Treatments For Ibs And Ibd
Treatment is very different for IBS and IBD. If you have IBD, you will take medications that lower the inflammation in the GI tract such as anti-inflammatory medications, biologic agents, and immunomodulators which can reduce the damage IBD is causing.
Treatment of IBS is different. You and your providers will focus on treating the specific symptoms you are having. Changes to your diet and exercise habits are a good first step.
Heres a few examples of some foods to avoid when you have IBS:
-
Apples
If diarrhea is one of your main IBS symptoms, you might take medications that reduce the diarrhea, such as rifamixin and eluxadoline . If you are more often constipated, you might take medications that help keep the GI tract moving, such as lubiprostone , linaclotide , or plecanatide .
You might also need treatment of stress, anxiety, or depression with medications or therapy if you and your provider think this is playing a role in your IBS.
What Side Effects Of Ibd Can Cause Malnutrition
There are several reasons why people with IBD may be at risk for malnutrition. The following list includes some side effects that contribute to malnutrition.
- Inadequate food/fluid intake may by caused by nausea, abdominal pain, loss of appetite or altered taste sensation
- Increased losses â intestinal inflammation during acute flares results in increased protein losses, losses from fistula fluids, diarrhea and bleeding
- Increased nutritional needs â inflammation or infection increases metabolic requirements
- Malabsorption with Crohn’s disease may be caused by severe intestinal inflammation, resection of small intestine and medications, such as prednisone and sulfasalazine
Data Safety And Monitoring Board
Any questions regarding patient exclusions, serious adverse events and potential study termination will be reported to and reviewed by the DSMB. In addition, the DSMB will annually monitor the study. Where appropriate, recommendations will be made to continue, modify or terminate the study or to unmask participants in case of serious adverse events.
Don’t Miss: How To Measure Pressure Ulcers
How Can I Cure Ibs Permanently
There is no permanent and medically known cure for IBS, but there are several tips that serve as treatment options to alleviate or get rid of the symptoms. Lifestyle tips include dietary modifications, high fiber diet , physical exercise, stress management and prescription medications. There is no specific diet for irritable bowel syndrome, and different individuals react differently to different foods.
Mucosal Inflammation Dysbiosis Intestinal Permeability And Visceral Hypersensitivity
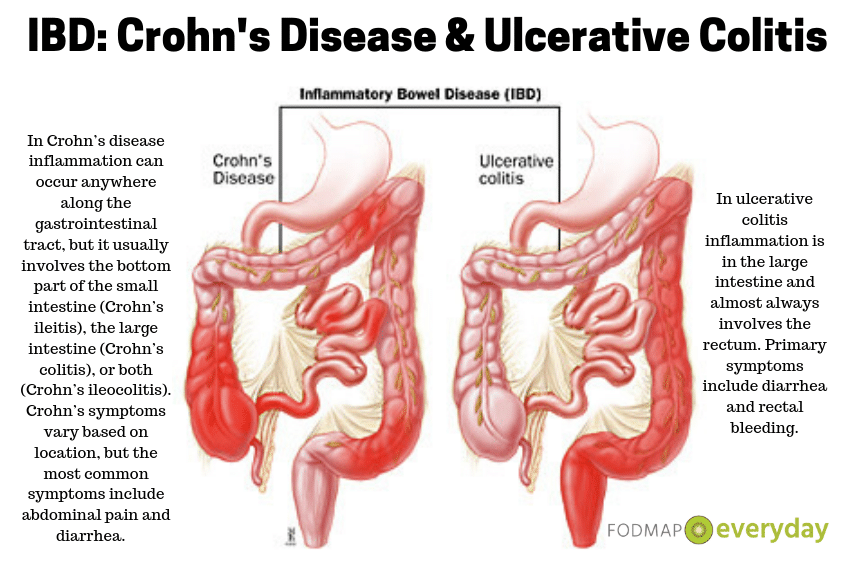
Mucosal inflammation is the hallmark of UC. However, recent advances in the understanding of the etiology of IBS suggest that subclinical mucosal inflammation and increased mucosal barrier permeability may play a role in the development of symptoms. Studies have demonstrated higher levels of circulating proinflammatory cytokines in peripheral blood, and higher levels of proinflammatory cell infiltrates in the intestinal mucosa of IBS patients than in patients in the control group. The exact cause of this inflammation is uncertain, but may be related to an alteration in the gut microbiome, with evidence of a dysbiosis in IBS, and a relative abundance of pro-inflammatory species compared with healthy individuals without IBS.
