Adjusting Your Diet To Reduce Ulcerative Colitis Pain
There isnt one diet thats best for everyone with UC. Itâs best to focus on getting balanced and diverse nutrition from a variety of foods. Cutting out whole food groups is unnecessary unless you have known food allergies or intolerances . For some people, following the guidelines of the Mediterranean diet is helpful.
Dont Miss: Best Oil For Horses With Ulcers
What Is Ulcerative Colitis
Ulcerative colitis causes irritation and ulcers in the large intestine . It belongs to a group of conditions called inflammatory bowel disease . It often causes diarrhea with blood, cramping and urgency. Sometimes these symptoms can wake a person up at night to go to the bathroom as well.
The severity of UC depends on the amount of inflammation and the location. Everyone is a little different. You could have severe inflammation in the rectum or very mild inflammation in the entire colon .
If you have ulcerative colitis, you may notice a pattern of flare-ups , when symptoms are worse. During times of remission, you might have little to no symptoms. The goal with therapy is to remain in remission as long as possible .
Symptoms of inflammatory bowel disease can include diarrhea, blood in the stool, weight loss, and abdominal pain. The type and location of abdominal pain is different, not only between the two main forms of IBD but also within the subtypes of these diseases.
Further, pain is even more individual to each person, to the point where people with the same subtype of Crohnâs disease or ulcerative colitis may experience pain in a different way.
In fact, some people with IBD donât have any abdominal pain at all during IBD flare-ups. In addition, abdominal pain can be related to other issues , such as appendicitis, gallstones, or gastroesophageal reflux disease .
When To Contact A Doctor
A person living with UC should talk with their doctor if they notice symptoms associated with sacroiliitis, such as pain in the hips when walking or any other types of arthritis. A primary care physician may refer a person to a rheumatologist for diagnosis.
A person may want to consider a second opinion if their doctor does not refer them to a rheumatologist. Early referrals can help improve treatment outcomes. However, referral rates are low, according to a 2018 study .
If symptoms get worse during treatment or do not improve, a person should talk with a healthcare professional. A doctor can recommend additional therapies that may help improve symptoms of either UC or sacroiliitis.
As a person begins to better manage their UC symptoms, they will often notice an improvement in their sacroiliitis symptoms, too.
Don’t Miss: Safety Considerations For Ulcerative Colitis
Urgency To Pass A Stool
Not only will the stool consistency change if you have ulcerative colitis, but the urge to pass could hit suddenly and strongly even though nothing comes out. If you have inflammation in the rectum, you have this sense of needing to get rid of something, even though its not there, says Dr. Englander.
What Is Life Like With Ulcerative Colitis
The only cure for ulcerative colitis is complete surgical removal of the colon. However, most patients will not require surgery to have their symptoms under control, and some patients may have complications after the surgery such as pouchitis. Whether they require surgery or not, our goal is to allow our patients to live a full and productive life with ulcerative colitis. Most patients will require medications for an indefinite period of time. Research has shown that patients with ulcerative colitis who do not take their medication, even if they are feeling well, are more likely to have a return of their symptoms compared to patients who continue their medications. It is very important that patients discuss with their doctor if they are considering stopping their medications.
It is important for patients with ulcerative colitis, even if they are feeling well, maintain regular visits with their physician. For example:
- Patients on medications may need routine blood work to monitor for side effects.
- Patients with ulcerative colitis should keep up to date on immunizations including influenza , pneumococcal , human papilloma virus , and hepatitis A and B.
- Some patients with ulcerative colitis, particularly those who have had been exposed to steroids , may need to have bone mineral density tests to screen for early osteoporosis.
- Patients with ulcerative colitis will need to have colonoscopies to screen for colon cancer.
Don’t Miss: Gastric Ulcer Treatment In Horses
How Often Do I Need A Colonoscopy
Especially when you have symptoms or are just starting or changing medications, your doctor may want to periodically look at the inside of the rectum and colon to make sure the treatments are working and the lining is healing. How often this is needed is different for each person.
