Diabetic Foot Ulcers: Surgery Options To Treat And Prevent Podiatric Emergencies
Diabetic foot ulcers open wounds on the feet are all too common in patients with uncontrolled blood sugar levels. In fact, 15% of people with diabetes will experience a foot ulcer, and 1 in 5 of those will be hospitalized for the condition.
Two of the most common disease processes that affect the feet in people with diabetes are diabetic peripheral sensory neuropathy and peripheral arterial disease.
Peripheral arterial disease involves damage to the medium and small arteries that supply blood and oxygen to nourish foot tissue.
Peripheral sensory neuropathy affects more than half of people with diabetes. Neuropathy damages the nerves in the feet, so people experience numbness or tingling, or feel like they have a heavy stocking or mud caked on their foot. In some cases, people experience burning or shooting pains in their feet, which are often worse at night.
Sensory neuropathy also creates an environment in which people can injure their feet but not feel the injury. For instance, people with diabetic sensory neuropathy can burn their feet with bath water that is too hot or when they walk on hot pavement barefoot during the summer.
Foot ulcers develop when the skin is exposed to repetitive pressure on the bottom of the foot, or from friction from poorly fitting shoes. Normally, people would feel pain because their shoes are rubbing against their foot, but neuropathy masks the pain.
History Of Previous Ulceration And Amputation
A diabetic patient with a history of previous ulceration or amputation is at increased risk for further ulceration, infection and subsequent amputation. Alterations in foot dynamics due to ulceration, joint deformity or amputation can cause the abnormal distribution of plantar pressures and result in the formation of new ulcers28.
Cysts Or Benign Soft Tissue Tumors
Benign cysts or soft tissue tumors, such as lipomas, can spontaneously develop on the bottom of the feet. These growths generally are not harmful.
Benign cysts or soft tissue tumors usually do not require treatment but may need to be surgically removed if they compress surrounding nerves or ligaments.
Recommended Reading: Removable Cast Walker Diabetic Foot Ulcers
Treatments For Sores On The Bottom Of Feet
To treat such kind of sores, there are two factors we have to consider. Treatment for underlying causes or treating the resultant symptoms. These may involve over the counter therapies, prescribed medicines or home remedies. Efforts to prevent infections must too be included. Here are the common treatments you can employ for your cases.
What Are Pressure Ulcers
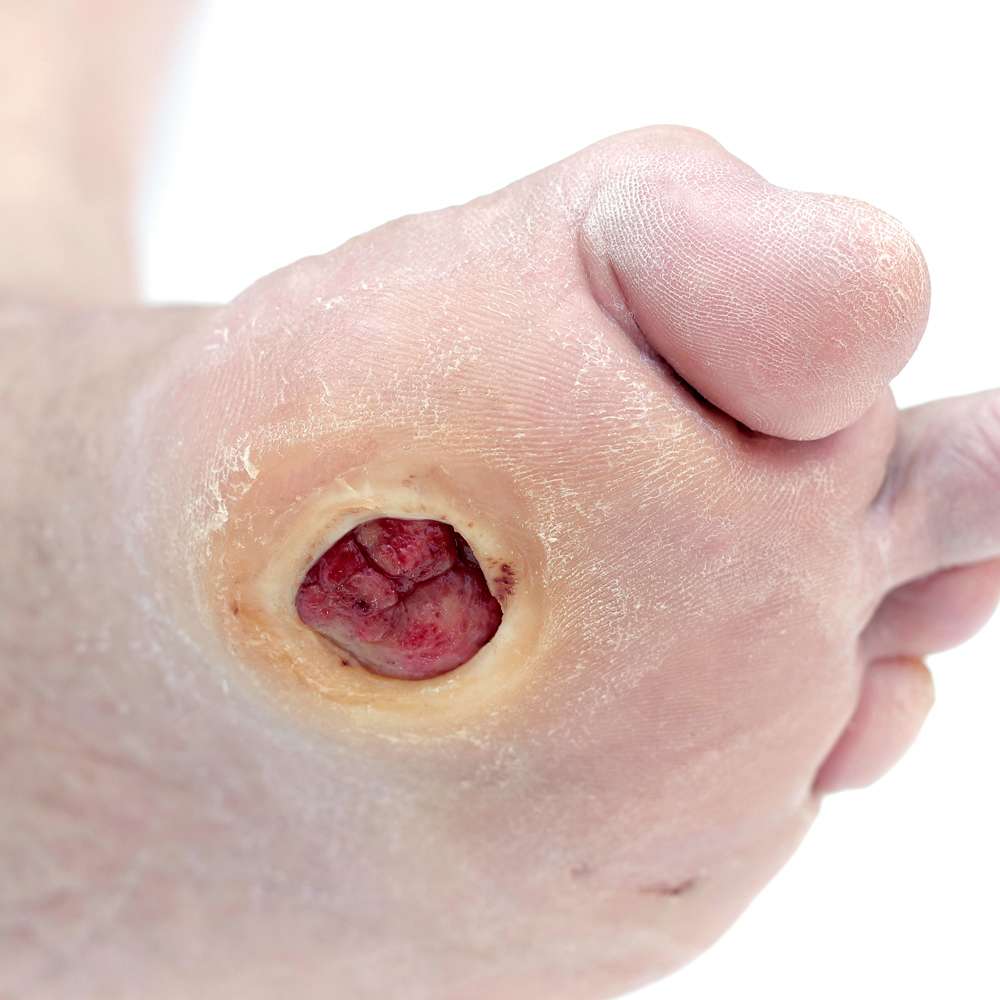
Pressure ulcers are sores that occur when pressure cuts off the blood supply to the skin. Stress caused by the bodys weight and the impact of striking the ground place the ball of the foot, the big toe, and the heel at the greatest risk. Left untreated, an ulcer may allow infection to enter your body. If infection reaches the bloodstream or bone, your life or limb may be at risk. But with your doctors help, your health can be protected. Pressure ulcers can be controlled and even prevented.
Read Also: Best Dog Food For Dogs With Stomach Ulcers
How Is A Diabetic Foot Ulcer Diagnosed And Treated
