Ulcerative Colitis Adversely Affects Many Patients And Current Treatments Are Relatively Ineffective
Ulcerative colitis adversely affects the quality of life of many patients with symptoms that include frequent diarrhea, urgent bowel movements, rectal bleeding, and fatigue. Patients quality of life and economic productivity are significantly impaired by chronic ulcerative colitis . This disease often strikes individuals in their teens and twenties, and continues to wax and wane for the remainder of their lives. The severity of the symptoms, as well as the unpredictability of flares of disease, can significantly impair the lives of those affected .
Current therapies for ulcerative colitis are only modestly effective, as up to 45% of patients eventually have total surgical removal of their colon . This is a daunting and irreversible choice for young patients to make. It is particularly difficult for young females, in whom the scarring of the pelvic organs after total colectomy can result in a three-fold increase in infertility . Therefore, it is quite important to evaluate all the symptoms that patients perceive as important in assessing disease activity, to determine whether the current medical treatment is truly effective.
Who Diagnoses Ulcerative Colitis
If you have symptoms of ulcerative colitis, your regular healthcare provider will probably refer you to a specialist. A gastroenterologist a doctor who specializes in the digestive system should oversee the care for adults. For young patients, a pediatric gastroenterologist who specializes in children should manage the care.
What Are Ulcerative Colitis Flare
With treatment , many people with ulcerative colitis will go into remission. That just means that you will have periods of time where your symptoms will be greatly reduced or nonexistent. That could mean weeks, months, or even years for some people, according to the Mayo Clinic. Unfortunately, ulcerative colitis flare-ups can occur. If you start feeling familiar symptoms like increased diarrhea, cramping, or rectal bleeding, let your medical team know.
Dr. Sinha says that sometimes symptoms can be more subtle during a flare, like bloating or fatigue. As far as triggers go, he says there are clear associations between IBD and stress. In my practice, I treat patients who are also students. Not uncommonly, we see students experiencing flares during exam times or other periods of high stress.
This is why, he says, its important that we not only consider medical treatments, but also take the overall picture into account, including diet, exercise, and other therapies.
Recommended Reading: How To Soothe Mouth Ulcers
When To Seek Medical Advice
You should see your GP as soon as possible if you have symptoms of ulcerative colitis and you havent been diagnosed with the condition.
They can arrange blood or stool sample tests to help determine what may be causing your symptoms. If necessary, they can refer you to hospital for further tests.
Read more about diagnosing ulcerative colitis.
If youve been diagnosed with ulcerative colitis and think you may be having a severe flare-up, contact your GP or care team for advice. You may need to be admitted to hospital.
If you cant contact your GP or care team, call NHS 24 111 service or contact your local out-of-hours service.
How Does Ulcerative Colitis Progress
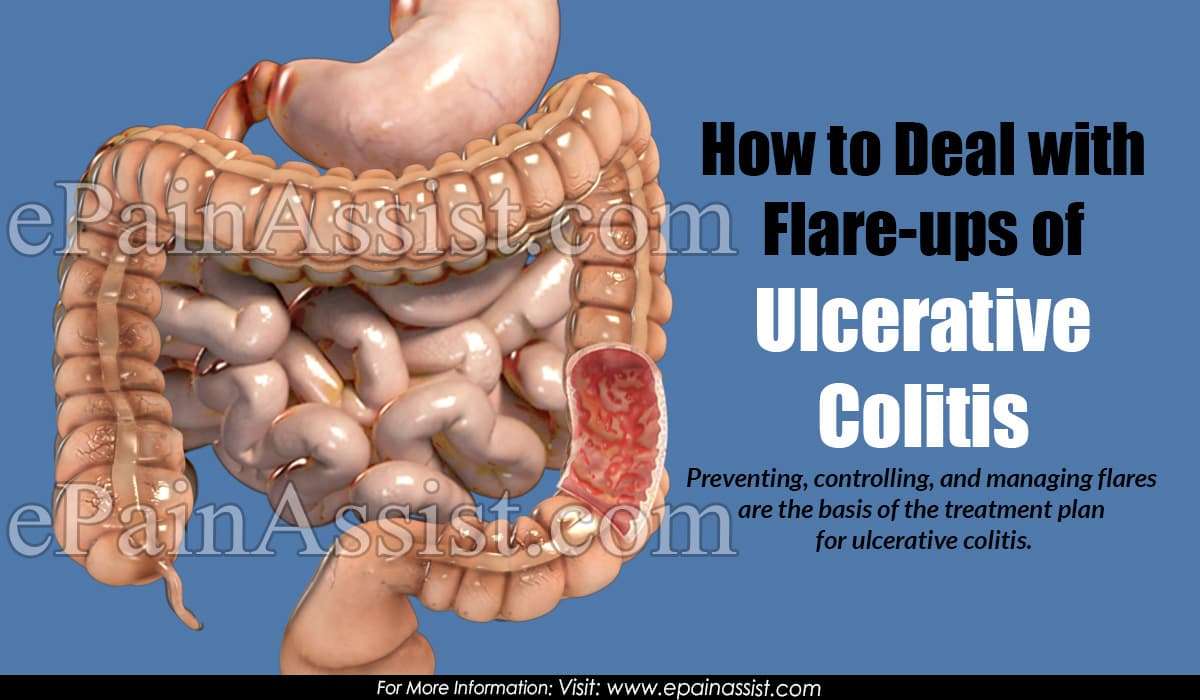
Ulcerative colitis is a chronic, relapsing condition. Chronic means that it is persistent and ongoing. Relapsing means that there are times when symptoms flare up and times when there are few or no symptoms . The severity of symptoms and how frequently they occur vary from person to person. The first flare-up of symptoms is often the worst.
