a leg ulcer.
This is because you’re at increased risk of having another one in the same leg within months or years.
Swelling In The Legs And Ankles
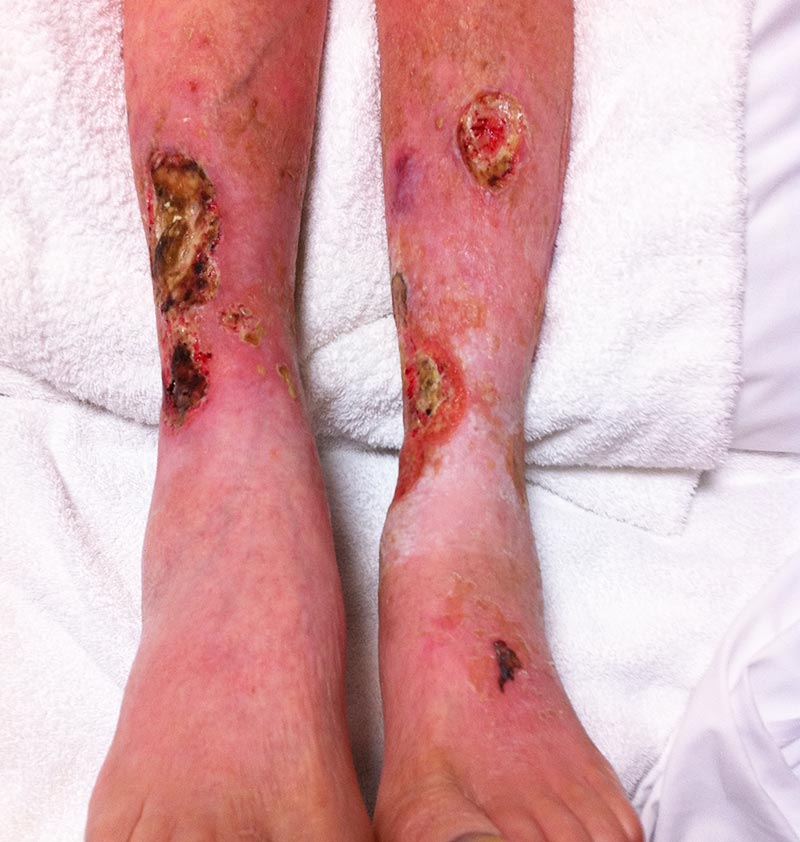
Venous leg ulcers are often accompanied by swelling of your feet and ankles , which is caused by fluid. This can be controlled by compression bandages.
Keeping your leg elevated whenever possible, ideally with your toes above your hips, will also help ease swelling.
You should put a suitcase, sofa cushion or foam wedge under the bottom of your mattress to help keep your legs raised while you sleep.
You should also keep as active as possible and aim to continue with your normal activities.
Regular exercise, such as a daily walk, will help reduce leg swelling.
But you should avoid sitting or standing still with your feet down. You should elevate your feet at least every hour.
Don’t Miss: How To Soothe An Ulcer
How Are Leg Ulcers Diagnosed
A vascular specialist a healthcare provider specializing in the circulatory system and knowledgeable about wound care can examine the ulcer. Your provider will examine your skin and the wound.
You may also get:
- Ankle-brachial index test, which uses ultrasound technology to measure blood pressure and blood flow in the legs.
- Biopsy to check skin cells and fluid from the wound for infections and skin diseases.
Symptoms Of Venous Leg Ulcers
Venous leg ulcers are open, often painful, sores in the skin that take more than a month to heal. They usually develop on the inside of the leg, just above the ankle.
If you have a venous leg ulcer, you may also have:
- discolouration and darkening of the skin around the ulcer
- hardened skin around the ulcer, which may make your leg feel hard or even resemble the shape of an upside-down champagne bottle
- a heavy feeling in your legs
- aching or swelling in your legs
- red, flaky, scaly and itchy skin on your legs
- swollen and enlarged veins on your legs
- an unpleasant and foul-smelling discharge from the ulcer
Don’t Miss: Ulcerative Colitis Abdominal Pain Relief
Looking After Yourself During Treatment
The following advice may help your ulcer heal more quickly.
