How Do H Pylori Cause A Peptic Ulcer And Peptic Ulcer Disease
H. pylori are spiral-shaped bacteria that can cause peptic ulcer disease by damaging the mucous coating that protects the lining of the stomach and duodenum. Once H. pylori have damaged the mucous coating, powerful stomach acid can get through to the sensitive lining. Together, the stomach acid and H. pylori irritate the lining of the stomach or duodenum and cause a peptic ulcer.
Donât Miss: Stomach Ulcer Treatment In Homeopathy
Does Acute Gastritis Cause Bleeding
Acute Gastritis generally cause bleeding, but it could be a sign of a more serious ailment. It could be a sign of a stomach ulcer or a perforated ulcer. To be sure, you should talk to a doctor. Before you visit your doctor, have a look at some of the symptoms of acute gastritis. Signs and symptoms of acute gastritis include: Your upper abdominal area aches Your upper abdomen feels full Food is regurgitated. Food is expelled through vomiting. Food is expelled through burping. Food is expelled through belching. Food is expelled in a lump. Food is expelled in a pile. There is a lump in the upper abdomen. The abdomen is tender to the touch. Pain in the chest radiates to the abdomen. Chest pain is associated with upper abdominal pain. The pain of the chest radiating to the back. There is bluish discoloration of the face. There is bluish discoloration of the lips. There is bluish discoloration of the nails. There is bluish discoloration of the fingers. There is bluish discoloration of the toes. There is a feeling of fullness in the abdomen. Abdominal pain is present on the right side. Abdom.
Can Diabetic Ketoacidosis Cause Black Stool
What effect does DKA have on the digestive system? The digestive symptoms of diabetic ketoacidosis are connected to the bodys effort to compensate for the shortage of useable glucose by burning fat instead of glucose for energy. Among these symptoms are the following: Pain in the abdomen. Mouth is parched.
Thousands of people suffering from erratic blood sugar has been using this ground-breaking solution
To help them burn away dangerous fat from their vital organs and bellies
While stabilizing their blood sugar levels naturally and effectively.
And starting today
Can diabetes have an effect on the bowels? When diabetes affects the nerves that connect to the stomach and intestines, food may be unable to pass properly. This results in constipation, but it is also possible to have alternating spells of constipation and diarrhea, particularly at night.
Is diabetes a possible cause of black stools? If a person has ingested any of these lately and their stool is black, there is probably no reason for alarm. According to the National Institute of Diabetes and Digestive and Kidney Diseases , bleeding in the digestive system may also result in dark, tarry stools.
Don’t Miss: Does Stomach Ulcer Cause Pain
How Does Gastritis Affect Bowel Movements
Gastritis sometimes affects the passage of bowel movements. The most common symptom of gastritis is stomach ache just before or just after eating food. This happens due to increased acid secretion in the stomach. The acid in the stomach reaches the duodenum within seconds while the food takes 10-15 minutes to reach the duodenum. This is the reason why people often experience pain while eating food. They also experience bloating, diarrhea, nausea, loss of appetite, vomiting, etc..
How Does Pediatric Ulcerative Colitis Affect My Childs Mental/emotional Health
Like many conditions, ulcerative colitis can have a negative psychological effect, especially on children. They can experience physical, emotional, social and family problems. Because of the medications and/or general stress from the situation, your child may experience:
- Worry about appearance and physical stamina.
- Vulnerability because their body doesnt function normally.
- Poor concentration.
- Misunderstandings with friends and family.
Children need mutual support from all family members. Its helpful for the entire family to learn about the disease and try to be empathetic. Seek out a psychiatrist and therapist to help your child manage such challenges of their ulcerative colitis.
Recommended Reading: How To Ease A Stomach Ulcer
Black Or Dark Red Blood In Stool
The longer blood is in the digestive tract, the darker it appears. Black, tarry stools are a sign of bleeding in the upper part of the digestive tract, such as the esophagus, stomach, and first part of the small intestine. Dark red blood in stool is a sign that bleeding may be in the small intestine or the beginning of the colon.
Causes of black or dark red blood in the stool may include:
- Inflammatory bowel disease
Of course, not all changes in stool color are due to underlying disease. Certain foods and supplements can also change the color of stool. For example, iron supplements and Pepto-Bismol are known to cause black stools. Black or dark red blood in the stool may also result from eating dark-colored foods like blueberries, black licorice, and dark chocolate.