Your healthcare provider will ask about your symptoms and examine your foot and the ulcer. He or she may check your shoes. He or she may also send you to a podiatrist for treatment. The goal of treatment is to start healing your foot ulcer as soon as possible. The risk for infection decreases with faster healing. Do the following to help the ulcer heal:
How Do Pressure Ulcers Form
Force or friction against the bottom of your foot causes the skin to thicken, forming a callus. If the skin keeps thickening, the callus presses up into the foot. This kills healthy tissue and causes pain. Unfortunately, you may not notice the pain if you have neuropathy, a health problem that limits how much feeling you have in your feet. As healthy skin dies, an ulcer forms. Ulcers may progress from hot spots to infected wounds very quickly. A callus pressing into the foot may kill healthy tissue and cause an ulcer.Hot SpotsRed hot spots on the skin are signs of pressure or friction. They are a warning that you need to take care of your feet. If pressure is not relieved, a hot spot is likely to blister. Left untreated, a blister can turn into an open wound or a corn or callus.UlcersIf a corn or callus presses into the foot, it destroys inner layers of skin and fat. Cracks and sores may form. These open wounds are ulcers. They provide a way for infection to enter the body. In some cases, dead skin may cover an open wound, making it harder to see.Infected UlcersIf bacteria enter the ulcer, infection sets in. This causes more healthy tissue to die. The infected ulcer may begin to drain. The discharge may be white, yellow, or greenish. Some infected ulcers bleed or have a bad odor. If you develop an infected ulcer, call your doctor right away.
Read Also: Is Omeprazole Good For Ulcers
Rare Causes Of Bottom
Though less common, additional causes of foot pain must also be considered.
Tarsal Tunnel Syndrome
The tarsal tunnel is a narrow space on the inside of the ankle. Many arteries, veins, tendons, and nerves that allow the foot to move in different directions run through the tarsal tunnel.
One of these nerves is the posterior tibial nerve, which is responsible for the sensations you feel on the bottom of your foot and in your toes. Tarsal tunnel syndrome occurs when the posterior tibial nerve gets compressed in the tarsal tunnel. This causes pain, numbness, and tingling in the foot.
Factors that increase your chances of developing tarsal tunnel syndrome include:
Guillain-Barré Syndrome
This rare autoimmune disorder can come in several different forms. The most common form in the United States is acute inflammatory demyelinating polyradiculoneuropathy .
AIDP is often triggered by an infection, such as the flu or a respiratory illness. It can also be triggered by an immunization, but this is extremely rare.
As many as 40% of Guillain-Barré syndrome cases are triggered by a bacteria called Campylobacter jejuni, which causes diarrhea. It’s often found in undercooked poultry, putting people who eat it at an increased risk of campylobacter infection. GBS tends to set in a few weeks after the infection took place.
Treatment For Diabetic Foot Ulcers
If a diabetic foot ulcer does occur, its important to seek medical care as soon as possible this is not a wound you should attempt to treat at home on your own. The faster a foot ulcer is properly treated, the greater chance it will heal completely and without infection or complications.