- Try to keep active by walking regularly. Sitting and standing still without elevating your legs can make venous leg ulcers and swelling worse.
- Whenever you’re sitting or lying down, keep your affected leg elevated.
- Regularly exercise your legs by moving your feet up and down, and rotating them at the ankles. This can help encourage better circulation.
- If you’re overweight, try to reduce your weight with a healthy diet and regular exercise.
- Stop smoking and moderate your alcohol consumption. This can help the ulcer heal faster.
- Be careful not to injure your affected leg, and wear comfortable, well-fitting footwear.
You may also find it helpful to attend a local healthy leg club, such as those provided by the Lindsay Leg Club Foundation, for support and advice.
What Is The Treatment For Skin Ulcers
Treatment involves:
- Dressing the ulcer in a way that encourages wound healing.
- Painkillers if needed.
- Treating the underlying condition.
Treatment will be different depending on the underlying cause. For example, in venous ulcers, compression bandages may be helpful as they help circulation, whereas this treatment is not used for malignant skin ulcers.
Recommended Reading: Peptic Ulcer Vs Gastric Ulcer
What Are The Symptoms Of Leg Ulcers
A lower leg wound that doesnt heal with treatment after two weeks is the first indication of a leg ulcer. The sore may be red, purple, brown or yellow . Nonhealing sores on your legs often have a liquid discharge.
Other signs of a leg ulcer include:
- Dry, scaly or itchy skin.
- Hard bumps on the skin or hardened skin.
- Leg pain, especially after standing for a while.
- Red, blue or purplish skin color .
- Swelling in the lower legs.
How Venous Leg Ulcers Are Treated
Most venous leg ulcers heal within 3 to 4 months if they’re treated by a healthcare professional trained in compression therapy for leg ulcers.
But some ulcers may take longer to heal, and a very small number never heal.
Treatment usually involves:
- cleaning and dressing the wound
- using compression, such as bandages or stockings, to improve the flow of blood in the legs
Antibiotics may also be used if the ulcer becomes infected, but they do not help ulcers heal.
But unless the underlying cause of the ulcer is addressed, there’s a high risk of a venous leg ulcer coming back after treatment.
Underlying causes could include immobility, obesity, previous DVT or varicose veins.
Recommended Reading: Cold Laser Therapy For Ulcerative Colitis
Ulcers Caused By Problems With Blood Circulation
The blood supply coming to the skin is needed for the skin to heal after it has become broken or split for any reason. If there is a problem with circulation, the break in the skin does not heal, and may persist, leaving an ulcer. This may be a problem with the veins, the arteries, or the smaller blood vessels. The kinds of ulcers caused by circulation problems are:
- Venous ulcers. These ulcers and their treatment are described in the separate leaflet called Venous Leg Ulcers. They occur when the circulation in your legs is not working very well. Fluid tends to pool in the legs because the veins don’t work well enough to pump the blood efficiently back to the heart . This type of ulcer is more common in people with varicose veins that have lead to associated skin problems such as varicose eczema. They are also more common if you are overweight or obese, or not very mobile for any reason. They can also occur when the circulation is damaged by a deep vein thrombosis .
- Arterial ulcers. These are caused by conditions affecting arteries – see the separate leaflet called Peripheral Arterial disease.
- Vasculitic ulcers. These are caused by a number of conditions which cause blood vessels to become inflamed. This is called vasculitis.
