How Are Foot Ulcers Treated
The treatment of foot ulcers varies depending on the cause of the ulcer.
Neurotrophic or diabetic ulcers: The main goal of treatment is to obtain wound closure. How treatment will be managed will depend on the severity and vascularity of the ulcer and whether there is any infection. Your doctor will advise you to rest and elevate the affected foot to relieve pressure.
Venous statis ulcers: Compression is applied to the leg to minimize edema or swelling. This can be achieved by wearing compression stockings,) multi-layer compression wraps, or wrapping an ACE bandage or dressing from the foot to just below the knee.
The type of compression that will be applied will depend on the ulcers characteristics and amount of drainage. After ulcer closure, compression stockings may help control the venous insufficiency.
Arterial or ischemic ulcers: Treatment depends on how severe the arterial disease is. Your doctor may recommend further testing to assess the potential for wound healing. Endovascular therapy or bypass surgery to restore circulation to the affected leg may be required.
Treatment often includes debridement of all necrotic, callused, and fibrous tissue, which is a mainstay of ulcer therapy.
After debridement, a saline wet-to-dry dressing is applied. If necessary, specialized footwear or bandages to relieve pressure on the ulcerated area may be prescribed. Infected ulcers are treated with antibiotics. Management of the underlying cause of the ulcer is essential.
When You Need More Treatment
If your wound doesnât heal in about a month or becomes an infection that spreads to the bone, you may need other treatments. These can include surgery and hyperbolic oxygen therapy, which involves breathing pure oxygen in a special room in order to help your body heal.
If your ulcer develops gangrene and your tissue dies, your doctor may have to amputate that area of your body.
How Do I Take Care Of My Ulcers
Your healthcare provider may teach you how to care for your ulcers at home. Some instructions may include:
- Wash the affected area with mild soap.
- Keep the wound clean and dry.
- Change the bandages as directed.
- Take prescribed medications as directed.
- Drink plenty of fluids. Ask your healthcare provider how much water you should drink every day.
- Follow a healthy diet, as recommended by your healthcare provider.
- Exercise regularly, under your healthcare providers care.
- Wear appropriate shoes.
- Wear compression wraps as directed.
Recommended Reading: Can You Give Blood If You Have Ulcerative Colitis
What Do Ulcers Look Like
Ulcers are wounds in your skin shaped like circles or ovals and can vary in size and color. When an ulcer starts you may notice:
- Dry skin.
- Redness.
- A rash.
As the ulcer gets worse, it can get wider, longer and deeper sometimes all the way down to the bone. In advanced stages you may see:
- A callus.
- A halo around the center that gets hard.
- Drainage in your sock, which may mean you have an infection.
- A brown discoloration.
Causes Of Diabetic Foot Ulcers
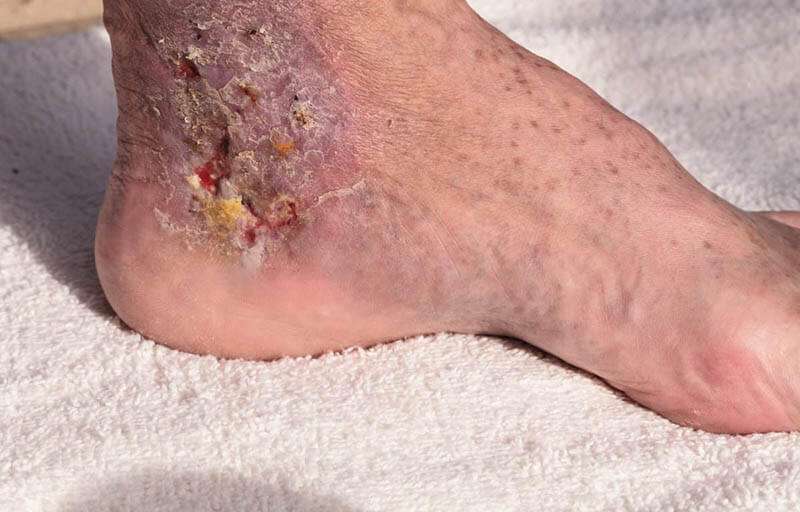
An ulcer is an open sore or wound on the skin. Ulcers on the feet are particularly common in those who have diabetes. Complications from the disease such as poor circulation and loss of feeling in the feet due to diabetes-related nerve damage make it more likely for a wound to develop, and also harder to heal.
People with diabetes who use insulin, have diabetes-related kidney, eye or heart disease, or who are overweight, use alcohol or tobacco have an even higher risk of developing foot ulcers.
Read Also: What To Take For Mouth Ulcers
Tips For Healthy Feet
Get to the bottom of any foot problems by using a mirror or asking for help.
