Description Of The Condition
Venous leg ulcers are common and recurring complex wounds that heal by secondary intention . Problems with the leg veins reduce the efficient return of blood to the heart and increase the pressure in the veins , which may result in venous leg ulcers. The precise chain of events that links high venous pressures with skin breakdown and a chronic wound is not fully understood .
Venous leg ulcers commonly occur on the gaiter region of the lower leg . A venous leg ulcer is defined as any break in the skin that has either been present for longer than six weeks or occurs in a person with a history of venous leg ulceration. Differential diagnosis of the type of leg ulcer is made by taking a clinical history, physical examination, laboratory tests and haemodynamic assessment . True venous ulcers are moist, shallow and irregularly shaped and lie wholly or partly within the gaiter area of the leg. Leg ulcers can be associated with venous disease in combination with vascular disease, which impairs arterial blood supply in these instances they are said to have a ‘mixed’ aetiology . Open skin ulceration due solely to limb ischaemia from vascular disease is less common.
How To Heal Venous Leg Ulcers
This article was co-authored by . Marsha Durkin is a Registered Nurse and Laboratory Information Specialist for Mercy Hospital and Medical Center in Illinois. She received her Associates Degree in Nursing from Olney Central College in 1987.wikiHow marks an article as reader-approved once it receives enough positive feedback. In this case, 90% of readers who voted found the article helpful, earning it our reader-approved status. This article has been viewed 23,737 times.
A venous skin ulcer is a shallow wound that occurs when veins dont return the blood back to the heart the way theyre supposed to. These ulcers usually form on the sides of the lower leg, above the ankle, and below the calf. They can heal over time with proper care, but without it, they can return and/or cause serious complications.XTrustworthy SourceNational Health Service Public healthcare system of the UKGo to source It’s very important to see a doctor or wound care nurse when you have an ulcer, then to keep them dressed and bandaged, take the right medications, and alter some of your habits at home.
Treating The Ulcer Medically
Also Check: Venous Leg Ulcer Dressing Treatment
Treating An Infected Ulcer
An ulcer sometimes produces a large amount of discharge and becomes more painful. There may also be redness around the ulcer.
These symptoms and feeling unwell are signs of infection.