Ulcerative colitis also increases your chance of developing colon cancer. To look for early cancer signs, your healthcare provider may have you come in for a colonoscopy every one to three years.
Dont Miss: Foods To Avoid During Ulcerative Colitis Flare Up
Increased Severity Of Back Pain After Uc Diagnosis
Anyway, over the years I used yoga to manage my pain. Sometimes I only experienced dull twinges. Other times I had to take a day to ice it so I could walk normally and bring down the pain level. But it never was as bad as it was in the beginning-until I moved back home.
I had forgotten how terrible the pain was. And after experiencing that awful two week period of constant bathroom visits and abdominal spasms, I thought nothing else could be as painful. After I got stuck in the backyard on my stomach because I couldnt get up, my parents shoved a phone in my hand and told me to call a doctor.
This time though I was armed with some new information. I had been doing some reading on ulcerative colitis and discovered that UC can affect other parts of the body, sometimes years before there are any signs of bowel disease.
Joints can be affected and in rare cases, there can be inflammation of the joints in the spine and pelvis. When I saw a doctor this time, I was still experiencing a lot of pain and he was able to better observe what I was going through.
Unfortunately, he could not prescribe me anything. All the stronger pain medications have anti-inflammatory drugs in them, which can cause bleeding in people with inflammatory bowel disease. I was referred to physical therapy, where I was told, once again, that it was SI joint dysfunction.
Recommended Reading: Where Does Ulcerative Colitis Occur
How Does Pediatric Ulcerative Colitis Affect My Childs Mental/emotional Health
Like many conditions, ulcerative colitis can have a negative psychological effect, especially on children. They can experience physical, emotional, social and family problems. Because of the medications and/or general stress from the situation, your child may experience:
- Worry about appearance and physical stamina.
- Vulnerability because their body doesnt function normally.
- Poor concentration.
- Misunderstandings with friends and family.
Children need mutual support from all family members. Its helpful for the entire family to learn about the disease and try to be empathetic. Seek out a psychiatrist and therapist to help your child manage such challenges of their ulcerative colitis.
Ulcerative Colitis And Crohn’s Disease Pain Locations Are Usually Different
Ulcerative colitis and Crohn’s disease pain locations are different, even though both of these conditions are classified as inflammatory bowel diseases . Also, the nature and location of pain vary from one person to the next.
This article explores Crohn’s and ulcerative colitis pain locations and types, what pain in different parts of the abdomen may mean, and how Crohn’s and ulcerative colitis pain locations can help with a diagnosis.
Jessica Olah / Verywell
You May Like: Preventive Measures For A Decubitus Ulcer Include
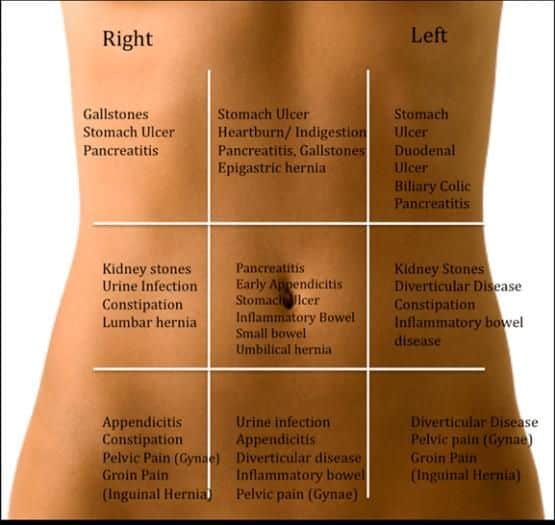
Right Or Middle Abdomen Pain
A pain that feels like cramps in the middle of the abdomen or the lower right quadrant is typical of the types of Crohns disease known as ileocolitis and ileitis.
Ileocolitis is the most common form of Crohns disease and is defined by inflammation located in the last section of the small intestine and in the large intestine .
Ileitis is a type of Crohns disease that affects only the ileum and is the second most common form. People with ileitis may also find that their pain or discomfort appears within a few hours of eating a meal.