A diabetic wound care specialist, such as the Wound Care Center at Harrington, can provide the most advanced and comprehensive diabetic wound treatment. Your primary care physician can provide a referral to the wound care center. Our Wound Care Center team will then continue working hand-in-hand with your doctor throughout the wound treatment process.
Our specialized diabetic wound treatment services include:
Don’t Miss: Best Home Remedy For Ulcer
How Can I Reduce My Risk Of Foot And Toe Ulcers
There are several things you can do to help reduce your risk of getting foot and toe ulcers. Sometimes, adopting these habits can even stop them from coming back. Try to:
- Manage your diabetes. If you have diabetes you should wear appropriate footwear and never walk barefoot.
- Examine your legs as well as the tops and bottoms of your feet and the areas between your toes every day. Look for any blisters, cuts, cracks, scratches or other sores. Also check for redness, increased warmth, ingrown toenails, corns and calluses. Use a mirror to view your leg or foot if necessary. If its difficult to see, ask a family member to look at the area for you. See a healthcare provider immediately if you notice any problems.
- Talk to your healthcare provider about ways you can stop smoking.
- Manage your blood pressure.
- Control your cholesterol and triglyceride levels by changing your diet. Limit salt in your diet.
- Care for your toenails frequently. Cut your toenails after bathing, when they are soft. Cut toenails straight across and smooth with a nail file. Take care of ingrown toenails.
- Wear appropriate shoes and socks. Talk to your podiatrist about what you need.
When Should I See My Healthcare Provider About Foot And Toe Ulcers
If you have diabetes, its important to see a podiatrist regularly. Whether you have diabetes or not, you should see a healthcare provider immediately if you find an ulcer on your foot or toe. Left untreated, it could get infected, leading to complications like amputations.
A note from Cleveland Clinic
It can be distressing to discover an open sore on your foot or toe. You might not know what caused it, it might not be healing and, if you have neuropathy from diabetes, you might not even feel it. Keep in mind that your healthcare provider can successfully treat your ulcer, especially if its found early. If left untreated, an ulcer can lead to serious complications.
If you have neuropathy caused by diabetes, remember that its important to check your feet and toes on a regular basis. Check your toes and feet every time you shower or when you go to put on your shoes. Contact your healthcare provider right away if you find an ulcer.
You May Like: How To Prevent Skin Ulcers
Sensory And Autonomic Neuropathy
Distal symmetric polyneuropathy is perhaps the most common complication affecting the lower extremities of patients with diabetes mellitus. This complication occurs in up to 58 percent of patients with longstanding disease.19 Neuropathy, a major etiologic component of most diabetic ulcerations, is present in more than 82 percent of diabetic patients with foot wounds.4 This lack of protective sensation, combined with unaccommodated foot deformities, exposes patients to undue sudden or repetitive stress that leads to eventual ulcer formation with a risk of infection and possible amputation.20
In the diabetic foot, autonomic neuropathy has several common manifestations. First, denervation of dermal structures leads to decreased sweating. This causes dry skin and fissure formation, which predispose the skin to infection. In vascularly competent patients, this autosympathectomy may lead to increased blood flow, which has been implicated as one of the primary etiologic factors in the development of Charcot’s joint and severe foot deformity.2123
The nylon monofilament test is a simply performed office test to diagnose patients at risk for ulcer formation due to peripheral sensory neuropathy.24 The test is abnormal if the patient cannot sense the touch of the monofilament when it is pressed against the foot with just enough pressure to bend the filament25 . Physicians can obtain a monofilament kit at a small cost from the National Diabetes Information Clearing-house .
