Patient Education And Support
Patient education and support are important components of our mission. We are committed to helping patients understand their disease, assess their treatment options, participate in their treatment decisions and feel in control of their disease.
If you are interested in obtaining more information about the various medical therapy for Crohns disease and ulcerative colitis, please click on the links below.
Our patients are welcome to attend the Crohn’s & Colitis Foundation of America support group, which holds regular monthly meetings at our center.
Meet Your Ibd Care Team
Video Length2:42
Meet your IBD Care Team If you or your loved one has IBD, you deserve the best care possible and that starts with finding the right healthcare professional or IBD specialist. Your IBD care team may include professionals from different medical specialties who work together to help improve your quality of life. Watch this video to meet some of the professionals who are part of the IBD care team.
The first step is to find a qualified gastroenterologist who is a specialist in treating patients with Crohns disease or ulcerative colitis. to learn more about how to find and communicate with an IBD specialist.
Below is a helpful tool to search for IBD care by specialty, name, state, or zip code. Our database consists of leading Crohns and colitis doctors, researchers, nurses, advanced practice providers, surgeons, dietitians, mental health providers, and other healthcare professionals working in the field who have chosen to become members of the Crohns & Colitis Foundation.
Please Note: We cannot make recommendations about your specific condition or guarantee that all members listed specialize in the treatment of Crohns disease or ulcerative colitis. The Foundation cannot attest to the credentials of its members, nor do we evaluate the competency of our members.
What Is The Best Medicine For Ulcerative Colitis
Treatment strategies for ulcerative colitis vary from person to person. Your doctor will base recommendations for medication on the intensity of your symptoms and severity of the disease. Drugs may be given as combination therapy or single drug therapy.
There are 6 types of medication used to treat UC.
Table: Medications for ulcerative colitis
| Drug | Oral or rectal | Examples |
|---|---|---|
|
Oral and rectal | |
|
Prescribed when previous medications are not effective |
|
|
| FDA-approved to treat moderate to severe | Oral | |
| Monthly shot or intravenous in a hospital setting |
|
|
|
If your body stops responding to medications or if you have emergency complications, you may need to undergo a surgical procedure to remove the affected part of the colon.
Don’t Miss: Where Do You Feel Pain With Ulcerative Colitis
Clinical Trials For Ulcerative Colitis
NewYork-Presbyterian investigators are conducting clinical trials to assess innovative therapies for ulcerative colitis. You may have the opportunity to participate in a clinical study evaluating a promising new treatment. If you are interested in learning more about current trials at NewYork-Presbyterian and other facilities across the nation, visit our Clinical Trials section.
Best Ulcerative Colitis Doctors Inphiladelphia Pa

We found 1310doctors who treat Ulcerative Colitis in Philadelphia.
Browse through a selection of 1310 Doctors who treat Ulcerative Colitis around Philadelphia, PA. Doctors who treat Ulcerative Colitis in this region have an average rating of 4.3 stars. Below are some of the best options around Philadelphia. The providers below have at least 11 or more past patient ratings, so you can be confident that these providers have the experience that you are looking for.
Don’t Miss: My Partner Has Ulcerative Colitis
Ulcerative Colitis Care At Rush
We are committed to being your partner in treating your ulcerative colitis and helping you avoid flares. Our team takes a holistic approach and includes you as part of our care team so we can offer the support you need to stay in remission longer.
This team includes the following experts who want to help you take control of your symptoms:
- A gastroenterologist who can diagnose your condition and provide access to investigational therapies and proven treatments like biologics that fight inflammation and reduce pain
- A dietitian who can help you create a diet plan so you can stay comfortable and healthy
- A psychologist who specializes in treating GI patients and understands your unique challenges
- A specialized IBD pharmacist to manage your biologic medications
If you need surgery to remove your large intestine, a surgeon can discuss minimally invasive and robotic surgical options to reduce pain and scarring, and help you recover faster.
What Should I Ask My Doctor
If you have ulcerative colitis, you may want to ask your healthcare provider:
- How much of my large intestine is affected?
- What risks or side effects can I expect from the medication?
- Should I change my diet?
- Will ulcerative colitis affect my ability to get pregnant?
- What can I do at home to manage my symptoms?
- What are my surgical options?