If your ulcer becomes infected, it should be cleaned and dressed as usual.
You should also elevate your leg most of the time. You’ll be prescribed a 7-day course of antibiotics.
The aim of antibiotic treatment is to clear the infection. But antibiotics do not heal ulcers and should only be used in short courses to treat infected ulcers.
Best Cream For Leg Ulcers
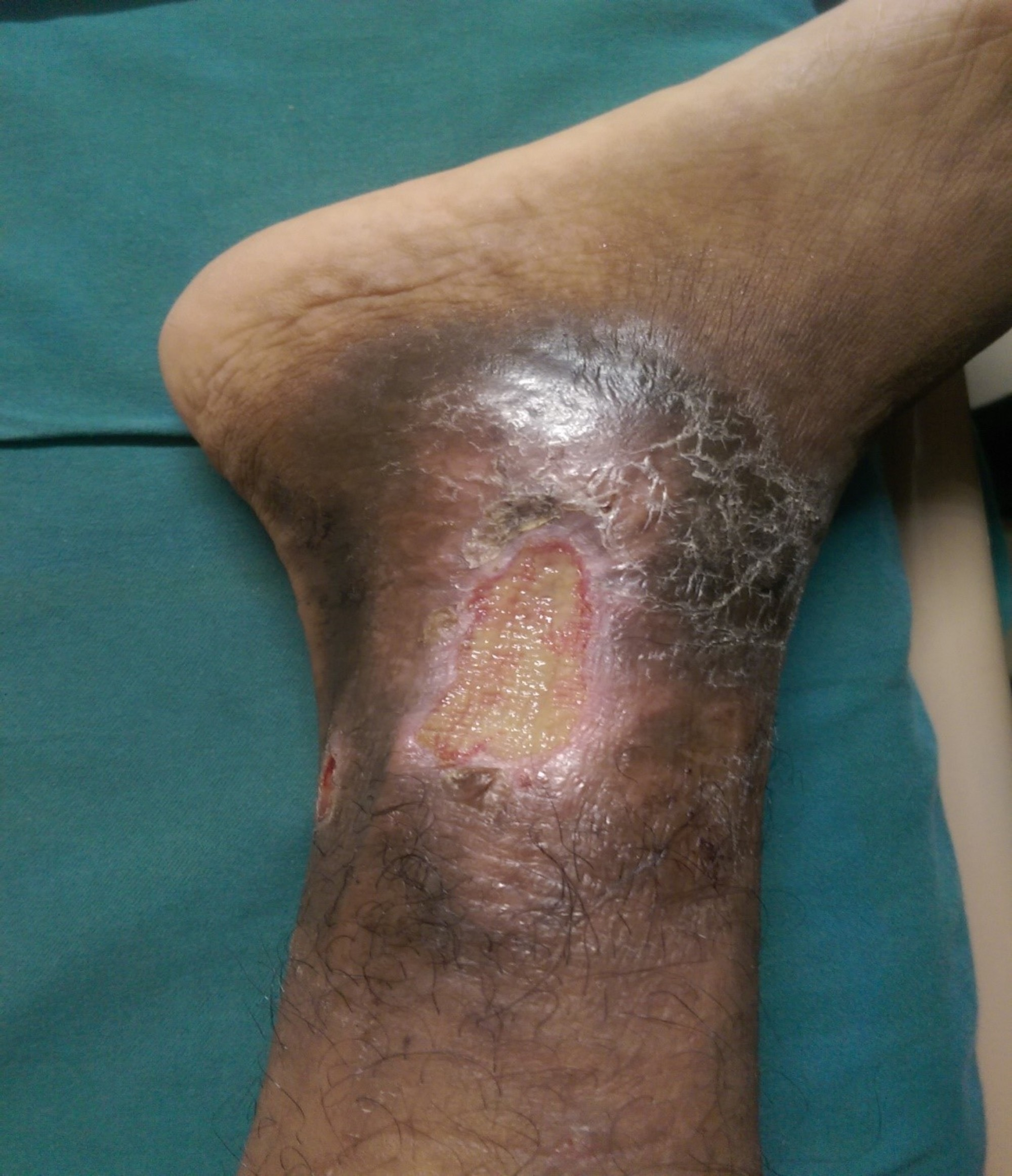
Many people suffer from leg ulcers. Leg ulcers are similar to a break in the skin of the leg, which allows air and bacteria to get to the underlying tissues. It can be formed by a minor injury that breaks the skin. It is also caused due to obesity, diabetes, and hypertension.
Contents
You May Like: Best Fiber Supplement For Ulcerative Colitis
Deep Vein Thrombosis Prophylaxis
The role of mechanical devices graduated compression stockings and intermittent pneumatic compression is dependent on the risk of venous thromboembolism in the medical or surgical patient. They may be used in combination with drug therapy or alone, especially if drugs are contraindicated because of an unacceptable bleeding risk. These mechanical devices are contraindicated in patients with severe peripheral vascular disease, severe leg deformity and severe peripheral neuropathy.
Evidence supports the use of graduated compression stockings as thromboprophylaxis for abdominal, cardiac, thoracic, vascular, major general or gynaecological surgery, neurosurgery and total hip replacement. Similarly, there is evidence for the use of intermittent pneumatic compression for total hip replacement, hip fracture surgery, total knee replacement, vascular, cardiothoracic surgery, neurosurgery, and for major gynaecological surgery. Graduated compression stockings should be measured for the individual and worn for as long as possible until the patient is fully mobile.20
Recommended Reading: Does Turmeric Help Ulcerative Colitis
What Can Cause Leg Ulcers
Venous hypertension / insufficiency the most common cause of poor healing on the lower leg is venous hypertension. This is when the veins struggle to take the blood back up the leg, so the blood can pool at the ankle creating pressure in your veins
Peripheral arterial disease another reason why our lower leg wound might not be healing is because not enough blood is getting down to our feet to heal the wound. This is then the opposite of the problem described above with veins.
Diabetes peripheral arterial disease is a known complication of diabetes, which can lead to developing a leg ulcer or diabetic foot ulcer.
