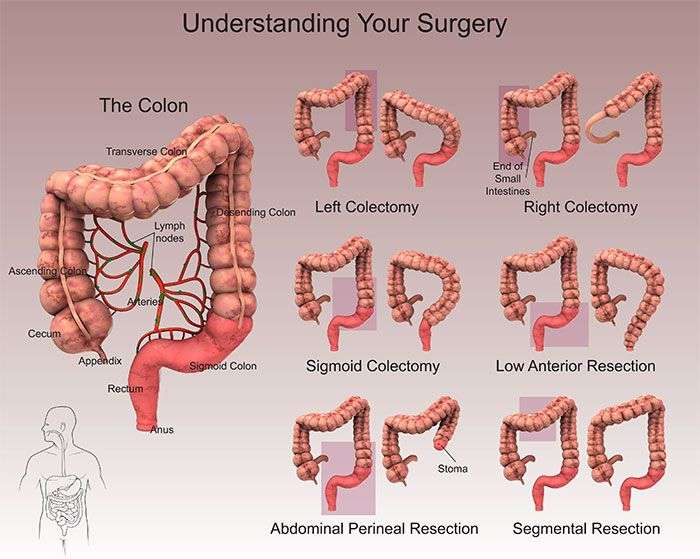
What Is A Colostomy And Why Is It Sometimes Necessary
In certain cases, it is necessary to allow the colon to heal before reattachment takes place. In such instances, an opening, called a stoma, is made through the abdominal wall into the remaining tissue at the upper end of the colon and a bag is fitted around the opening to collect intestinal waste. This procedure is called a colostomy and, while frequently reversible,
What To Expect After J
Your body will need time to adapt to the pouch after your surgery. We can help you learn what to expect after surgery and questions you may want to ask your healthcare providers.
-
Some patients experience an increased number of bowel movements, sometimes up to 12 times per day. This will typically decrease over time.
-
Some male patients may experience sexual dysfunction as a result of nerve damage.
-
Female patients may develop scar tissue that surrounds their ovaries and fallopian tubes, which may lead to infertility.
-
Both men and women should discuss sexual function with their surgeon and ask when it is safe to resume sexual activity.
-
Ask your healthcare providers what supplies you may need at home, especially if you will have a temporary ileostomy.
-
Your healthcare team will advise you on how to manage your temporary ostomy and how to keep it clean.
Risks Of The Procedure
Every surgery has risks. The risks of this surgery include:
-
Bleeding
-
Infection at the skin incision site or inside the stomach
-
Blood clots that form in the leg veins and then move to the lungs
-
Leaking through the joined tissues and vessels
-
Trouble passing urine
-
Slower wound healing, opening of the wound or scar tissue
-
Sexual problems
-
Heart or brain injury from anesthesia
There may be other risks, depending on your health. Talk with your healthcare provider before the procedure if you have concerns.
Read Also: New Meds For Ulcerative Colitis
What Should I Ask My Doctor On Behalf Of My Child Or Teenager
Ask your healthcare provider the following questions in addition to the ones listed above:
- What vitamins should my child take?
- Will my other children have pediatric ulcerative colitis?
- Is my child at risk for other conditions?
- Can you recommend a psychiatrist or therapist to help my child with emotional issues related to pediatric ulcerative colitis?
- Is my child growing at a normal rate?
- What can I do to help my child cope at school?
A note from Cleveland Clinic
When you have ulcerative colitis, its essential to work closely with your healthcare team.
Take your medications as prescribed, even when you dont have symptoms. Skipping medications youre supposed to take can lead to flareups and make the disease harder to control. Your best shot at managing ulcerative colitis is to follow your treatment plan and talk to your healthcare provider regularly.
Key Points To Remember
- Most people who have mild colitis can control their symptoms with medicine. Surgery isn’t usually done for mild colitis.
- The only cure for ulcerative colitis is surgery to remove the colon and the lining of the rectum. After the most common type of surgery, you will still be able to have bowel movements. After the less common type of surgery, you will wear an ostomy bag to remove body waste.
- You are more likely to get colon cancer if you have had ulcerative colitis for 8 years or longer. But surgery removes the risk of colon cancer.
- Surgery is usually successful, but it does have risks. These include blockages in the small intestine and leaking of stool.
- Surgery may be needed if cancer cells are found during a biopsy.
Ulcerative colitis is a common type of inflammatory bowel disease. Parts of the digestive tract get swollen and have deep sores called ulcers.