It starts in the rectum in most cases. This causes a proctitis, which means inflammation of the rectum. In some cases it only affects the rectum and the colon is not affected. In others, the disease spreads up to affect some, or all, of the colon. Between flare-ups the inflamed areas of colon and rectum heal and symptoms go away. The severity of a flare-up can be classed as mild, moderate or severe:
- Mild – you have fewer than four stools daily and only have small amounts of blood in your stools. You do not feel generally unwell .
- Moderate – you have four to six stools a day, have some blood in your stools but do not feel generally unwell in yourself .
- Severe – you have more than six stools a day and have blood in your stools. You also feel generally unwell with more marked systemic disturbance with things such as high temperature , a fast pulse rate, anaemia, etc.
Read Also: Does Smoking Cause Ulcers After Gastric Bypass
How To Calm An Ulcerative Colitis Flare
This article was co-authored by Peter Gardner, MD. Peter W. Gardner, MD is a board certified physician who has practiced Gastroenterology and Hepatology for over 30 years. He specializes in diseases of the digestive system and liver. Dr. Gardner earned his Bachelors degree from the University of North Carolina and attended Georgetown Medical School. He completed his residency in Internal Medicine and then his fellowship in Gastroenterology at the University of Connecticut. He is a previous Chief of Gastroenterology at Stamford Hospital and remains on the staff. He is also on the staff of Greenwich Hospital and New York Presbyterian Hospital. Dr. Gardner is an Approved Consultant in Internal Medicine and Gastroenterology with the American Board of Internal Medicine.There are 8 references cited in this article, which can be found at the bottom of the page.wikiHow marks an article as reader-approved once it receives enough positive feedback. In this case, 100% of readers who voted found the article helpful, earning it our reader-approved status. This article has been viewed 9,951 times.
Who Develops Ulcerative Colitis
About 2 in 1,000 people in the UK develop ulcerative colitis. It can develop at any age but most commonly first develops between the ages of 10 and 40. About 1 in 7 cases first develop in people over the age of 60 years. Non-smokers are more likely than smokers to develop ulcerative colitis. However, smoking brings other dangers to health which far outweigh this benefit.
Don’t Miss: What Is A Decubitus Ulcer Why Does It Occur
What Can I Expect If I Have A Diagnosis Of Ulcerative Colitis
Ulcerative colitis is a lifelong condition that can have mild to severe symptoms. For most people, the symptoms come and go. Some people have just one episode and recover. A few others develop a nonstop form that rapidly advances. In up to 30% of people, the disease spreads from the rectum to the colon. When both the rectum and colon are affected, ulcerative symptoms can be worse and happen more often.
You may be able to manage the disease with medications. But surgery to remove your colon and rectum is the only cure. About 30% of people with ulcerative colitis need surgery.
Rapid Bowel Movements After Eating
The concern among participants that eating anything results in the need to have a bowel movement has also been supported during a flare.
I dont eat breakfast because I know within so many minutes of eating that I will need to go the bathroom.
When Ive got a flareup going, I mean, its always, I eat, and then half an hour later Im in the bathroom.
Recommended Reading: Are Mouth Ulcers A Sign Of Hiv
Check Out Some Relatable Situations And How To Deal With Them
Everyday struggles can come with having ulcerative colitis like socializing or traveling. But the best way to navigate life with UC is to seek an effective treatment plan. Beyond that, its helpful to maintain a hopeful outlook, healthy lifestyle, and strong support networkand strive to lead a full life.
Layers Of The Bowel Wall
The walls of your bowel have layers. The inner layers take in nutrients from food. The outer layers help move food through the gut and waste out of the body.