Read Also: Ulcerative Colitis Versus Crohn’s Disease
Women’s Reproductive Health Center
Together with Dr. Jeffrey Ecker, Dr. Allison Bryant Mantha and Dr. Kristen Eckler from the Mass General Department of Obstetrics and Gynecology, the Crohn’s and Colitis Center has a multidisciplinary approach to high-risk obstetrical care. Care of the patient with IBD contemplating pregnancy begins with pre-conception counseling to discuss the optimal timing for a safe and healthy pregnancy outcome, close monitoring throughout pregnancy, formulating an optimal childbirth plan, and post-partum care. Our surgeons are also specially trained in minimally invasive gynecological surgery and have expertise in the management of complex rectovaginal fistulas and urogynecological complications related to inflammatory bowel disease. We hold regular joint conferences with the Department of Obstetrics and Gynecology to discuss complex cases that require the input of expert gastroenterologists, obstetricians and gynecologists to ensure that a woman is receiving appropriate IBD care from reproductive age through menopause and before, throughout and after her pregnancy.
How Do Doctors Treat Ulcerative Colitis
Doctors treat ulcerative colitis with medicines and surgery. Each person experiences ulcerative colitis differently, and doctors recommend treatments based on how severe ulcerative colitis is and how much of the large intestine is affected. Doctors most often treat severe and fulminant ulcerative colitis in a hospital.
Also Check: What Should You Not Eat With An Ulcer
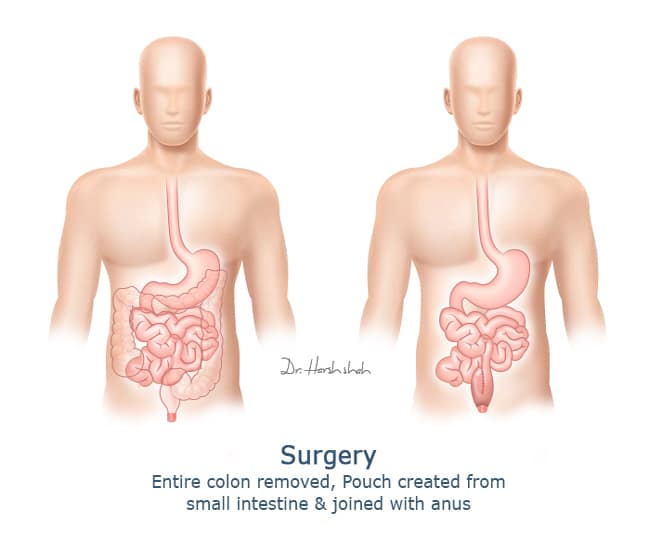
Surgical Removal Of The Colon Rectum
Surgical removal of the colon or the colon and rectum may be recommended to treat ulcerative colitis if:
- Medical therapy is no longer effective
- You are experiencing significant bleeding
- You face a risk of cancer
When the entire colon is removed, an opening called a stoma may be created in the abdominal wall, and an external pouch attached, which must be worn at all times.
Seek Care From An Ibd Specialist
Whether your disease is mild or complex, our gastroenterologists who specialize in IBD treatment can work with you to control your disease and its symptoms. We help restore your quality of life and watch for any complications related to the disease or its treatment.
Expertise in Diagnosing and Treating IBDDoctors from across the region refer their patients to us because of our expertise in diagnosing and treating IBD and its complications. If you are referred to us, we will partner with your current doctors to ensure you receive the best possible care. We also welcome people who are new to the Triangle and want to establish care with an experienced IBD provider.
Experience with Complicated ConditionsWhether you are newly diagnosed with Crohns or ulcerative colitis, or are seeking another opinion about your treatment, our IBD providers are ready to see you. We work with people who:
- Have complex IBD histories
Recommended Reading: How Many People Have Ulcerative Colitis
What Causes Ulcerative Colitis
UC affects the inner lining of the intestine, causing inflammation and ulcers. The disease is thought to be largely autoimmune in nature, which means your immune system malfunctions and attacks its own gut cells. Your body then produces substances that attack and damage normal intestinal cells and good gut bacteria.
While the cause of UC is unknown, suppressing the immune system can help symptoms subside and create longer periods of remission. When creating a treatment plan, your doctor will conduct thorough physical exams and blood tests to grade the disease and classify it as mild, moderate or severe. They will then prescribe medication accordingly.
