Caring For A Pressure Sore
Stage I or II sores will often heal if cared for carefully. Stage III and IV sores are harder to treat and may take a long time to heal. Here’s how to care for a pressure sore at home.
Relieve the pressure on the area.
- Use special pillows, foam cushions, booties, or mattress pads to reduce the pressure. Some pads are water- or air-filled to help support and cushion the area. What type of cushion you use depends on your wound and whether you are in bed or in a wheelchair. Talk with your health care provider about what choices would be best for you, including what shapes and types of material.
- Change positions often. If you are in a wheelchair, try to change your position every 15 minutes. If you are in bed, you should be moved about every 2 hours.
Care for the sore as directed by your provider. Keep the wound clean to prevent infection. Clean the sore every time you change a dressing.
Avoid further injury or friction.
- Powder your sheets lightly so your skin doesn’t rub on them in bed.
- Avoid slipping or sliding as you move positions. Try to avoid positions that put pressure on your sore.
- Care for healthy skin by keeping it clean and moisturized.
- Check your skin for pressure sores every day. Ask your caregiver or someone you trust to check areas you can’t see.
- If the pressure sore changes or a new one forms, tell your provider.
Take care of your health.
Predictors For Heel Pressure Ulcer
No variables assessed in the ambulance or at the ED predicted heel pressure ulcer during the hospital stay. However, at Day 1 at the ward, statistically significant differences were identified between patients who later developed heel pressure ulcer and those who did not, regarding the MNS sub-categories , physical activity , mobility , and incontinence ), as well as total risk score . Also, at Day 1 at the ward, significantly fewer patients with a heel pressure ulcer or who developed heel pressure ulcer later during their hospital stay received an oral nutritional supplement compared to those with no heel pressure ulcer . Statistically significant differences could not be noted regarding other preventive actions, such as using a pressure-reducing mattress and a turning schedule.
Evaluation Of The Product
The evaluation of the Repose foot/heel protectors was carried out over a three-month period. Inclusion criteria selected patients who:
– Had sustained a fractured neck or shaft of femur
– Were anticipated to be on bed-rest for 24 hours or more and were over 70 years old
– Had a spinal injury .
The limb was excluded from the study, if on admission:
– The heel had a ulcer classified as stage 3 or greater
– The leg was in a plaster of Paris cast
– Specific treatment regimens prescribed by the patientâs consultant would not allow Repose boots to be worn .
The evaluation took the following format: patients were fitted with a pair of Repose boots on admission to the ward. Heels were reviewed daily for signs of pressure or friction damage and recorded on the data sheet. If the patient developed a stage 2 ulcer during the study the use of the boots was discontinued and preventative management was reassessed.
If the patient had to be taken out of the study for any other reason this was documented on the data form. Otherwise the Repose boots were worn at all times when the patient was on bed rest until discharge from the ward or transfer back to referring hospital.
Read Also: Can Stomach Ulcers Be Cancerous
New Sizes Now Available
The Repose Foot Protector is now available in a range of sizes to support a variety of patient needs.
New sizes include the Repose Foot Protector Small and Repose Foot Protector Extra Small products.
To learn more about Repose Foot Protector please contact us using the button below.
- Low Air technology distributes weight evenly and doesnt lose its shape
- Designed to relieve pressure on soft tissue areas and provide comfort
- Lightweight for easier transport
- Easy to clean and will deflate down to a compact size
- Helps distribute pressure evenly
- Repose can be cleaned and reused
- Can be used with other dynamic or static support surfaces
- Reduces impact of pressure, friction and shear
Professional Guidelines And Recommendations
Wound Ostomy and Continence Nurses Society GuidelinesMaintaining alignment may be difficult if the patient moves. In addition, pillows do not prevent plantar flexion contracture or lateral leg and foot rotation.1
AHRQ/AHCPR Supported Clinical Practice GuidelinesIndividuals in bed who are completely immobile should have a care plan that includes the use of devices that totally relieve pressure on the heels, most commonly by raising the heels off the bed.2
NPUAP/EPUAP Prevention GuidelinesEnsure that the heels are free of the surface of the bed Heel-protection devices should elevate the heel completely in such a way as to distribute the weight of the leg along the calf without putting pressure on the Achilles tendon.3
Association of Perioperative Registered Nurses Standards Recommended Practices and GuidelinesUse devices that eliminate or redistribute pressure to preventperioperative* heel pressure injuries.4
*Perioperative defined as a pressure-related deep tissue injury under intact skin that presents within the first 5 days following surgical procedures.
Also Check: Artificial Sweeteners And Ulcerative Colitis
Prevalon Heel Protectors Reducing Heel Pressure Ulcer Risk
Multiple guidelines recommend the use of a heel protection device that completely offloads the heel to help prevent the development of heel pressure ulcers. Prevalon® Heel Protectors are the number one brand of heel protection. They offer continuous heel offloading to protect your patients heels.