In Colitis, theres inflammation and swelling of the inner layer of the bowel wall. This can cause bleeding. More mucus may be produced by the inner layer of the bowel wall. Ulcers develop on the inner layer as the condition gets worse, but they can also go as the condition gets better.
The inflammation in Colitis affects how your body digests food, absorbs nutrients and gets rid of waste.
Everyone experiences Colitis differently. When youre having symptoms, its known as active disease, a flare-up or relapse. Symptoms may be mild or severe and are likely to change over time.
Your symptoms may vary depending on where Colitis is active in your bowel and how severe it is. Find out more in the section Types of Colitis.
The most common symptoms are:
Andy
Living with Colitis
You May Like: Does Gluten Affect Ulcerative Colitis
Do Different Types Of Ulcerative Colitis Cause Different Symptoms
Certain symptoms may point to different types of ulcerative colitis. These types, as outlined by the Mayo Clinic, are classified by location within the body:
- Ulcerative proctitis: With this form of the condition, which tends to be the mildest, a person has inflammation in the area closest to the rectum. Rectal bleeding may be the only sign of the disease.
- Proctosigmoiditis: Inflammation with this form of the disease involves a persons rectum and lower end of the colon. Symptoms can include bloody diarrhea, abdominal pain, and an inability to go despite feeling like you need to let loose.
- Left-sided colitis: This involves inflammation from the rectum, through the lower colon, and into the descending colon. In addition to bloody diarrhea and abdominal pain on the left side, you may also experience weight loss. Most patients will have left-sided disease, Dr. Sinha says.
- Pancolitis: This usually impacts a persons entire colon, causing bloody diarrhea that can be severe, abdominal pain, fatigue, and rapid weight loss.
Easing Symptoms During A Flare
The below suggestions can also help ease symptoms or help keep your body healthy during a flare-up.
Drink water: In UC, the large intestine can have a hard time absorbing water and salt, which can contribute to diarrhea and dehydration. Drinking plenty of water or an electrolyte replacement drink can help avoid dehydration if you’re experiencing a flare.
Eat plain, easy-to-digest foods: During a UC flare, it’s common to lose your appetite. To keep your energy levels up and avoid malnutrition and weight loss, it’s important to continue to fuel your body with food. Unfortunately, fruits and vegetables, particularly when raw, are bothersome for many people with UC. Avoid fatty and greasy foods as well. Your doctor may also suggest meal replacement drinks if you’re losing weight from UC flare-ups.
Get some exercise: If you’re experiencing symptoms like stomach pain and diarrhea, exercise may sound like the last thing you want to do. But in addition to the well-known mood and health-boosting benefits of exercise, a workout can also have specific benefits for UC symptoms. Uncontrolled inflammation in the intestinal tract leads to UC symptoms. Exercise has an anti-inflammatory effect that can help these symptoms.
Read Also: Best Natural Remedies For Stomach Ulcers
How Is Ulcerative Colitis Treated
Theres no cure for ulcerative colitis, but treatments can calm the inflammation, help you feel better and get you back to your daily activities. Treatment also depends on the severity and the individual, so treatment depends on each persons needs. Usually, healthcare providers manage the disease with medications. If your tests reveal infections that are causing problems, your healthcare provider will treat those underlying conditions and see if that helps.
The goal of medication is to induce and maintain remission, and to improve the quality of life for people with ulcerative colitis. Healthcare providers use several types of medications to calm inflammation in your large intestine. Reducing the swelling and irritation lets the tissue heal. It can also relieve your symptoms so you have less pain and less diarrhea. For children, teenagers and adults, your provider may recommend:
Children and young teenagers are prescribed the same medications. In addition to medications, some doctors also recommend that children take vitamins to get the nutrients they need for health and growth that they may not have gotten through food due to the effects of the disease on the bowel. Ask your healthcare provider for specific advice about the need for vitamin supplementation for your child.
You might need surgery that removes your colon and rectum to:
- Avoid medication side effects.
- Prevent or treat colon cancer .
- Eliminate life-threatening complications such as bleeding.
Medications For Ulcerative Colitis
No medicine can cure UC. The goal of medication is to make a patients ulcerative colitis manageable. People with UC may have to take medicines indefinitely to control their condition.
Medications for treating ulcerative colitis:
- Aminosalicylates
- These medications may be used in people with mild or moderate symptoms and most people can tolerate them. They contain an active ingredient called 5-aminosalisylic acid, or 5-ASA, which helps control inflammation. Drugs in this class include balsalazide, mesalamine, olsalazine and sulfasalazine.