What Are Skin Ulcers
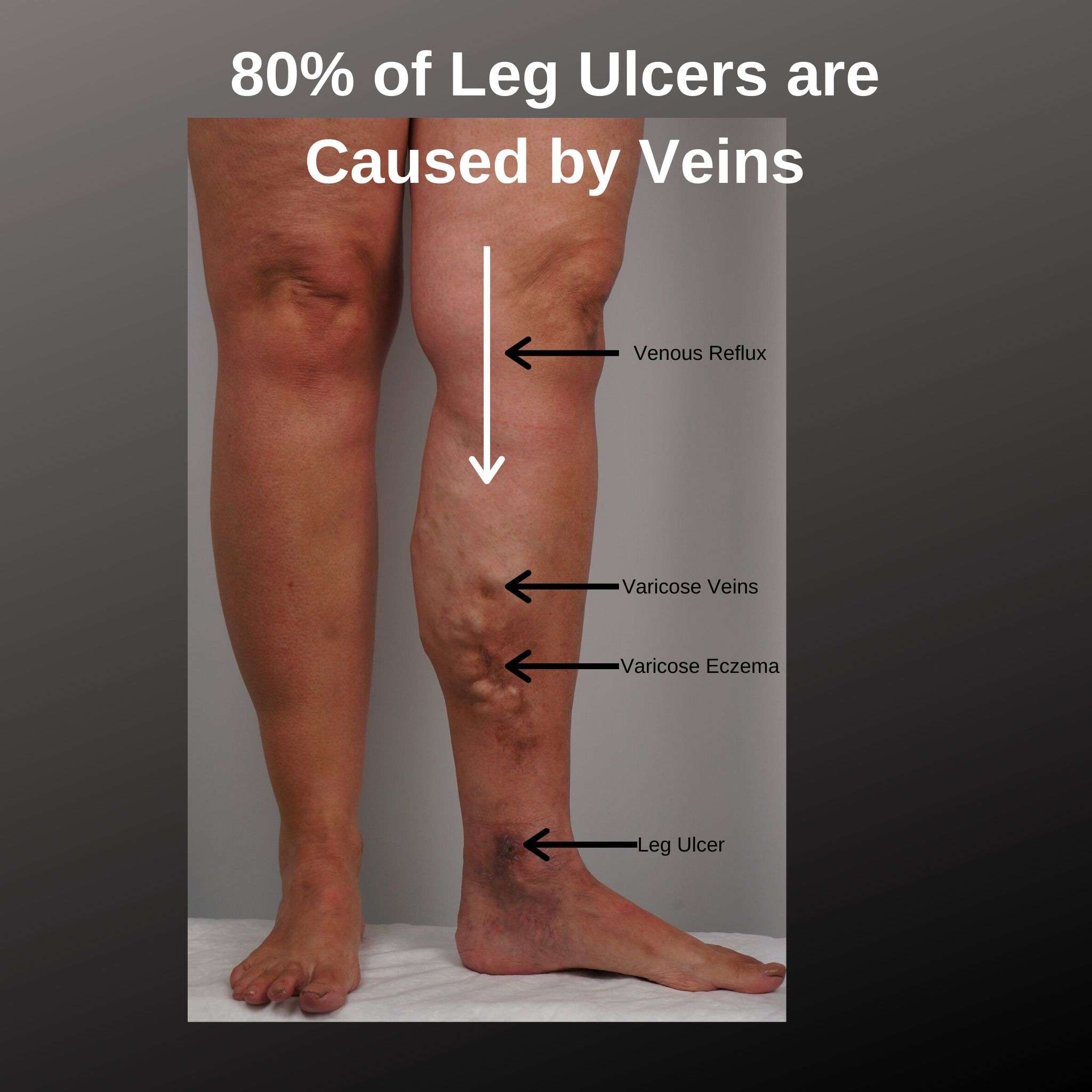
This is not a very pretty or fun topic to cover. However, we feel that it is necessary to make our readers more aware of Skin Ulcers. The fact that they affect so many people especially older populations brings the seriousness of these conditions to the forefront.
Skin ulcers are open sores caused by poor blood circulation. If you have poor blood circulation, then minor wounds may not heal properly leaving that injury to develop into a painful skin ulcer. These sores and ulcers often become infected if not properly treated. The infection, left untreated, can spread to deeper tissue, bones, joints, and blood resulting in a very serious issue where immediate medical attention is needed.
These ulcers can appear on most parts of the body. Common places include the legs, hips, feet, buttocks, and back. Skin ulcers are more likely to affect elderly people.
Don’t Miss: Possible Causes Of Ulcerative Colitis
Referral To A Specialist
In some cases, your GP or nurse may decide to refer you to a specialist in conditions affecting the blood vessels .
For example, you may be referred to a vascular specialist if your GP or nurse is unsure about your diagnosis, or if they suspect your ulcer may be caused by artery diseases, diabetes or rheumatoid arthritis.