Read Also: Bowel Ulcers Signs And Symptoms
Signs Of An Infection
A venous leg ulcer can be susceptible to bacterial infection. Symptoms of an infected leg ulcer can include:
- worsening pain
A number of factors can increase your risk of developing a venous leg ulcer, including:
- obesity or being overweight this increases the pressure in the leg veins
- if you have difficulty walking this can weaken the calf muscles, which can affect circulation in the leg veins
- previous deep vein thrombosis blood clots that develop in the leg can damage valves in the veins
- varicose veins swollen and enlarged veins caused by malfunctioning valves
- previous injury to the leg, such as a broken or fractured bone, which may cause DVT or impair walking
- previous surgery to the leg, such as a hip replacement or knee replacement, which can prevent you from moving about
- increasing age people find it harder to move around as they get older, particularly if they suffer from arthritis
Other Types Of Leg Ulcer
Other common types of leg ulcer include:
- arterial leg ulcers caused by poor blood circulation in the arteries
- diabetic leg ulcers caused by the high blood sugar associated with diabetes
- vasculitic leg ulcers associated with chronic inflammatory disorders such as rheumatoid arthritis and lupus
- traumatic leg ulcers caused by injury to the leg
- malignant leg ulcers caused by a tumour of the skin of the leg
Most ulcers caused by artery disease or diabetes occur on the foot rather than the leg.
Page last reviewed: 11 January 2019 Next review due: 11 January 2022
Don’t Miss: Best Way To Treat Mouth Ulcers
Who Gets Foot And Toe Ulcers
Youre at higher risk for foot and toe ulcers if you are:
- Native American.
- Male.
- Elderly.
If you have an eye, kidney or heart disease related to diabetes, youre also at a higher risk. About 15% of people with diabetes will get an ulcer, typically on the bottom of their foot. Around 6% of that 15% will have to be hospitalized because of complications.
Youre also at a higher risk of getting foot and toe ulcers if you have any of the following:
- Problems with circulation.
Dont Miss: Signs Of Ulcers In Humans
How Venous Leg Ulcers Are Treated
Most venous leg ulcers heal within 3 to 4 months if they’re treated by a healthcare professional trained in compression therapy for leg ulcers.
But some ulcers may take longer to heal, and a very small number never heal.
Treatment usually involves:
- cleaning and dressing the wound
- using compression, such as bandages or stockings, to improve the flow of blood in the legs
Antibiotics may also be used if the ulcer becomes infected, but they do not help ulcers heal.
But unless the underlying cause of the ulcer is addressed, there’s a high risk of a venous leg ulcer coming back after treatment.
Underlying causes could include immobility, obesity, previous DVT or varicose veins.
Read Also: Ulcerative Pancolitis With Rectal Bleeding
How Did You Implement The Project
Education and guidance was offered to all wound care clinicians. This covered information on how to use the pathway, appropriate product selection at the ideal time, and for the correct duration. This was coupled with a pathway launch day. Subsequent supportive visits from the tissue viability team and clinical specialist have taken place.
To support continuity, the leg ulcer pathway was designed as a booklet for use in all settings, for example at home in leg ulcer clinics district nurse clinics. It now contains QoL assessment tools, a treatment algorithm guidance for use, a leg ulcer assessment form and a wound treatment chart.
The data used for the analysis had been routinely collected for many years by the tissue viability team on a leg ulcer proforma. Verbal consent for treatment and use of data was gained from the patient. Any patient with a recurrence after a period of 2 weeks healed were included as a separate active ulcer. The inclusion criteria was patients with a completed leg ulcer clinic proforma who met the referral criteria, had an active leg ulcer, and attended their appointments.
We compared 2 periods of 12 months, the first was before the development of the leg ulcer pathway, and the second was a period of 12 months from the implementation date of the pathway.