The advent of 16s ribosomal RNA gene sequencing has provided a specific and inexpensive method of studying microbial diversity in the gut and with it further investigating the association of altered gut microbial composition with the development of various GI diseases including IBS, IBD, and colorectal cancer. The mechanism by which gut microbes may be able to affect intestinal permeability and thus propagate symptoms compatible with IBS is complex, but dysregulation of the enteric nervous system in response to an altered microbiome has been proposed as a cause.,
You May Like: What To Do When You Have An Ulcer
What Life With Chronic Intestinal Pseudo Obstruction Is Actually Like
This is reality. I drove my car for the first time since June a few days ago. I had to drive 5 hours to Michigan to see my doctor. Just doing that simple thing has wiped me out. I slept until almost 2PM the day after I got back to Illinois and Ive been running a slight temperature and feel overall awful. My nausea has been a lot worse the past month or two but we switched my nausea med to the IV version so hopefully that will help.
Living with the rare disease, CIPO and Intestinal failure caused by CIPO is difficult. Like really, really difficult. Normally if a patient comes into the ER with extremely dilated loops of bowel with air fluid levels and has symptoms of severe pain, nausea, and vomiting they are treated as an emergency. They are admitted and will have an NG tube placed for decompression and will be NPO and put on IV fluids and pain medicine. Sometimes surgery is required. Luckily for them there is a resolution. An end in sight.
Dilated loops of bowel with air fluid levels is the radiographic picture of a bowel obstruction. That is what a bowel obstruction looks like on imaging tests like CT scans and X-rays, MREs and barium follow-throughs. In patients with severe CIPO we live that every day of our lives but there is no fix. No surgery or solution to make it go away like for patients with actual mechanical obstructions or temporary ileus.
Every
day.
Does Stress Affect Ibs Or Ibd
- The diet for IBS is far simpler.
- Drink plenty of water.
- Avoid any foods that make you bloated or gassy.
- Do not over-eat fiber as this may cause gas and bloating. Probiotics may help reduce symptoms.
If you have irritable bowel syndrome or inflammatory bowel disease diet changes may be useful for patients with IBS, and especially IBD, to seek advice from a dietician.
Also Check: Stomach Ulcer Blood In Stool
Do Any Medications Have Nutritional Side Effects
Moderate to severe flares of IBD are often treated with corticosteroids , cholestyramine and 5-ASA compounds . These medications have nutritional side effects that should be addressed. If you use any of these medications, talk to your doctor or registered dietitian for treatment advice.
- Prednisone causes decreased absorption of calcium and phosphorus from the small intestine. It also causes increased losses of calcium, zinc, potassium and vitamin C. With continual use of high doses of prednisone, the result may be bone loss and development of bone disease. People on prednisone may need up to 1200 milligrams a day. Protein needs also are increased for people taking prednisone because it increases protein breakdown in the body.
- Cholestyramine decreases absorption of fat-soluble vitamins , as well as folate, vitamin B-12, calcium and iron.
- Sulfasalazine interferes with folate absorption. People taking this drug also should take a 1 milligram folate supplement each day.
Who Is At Risk Of Ulcerative Colitis
- Age: Ulcerative colitis may affect any age group, although there are peaks at ages 15 to 30 years, and again at ages 50 to 70 years.
- Race/ethnic background: Ulcerative colitis is more common among caucasians and in people of Ashkenazi Jewish descent.
- Family history: People with a first-degree relative with ulcerative colitis are at greater risk of developing the condition.
Read Also: How To Know If You Have Ulcerative Colitis
How Ulcerative Colitis Is Treated
Treatment for ulcerative colitis aims to relieve symptoms during a flare-up and prevent symptoms from returning .
In most people, this is achieved by taking medicine, such as:
- aminosalicylates
- corticosteroids
- immunosuppressants
Mild to moderate flare-ups can usually be treated at home. But more severe flare-ups need to be treated in hospital.
If medicines are not effective at controlling your symptoms or your quality of life is significantly affected by your condition, surgery to remove your colon may be an option.
During surgery, your small intestine will either be diverted out of an opening in your abdomen or be used to create an internal pouch that’s connected to your anus called an ileoanal pouch.
How Is Inflammatory Bowel Disease Treated
IBD is treated with medicines, changes in diet, and sometimes surgery. The goal of treatment is to relieve symptoms, prevent other problems and future flare-ups, and possibly heal the inflamed intestines.