After taking your medical history and examining you, the vascular specialist may need to arrange further investigations to plan your treatment.
About Venous Leg Ulcers
A leg ulcer is a long-lasting sore that takes more than 4 to 6 weeks to heal. They usually develop on the inside of the leg, just above the ankle.
The symptoms of a venous leg ulcer include pain, itching and swelling in the affected leg. There may also be discoloured or hardened skin around the ulcer, and the sore may produce a foul-smelling discharge.
See your GP if you think you have a leg ulcer, as it will need specialist treatment to help it heal.
Your GP will examine your leg and may carry out additional tests to rule out other conditions.
Read more about how a venous leg ulcer is diagnosed.
Also Check: Aip Diet For Ulcerative Colitis
Milia Or Tiny Epidermoid Cysts
Milia or tiny epidermoid cysts is a condition where small 1-2 mm white to yellow papules occur underneath the surface of the skin.
Common characteristics:
· These cysts can occur in all ages· They can be extracted without scarring· They are fixed and long-lasting· They often occur on the cheeks, eyelids, forehead, and genitalia.
How Can I Prevent Leg Ulcers
Leg ulcers commonly open up again after healing. These steps can lower the risk of getting a leg ulcer or a wound recurrence:
- Elevate your legs above your heart when youre sitting or sleeping.
- Maintain a healthy weight and stay physically active.
- Manage health conditions that affect blood circulation, including diabetes, high blood pressure, high cholesterol and Raynauds syndrome.
- Quit smoking and using tobacco products. Talk with your healthcare provider about ways to stop smoking.
- Use gentle cleansers, and apply moisturizing lotion to prevent dry skin.
- Wear compression stockings or bandages for an hour each day to improve blood flow to the legs.
Also Check: How Do You Heal A Bleeding Ulcer
What Are My Treatment Options
Treatment will depend on many factors, including the reason for the condition and your health status and history. Other factors your doctor will consider are:
- Your specific symptoms.
- How severe your condition is.
- How well you can tolerate medications or procedures.
The most common treatment for venous insufficiency is prescription-wear compression stockings, she says. These special elastic stockings apply pressure at the ankle and lower leg. They help improve blood flow and can reduce leg swelling.
You also can improve blood flow by keeping your legs elevated whenever possible, which means keeping them uncrossed when you are seated and by exercising regularly.
If you need medication, the most commonly prescribed include:
- Diuretics. These medications draw extra fluid from your body through your kidneys.
- Anticoagulants. These medications thin the blood.
- Pentoxifylline . This medication helps improve blood flow.
When To Call A Healthcare Provider
If the ulcer is large or deep, growing in size, incredibly painful, or if you have any signs of infection , you notice a bad smell coming from your ulcer, or you’re running a fever, call your healthcare provider right away.
You’ll also want to call your healthcare provider if your ulcer, no matter how minor, isn’t showing signs healing after a week to 10 days.
In most cases, the ulcer will be dressed to protect the wound. However, if your ulcer is draining considerably, your healthcare provider may recommend leaving the wound uncovered. Dressing the ulcer if it’s draining considerably can impede healing.
If your ulcer is painful, pain medication can be prescribed. Antibiotics may also be prescribed either prophylactically to prevent infection or to treat an already infected wound.
Debridement is done to remove dead tissue from more serious ulcers. For deep ulcers or those that aren’t healing after a long period of time, skin grafts may be needed. In the most severe cases, part of the foot, leg, or other appendage may have to be amputated.
Restoring good circulation is key in treating and preventing ulcers. This includes elevating the legs, wearing compression stockings, reducing pressure on ulcer-prone areas, superficial vein surgery. Leg ulcers, in particular, are incredibly likely to reoccur, so compression stockings are often needed to be worn for life.
Read Also: What Is The First Sign Of Stomach Ulcer
What Are The Symptoms
Skin ulcers look like round, open sores. They range in severity and are usually minor injuries on the skin.
In severe cases, ulcers can become deep wounds that extend through muscle tissue, leaving bones and joints exposed.