Who Can Get A Diabetic Foot Ulcer
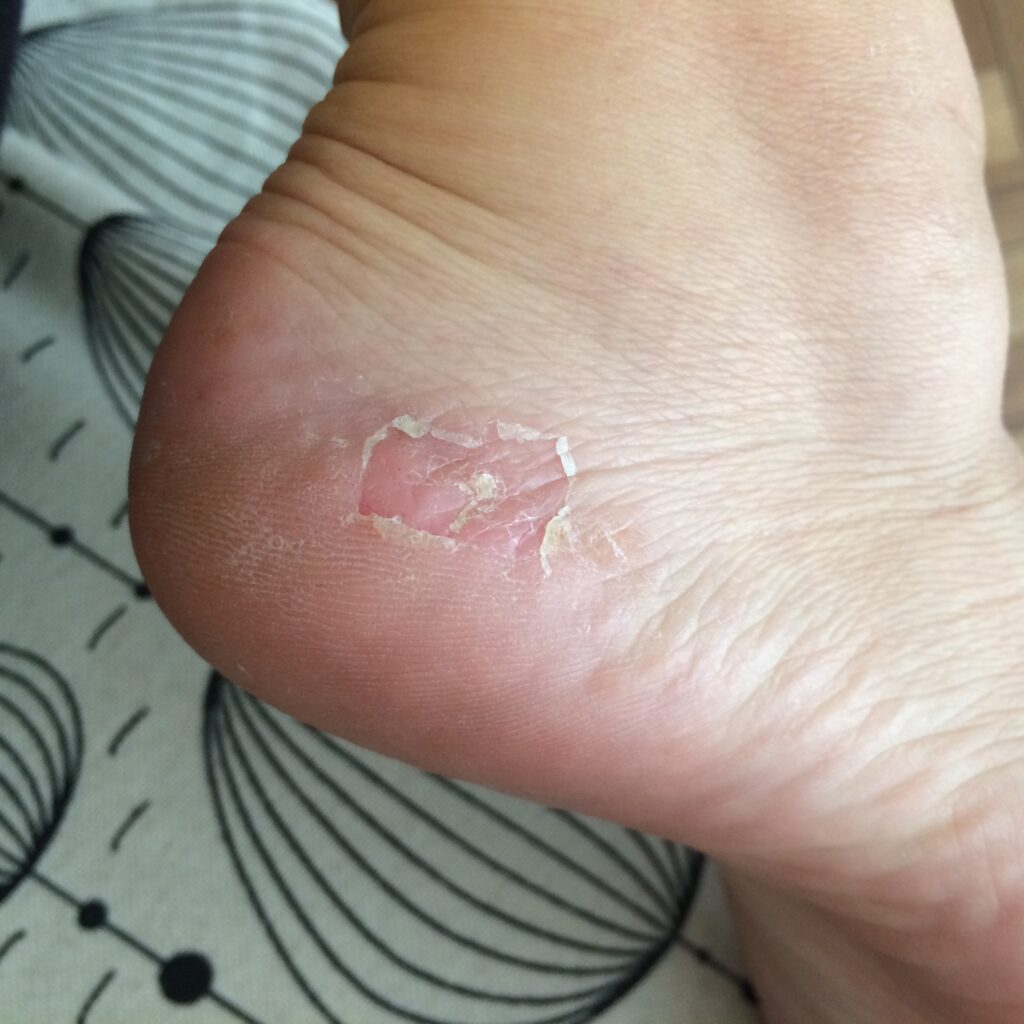
Anyone who has diabetes can develop a foot ulcer. Native Americans, African Americans, Hispanics and older men are more likely to develop ulcers. People who use insulin are at a higher risk of developing a foot ulcer, as are patients with diabetes-related kidney, eye, and heart disease. Being overweight and using alcohol and tobacco also play a role in the development of foot ulcers.
Read Also: Do I Have A Stomach Ulcer Test
Pressure Ulcer In The Diabetic Foot
All patients with neuropathic or neuroischaemic feet are at risk of pressure ulcers, especially of the heel. Pressure over heel ulcers can be off-loaded by pressure relief ankle foot orthoses. This orthosis is a ready-made device that has a washable fleece liner with an aluminium and polyproprylene adjustable frame and a non-slip, neoprene base for walking. It is used to relieve pressure over the posterior aspect of the heel and maintain the ankle joint in a suitable position, thus preventing pressure ulceration, aiding healing, and preventing deformity.deformity.
Pressure relief ankle/foot orthosis for use with heel ulcers
How Are Foot Ulcers Treated
The treatment of foot ulcers varies depending on the cause of the ulcer.
Neurotrophic or diabetic ulcers: The main goal of treatment is to obtain wound closure. How treatment will be managed will depend on the severity and vascularity of the ulcer and whether there is any infection. Your doctor will advise you to rest and elevate the affected foot to relieve pressure.
Venous statis ulcers: Compression is applied to the leg to minimize edema or swelling. This can be achieved by wearing compression stockings,) multi-layer compression wraps, or wrapping an ACE bandage or dressing from the foot to just below the knee.
The type of compression that will be applied will depend on the ulcers characteristics and amount of drainage. After ulcer closure, compression stockings may help control the venous insufficiency.
Arterial or ischemic ulcers: Treatment depends on how severe the arterial disease is. Your doctor may recommend further testing to assess the potential for wound healing. Endovascular therapy or bypass surgery to restore circulation to the affected leg may be required.
Treatment often includes debridement of all necrotic, callused, and fibrous tissue, which is a mainstay of ulcer therapy.