Read Also: Nutritionist Specializing In Ulcerative Colitis
What Causes Gi Bleeding
Many conditions can cause GI bleeding. A doctor can try to find the cause of your bleeding by finding its source. The following conditions, which are listed in alphabetical order, include possible causes of GI bleeding:
Angiodysplasia. Angiodysplasia is when you have abnormal or enlarged blood vessels in your GI tract. These blood vessels can become fragile and bleed.
Benign tumors and cancer.Benign tumors and cancer in the esophagus, stomach, colon, or rectum may cause bleeding when they weaken the lining of the GI tract. A benign tumor is an abnormal tissue growth that is not cancerous.
Colitis. Ulcers in the large intestine are a complication of colitis. Ulcerative colitis is an inflammatory bowel disease that can cause GI bleeding.
Colon polyps.Colon polyps can cause GI bleeding. You can have more than one colon polyp at a time. Some types of polyps may be cancerous or can become cancerous.
Diverticular disease.Diverticular disease can cause GI bleeding when small pouches, or sacs, form and push outward through weak spots in your colon wall.
Esophageal varices.Esophageal varices can cause GI bleeding. Esophageal varices are usually related to a chronic liver condition called cirrhosis.
Esophagitis. The most common cause of esophagitis is gastroesophageal reflux . GER happens when your lower esophageal sphincter is weak or relaxes when it should not. Stomach acid can damage your esophagus and cause sores and bleeding.
Gastritis. Some common causes of gastritis include
Don’t Miss: Stelara Dosing For Ulcerative Colitis
How Do You Treat Melena
Diagnosis or treatment begins by identifying the sources of bleeding in order to determine and treat the underlying cause. An assessment of the individuals medical history is performed to identify related causes, such as chronic NSAID use. A lavage can be used to determine the severity of blood loss and to prepare the GI tract for endoscopy, which is a minimally invasive procedure used to look inside the . An upper endoscopy will often be performed to determine the exact source of bleeding.
Medication therapy with , such as or , can help reduce acid production, which encourages the healing of and thus reduces the risk of recurrent bleeding. Proton pump inhibitors, along with antibiotics, can also be used to treat infection, which is another potential cause of .
If necessary, the bleeding can be controlled through a combination of endoscopic therapies. The most commonly performed endoscopic therapy is injection therapy, in which medication is injected directly into the source of bleeding to encourage ” rel=”nofollow”> blood clotting). It is often combined with other endoscopic therapies, such as thermal techniques that apply heat probes to cauterize the bleeding, or mechanical techniques that apply pressure, using devices like clips or rubber band ligation.
Which Of The Following Is The Most Often Occurring Cause Of Diabetic Ketoacidosis
DKA is a condition of absolute or relative insulin insufficiency that is exacerbated by the subsequent hyperglycemia, dehydration, and acidosis-producing abnormalities in intermediate metabolism. The most prevalent reasons include an underlying infection, a disturbance in insulin therapy, or the acquisition of diabetes for the first time.
Also Check: Foods Bad For Ulcerative Colitis
Rectal Bleeding Tumors Colon Polyps And Other Causes
Polyps: Lumps of tissue or polyps bulge out from the lining of the colon. Bleeding occurs when large polyps develop, which can be hereditary. Usually harmless, some types can be precancerous.
Tumors: Both benign and malignant forms frequently appear in the colon and rectum. People older than 50 years of age are most affected. However, tumors also appear in younger people.
- Few people with tumor or polyps will have rectal bleeding. When bleeding does occur, it is usually slow, chronic, and minimal.
- If cancerous lesions are advanced, additional symptoms such as weight loss, a change in the caliber of stools, a sense of rectal fullness, or constipation may be experienced.
- Diagnosis requires evaluation with colonoscopy.
Trauma: Rectal bleeding from a traumatic cause is always a critical concern. Rectal damage from a gunshot wound or foreign body insertion can result in extensive infection or rapid and fatal blood loss. Prompt emergency evaluation is necessary.
Upper gastrointestinal source: A common source of rectal bleeding is bleeding from the upper gut, usually the stomach or duodenum. This can occur after someone has swallowed a foreign object that causes injury to the stomach lining, bleeding stomach ulcers, or Mallory-Weiss tears.
- Long-term, chronic alcohol consumption can also cause ulcers, esophageal varices, and gastritis. All of these upper GI tract problems can bleed so briskly that people may note blood in the stool or in the rectum.
Increase Dietary Fiber And Fluid Intake
According to the PubMed Health, fiber can help to soften stool and make them easier to pass. This can help to ease digestive discomfort and prevent conditions like constipation that can lead to enlarged hemorrhoids. It was reported that increased fiber in the diet also reduces the frequency of rectal bleeding and bloody stools.17
Always increase fiber slowly to prevent uncomfortable side effects, such as gas and bloating, constipation, diarrhea and abdominal pain.