A doctor may recommend:
- anti-inflammatory drugs to decrease the inflammation
- immunosuppressive agents to prevent the immune system from causing inflammation
- biologic agents to block proteins that cause inflammation
- nutrition therapy to give the bowel a chance to heal
Doctors may prescribe antibiotics to prevent or treat infections. People with IBD should always check with their doctor before using antidiarrheal medicine.
Because some medicines make it harder to fight infections, it’s important that your child be tested for tuberculosis and have all recommended vaccines before starting treatment.
Poor appetite, diarrhea, and poor digestion of nutrients can make it hard for people with IBD to get the calories and nutrients they need. Children with IBD should eat a variety of foods, drink plenty of fluids, and avoid foods that make symptoms worse. Some kids may need vitamin and mineral supplements, calcium or vitamin D. Kids who are not growing well may need special formulas to boost calories and nutrition.
Someone with IBD might need surgery if:
- the bowel gets a hole
- the bowel gets blocked
- symptoms don’t respond to treatment
Also Check: Foods For Gerd And Ulcers
Does Ibs Get Worse With Age
IBS is long-term disorder of the gut and is an inevitable part of aging. It comes and goes over time. The sensitivity of the gut nerves may elevate with age and the symptoms overlap is possible. Different signs and symptoms related to IBS may show up with age. However, there are some ways like exercise, avoidance of foods that irritate the digestive system etc. that help to help reduce the overall risk of IBS and aid in reducing the symptoms.
What Are The Risk Factors Of Ulcerative Colitis
The cause of ulcerative colitis is unclear, but its thought that a combination of genetics and environmental factors are at play. Up to 20 percent of people with ulcerative colitis have a parent, sibling or child with the disease.
Ulcerative colitis is more common for people living in urban, industrialized areas compared to undeveloped countries, which indicates that highly refined diets may play a role. Although all ethnic groups are affected, the problem is most common among Caucasians and people of Eastern European Jewish descent.
Lastly, there appears to be a connection to nonsteroidal anti-inflammatory medications. Its not that these medications cause the disease but, because they inflame the bowel, they can worsen symptoms. This category of medication includes ibuprofen , naproxen sodium and diclofenac sodium .
Recommended Reading: Can Ulcerative Proctitis Be Cured
Are Inflammatory Bowel Diseases Different From Irritable Bowel Syndrome
Yes! IBD and IBS are very different, even though the symptoms can be similar. Most importantly, the treatments are not the same. Working with your provider to figure out what condition you have is important so that you can find the best treatment.
IBS is much more common than IBD. About 11% of people have IBS. That makes it about 10 times more common than IBD.
Fortunately, its also less serious. IBD is caused by inflammation and damage to the GI tract. With IBS, this isnt the case. IBS is a collection of gut symptoms caused by unusual functioning of the bowel.
Similar Symptoms With Important Differences: Colitis Vs Ibs
The main symptoms of colitis are ongoing diarrhea and pain in the stomach. Some people will feel very tired or even exhausted, and they may also lose weight and find that their appetite goes down. Sufferers of the ulcerative type may find that when they pass a bowel movement, they also pass blood or mucus however, blood is not present in microscopic colitis.
Irritable bowel sufferers can have ongoing diarrhea as a key symptom, but they may also swing from diarrhea to constipation or only ever have constipation. Unlike colitis, IBS does not cause bleeding as the bowel itself is intact, so even a severe bout of IBS does not damage the gut. Weight loss and fatigue are also not symptoms of IBS, but stomach pain definitely is, along with bloating and an urgent need to get to a bathroom.
Usually IBS sufferers only experience bowel and stomach symptoms, but colitis can cause problems with other parts of the body such as painful swelling of the joints, eye or skin irritation and mouth ulcers. If the condition is very severe, patients can also have a high temperature or fast heartbeat.
Colitis is similar to IBS in that it can come and go over time. Patients with both disorders might refer to a flare-up when their symptoms are particularly bad, but they will usually have times when they feel much better and the symptoms are in remission.
Read Also: Smoking And Crohn’s Disease Ulcerative Colitis
Is There A Connection Between Ibs And Colitis
Colitis is defined as inflammation in the large intestine. It can be caused by many things, including:
- Infection
- Autoimmune disease
- Lack of blood supply
- Diverticulosis
- Other serious conditions
Colitis can result in symptoms that are similar to those of irritable bowel syndrome . This raises the question: Is there an overlap or connection between IBS and colitis?