World’s Best Specialized Hospitals 2021
In our nine decades, Newsweek has covered all aspects of health carescientific challenges, economic disruption, the occasional medical miracle and most of all, what these developments mean for our readers. As part of that commitment, we’ve partnered with Statista Inc., the global market research and consumer data firm, to rank the world’s best hospitals.
Now we’re expanding that expertise by looking at specialties. After the publication of the first part in September, in which we awarded the best hospitals for cardiology, oncology and endocrinology, we conclude this year’s ranking with the best hospitals for neurology, gastroenterology and orthopedics. Each list includes a ranking of the 50 best global hospitals, while ranks 51 to 100/200 are sorted alphabetically. If you or a loved one needs specialized care in one of those areas, as millions of us do, you want to know which hospitals or medical centers have state-of-the-art facilities and the most knowledgeable, accomplished physicians.
Where will you have access to the best diagnosticians, highest level of care and most effective treatments? We’re proud to offer our readers these independent, authoritative and reliable Newsweek/Statista rankings.
Methodology:
Hospitals which are not accessible to the public and/or are very small were excluded from the ranking since they were very unlikely to receive enough recommendations to make the final list.
Licensing Information:
Recommended Reading: Ulcerative Colitis Symptoms Mayo Clinic
Psychologist And Mental Health Care
Apart from the physical symptoms, Crohns disease and ulcerative colitis can also significantly impact one’s psychological status. Individuals with these conditions are at higher risk for depression and anxiety. Moreover, stress can also serve as a trigger for disease flares for some patients. The Crohns and Colitis Center provides both single and longitudinal consultations with psychologists and other behavior specialists in the management of chronic illness to address this aspect of care as well as food aversion that develops in the setting of IBD. We also provide cognitive behavioral therapy and facilitate other mind-body interventions to provide a holistic approach to the management of IBD.
How Is Ulcerative Colitis Diagnosed In Children
Diagnosing ulcerative colitis begins with an examination and a detailed medical history. Your childs clinician will rule out other possible causes and may recommend one or more of the following tests:
Drug therapy can reduce inflammation and control symptoms. Ulcerative colitis medications may include:
- anti-inflammatory drugs, such as steroids, to bring the disease under control
- immune system suppressants that can reduce swelling
- antibiotics to treat related complications, such as abscesses or fistulas
- antiulcer/H2 blockers to treat related ulcers and irritation
Recommended Reading: How Do You Know If You Have A Stomach Ulcer
What Are The Most Effective Treatments For Ulcerative Colitis
There are a variety of factors that can determine whether a specific medication can be effective at treating UC. Here are the most common medications for UC:
- 5-amino salicylic acid . This is the first-line treatment for UC. Commonly used medications are sulfasalazine, mesalamine, balsalazide, and olsalazine. The particular 5-ASA medication prescribed to a person with UC depends on the area of the colon thats affected by the condition.
- Corticosteroids. Corticosteroids, such as prednisone and budesonide, are another treatment for UC. These drugs cause significant side effects when used for longer periods, so theyre used only for moderate to severe illness.
- Immunomodulators. These medications minimize inflammation by controlling the immune response. Some common examples include cyclosporine, which is only used in short durations, as well as azathioprine and mercaptopurine. These two medications can cause side effects in the liver and require close monitoring of the blood by a physician.
- JAK inhibitors. The JAK inhibitor tofacitinib was approved recently for use in UC. It blocks an enzyme that can trigger inflammation.
- Biologics. Infliximab, adalimumab , and golimumab work by neutralizing proteins produced by the immune system. Another biologic, vedolizumab , targets the gut and helps reduce inflammation.
Untreated UC may progress over time, potentially becoming difficult to treat later on.
Treating UC can help minimize the risk of developing serious complications, including:
Biological Therapies For Inflammatory Bowel Disease
That includes the revolutionary development of biological therapies for IBD. Biological therapies are proteins that are made in living cells. There are now three classes of biological therapies available for Crohns disease and ulcerative colitis.
The first class, the anti-TNF class, includes drugs that block the bodys signals that fight infection or cause inflammation. By targeting the inflammatory protein called TNF, anti-TNF therapies can shut down inflammation broadly across the body. These drugs are also used to treat rheumatoid arthritis, psoriasis and other inflammatory conditions.