Check your feet every day for cuts, redness, swelling, sores, blisters, corns, calluses, or any other change to the skin or nails. Use a mirror if you cant see the bottom of your feet, or ask a family member to help.
Wash your feet every day in warm water. Dont soak your feet. Dry your feet completely and apply lotion to the top and bottombut not between your toes, which could lead to infection.
Never go barefoot. Always wear shoes and socks or slippers, even inside, to avoid injury. Check that there arent any pebbles or other objects inside your shoes and that the lining is smooth.
Wear shoes that fit well. For the best fit, try on new shoes at the end of the day when your feet tend to be largest. Break in your new shoes slowlywear them for an hour or two a day at first until theyre completely comfortable. Always wear socks with your shoes.
Trim your toenails straight across and gently smooth any sharp edges with a nail file. Have your foot doctor trim your toenails if you cant see or reach your feet.
Dont remove corns or calluses yourself, and especially dont use over-the-counter products to remove themthey could burn your skin.
Get your feet checked at every health care visit. Also, visit your foot doctor every year for a complete exam, which will include checking for feeling and blood flow in your feet.
Be sure to ask your doctor what else you can do to keep your feet healthy.
What To Do If You Notice A Problem
The signs of diabetic ulcers on the foot should never be left untreated. If you have any of the symptoms mentioned above or think you might have a foot sore or ulcer, you should be seen by a doctor as soon as possible to avoid further damage and possible infection. The earlier you seek medical help, the less chance of complications further down the line.
Here at the Midwest Institute for Non-Surgical Treatment , we have qualified podiatrists who can provide you with the right treatment for your diabetic foot ulcer. We’ll also advise you on how best to look after your feet to prevent reoccurrences.
Book an appointment with Dr. Akinwande and the team who can treat you at one of our convenient locations in the St Louis area. Call us today, and we’ll get you back on your feet and the path to recovery.
Recommended Reading: Stage 2 Pressure Ulcer Characteristics
Choice Of Outcome Measure
The primary outcome in the types of study being described should be clinically relevant. In studies of people with active ulcers, the ulcer-centered outcome of choice is healing by a fixed time or time to healing. An alternative measure is to document change in cross-sectional area , and this may not always be easily accomplished because of the curved surfaces of the foot . As change in early-phase cross-sectional area has been shown to correlate with later healing , the chosen primary outcome may be a relative short-term reduction in ulcer area. It is less precise as a measure but can potentially allow exploratory studies to be conducted more quickly.
But when expressed in person-centered termswhich is generally preferablethe outcome should ideally refer not just to the healing of the index ulcer but to the patient being ulcer free . If such a person-centered outcome measure is adopted, it might be expressed in terms of time to being ulcer free, being ulcer free after a fixed interval , or ulcer-free days from the date of randomization to a fixed point . The use of ulcer-free days as a primary outcome is also valuable in studies of attempts to reduce ulcer recurrence, just as antibiotic-free days may be used in studies designed to prevent or treat infection and amputation-free survival in people with limb-threatening PAD.
Why Do Diabetics Get Foot Ulcers
Not all people living with diabetes get foot ulcers. However, if diabetes goes untreated or is managed poorly, issues like diabetic ulcers of the foot tend to be more common. Diabetic ulcers of the foot happen when the foot does not get proper circulation, and a combination of high blood sugar, irritated skin or tissue in the feet, and damaged tissue all combine to create the perfect conditions for foot ulcers.
Often, diabetic ulcers of the foot go unnoticed due to poor circulation and are only noticed after drainage, discoloration, and lumps form on the feet.
Recommended Reading: Can You Have An Ulcer In Your Colon
Tell Us About The Skin
Our research, for the first time, uncovered a skin-to-brain signaling pathway. It showed that the wound itself could cause subsequent central nervous system and behavioral changes.
We, and others, have observed behavioral and cognitive changes in our patients who have chronic wounds. It is unknown if the wound causes these changes, or they are just associated findings. The idea we proposed is that when a patient gets a wound that heals right away, there is not much sustained signaling of stress to the brain. But a chronic wound keeps activating the sensory receptors for painful stimuli , sending a more continuous skin-to-brain relay. This continuous flare generates brain signals of stress that are translated into behavioral changes.
We carried out research in mice and found that skin wounds result in a relay to the brain. This relay leads to the activation of stress markers, alteration of inflammatory mediators and changes in behavior and cognition. Mice with wounds showed more signs of despair and impaired memory than those with no wounds.
We often see similar behavior in patients with chronic wounds that need daily wound care. Some seem unable to attend to their wounds despite the serious risk of losing their foot to amputation. We also observe depression and cognitive disability reflected in the perception of inability to take care of their wounds. Some even seem to be disassociated from the reality of the serious nature of this problem.