For more information on how to increase dietary fiber in your diet and alleviate many digestive conditions, please read my articles about the best foods to cleanse your colon and how to effectively cleanse your colon with only 2 ingredients.
Read Also: Can I Donate Blood If I Have Ulcerative Colitis
Hemorrhoid Blood Clot Tips
Thrombosed hemorrhoids are the product of a blood clot forming inside of a external hemorrhoid.
External hemorrhoids can be painful and uncomfortable, and the formation of a blood clot inside of them certainly does not make it any better.
One of the most important things to remember is that a clot will usually go away on its own.
Dont try to pop a thrombosed hemorrhoid yourself, as you could develop an infection.
Instead, use wipes with witch hazel or creams designed for hemorrhoid relief to reduce swelling and discomfort.
Gently soak in a warm bath or a sitz bath for twenty minutes to alleviate the pain of a blood clot.
The best method of dealing with a blood clot is to see your physician or medical care provider.
Your blood clot may need to be lanced and drained, which is best left to a medical professional. Blood clots can leave behind a skin tag, and this can irritate through friction.
A proctologist or gastroenterologist should be able to help remove the blood clot safely and efficiently.
The most common procedures for removal of bloody hemorrhoids include:
Read Also: What Foods Can I Eat If I Have An Ulcer
How Can I Be Sure Its An Ulcer
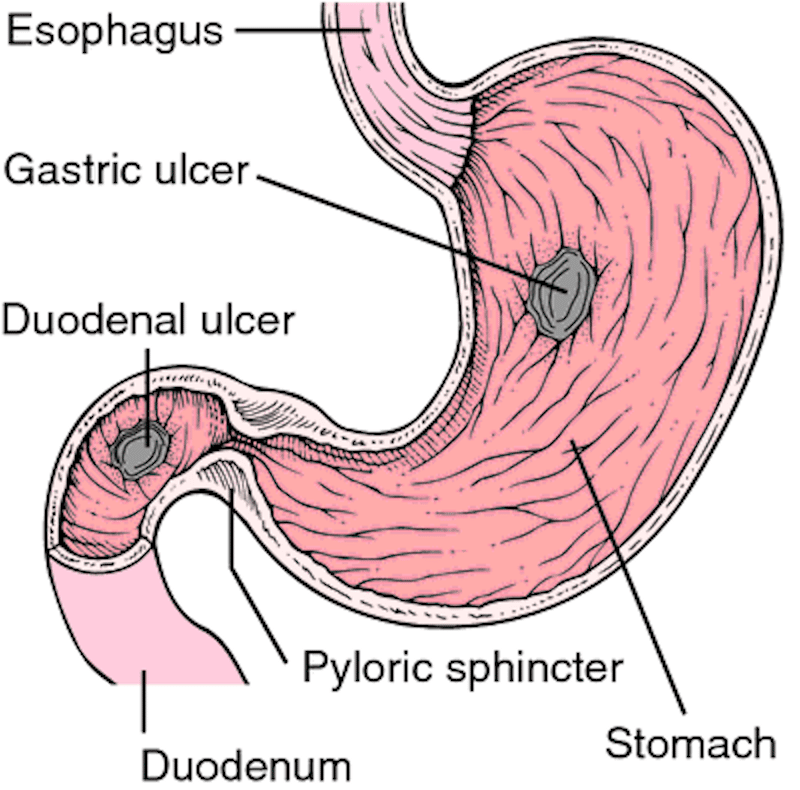
The only way to be sure an ulcer is causing your discomfort is with a medical diagnosis. We will evaluate your medical history and conduct a thorough physical examination.
To determine the root cause of your ulcer, we may run blood, stool, or breath tests. These tests are designed to look for signs of helicobacter pylori, the bacteria linked to ulcers.
Depending on your unique symptoms, we may also order an endoscopy. During an endoscopy, we insert a tube with a tiny camera down your throat and into your stomach to take pictures of any potential damage and collect tissue samples for analysis.
You May Like: Good Foods To Eat With An Ulcer
What Causes Bleeding From The Rectal Area
There are many causes of rectal bleeding. Common causes include hemorrhoids, , diverticulosis, infection, inflammation , blood vessel problems . Other causes of rectal bleeding include polyps, tumors, trauma, an upper gastrointestinal source like stomach ulcers, and Meckelâs diverticulum . Ischemia of the bowel occurs when blood flow to the bowel reduces or stops. For example, ischemic colitis usually occurs at the junction of the transverse and descending colon and can produce bright red or maroon blood. This article provides some of the details of the major causes of rectal bleeding.