Another biological antibody therapy selectively targets the white blood cells on their way to the bowel. The newest antibody class targets a different inflammatory protein called IL-23, and works in IBD and psoriasis.
The strategy is to turn down the overactive immune response long enough so that the body can take over and then heal, Rubin explained.
Also Check: What Vegetables Are Good For Ulcerative Colitis
Research And Clinical Trials
At NYU Langone, we provide access to a full range of clinical trials in the treatment of IBD, making new investigational therapies available to our patients who have Crohns disease or ulcerative colitis. To learn more about any of our current trials, contact Ghoncheh Ghiasian, research program manager, at .
In addition, our basic science and translational researchparticularly in the areas of personalized treatment options, biomarkers, and infectious triggers of IBDcontributes to advancements in the prevention of IBD and the development of more effective treatments.
When Can You Leave The Hospital
You’ll be discharged from the hospital as soon as your symptoms respond to treatment. Your medical team will take different samples in order to look for signs of inflammation. They’ll also monitor your stool for consistency and track the frequency of bowel movements.
You’ll be allowed to leave as soon as your inflammation decreases, your stool thickens, and your number of bowel movements go down. Your doctor will only consider surgery if you don’t respond within the first five days of treatment or if an emergency condition develops.
After you leave the hospital, you should try to avoid situations that lead to flare-ups. This may involve dietary changes or stress-management techniques. Your doctor will decide on the best treatment plan for you after your hospital stay.
Also Check: Can Stomach Ulcers Be Cancerous
What Are Possible Complications Of Ulcerative Colitis
Ulcerative colitis is a long-term condition. It can lead to problems over time, including:
- Loss of appetite, leading to weight loss
- Hole or tear in the colon
- Colon infection
- Eating more frequent, smaller meals
- Keeping a food diary that identifies foods that cause symptoms
Nutritional supplements and vitamins may be advised if nutrients arent being absorbed. If you use complementary or alternative therapies, including dietary supplements and probiotics, tell your healthcare provider. This is important for ensuring safe care.
Ulcerative colitis requires long-term management. It can cause great physical, financial, and emotional stress to both the person and their family. If you or your family members are having trouble coping with this disease, ask your provider for resources. These can include mental health counselors or local and online support groups.
In some cases, your provider may ask you to avoid taking NSAIDs, pain medicines such as ibuprofen, naproxen, or similar. This is because these medicines can cause the ulcerative colitis to flare in some people.
The Emergency Room Is Scary For Someone With Ibd

As a person who suffers from inflammatory bowel disease, I can tell you that the emergency room is one of the scariest places to be. There are so many reasons for this that I want to briefly go into.
The first being, because of the complex nature of inflammatory bowel disease, most emergency room doctors arent very helpful. And even though many do understand IBD, they do not understand YOUR IBD. All of our stories and journeys with this illness are so different. For example, the medications we respond to, the type and amount of surgeries we have had, the extraintestinal manifestations of the disease that impact our individual bodies are just some of the things that need to be taken into account when a doctor is caring for you. We also know our bodies better than anyone which I think is a hard concept for a random doctor to grasp.
Also Check: Why Do I Keep Getting Mouth Ulcers
Recommended Reading: List Of Foods To Avoid With Ulcerative Colitis
You Can Use Telemedicine To Build A Strong Patient
Dont underestimate the importance of a good relationship with your doctor. When patients have good communication with their doctors, theyre especially likely to stick with their treatments and be more satisfied with their care, according to a review published in 2010 in The Ochsner Journal. If the communication between patient and doctor is poor, the patient can feel disheartened and may be less likely to stick with their treatment plan.
Both Battat and Chachu agree that combining in-person visits with telemedicine visits and the use of patient portals usually allows the doctor and patient to communicate with each other more effectively.
Its great to have access to both , as they each provide different options for patients, says Battat.
Complications of ulcerative colitis include:
- primary sclerosing cholangitis where the bile ducts inside the liver become damaged
- an increased risk of developing bowel cancer
- poor growth and development in children and young people
Also, some of the medications used to treat ulcerative colitis can cause weakening of the bones as a side effect.
Read Also: How Do You Cure Mouth Ulcers