After debridement, a saline wet-to-dry dressing is applied. If necessary, specialized footwear or bandages to relieve pressure on the ulcerated area may be prescribed. Infected ulcers are treated with antibiotics. Management of the underlying cause of the ulcer is essential.
Also Check: What Does Asacol Do For Ulcerative Colitis
How Should A Diabetic Foot Ulcer Be Treated
The primary goal in the treatment of foot ulcers is to obtain healing as soon as possible. The faster the healing of the wound, the less chance for an infection.
There are several key factors in the appropriate treatment of a diabetic foot ulcer:
- Prevention of infection
- Taking the pressure off the area, called off-loading
- Removing dead skin and tissue, called debridement
- Applying medication or dressings to the ulcer
- Managing blood glucose and other health problems
Not all ulcers are infected however, if your podiatric physician diagnoses an infection, a treatment program of antibiotics, wound care, and possibly hospitalization will be necessary.
Preventing Infection
There are several important factors to keep an ulcer from becoming infected:
- Keep blood glucose levels under tight control
- Keep the ulcer clean and bandaged
- Cleanse the wound daily, using a wound dressing or bandage
- Do not walk barefoot
Off-Loading
For optimum healing, ulcers, especially those on the bottom of the foot, must be off-loaded. Patients may be asked to wear special footgear, or a brace, specialized castings, or use a wheelchair or crutches. These devices will reduce the pressure and irritation to the ulcer area and help to speed the healing process.
Applying Medication and Dressings
For a wound to heal there must be adequate circulation to the ulcerated area. Your podiatrist may order evaluation test such as noninvasive studies and or consult a vascular surgeon.
Managing Blood Glucose
Uneven Weight Distribution From Diabetes
Charcot foot is a rare condition characterized by a large, bony lump that forms on the bottom of the foot. It can develop as a serious complication of diabetes caused by chronic inflammation. A Charcot foot causes pain and swelling at the bottom of the foot and increases your risk of developing diabetic ulcers.
Treatment for a Charcot foot that develops from uneven weight distribution of the feet involves putting the affected foot in a cast and avoiding weight-bearing activities on that foot for several months. During this time, you will have to use crutches or a wheelchair to move around.
Gradual progression to normal weight-bearing with prescription footwear or a CROW will begin when your symptoms decrease. In cases that do not improve, surgery may be performed to remove bone spurs , increase the length of the Achilles tendon to improve the alignment of the foot and ankle, and fuse bones of the foot together for better stability.
Recommended Reading: What Is A Gastric Ulcer And What Is Its Cause
How To Prevent Diabetic Foot Ulcers
The first line of defense in preventing diabetic wounds is to follow the guidelines recommended to keep the disease itself under control:
- Maintain healthy blood sugar levels through a healthy diet and by taking medications as instructed by your doctor.
- Keep your blood pressure within a healthy range.
- Avoid alcohol and tobacco.
You should also take measures to avoid causing sores or wounds on the feet:
- Never walk barefoot.
- Wear shoes that fit properly and dont rub the skin.
- Wash your feet daily with mild soap and lukewarm water to prevent the buildup of bacteria on the skin, which can cause infection even in the tiniest skin breaks.
Because a loss of sensation in the feet may mean theres no pain felt even when an ulcer is present, its also extremely important for those with diabetes to regularly check for any foot sores or skin irritation. This way, the ulcer can be properly treated as early as possible.
Which Complications Of Pressure Ulcers Develop
The most serious complication that can occur as a result of a pressure ulcer on your foot or ankle is infection and sepsis. This occurs when bacteria enter the bloodstream through the compromised, ulcerated skin.
Infection then spreads throughout the body, endangering the patients life. Sepsis can also take the form of , a dangerous infection of the joints. If treatment is not administered, there is also the risk that gangrene could set in.
Even if sepsis does not occur, the patient is vulnerable to cellulitis infection of the skin, which can cause severe pain and swelling.
Read Also: What Can Help Stomach Ulcers
Foot Care Tips To Prevent Diabetic Foot Ulcers
Along with controlling your blood glucose levels, these basic foot care tips can help reduce your risk of foot ulcers and improve your overall health.
1. Inspect your feet every day. You may not have the flexibility to see the bottoms of your feet, or you may not see well. If this is the case, have your spouse or a family member inspect your feet and shoes for cuts, bruises, cracks, blisters, redness, or other signs of an abnormality. Call your doctor if you notice even a small wound the earlier we can help, the better.
2. Show your doctor your feet. Remove your shoes and socks when you visit your primary care doctor. Ask them to examine your feet for nerve damage and circulation, even if they dont initiate the request.