Ulcerative colitis affects the colon and the rectum. Symptoms include:
- Belly pain.
- Diarrhea.
- Bleeding or mucus during bowel movements.
You may also start to have symptoms in other parts of your body, such as your joints, eyes, and skin.
Read Also: What Medicine Is Good For Ulcers
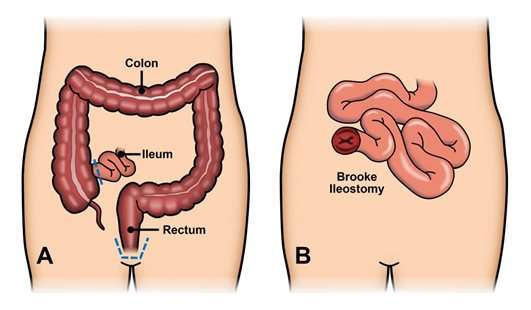
Proctocolectomy And Ileoanal Pouch
Proctocolectomy and ileoanal pouch-anal anastomosis is a newer procedure that allows a person to have bowel movements out of their natural anal opening. This procedure is sometimes called ileoanal pouch reservoir surgery or J-pouch surgery.
IPAA preserves the anus, rather than removing it. This procedure involves the following steps:
Stool gradually collects in the internal pouch and exits the body via the anus, making it more like a standard bowel movement.
If a persons anal muscles are in good condition, they will be able to feel stool coming out and will be able to use the toilet for bowel movements, as usual.
Although a surgeon preserves the anus with this procedure, the bowel movements are often more frequent and may be very soft or watery because the colon is missing.
Fecal incontinence may occur in some people, but medications are available that can help control bowel movements. A person should have good functioning of the anal muscles to help reduce the risk of incontinence.
Sometimes, surgeons perform IPAA in stages. The first stage involves making the pouch and connecting it to the anus. Then, the surgeon will leave the pouch alone to heal for several weeks.
How Is Ulcerative Colitis Surgery Performed
Ulcerative colitis surgery takes place in a hospital using general anesthesia. The details of the surgery will vary depending on the specific procedure you need. Usually, emergency surgeries are traditional open procedures.
Elective surgeries can be either open surgery or minimally invasive. In general, minimally invasive surgery involves less pain, fewer complications, and a faster recovery. However, there are times when open surgery may be the safest or most effective choice. Talk with your doctor to find out if you are a candidate for minimally invasive surgery.
Some surgeries only involve one procedure. This includes the Brooke ileostomy and the Kock pouch. The other options require two procedures. The first procedure connects the small intestine to either the rectum or anus and creates a temporary ostomy. After the connection heals, a second surgery closes the ostomy.
In emergency situations, three procedures may be necessary. The first removes the colon and creates an ostomy. After recovery, a second procedure removes the rectum and connects the small intestine to the anus. After the connection heals, a third surgery closes the ostomy.
Also Check: Best Acid Reducer For Ulcer
Ostomy Is Not A Dirty Word
The ileostomy was not at all what I expected. After years of ulcerative colitis and wondering when diarrhea would strike and when I would need a bathroom in a hurry, the ileostomy was like having my freedom again. I simply went and emptied my ostomy pouch when it became full. I didn’t change my wardrobe at all â I wore all the same clothes I did before my ileostomy. I started to expand my diet, although I was careful to follow my surgeon’s instructions and avoid roughage like nuts or popcorn. I even began to put on weight, for the first time in my adult life. I never did have a blowout for the 3 months I had my ileostomy. I don’t think I had any great skill at attaching my ostomy appliance, but even so I never had any issues or embarrassing incidents.
Changing my ileostomy appliance about twice a week became part of my routine. My stoma became just another part of my body. It did seem weird, if I thought about it too much. After all, the stoma is part of your intestine, and it was on the outside of my body! But, this was the surgery that allowed me to live, hopefully for a very long time. Without it, the dysplasia and the hundreds of polyps found in my colon may have resulted in colon cancer and a worse outcome for me.
Recovery: What To Expect In The Next Few Weeks
Most patients will be fully recovered in two weeks and can resume some normal activities, such as driving, walking and some duties at work. Since this surgery requires internal stitches, patients should refrain from any heavy lifting pushing or pulling until it is approved by the surgeon.