The symptoms of skin ulcers include:
- discoloration of the skin
People can develop the following types of skin ulcer:
What Are The Complications Of Leg Ulcers
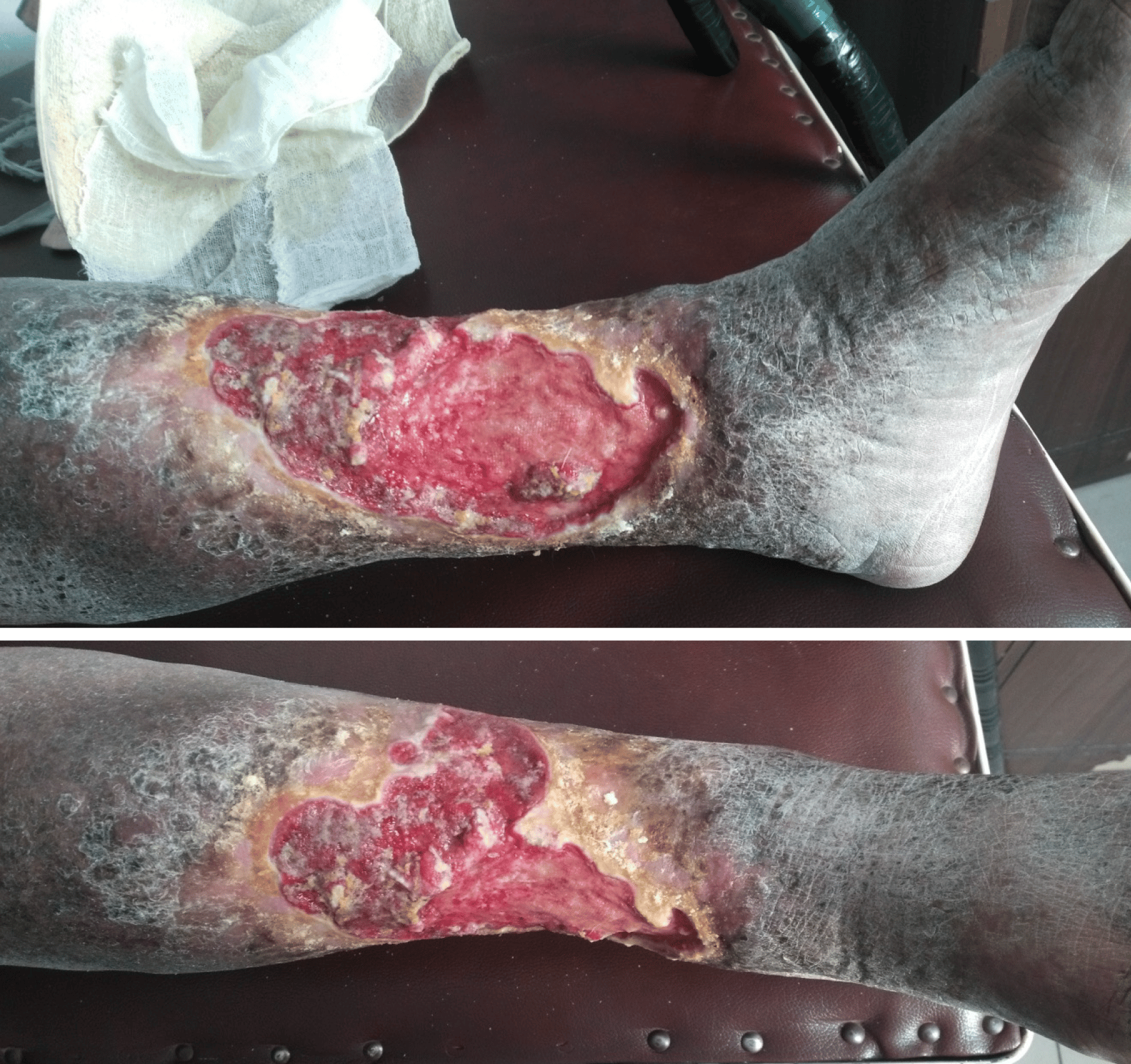
People with nonhealing wounds are at risk for:
- Bone infections such as osteomyelitis, which may lead to limb loss .
