How Is Ibd Diagnosed
Links with this icon indicate that you are leaving the CDC website.
- The Centers for Disease Control and Prevention cannot attest to the accuracy of a non-federal website.
- Linking to a non-federal website does not constitute an endorsement by CDC or any of its employees of the sponsors or the information and products presented on the website.
- You will be subject to the destination websites privacy policy when you follow the link.
- CDC is not responsible for Section 508 compliance on other federal or private website.
Dont Miss: Foods That Cure Ulcerative Colitis
Whats The Difference Between Ulcerative Colitis And Crohns Disease
UC and Crohns disease are the most common forms of IBD. Both conditions are thought to be the result of an overactive immune system.
They also share many symptoms, including:
However, UC and Crohns disease do have distinct differences. Understanding the key differences between them can help you obtain a proper diagnosis.
Location
These two conditions affect different portions of the GI tract.
Response to treatment
Similar medications are prescribed to treat both conditions. Surgery is also a treatment option. Its a last resort for both conditions, but it can be a cure for UC, whereas its only a temporary therapy for Crohns.
Symptoms Of Ulcerative Colitis
Most symptoms are related to the inflamed rectum. The inflammation does not allow the rectum to stretch or store properly. This affects a patient’s ability to sense what is in the rectum, making them feel the urgency to use the bathroom more often. Very little stool will pass during these many trips to the bathroom â sometimes just mucus and blood.
When inflammation spreads to the lower part of the intestine, people can feel paradoxically constipated. The reason for this is that the bowel above the inflammation is working fine, but when it gets to the inflamed area, it can’t stretch like it is supposed to. That can cause an internal back up, causing bloating and gas.
Some people may experience extraintestinal manifestations, which refers to inflammation in other parts of their body. The most common manifestation is symmetrical joint pain, which occurs on both sides of the body, often in smaller joints. Other less common types include skin and/or liver inflammation. Extraintestinal manifestations are connected to the bowel inflammation and will get better if the inflammation in the large intestine is treated.
You May Like: Foods To Avoid If You Have A Stomach Ulcer
Caring For An Ostomy Bag
If you need this bag after your surgery you’ll get advice from your medical team about how to care for it and the stoma. You can empty or throw out the bags when you need to. Irrigating the stoma can help you control the timing of bag changes. To prevent leaks, the pouch system that connects the stoma to the bag needs to be changed every 4 to 7 days. Call your doctor if you notice a change in color, bleeding, or swelling.
Youre Avoiding Certain Healthy Foods
It can be hard to eat a healthy diet or anything at all if youre experiencing abdominal pain, cramps, or nausea. But if youre not eating the right foods, you could be at risk of nutrient deficiencies, malnutrition, and unwanted weight loss. The National Institute of Diabetes and Digestive and Kidney Diseases says that because people with ulcerative colitis can lose their appetite, it is important to focus on eating a healthy, balanced diet.
While theres no one meal plan that works for everyone, many people find they can tolerate low-fiber fruits , lean proteins, cooked veggies, sourdough bread, and grains such as oatmeal. A doctor or dietitian who specializes in IBD can help you develop a personalized meal plan.
Don’t Miss: Can You Take Tylenol With Stomach Ulcers
Meet Your Uc Surgeons And Team
Most people who have surgery for ulcerative colitis are referred from their gastroenterologist. The surgeon that will complete the surgery is most often a colorectal surgeon, who specializes in surgery of the digestive system.
An enterostomal therapy nurse will be helpful before and after surgery to place an ileostomy. An ET nurse will help decide where the stoma will be placed and will make suggestions on which type of appliance will work best.
Ulcerative Colitis In Children
According to one study of IBD in the United States, 1 in 1,299 children between ages 2 and 17 years old were affected by the condition in 2016. Crohns disease was twice as common as UC, and boys were more likely to have IBD than girls.
For children with IBD, a diagnosis is more likely after 10 years old.
UC symptoms in children are similar to symptoms in older individuals. Children may experience bloody diarrhea, abdominal pain and cramping, and fatigue.
In addition, they may experience issues compounded by the condition, such as:
- anemia due to blood loss
- malnutrition from poor eating
- unexplained weight loss
UC can have a significant effect on a childs life, especially if the condition isnt treated and managed properly. Treatments for children are more limited because of possible complications. For example, medicated enemas are rarely used as a treatment method in children.
However, children with UC may be prescribed medications that reduce inflammation and prevent immune system attacks on the colon. For some children, surgery may be necessary to manage symptoms.
If your child has been diagnosed with UC, its important that you work closely with their doctor to find treatments and lifestyle changes that can help. Check out these tips for parents and children dealing with UC.
Recommended Reading: What Causes Stomach Ulcers To Flare Up
What Are The Tubes Coming Out Of My Body
When you wake up, you may find some tubes attached to you. These could include:
When you are fully awake and recovering well from the anaesthetic medicines you will be moved to a ward. For most people this will be a regular surgical ward. Some people need more monitoring. They will be moved to a specialty ward like a high dependency or intensive care unit. This may include people with other conditions, like heart or lung disease. You may also need more monitoring if your surgery was an emergency, as you may be at higher risk of complications.