- Corticosteroids
- More commonly known simply as steroids, these medicines reduce the immune systems response. They are used if aminosalicylates dont seem to work. Drugs in this class include prednisone, methylprednisone, hydrocortisone and budesonide. These drugs shouldnt be used long-term.
- Immunomodulators
- These drugs reduce immune system activity as well, but may take as long as three months to work. Immunomodulators include Azasan or Imuran and Purinethol or Purixan .
- Biologics or TNF therapy
- This group includes Humira , Simponi and Remicade , medications that decrease inflammation by targeting a protein made by the immune system called tumor necrosis factor, or TNF. Side effects of these medications include higher risks for tuberculosis, fungal infections, skin cancer and psoriasis.
Doctors may also recommend antibiotics to prevent infection and other medications to treat diarrhea.
Read Also: Ulcerative Colitis Unspecified Without Complications
What Should I Eat During An Ulcerative Colitis Flare
There is no specific type of diet that has been proven to relieve symptoms in people with ulcerative colitis. However, you may find that particular foods make symptoms worse.
It is important to identify and limit any foods that lead to worsening of your symptoms. Keeping a food journal may help you track how your diet relates to your symptoms.
Some suggestions that may help during a flare-up include:
- Limit fiber
- Reduce dairy products containing lactose
- Avoid high-fat foods
- What remedies help during an ulcerative colitis flare-up?
In addition to taking medication as prescribed and eating a well balanced diet, maintaining a healthy lifestyle can be beneficial for managing ulcerative colitis. Regular exercise and mindfulness strategies have been shown to improve overall health and quality of life.
Arastéh, K., Baenkler, H. W., Bieber, C., Brandt, R., & Chatterjee, T. T. . Duale Reihe Innere Medizin. Georg Thieme Verlag.
Dignass, A., Preiß, J. C., Aust, D. E., Autschbach, F., Ballauff, A., Barretton, G., … & Jantschek, G. . Aktualisierte Leitlinie zur Diagnostik und Therapie der Colitis ulcerosa 2011Ergebnisse einer Evidenzbasierten Konsensuskonferenz. Zeitschrift für Gastroenterologie, 49, 1276-1341.
Elizabeth Oliver, PhD
Dont Skip Your Medication
If you already have prescription medication for colitis, take your medication as prescribed. Dont skip your medicine, even if you feel better.
If you need help remembering to take your medication, use a reminder on your phone and/or set a sticky note on your keys
Sticking with your medication schedule can help you stay in remission and avoid a flare-up.
You May Like: Foods That Prevent Stomach Ulcers
How Do You Get An Ulcerative Colitis Diagnosis
One important thing to note is that people with more severe cases of ulcerative colitis are at an increased risk of developing colon cancer and other serious health conditions, like liver disease, Rudolph Bedford, M.D., a gastroenterologist at Providence Saint John’s Health Center in Santa Monica, California, tells SELF. Thats why its important to reach out to a medical professional if you do have any of the above symptoms.
However, an ulcerative colitis diagnosis can be challenging because other conditions can mimic symptoms of IBD, like infections or even hemorrhoids, Dr. Sinha says. In terms of differentiating between Crohns and ulcerative colitis, he says, Theres no single test that we have that 100% distinguishes between the two. We rely on the patient history and other information such as radiographic imaging and endoscopy. Doing a colonoscopy, for example, can be one of the most reliable ways to identify IBD and to then distinguish between Crohns and ulcerative colitis.
While a colonoscopy is an effective tool, Dr. Sinha clarifies that its not the only way. Rather, theres an entire constellation of tests and data that can be considered, including imaging, lab tests, and a detailed intake of the patients symptoms and presentation.
Home Remedies For Ulcerative Colitis
Ulcerative colitis is an inflammatory bowel disease that impacts the lining of the large intestine, also known as the colon. It can cause diarrhea, abdominal pain, and bloody stools.
The symptoms of ulcerative colitis and Crohns disease, the other IBD, are similar but there are many differences between the two diseases. One key difference is ulcerative colitis affects just the colon, while Crohns disease can cause inflammation anywhere in the digestive tract, which stretches from the mouth to the anus.
There is no cure for ulcerative colitis, but there are a number of treatments available. Treatment options may include medications, surgery, and changes to diet and nutrition. Some people may find natural treatments like eating foods containing omega-3 fatty acids or practicing yoga beneficial for the management of their symptoms.
Complementary and alternative medicines will not cure ulcerative colitis, and they should not replace conventional therapies.
In this article, well discuss seven different home remedies that have been shown to help with symptoms of UC.
Brooke Pelczynski / Verywell
Roughly half of people with ulcerative colitis report experiencing mild symptoms. Possible symptoms include:
- Abdominal pain
Read Also: What Are The Symptoms Of Having An Ulcer