Upper Middle Abdominal Pain
A type of IBD called gastroduodenal CD often causes pain in the middle and upper sections of the abdomen. These Crohn’s disease pain locations correlate with problems in the:
This disease type is rare, accounting for only about 4% of all diagnoses. It’s even more rare for it to only impact the duodenum. This happens in just 0.07% of all CD cases.
Other symptoms of gastroduodenal CD may include:
- Fullness, or an inability to eat very much at once
| Jejunoileitis |
You May Like: Can You Eat Pizza With Ulcerative Colitis
What Happens If You Dont Treat Colitis
Colitis is usually a temporary condition that resolves on its own in a few days to a week. It can, however, be a sign of a more serious condition such as ulcerative colitis, Crohns disease, autoimmune disorders, metabolic disorders, circulation problems, heart problems, or radiation injury. It can also be a sign of a serious infection, such as a potentially fatal E. coli gut infection or amoebic dysentery. If the symptoms become severe or last longer than a week, its time to talk to a doctor.
Muscle Strain Or Sprain
A muscle strain or sprain is the most common cause of low back pain.
A strain is a tear or stretching in a tendon or muscle, while a sprain is a tear or stretching in a ligament.
Sprains and strains usually happen when you twist or lift something improperly, lift something heavy, or overstretch your back muscles.
These injuries can cause swelling, difficulty moving, and back spasms.
Read Also: Coconut Milk Good For Ulcerative Colitis
Can You Die From Ulcerative Colitis
Ulcerative colitis usually isnt fatal, according to the Mayo Clinic. But it can cause severe and even life-threatening complications.
This means that ulcerative colitis is considered a serious illness, and you should treat its management and treatment with a similar seriousness.
Getting the right treatments for ulcerative colitis can cause a dramatic reduction in symptoms and possibly lead to lasting remission.
Dont Miss: Bland Diet Recipes For Ulcers
How Does Kidney Infection Affect Your Stomach
Stomach is one of essential organs of your digestive system. And the kidneys are part of your urinary system. But sometime they can affect each other if one of them goes awry. For instance if you have infection in the kidney, it may also cause pain in the stomach. There are a number of ways of how kidney infection can affect your stomach.
Donât Miss: Aleve Or Advil For Lower Back Pain
You May Like: What Does An Eye Ulcer Look Like
Gi Issues Caused By Kidney Stones
Normally, kidney stones cause symptoms such as pressure and pain in your lower back, fever, frequent urination, discomfort urinating, and bloody or discoloured urine. However, sometimes kidney stones can cause gastrointestinal symptoms such as nausea, vomiting, and stomach discomfort.
If youre experiencing sudden low back pain and gastrointestinal discomfort, dont ignore the possibility that it might be kidney stones.
Also Check: Advil For Lower Back Pain
Ulcerative Colitis Symptoms You Should Never Ignore
Ulcerative colitis is an autoimmune disease in which the immune system attacks the colon and causes a range of symptoms, both in the GI tract and around the body.
Symptoms of ulcerative colitis, a type of inflammatory bowel disease , can vary widely depending on how much inflammation a person has and where the inflammation is located.
Abdominal pain and bloody diarrhea are the most common warning signs of UC, and can range from mild and intermittent to severe and chronic. The pain of UC is quite common and can significantly impact quality of life. Ulcerative colitis symptoms tend to come and go, often with extended periods of time in between flares. These are called remission periods.
The disease tends to develop gradually over time, so you might not automatically think of ulcerative colitis or IBD if you have occasional abdominal pain or digestive distress.
Ongoing inflammation along with ulcers and abscesses in the intestines are additional common causes of pain. Scarring in the lining of the intestinal tract can lead to painful obstructions. Pain may occur in different areas such as the abdomen or rectal area, depending where the inflammation is located. For example, people may experience moderate to severe pain on the left side of the abdomen if the UC affects the rectum and the lower segment of colon.
UC symptoms might ebb and flow, but they wont go away unless you see a gastroenterologist and start treatment.