- Cellulitis, a potentially severe bacterial infection of the skin and layers beneath the skin.
- , a potentially life-threatening bacterial infection.
- Skin cancers like squamous cell carcinoma.
You May Like: Foot Ulcer Treatment At Home
Can Skin Ulcers Be Prevented
There are different strategies for preventing the different types of skin ulcers. Many can be prevented. For example:
- Avoiding excessive exposure to sun helps in avoiding cancerous skin ulcers – for example, protecting skin with sunscreen and/or clothing, and wearing hats where appropriate. See the separate leaflet called Sun and Sunburn.
- Ulcers related to diabetes can be prevented by good control of the diabetes through lifestyle and medication where required. If there are problems with feeling the feet then strategies to avoid injuring the feet without realising it help to prevent ulcers. For example, wearing well-fitting shoes and slippers, and inspecting the feet and legs regularly.
- Circulation in the legs is improved by regular exercise and keeping weight within a healthy range. Not smoking is also very important in maintaining a healthy circulation, as smoking is the main cause of peripheral arterial disease.
- Protecting skin from being dry and scaly – for example, with moisturising creams – helps to prevent the breaks in the skin which can lead to an ulcer. This is helpful particularly in people with varicose eczema or poor circulation.
- Avoiding the same position for long periods of time helps to prevent pressure ulcers. For those who are not very mobile, a health professional can advise on strategies to avoid pressure ulcers.
After The Ulcer Has Healed
Once you have had a venous leg ulcer, another ulcer could develop within months or years.
The most effective method of preventing this is to wear compression stockings at all times when you’re out of bed.
Your nurse will help you find a stocking that fits correctly and you can manage yourself.
Various accessories are available to help you put them on and take them off.
Page last reviewed: 11 January 2019 Next review due: 11 January 2022
Read Also: Pain Medicine For Ulcerative Colitis
What To Expect After Treatment With Cvm
At CVM, we’re ready to help diagnose and treat your leg ulcers at our select wound care locations:
Our expert team will carefully consider all potential chronic pelvic pain causes, with a special emphasis of diagnosing any potential vascular disorders.
We provide complete chronic pelvic treatment for pain. Aside from implementing innovative techniques to treat your pain, including treatments for vascular issues, we’re committed to listening to your concerns and treating your pain seriously. Many of our patients go on to have significant improvement or resolution of their symptoms.
Caring For Venous Ulcers
Venous ulcers need proper care and treatment to prevent infection and to heal. It’s important to have any venous ulcers checked right away by your healthcare provider.
Treatment may require focusing on the circulatory or vein problems that are causing the ulcers. Or it may mean removing some tissue around the wound. You may be asked to:
-
Clean the wound regularly
-
Apply a dressing to the ulcer
-
Avoid products that cause skin sensitivity
-
Wear compression stockings to prevent blood from pooling in the legs and to speed healing
-
Apply an antibacterial ointment or another topical medicine to prevent or treat an infection
-
Take oral antibiotic medicines to prevent or treat an infection
-
Have allergy testing done
Wearing a compression wrap to keep blood flowing back up to your heart can also help ulcers heal more quickly. In some cases, surgery or a skin graft is needed to close up the opening in the skin.
Don’t Miss: What Happens When You Have A Stomach Ulcer
Causes Of Venous Ulcers
Venous ulcers most often form around the ankles.
Venous ulcers typically occur because of damage to the valves inside the leg veins. These valves control the blood pressure inside the veins. They allow it to drop when you walk. If the blood pressure inside your leg veins doesn’t fall as you’re walking, the condition is called sustained venous hypertension. That increase in blood pressure causes ulcers to form on your ankles.
Venous ulcers may also be caused by other problems with your leg veins. These include:
-
Varicose veins. These are large, bulging leg veins. They occur when valves in the leg veins dont work well, allowing blood to collect in the lower leg.
-
Chronic venous insufficiency. Like varicose veins, this condition occurs when your leg veins cant pump blood back up to your heart. Blood then pools in your lower legs, causing your legs to swell. Since the blood can’t flow well in your legs, the swelling may be extreme. This extreme swelling can put so much pressure on your skin that venous ulcers form.