Alternative Names
Colectomy, laparoscopic colon surgery laparoscopic colon resection. Other terms: ostomy, stoma, Crohn’s disease, ulcerative colitis
Also Check: Signs And Symptoms Of Peptic Ulcer
How Common Is Surgery For Ulcerative Colitis
About 25% to 40% of people with ulcerative colitis will have to have surgery to remove their colons. The reasons that surgery becomes necessary include:
- Medical treatment — for instance, drug therapy — fails to provide results.
- There may be a risk of cancer without surgery.
- The colon has ruptured.
- The patient experiences a severe, sudden onset of the disease.
- There is extensive bleeding.
- Treatment causes side effects severe enough to compromise the patient’s health.
- Toxic megacolon has set in. In this dangerous condition, the muscles of the large intestine are dilated, and the colon can rupture.
In some cases, surgery to remove the colon is recommended if other treatments do not work or if the side effects of medications are harming the patient.
There Are Two Surgery Types
The standard UC surgery is a proctocolectomy. There are two versions: proctocolectomy with ileal pouch-anal anastomosis and proctocolectomy with end ileostomy. In the J-pouch procedure, your colon and rectum are removed in the end ileostomy, your colon, rectum, and anus are taken out. The J-pouch is most common, says Rudolph Bedford, M.D., a gastroenterologist at Providence Saint Johns Health Center in Santa Monica, CA. This is really the surgery for ulcerative colitis, he says. End ileostomies remain an option, says David M. Poppers, M.D., Ph.D., a gastroenterologist at NYU Langone Health in New York City, but arent as common.
Read Also: Can Ulcerative Colitis Cause Cancer
What Matters Most To You
Your personal feelings are just as important as the medical facts. Think about what matters most to you in this decision, and show how you feel about the following statements.
Reasons to choose surgery
- Diarrhea.
- Bleeding or mucus during bowel movements.
You may also start to have symptoms in other parts of your body, such as your joints, eyes, and skin.
What Really Constitutes Laparoscopic Ipaa Variability Within The Same Definition
A variety of techniques is currently referred to as laparoscopic IPAA. In some cases, the dissection of the rectum and the transection at the anorectal ring are performed using standard laparoscopic techniques. The specimen is then removed through either a small lower midline incision, a Pfannenstiel incision, or through the site where a subsequent diverting loop ileostomy will be created. Some surgeons perform a completely laparoscopic rectal dissection, but prefer to transect the distal rectum through the extraction site using a conventional linear stapler. In other cases, the rectal dissection is not performed laparoscopically, rather it is performed under direct vision using the future extraction site and following complete laparoscopic mobilization of the abdominal colon.
Also Check: Diabetic Foot Ulcer Treatment Guidelines
Functional Results Cosmesis And Body Image
It is important to point out that both in case-matched studies and especially in purely retrospective analyses, patient selection could explain at least some of the differences in favor of laparoscopic IPAA. The evidence to date suggests that there might be some functional and quality of life benefits associated with laparoscopic IPAA. However, the consistency and relevance of these benefits remains questionable and will require further evaluation with longer follow-up.
What Should I Ask My Doctor
If you have ulcerative colitis, you may want to ask your healthcare provider:
- How much of my large intestine is affected?
- What risks or side effects can I expect from the medication?
- Should I change my diet?
- Will ulcerative colitis affect my ability to get pregnant?
- What can I do at home to manage my symptoms?
- What are my surgical options?
Recommended Reading: Is Oatmeal Good For Ulcerative Colitis
Elective Surgical Management Of Ulcerative Colitis
Surgical options for elective management of ulcerative colitis include total proctocolectomy with creation of an end ileostomy, total proctocolectomy with continent ileostomy, total proctocolectomy with IPAA, and total abdominal colectomy with ileorectal anastomosis. Among these, a creation of an IPAA is currently considered the preferred standard of care. Patients who are not suitable candidates for IPAA can be treated with laparoscopic total proctocolectomy and end ileostomy. On the other hand, laparoscopic surgery in the creation of an ileorectal anastomosis following total abdominal colectomy is technically feasible, but is rarely indicated. Similarly, total proctocolectomy and creation of a continent ileostomy is generally performed on patients who had previous surgical procedures for ulcerative colitis and is therefore typically performed using open technique. Ileorectal anastomosis and continent ileostomy will therefore not be further discussed in this review.
Elective Colorectal Cancer Surgery
Patients with Crohns disease and ulcerative colitis have a higher risk for colorectal cancer than the general population, so elective surgery may be recommended to eliminate that risk.