Recommended Reading: How To Diagnose Gastric Ulcer
Back Pain And Ulcerative Colitis
| | |
Research indicates that nearly 25 percent of people with inflammatory bowel disease including ulcerative colitis and Crohns disease experience chronic lower back pain. Ankylosing spondylitis and axial arthritis both of which can cause back pain are two common causes of back pain for people with UC.
That said, a doctor may not suspect that a person with back pain has UC unless they also experience gastrointestinal symptoms. If you do experience back pain, its important to let your doctor know even if you dont suspect its related to UC. They will be able to determine the cause of your pain and work with you to find the best way of managing it.
A person having backaches may not realize theyre related to digestive problems or think to mention it to their doctor. However, ulcerative colitis can cause extraintestinal symptoms including back pain.
Although back pain can result from other causes, such as injury or overexertion, UC-related back pain stems from inflammation. Generally speaking, people with ulcerative colitis can trace their back pain to spondyloarthritis. Spondyloarthritis, also known as spondylitis, is a type of arthritis that causes inflammation specifically in the axial joints those of the spine, chest, and pelvis. Spondyloarthritis includes axial arthritis and ankylosing spondylitis.
Link Between Lower Back Pain And Bowel Problems
When we talk about bowel disorders, we are referring to conditions that affect your small intestines. Bowel disorders can also affect other parts of your digestive system, like your large intestine. Bowel problems are usually caused by smoking, diet, microbial and immunologic factors, and a family history of Crohns disease.
The most familiar symptoms of bowel disorders are abdominal pain, swelling, bloody stool, constipation, diarrhea, and gas. What many people do not realize is that bowel problems are also related to lower back pain. The truth is that bowel problems and lower back pain are inextricably linked. This is because the nerves of both the back and the abdominal area run through the lower part of the spine.
If you suffer from abdominal pain and bloating, it is likely that you also suffer from irritable bowel syndrome. In addition to the classic symptoms like bloating and gas, individuals with IBS often develop extraintestinal symptoms, or symptoms that involve parts of the body beyond the gut. This can include sleep problems, headaches, trouble urinating, fatigue, muscle pain, pain in the pelvis or jaw, and back pain.
You May Like: Can Stomach Ulcers Cause Gas
Diagnosing Lower Back Pain
To diagnose lower back pain, a doctor will first do a physical exam. Theyll look at how well you move and if your back has any visible issues.
Then theyll take a medical history. This will cover your symptoms, any recent injuries, previous back issues, and the severity of your pain.
A physical exam and medical history are often enough for a doctor to determine the cause of your pain. However, they may also need to do an imaging test. Potential tests include:
- X-ray, which can find broken or misaligned bones.
- CT scan, which shows soft tissues such as the discs between vertebrae and potential tumors
- myelogram, which uses dye to enhance the contrast in a CT scan or X-ray to help a doctor identify nerve or spinal cord compression
What Is The Makeup Of The Lower Back
To understand numerous reasons for lower back pain, it is important to appreciate the typical style of the cells of this area of the body. Vital frameworks of the lower back that can be related to signs in this region consist of the bony lumbar spinal column , discs between the vertebrae, tendons around the spine and also discs, spinal cord and also nerves, muscles of the lower back, interior body organs of the hips and abdominal area, as well as the skin covering the lumbar location. Ulcerative Colitis And Lower Back Pain
The bony lumbar back is developed to make sure that vertebrae stacked together can offer a movable assistance structure while also protecting the spine from injury. The spinal cord is composed of nervous cells that prolongs down the spinal column from the mind. Ulcerative Colitis And Lower Back Pain
Each vertebra has a spinous process, a bony importance behind the spine, which guards the cords nervous cells from influence injury. Spine also have a strong bony body before the spinal cord to give a platform appropriate for weight bearing of all tissues above the buttocks. The back vertebrae stack right away atop the sacrum bone that is located in between the buttocks.On each side, the sacrum satisfies the iliac bone of the hips to create the sacroiliac joints of the butts.
You May Like: How To Tell Stomach Ulcer
Read Also: How To Lose Weight With Stomach Ulcers