Youre Not On The Right Treatment Plan
UC treatment plans are typically based on how severe your symptoms are and how well you respond to medications. Usually, youll start with the least aggressive treatment and move on to stronger medications if necessary.
Frequent flares, hospitalizations, or the need for short-term corticosteroid prescriptions are signs that you might need to adjust your current treatment strategy. If you arent satisfied with the level of control you have over your UC, talk to your doctor about other options.
Recommended Reading: Another Name For Pressure Ulcer Is
Will I Need Additional Surgeries Or Treatments
If you have an IPAA, you may have a temporary ostomy in order to give the ileoanal pouch time to heal. Another surgery may be needed about 12 weeks after the first to reconnect your intestines to the pouch.
About one-third of people with UC who get a colectomy have short- or long-term complications. Some of the most frequent are pouchitis and bowel obstructions . These conditions may require additional medical treatments, such as antibiotics or additional surgeries.
How Does It Affect You
The condition also leads to several health issues. For example, people with this disorder often experience unhealthy weight loss as they have difficulty absorbing enough nutrients and fluids from their diet.
In addition, affected children usually grow more slowly than usual. Although it is not so common, Ulcerative Colitis causes skin, eyes, joints, kidneys, or liver issues. However, these complications occur most likely due to abnormal inflammation. Furthermore, Ulcerative Colitis also increases the risk of colon cancer, especially in people having the disease for years.
Ulcerative colitis is one of the two major types of inflammatory bowel disease . Crohns disease is another type of IBD that causes chronic inflammation of the intestines. However, unlike ulcerative colitis, which affects only the inner surface of the large intestine, Crohns disease may cause inflammation in any part of the digestive system. In addition, the inflammation extends deeper into the intestinal tissue.
Read Also: Things To Eat When You Have An Ulcer
Read Also: Differential Diagnosis For Ulcerative Colitis
Ulcerative Colitis Treatment: Medication
The most common medication option is anti-inflammatory drugs. These can be used orally or topically to reduce inflammation of the colon and rectum.
Treating ulcerative colitis is a highly individualized process. At Johns Hopkins, we tailor your treatment to your specific needs and alter the medication as necessary. Your specific medication regimen will depend largely on the severity of your condition.
Other medications include:
-
Immunosuppressive medications: These drugs slow your immune system to stop the immune response that is causing the colon and rectum to swell.
-
Biologics: Like immunosuppressive medications, biologics target the immune system, but biologics act on specific immune system proteins that encourage inflammation.
What Is The Treatment For Ulcerative Colitis
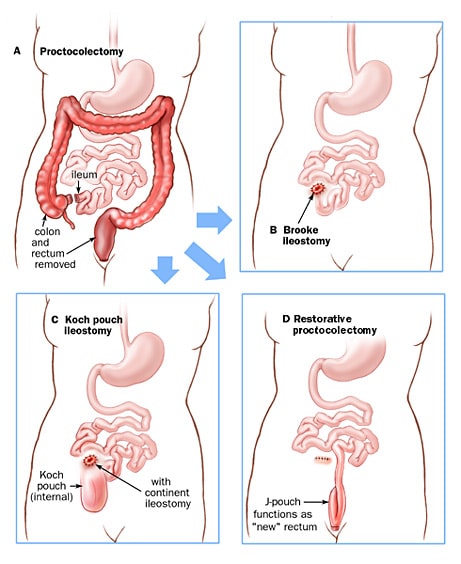
At this time the only cure for ulcerative colitis is surgical removal of the large intestine. There are things that can be done to help control ulcerative colitis before surgery is desired or required. At CHOC, treatment plans are developed based on each patients unique medical, physical, social and emotional needs.
The goals of treatment may include:
- Correcting nutritional deficiencies
- Supporting optimal growth and weight gain
- Reducing symptoms so the child can live a more normal life.
Specific treatment will be determined by your childs doctor based on the following:
- The childs age, overall health and medical history
- The symptoms and extent of the childs ulcerative colitis
- The childs tolerance for specific medications, procedures or therapies
- The familys opinion or preference.
Treatment may include the following:
Medication therapy. The childs gastroenterologist may recommend one or a combination of medications that will help the intestine heal. The classes of medications available include aminosalicyclates, antibiotics, corticosteroids, immunomodulators and biologic therapies.
Children with ulcerative colitis may lose weight because they are not getting enough calories because:
- They may avoid eating to prevent pain that comes with digestion.
- They have greater nutritional needs than average because of their disease.
- They may not be enthusiastic about eating when favorite foods are eliminated from their diet.