Colorectal cancer risk factors
-
The risk of CRC increases after living with IBD for 8 to 10 years
-
The risk increases the longer a person lives with IBD
-
The greatest risk is for people with IBD affecting their colon
-
Patients who have a family history of primary sclerosing cholangitis are also at higher risk of developing colorectal cancer
In most cases, colorectal cancer starts as a polyp, or a small lump growing from the wall of the intestine. Polyps typically start out benign but become cancerous over time. But in patients with IBD, abnormal and potentially precancerous tissue, called dysplasia, may lay flat against the wall of the intestine and can even be found in areas of the intestinal wall that appear normal during a colonoscopy.
Also Check: Wound Vac For Pressure Ulcers
Does Ulcerative Colitis Make You Immunocompromised
Ulcerative colitis doesnt make you immunocompromised. Some of the medicines that treat it may change the way your immune system responds. This change is different for each medication. Some of these changes may increase the risk of certain infections or other issues. A discussion with your health care team before starting a medication is the best way to understand these risks and ways to prevent them.
What Causes Ulcerative Colitis Flareups
When youre in remission from ulcerative colitis, youll want to do everything you can to prevent a flareup. Things that may cause a flareup include:
- Emotional stress: Get at least seven hours of sleep a night, exercise regularly and find healthy ways to relieve stress, such as meditation.
- NSAID use: For pain relief or a fever, use acetaminophen instead of NSAIDs like Motrin® and Advil®.
- Antibiotics: Let your healthcare provider know if antibiotics trigger your symptoms.
Don’t Miss: How Do You Know If You Have A Stomach Ulcer
Ulcerative Colitis Recovery Time
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
HealthTap doctors are based in the U.S., board certified, and available by text or video.
When Is A Colon Resection Necessary
Colon resection surgery may become necessary when the colon is so damaged that part or all of it has to be removed. This damage may occur as part of certain genetic conditions or as a result of one of the following conditions:
- Uncontrolled bleeding
- Injury to the colon or rectum
- Fistula, an abnormal connection between organs
You May Like: Align Probiotic For Ulcerative Colitis
When Is Ulcerative Colitis Surgery Needed
Your doctor may suggest surgery if you can’t control inflammation and ulcers with medication or other treatments. You may also need an operation if you get emergency complications of ulcerative colitis such as severe bleeding or tears in the colon. Some people choose to have surgery if their symptoms affect their ability to work and stay active.
Baseline Endoscopic Disease Activity
In the pre-biological therapy era, the IBSEN cohort demonstrated that patients with mucosal healing at one year had a lower risk of colectomy at 5years. In two trials evaluating the efficacy of IV steroids and IV cyclosporine in acute severe UC, severe endoscopic lesions at baseline were associated with a significantly higher colectomy rate during follow-up.
Read Also: Can Stomach Ulcer Cause Fever
Meet Your Uc Surgeons And Team
Most people who have surgery for ulcerative colitis are referred from their gastroenterologist. The surgeon that will complete the surgery is most often a colorectal surgeon, who specializes in surgery of the digestive system.
An enterostomal therapy nurse will be helpful before and after surgery to place an ileostomy. An ET nurse will help decide where the stoma will be placed and will make suggestions on which type of appliance will work best.
Surgery For Ulcerative Colitis: Before And After
Many people with ulcerative colitis end up needing surgery, sometimes sooner rather than later. Here’s what to expect if you’re considering or preparing for surgery.
When medications fail to manage symptoms of ulcerative colitis, you may need surgery. In fact, a surgical procedure is currently the only method that can cure someone of this condition.
Ulcerative colitis is an inflammatory disease that affects your colon and rectum, and treatment usually begins with medications to control inflammation and other symptoms. However, 23 percent to 45 percent of people with ulcerative colitis will need surgery.
New drugs are starting to reduce the number of people who need surgery, but when drugs can’t control ulcerative colitis symptoms, surgery can be a solution, says Thomas Ullman, MD, an associate professor of gastroenterology at the Icahn School of Medicine at Mount Sinai Hospital in New York City.
But when is surgery the best choice for ulcerative colitis? For some people, surgery could be necessary sooner rather than later possibly even during a first attack, especially with the onset of sudden and severe symptoms. If an ulcerative colitis flare causes serious symptoms such as severe bleeding or a rapid enlargement of the colon called toxic megacolon, emergency surgery may be required. About 15 percent of people with ulcerative colitis may experience this type of flare.
You May Like: List Of Foods To Eat When You Have An Ulcer