How Can Diabetes Affect My Feet
Over time, diabetes may cause nerve damage, also called diabetic neuropathy, that can cause tingling and pain, and can make you lose feeling in your feet. When you lose feeling in your feet, you may not feel a pebble inside your sock or a blister on your foot, which can lead to cuts and sores. Cuts and sores can become infected.
Diabetes also can lower the amount of blood flow in your feet. Not having enough blood flowing to your legs and feet can make it hard for a sore or an infection to heal. Sometimes, a bad infection never heals. The infection might lead to gangrene.
Gangrene and foot ulcers that do not get better with treatment can lead to an amputation of your toe, foot, or part of your leg.A surgeon may perform an amputation to prevent a bad infection from spreading to the rest of your body, and to save your life. Good foot care is very important to prevent serious infections and gangrene.
Although rare, nerve damage from diabetes can lead to changes in the shape of your feet, such as Charcots foot. Charcots foot may start with redness, warmth, and swelling. Later, bones in your feet and toes can shift or break, which can cause your feet to have an odd shape, such as a rocker bottom.
Don’t Miss: How To Cure Tongue Ulcer
How To Spot Diabetic Foot Complications Early
Foot infections are among the most common health complications in people with diabetes. When a seemingly normal wound is left untreated, it can become severely infected.
We look at the reasons why diabetics should take special care of their feet.
Why diabetics are prone to foot conditions
Diabetics have abnormally high levels of glucose in their blood for long periods of time. This can lead to artery and nerve damage, which can compromise sensation in the feet.
When diabetics get a simple cut, scrape or foot ailment and they leave it untreated, it can lead to serious complications.
The two major conditions that can ultimately cause foot problems in diabetes are:
- Neuropathy occurs because of nerve damage, causing diminished sensation in the feet. This can lead to injuries such as wounds or scrapes getting infected.
- Peripheral vascular disease a condition that affects blood flow, making it more difficult for a cut or wound to heal.
“It’s not that these two conditions will cause ulcers as such, but they can result in extremely poor healing of any skin injuries. Often diabetics will have an injury, such as a blister or a cut, and because they have no feeling in that region, they do not realise that they have been hurt, and continue walking on an injured foot or leg,” says podiatrist Chris Delpierre.
The risk of foot ulcers and amputation
This research also states that the risk of amputation is 15 to 46 times higher in diabetics than in people who do not have diabetes.
Sensory And Autonomic Neuropathy
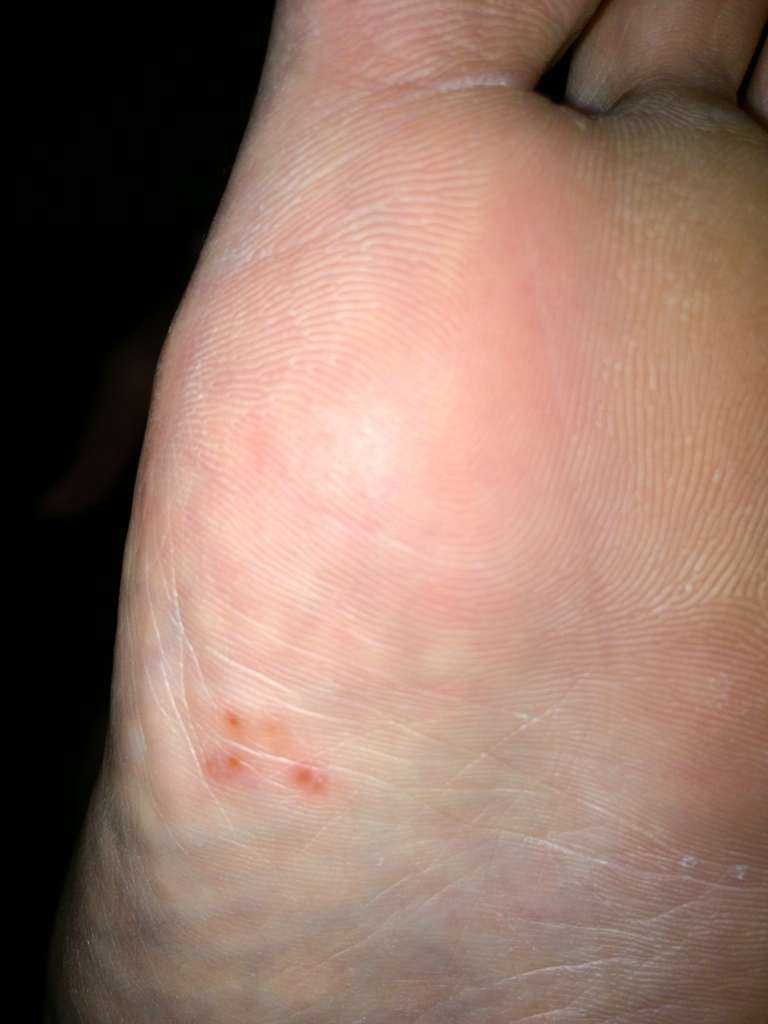
Distal symmetric polyneuropathy is perhaps the most common complication affecting the lower extremities of patients with diabetes mellitus. This complication occurs in up to 58 percent of patients with longstanding disease.19 Neuropathy, a major etiologic component of most diabetic ulcerations, is present in more than 82 percent of diabetic patients with foot wounds.4 This lack of protective sensation, combined with unaccommodated foot deformities, exposes patients to undue sudden or repetitive stress that leads to eventual ulcer formation with a risk of infection and possible amputation.20
In the diabetic foot, autonomic neuropathy has several common manifestations. First, denervation of dermal structures leads to decreased sweating. This causes dry skin and fissure formation, which predispose the skin to infection. In vascularly competent patients, this autosympathectomy may lead to increased blood flow, which has been implicated as one of the primary etiologic factors in the development of Charcot’s joint and severe foot deformity.2123