Choose the optimal heel protector
Experts suggest the optimal heel protector should go beyond offloading the heel. In order to effectively protect the foot and lower limb, a heel protector should prevent foot drop and use an anti-rotation wedge to keep the foot in a neutral position to protect the peroneal nerve. Prevalon® Heel Protectors are available with a contracture strap to help prevent the foot from dropping and an anti-rotation wedge to keep the limb from externally rotating. They also feature a unique dermasuede interior designed to gently grip the limb so it remains fully offloaded, even when the patient moves.
Proven prevention results and cost savings
A study published in JWOCN demonstrated a 100% prevention of both heel pressure ulcers and plantar flexion contracture over a seven month period when using Prevalon® Heel Protectors.
Why Heelift Boots Create A Cooler Drier Microclimate
There are a few features of Heelift® Brand Boots that help create the desired cooler, drier microclimate that prevents pressure ulcer development. As the above cut-away shows, HEELIFT® completely offloads the heel, allowing heat and moisture to escape so long as the patient is turned regularly. Additionally, the ventilation holes found in the HEELIFT® AFO, HEELIFT® Glide, and HEELIFT® Classic further help the flow of heat and moisture.
You May Like: How Do You Cure Ulcerative Colitis
Ulcer Aids Sheets Boots Socks And Heel Protectors
Ulcer Aids: Pressure ulcers are areas of injured skin that remain in the same position for too long. Continuing education for pressure ulcer prevention: Taking the pressure off!
They commonly form where the bones are closer to the skin, such as the ankles, heels and hips.
The risk is greater if you are confined in a bed, you use a wheelchair or you can not change positions.
Pressure ulcers can cause serious infections, some of which can be life-threatening.
They can be a problem for people in specialized care centers.
This is one of the most common health problems we face in our daily work.
Preventing The Development Of Heel Pressure Ulcers
Patricia Davies Senior lecturer, Course leader tissue viability pathway and modules, Birmingham City University, Birmingham, England
Why you should read this article:
-
» To improve your knowledge of the causes and risk factors associated with heel pressure ulcer development
-
» To understand the various elements of an effective risk assessment for pressure ulcers
-
» To provide effective patient care in the prevention of pressure ulcers, based on the latest clinical evidence and research
The heel is a common site for pressure ulcer development, particularly in people who are supine or semi-recumbent because of immobility. There is little protective subcutaneous tissue and no muscle or fascia within the heel, which means that it is vulnerable to pressure, friction and shear forces. Heel pressure ulceration remains a clinical challenge for nurses and the wider healthcare team, as well as a cause of pain and physical debilitation for the patient. This article examines the risk factors for heel pressure ulceration, and details patient assessment and specific measures that can be undertaken to prevent the development of heel pressure ulcers.
Nursing Standard. doi: 10.7748/ns.2018.e11294
Recommended Reading: Is Soy Sauce Ok For Ulcerative Colitis
Why Is Microclimate Important
In a recent study published in the Journal of Tissue Viability, Amit Gefen PhD. Dept. of Biomedical Engineering wrote, There is increasing evidence that thermodynamic conditions within and around skin tissue strongly influence the susceptibility of skin to SPUs Successful pressure ulcer prevention depends upon a complex balance between two sets of parameters the external loads applied to the skin and soft tissues, and the intrinsic ability of the skin and soft tissues to withstand prolonged or excessive loading. If the intrinsic resilience of the skin and soft tissues deteriorates, pressure damage is more likely to occur. Hence, a full understanding of a patients conditions, and immediate environment, including anything that may cause the patients skin to increase in temperature or moisture should be considered.
What Is A Pressure Ulcer?
A pressure ulcer is an injury to the skin as a result of sustained pressure applied to the skin over time . The pressure results in reduced blood flow and eventually causes skin breakdown and the development of an open wound. If the conditions leading to the sore are not rapidly corrected, the localized skin damage may spread to deeper tissue layers, affecting muscle, tendon, and bone. If not adequately treated, open ulcers can become a source of pain, disability, and infection.
Why is Prevention Important?
Customers Were Also Interested In
Vat Refunds For Disabled Users
If you are chronically sick or disabled you may be eligible to claim back the VAT on your Repose order.
Quick Guide
Step 2: Download and complete the Eligibility Declaration Form.Step 3: Send the completed form to Frontier Medical Group.Step 4: If eligible we will refund the VAT to the card you used to process your Repose order.
To apply for VAT relief please complete your purchase and download the Eligibility Declaration Form. Please send the completed form to Frontier Medical Group, we will then process your application. If you are eligible for VAT relief we will refund the VAT to the card you used to process your order payment.
For further details please see our terms and conditions or visit the HMRC website.