Treatment What Treatment Will I Be Offered For My Leg Ulcer
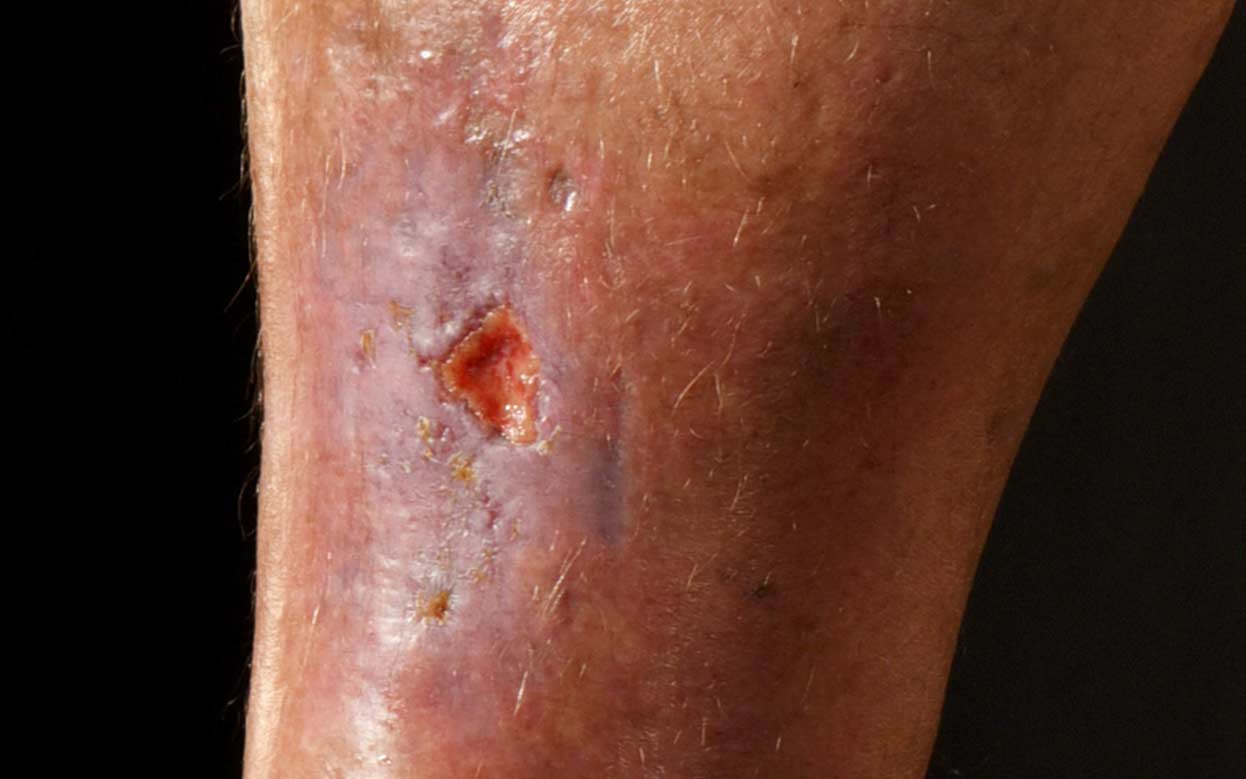
If your wound isnt healing because of venous hypertension and there are no problems with the blood supply to your legs, then you should be offered compression therapy.
Compression therapy improves blood supply by applying pressure to the leg. This can be done by bandaging the lower leg or by wearing supportive socks, stockings or tights. Compression therapy is very effective at reducing swelling, improving blood flow in the veins and healing or preventing sores or ulcers.
There are lots of different types of compression therapy so ask your nurse to find something that is right for you.
Compression can be a little uncomfortable when you first start treatment but should not cause you any pain. Any discomfort should reduce as the swelling goes down. If you do experience discomfort, talk to your nurse or doctor about it and they will advise you on ways of alleviating this.
In addition to the compression, your nurse should also advise you on wound care and dressings to keep your wound healthy.
Also Check: Foods To Avoid With Peptic Ulcer
Recommended Reading: How Do You Check For Ulcers
Does Cleaning Venous Leg Ulcers Help Them To Heal
Background
Leg ulcers are open skin wounds that develop below the knee, usually because blood flow is poor in the lower leg. This can occur because of blockages, for example when small blood clots form in the veins. It can also happen when the valves in the veins that prevent blood from flowing backwards stop working properly. Poor blood flow damages the skin and tissue, and creates venous leg ulcers.
Ulcers are unsightly and may become painful or infected. On average, ulcers take from six to nine months to heal. However, some ulcers can take years to heal, and a small number never do. Once ulcers have healed, they can reoccur.
The main treatment for venous leg ulcers is to use bandages or stockings that compress the leg , to increase blood flow in the veins. It is also thought to be important to clean the wound. Different types of cleaning solutions can be used, including: normal saline water antiseptics detergents or disinfectants .