Blood From The Stomach/small Intestine
This blood travels along the gut before it is passed out and the blood becomes dark and altered during this. Faeces can turn black or plum coloured- this is referred to a melaena. Bleeding stomach or duodenum should be immediately treated by the doctor, as it indicates internal bleeding.
When you have bloody stool, you may be asked about weight loss, family history of bowel disease, itching in the lower regions, diarrhoea or constipation. The doctor will also have toe examine you and diagnosis may require further tests than a mere physical examination or proctoscope.
Don’t Miss: Best Way To Treat Mouth Ulcers
Why You Should Never Ignore Blood In Your Stool
Its perfectly normal to feel concerned if you spot blood in your stool or on the toilet paper after wiping. Bloody stool isnt a normal occurrence and should be evaluated immediately. Whether you notice a faint red streak or dark blood in your stool, it can be a sign that something is amiss. If you ignore the symptom, whatever condition is causing it may get worse, so getting in to see a gastroenterologist can help get to the bottom of things.
At Digestive Disorders Associates, we see patients with a wide variety of digestive complaints and can provide a comprehensive evaluation for issues such as bloody stools. Sometimes theres an innocent explanation for finding blood in your stool. The only way to know for sure is to have a thorough examination.
Here are some of the possible reasons behind bloody stools.
Read Also: Compression Therapy For Venous Leg Ulcers
Can Stomach Olsers Cause A Lot Of Blood In Your Stool
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
HealthTap doctors are based in the U.S., board certified, and available by text or video.
You May Like: Classic Features Of Ulcerative Colitis
How To Prevent Gastrointestinal Bleeding
The prognosis for a person with GI bleeding depends upon the cause and location of the bleeding, how bad the bleed is when the person sees the doctor, and any underlying medical conditions that may affect the patients recovery.
-
Alcohol & Upper GI Bleeding
For those that consume alcohol, do so in moderation. Patients with high alcohol consumption are widely at risk for gastrointestinal bleeding within the upper digestive tract, which can result in death. Alcohol also accelerates the development of gastritis, which is an inflammation of the stomach lining. Over time, the inflammation can lead to erosion of the stomach lining, which plays a vital role in regulating stomach acid.
-
NSAIDs Increase The Risk Of Lower GI Bleeding
Non-steroidal anti-inflammatory drugs, or NSAIDS, are drugs that intend to reduce pain and fever, prevent blood clots, and reduce inflammation. They can also cause gastrointestinal bleeding, so it would be best to take these medications as rarely as possible. Examples of NSAIDs include ibuprofen, Advil, Motrin, aspirin, Celebrex, and Naproxin.
-
Can Smoking Cause Gastrointestinal Bleeding?
The risk of developing gastrointestinal bleeding increases significantly in individuals that smoke. Smoking not only causes peptic ulcers and other severe medical conditions, but it also can slow down the healing process for peptic ulcers. Furthermore, smoking interferes with ulcer medication, making the treatment less effective.
Other Causes And Factors
Other causes are rare. For example, some viral infections can cause a stomach ulcer. Crohns disease may cause a stomach ulcer in addition to other problems of the gut.
Stomach cancer may at first look similar to an ulcer. Stomach cancer is uncommon but may need to be ruled out if you are found to have a stomach ulcer.
If your stomach ulcers caused by a Helicobacter pylori bacterial infection, youll be given:
- a course of antibiotics
- a medication called a proton pump inhibitor
This is also recommended if its thought your stomach ulcers caused by a combination of an H. pylori infection and non-steroidal anti-inflammatory drugs .
You May Like: Can An Ulcer Cause Stomach Pain
How Would My Stool Look If I Had Rectal Bleeding
When you have blood in your stool it can look a few different ways. You may have bright red streaks of blood on your poop or you could see blood mixed in with it. Stool could also look very dark, almost black, and tarry.
Sometimes, you can have blood in your stool thats not visible. This is called occult bleeding. This can be a sign of bleeding inside your digestive tract. It can also signal a more serious condition like an inflammation disease in your intestines or cancer. Occult bleeding is usually found during lab tests that look at a sample of your poop to check for small amounts of blood. This is called a fecal occult blood test and it can be used as a way to screen for possible colorectal cancer. Your healthcare provider might recommend this if you have a family history of colorectal cancer.
One thing to keep in mind when you see an unusual color in your poop is what you ate. There are certain foods that can change the color of your stool and make it look red or even black. This is often mistaken for blood in your stool.