The nylon monofilament test is a simply performed office test to diagnose patients at risk for ulcer formation due to peripheral sensory neuropathy.24 The test is abnormal if the patient cannot sense the touch of the monofilament when it is pressed against the foot with just enough pressure to bend the filament25 . Physicians can obtain a monofilament kit at a small cost from the National Diabetes Information Clearing-house .
Read Also: How Can I Ease The Pain Of A Stomach Ulcer
Foot Ulcer Prevention Tips You Should Consider
People with diabetes and others who know they are at risk for foot ulcers should examine their feet daily and practice good foot hygiene.
Those with foot ulcers should keep the wound clean and dry, change the dressing as directed, take prescribed medications, maintain a healthy diet, and wear appropriate shoes.
Medical References:
Check Your Feet Every Day
You may have foot problems, but feel no pain in your feet. Checking your feet each day will help you spot problems early before they get worse. A good way to remember is to check your feet each evening when you take off your shoes. Also check between your toes. If you have trouble bending over to see your feet, try using a mirror to see them, or ask someone else to look at your feet.
Look for problems such as
- cuts, sores, or red spots
- swelling or fluid-filled blisters
- ingrown toenails, in which the edge of your nail grows into your skin
- corns or calluses, which are spots of rough skin caused by too much rubbing or pressure on the same spot
- plantar warts, which are flesh-colored growths on the bottom of the feet
- athletes foot
- warm spots
If you have certain foot problems that make it more likely you will develop a sore on your foot, your doctor may recommend taking the temperature of the skin on different parts of your feet. A hot spot can be the first sign that a blister or an ulcer is starting.
Cover a blister, cut, or sore with a bandage. Smooth corns and calluses as explained below.
Read Also: Can I Take Imodium If I Have Ulcerative Colitis
What Causes Foot And Toe Ulcers How Do You Get An Ulcer
There are many possible causes. The most common include:
- Neuropathy from diabetes.
- Peripheral arterial disease.
- Deformed toes.
- Walking in an odd way where you put too much pressure on one part of your foot or toe.
- Friction. Your foot or toe may rub against the toebox of your shoe.
Although they dont cause ulcers, foot and toe ulcers are often found alongside toe deformities such as hammertoe, mallet toe and clawtoe.
What Does A Diabetic Ulcer On The Foot Look Like
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
HealthTap doctors are based in the U.S., board certified, and available by text or video.
Don’t Miss: Eye Drops For Eye Ulcer
Signs & Symptoms Of A Foot Ulcer
A foot ulcer can be shallow or deep. When it starts, it looks like a red crater or dimple on the skin. If it becomes infected, it can develop drainage, pus, or a bad odor.
If you have nerve damage in your feet, then you won’t notice the pain of a small stone, too tight shoes, or the formation of a foot ulcer. As you get older or have a medical condition like diabetes or Raynaud’s phenomenon, it’s best to check your feet regularly for damage and sore spots and consult your doctor.
Venous ulcers – Patients with vein ulcers may complain of swollen, tired, and achy legs. Venous ulcers are not typically very painful unless touched, or unless they are infected.
Arterial ulcers – Patients with arterial disease may complain of tingling, burning, or coldness in the feet or toes. Patients may also experience leg pain when walking, or foot pain when elevating the legs. Ulcers usually occur at the tips of toes or on the sides of the ankles or lower calves. The ulcer may look punched out with a yellow-brown or black color. They are often very painful unless there is nerve damage.