Cleaning solutions can be applied to the ulcer using a swab , a syringe with a needle, or a spray canister. Ulcers can also be bathed in the cleaning solution, using a basin or bucket, or during a shower. Cleaning can cause discomfort, and may be painful.
What did we want to find out?
We wanted to find out:
– whether cleaning venous leg ulcers helps them to become smaller and heal
– whether some cleaning solutions, or methods of applying solutions, are more effective than others
– how much cleaning wounds costs and
Our methods
Basic Principles Of Compression Therapy
Depending on the position of the body, compression therapy improves venous return . The consistent pressure applied to the veins results in a decrease in vessel diameter, in reduced transmural pressure, and thus in a flow rate that is almost twice as high. In a lying position, pressure values as low as 15 mmHg are sufficient to constrict superficial and deep veins, which subsequently leads to an acceleration in blood flow. To achieve this while standing up, significantly higher pressure values are required . Compression with a stiff, rigid material provides stable support for the leg muscles, thereby increasing the effects of the muscle pump, which in turn results in improved venous return . The latter leads to edema reduction as well as pain relief. The question as to whether leg ulcer patients might potentially benefit from additional compression of the thighs cannot be unequivocally answered based on current literature. Although strong nonelastic thigh bandages may reduce venous return , there are as yet no reports on accelerated ulcer healing. Moreover, additional thigh compression is likely to result in poorer adherence, which has similarly been described for the use of thromboembolic devices and compression stockings for the prevention of PTS . Thus, although thigh compression may indeed be applied in individual cases, it is currently not recommended as standard treatment for venous leg ulcers.
Also Check: What Foods Are Good For Ulcers And Gastritis
Risk Factors For Leg Ulcers
- Age peripheral circulation becomes less efficient with old age.
- Varicose veins the one-way valves that stop blood from travelling backwards in the vein stop working. The pooling of blood stretches and distorts the vein.
- Cigarette smoking tobacco is known to constrict the vessels of the circulatory system.
- Arterial disease vein problems are more likely if the person already has other diseases of the arteries.
- Certain disorders these include diabetes and arthritis.
- Pressure sores bed-bound people are at risk of pressure sores, which are areas of damage to the skin caused by constant pressure or friction.
- Medication some cardiovascular medications can contribute to leg oedema and altered circulation.
When You Need More Treatment
If your wound doesnât heal in about a month or becomes an infection that spreads to the bone, you may need other treatments. These can include surgery and hyperbolic oxygen therapy, which involves breathing pure oxygen in a special room in order to help your body heal.
If your ulcer develops gangrene and your tissue dies, your doctor may have to amputate that area of your body.
Also Check: Children’s Mouth Ulcers Treatment
Four Categories Of Compression Hosiery
1) Support Wear:Contains a very mild compression of 8-5 mmHg
- Tired aching legs
- Mild swelling
- Prevention for people who are required to stand or sit in one position for long periods of time.
2) Medical Leg Wear:Available in compressions from 15-50 mmHg
- Management and prevention of venous leg ulcer minor to severe varicosities
- Minor to severe edema
- Pregnancy related edema and varicosities
- Lymphatic edema
- Management of Chronic Venous Insufficiency
3) Custom Wear:Available in compression of 15-90 mmHg
- Patients with abnormal limb shapes
- Patients who need an unlimited size range
- Patients who need specific garment options to improve compliance and fit
- Patients who need long-term management of lyphedema or vascular edema
4) Ulcer Care:Contains a compression of 40 mmHg
- Designed specifically for use with venous ulcerations
- Two-part system providing a total pressure of 40+ mmHg
- Liner holds dressing in place, is easy to put one, is worn 24 hours a day, facilitates donning of outer stocking
- Is used until the ulceration heals
- Outer stocking has zipper to facilitate donning and is worn during ambulation over the white liner
- Open toe stocking
A follow-up appointment is usually arranged after the hosiery has been fitted to ensure that the stocking is being used properly. Regular review may be required to check for any problems.Ideally, new hosiery should be re-ordered every four to six months.
Ten Top Tips On Leg Ulcers
Una Adderley04 Jun 2018
Don’t Miss: What Doctor Treats Ulcerative Colitis