Types Of Colitis And Ibs Pain
Abdominal pain is a symptom of both IBS and colitis.
A person with IBS may experience stomach cramps, pain, and discomfort. They can relieve the pain by going to the bathroom and having a bowel movement. They may also feel bloated and have a lot of stomach gas.
A person with colitis also experiences abdominal pain, but this is due to gut inflammation. The pain could be from:
- Narrowed intestines : These are blockages or obstructions, making it difficult for food to pass.
- Fistulas: Some pain may be a result of ulcers or sores on the inside of the intestine wall. These may link and cause pain in other parts of the body, including a persons bladder, vagina, or skin.
- Bacteria: Too many bacteria in the small intestine could lead to gas, bloating, or cramps.
- Poorly digested food: This may cause too much gas and discomfort in the abdomen.
A person with colitis may also experience IBS symptoms.
A healthcare professional will use the following to diagnose IBS:
- medical history, including family and close relative medical history
- physical examination
- diagnostic testing, such as collecting a stool sample
Diagnosis for colitis is typically the same. It will begin with a medical history as well as a physical examination. A person may consider sharing previous lab results or a summary of previous visits to a healthcare professional.
IBS and colitis could both present as colon cancer, and a doctor will be able to rule this out.
Neither IBS nor colitis has a definitive cause.
Also Check: What Are The Symptoms Of An Ulcer In Your Stomach
About Irritable Bowel Syndrome
IBS is fairly common, with anywhere from 25-45 million Americans suffering from it. The basic cause isnt understood, but you suffer symptoms because your colon muscle contracts more readily than normal. Triggers for IBS include certain foods, stress, hormones, or other illnesses.
Symptoms of IBS may involve:
- Excess gas
- Harder or looser bowel movements than normal
- Pain or cramps in the abdomen, usually in the lower half
- Diarrhea, constipation, or alternating between the two
Rectal bleeding and black stool is not a symptom of IBS. You should seek immediate evaluation at our office if you experience possible blood in your stool.
Rest assured that IBS does not raise your risk of developing other serious issues of the digestive system, including colitis, Crohns disease, or cancer.
Nutrition Tips For Inflammatory Bowel Disease
Inflammatory Bowel Disease is a term used for two specific and separate diseases: Crohn’s disease and ulcerative colitis. Nutritional recommendations are different for each disease and for each individual patient. It is important to discuss the treatments that are right for you with a registered dietitian and with your doctor.
Recommended Reading: What Should You Eat With Ulcerative Colitis
Switching To A Biosimilar: Effies Experience
At the start of 2020 the government announced that coverage was changing for people who take Remicade® for the treatment of Crohns disease or ulcerative colitis. This meant that patients receiving the biologic drug infliximab, marketed as Remicade®, would see this coverage discontinue with new coverage for the biosimilar version: Inflectra and Renflexis.
Ulcerative colitis advocate Effie was one of those people. In this self-produced video, Effie talks all about her experiences with switching to a biosimilar, takes us through her first Inflectra infusion, and answers some of the same questions you may be asking yourself if you will be going through the same process:
- What is a biosimilar?
Faq: Dietary Management Of Ibd

Information regarding dietary treatments for IBD is often confusing. Many people receive information telling them to avoid entire food groups or specific foods. However, there is no need to avoid foods unless they worsen your symptoms. It is best to restrict as few foods as possible to increase the chances that you are getting a balanced, nutritious diet. This is important for maintaining the function of your digestive tract and your overall health.
You May Like: What Foods Should I Eat With Ulcerative Colitis
Why The New Site
A decade ago when I started Inflamed & Untamed I had no idea what I was starting. In fact my site wasnt even called Inflamed & Untamed until months later. This all began one day during the summer when I was out of work , just out of the hospital , and tapering off steroids again! I just wanted something to do and so I started my site on Tumblr and I also started making videos on YouTube.
I had no idea that I would receive the kind of traffic I ended up getting and it all happened so fast. I never went into it thinking I was creating anything more than a small personal blog that would maybe get a few followers and connect me to a community. This was back before Instagram existed and when there were not very many patient advocates out there at all especially on YouTube. I think that was part of my unexpected success. Here I am now a decade later and all this time Ive been a patient advocate which is an honor and privilege I hold near and dear to my heart.
You May Like: Doctors Specializing In Ulcerative Colitis