The common surgical options:
Recommended Reading: How To Avoid Pressure Ulcers
What Is The Difference Between A Colectomy And A Colostomy
A colectomy removes part or all of your colon. But what happens to the rest of your intestinal tract after the diseased tissue is removed? That varies, depending on several factors. Sometimes the two remaining ends of your intestines can simply be stapled together in the same surgery, and your intestinal tract can continue to function as usual. But sometimes thats not possible. In this case, you may need an ostomy either an ileostomy or a colostomy. The ileostomy or colostomy may be temporary or permanent.
Not all colectomies require an ostomy, and not all colostomies are permanent. You may only need one temporarily while your intestines are healing from the colectomy. After a few months, many ostomies are reversible, depending on your health. You may return to surgery to have the severed ends of your intestines reconnected and your stoma closed. Others may need a permanent ostomy.
What Are The Complications Of Ulcerative Colitis Surgeries
Complications from ileoanal anastomosis may include:
- More frequent and more watery bowel movements
- Inflammation of the pouch
- Blockage of the intestine from internal scar tissue, called adhesions, caused by surgery
- Pouch failure, which happens within 5 years in about four out of every 100 patients with IPAA
If your pouch fails, youâll need a permanent ileostomy.
A hemicolectomy has some of the same risks as other surgeries. Your doctor will give you anesthesia to put you to sleep. Itâs safe for most people, but you could have a reaction that makes you feel sick for a few days. Itâs rare, but some people may feel confused for a week or so.
You could also get blood clots in your legs or lungs. To lessen the chances of this, a doctor or nurse will get you to walk around every hour or so in your hospital room.
Other possible problems include:
You May Like: How To Treat Skin Ulcers
How Is Colectomy Surgery Done
There are a few different types of colectomy surgery and its important to understand which you are having. These are:
- Right hemicolectomy – resection of the ascending colon
- Left hemicolectomy – resection of the descending colon
- Transverse colectomy – resection of the horizontal part of the colon
- total colectomy – removal of all of the colon, leaving the rectum
- Partial colectomy – resection of a small part of the colon
- Sigmoidectomy – resection of the sigmoid colon
- Proctocolectomy – removal of all of the colon and also the rectum
This article refers to the right and left hemicolectomy, transverse colectomy and total and partial colectomy surgery. There are separate articles on sigmoidectomy and proctocolectomy surgery.
The day before your surgery you will likely be asked to take a bowel preparation which will give you diarrhoea to clear the bowel of any faeces to make the operation easier. You may also need to follow a specific diet and avoid some medications.
Shortly before your surgery your blood pressure and breathing will be monitored and you will be prepared for theatre. You may be given medicine through a vein in your arm. Just before the surgery you will be given a general anesthetic which will put you in a sleep-like state so that you wont be aware of whats happening.
Open surgery: An incision will be made along your abdomen to provide access to the colon for your surgeon. They will then identify the damaged section of the colon and remove it.
Feeling Better After Surgery
When you feel better will be different for each person. When you first get home, youll probably feel quite weak and tired. You may not feel like doing much.
You should avoid any strenuous exercise for at least a few weeks after your surgery. This is so your wounds can heal properly. This means avoiding any heavy lifting or housework. You may struggle to go up stairs for a short time after surgery.
I couldn’t even lift a full kettle when I was first home. When I had to be on my own, my dad would make a flask of tea for me to have throughout the day, as this was easier for me to lift and pour. I also found it very useful to wear loose long T-shirts or nightgowns so that clothing didn’t pull on my stomach which was very sore for the first few days.
NiaLiving with Colitis
As time goes on youll notice your strength coming back. After a few weeks, you should be able to gradually introduce exercise into your daily routine. A gentle exercise programme may help speed up your recovery and you will likely be given advice on this by your surgical team.
You should be able to start going back to your normal daily activities. Its important to listen to your body and only do as much as feels comfortable. Everybody is different, so try not to put too much pressure on yourself to get back to normal life straight away.
Living with Colitis
Also Check: Can Acid Reflux Cause Ulcers
When Is A Colectomy Recommended For Ulcerative Colitis
Many people with ulcerative colitis are prescribed medications, such as corticosteroids or biologics, to eliminate symptoms and treat inflammation. These medications successfully treat about 70 percent of people with UC. About one-third to one-quarter of people living with UC will need surgery to help manage their condition, however.
People with ulcerative colitis may need a colectomy if they have:
- Severe symptoms, such as extreme bleeding, perforations , or toxic megacolon
- Symptoms that dont get better with medication
- Cancer or precancerous changes in the intestine
Who You’ll See: Your Ibd Team
Not everyones IBD team looks the same but whoever you see, theyre all working to help keep you as healthy as they can. As well as those who may already be involved in your care , if youre having surgery your IBD team may also include your:
- Surgeon they will carry out your bowel surgery
- Anaesthetist they will manage the anaesthetic and pain relief during your surgery
- Stoma nurse they will provide information and ongoing support if you have a stoma
- Physiotherapist they will help you with movement and exercise after the surgery
Living with Colitis
Also Check: Ulcerative Colitis Pain In Legs