Don’t Miss: Drugs To Treat Ulcerative Colitis
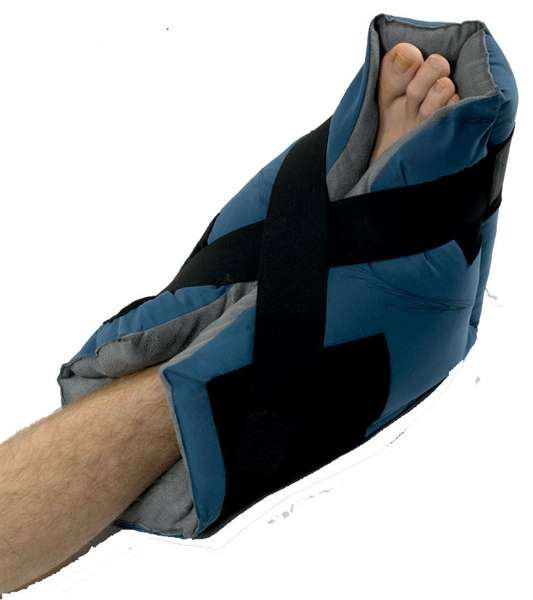
The Repose Foot/heel Protector
Repose foot protectors are designed specifically to minimise the risk of pressure damage to heels. They come in the form of splints made of Platilon, a polyurethane material with unique stretch, thermal and vapour-permeable properties. They are most effective when the patient is recumbent, semirecumbent or upright while on bed-rest, as the heels are supported above a void and therefore close to zero pressure, while the malleoli are protected by air-filled compartments.
The foot protectors are inflated using a hand-help pump. A valve ensures they are inflated to the correct pressure with no chance of over-inflation. This provides a pressure-reducing splint where the weight of the lower leg is redistributed over a wider area.
Prevention Of Heel Pressure Ulcers In An Orthopaedic Unit

18 June, 2002
VOL: 98, ISSUE: 25, PAGE NO: 53
Anne Wilson, RGN, BSc, is tissue viability nurse, Royal Alexandra Hospital, Paisley
The development of hospital-acquired pressure ulcers on the heel is a well-acknowledged problem . In fact, after the sacrum the heels are the second most common anatomical site for the development of ulcers , and their incidence has increased steadily over the past few decades .
Although tissue breakdown is a complex multifactorial process, the focus with pressure ulcer development in the heels is on extrinsic factors such as pressure, shear and friction, with the most plausible explanation being the failure to relieve pressure. While many advances, such as pressure-relieving mattresses and beds, have greatly reduced the incidence of sacral ulcers . Krasner recognised that, even with pressure reduction, most support surfaces do not adequately relieve heel pressure.
Pressure ulcers may form when heel pressure on the mattress exceeds the capillary closing pressure and the heel position is not changed frequently enough . The heel is at increased risk of ulceration as it has a relatively low resting blood perfusion level if subjected to lower pressures than 32mmHg .
Cheney suggests this problem is compounded by orthopaedic surgical procedures requiring long periods in the operating room and in recuperation. To prevent the development of heel ulcers, therefore, predisposing factors must be identified, minimised and/or relieved .
Recommended Reading: Low Residue Diet For Ulcerative Colitis
Heel And Elbow Protector Applications And Uses
Bed Sore Treatment
Material options for pressure relief include foam and synthetic sheepskin construction to achieve softness with a boot-like fit. Both options offer extra padding and comfort to protect bony prominences. These materials naturally contour to the body for complete protection. Some protector options are universal to apply to either the heel or elbow and fastens with a hook and loop strap. Sheepskin is washable for multiple uses.
Another option for pressure relief is to use a free-standing offloading device like the HeelZup. The patient props up the feet onto a high-density foam platform to relieve pressure from the heels. This product is free-standing and doesn’t require direct application to the foot or elbow, which may be helpful to patients with wounds.
Examples:
- Medi-Pak Heel and Elbow Protector Pads, 1203735-852, are constructed out of foam with a hook and loop fastener to protect either the foot or heel.
- Skil-Care Triple-Ply Heel Protector Pads, 503010, have triple-ply sheepskin with side vents to create airflow and keep skin dry.
Protection from Shear and Friction
Sitting for a long period can cause skin breakdown. Repositioning the arms or feet adds friction to the vulnerable skin. Protection is simple and easy with heel and elbow pads. The stretchable woven fabric places a barrier to reduce downward pressure and friction.
Examples:
Frequently Asked Questions
Compare Products
You have no items to compare.
My Quote
Bootees To Aid In The Prevention And Treatment Of Pressure Ulcers
Parafricta® Bootees are made using a smart, strong, breathable, silk-like, low-friction, proprietary fabric that reduces the risk of friction and shear-related skin breakdown on the feet.
The foot is particularly vulnerable to pressure ulcers and other skin damage. This is because people frequently dig in their heels to push themselves up in bed, or rub their feet on the bed due to agitation or spasms. When subjected to friction and the associated internal shearing, the cells and tissues of the feet begin to break down, which first manifests itself as redness and inflammation and may progress to blistering and ulceration .
Parafricta® Bootees provide a comfortable way to protect the feet and ankles from the risk of friction and shear-related pressure ulcers and other skin conditions.
There are two types of bootee.
Washable and reusable bootees in a slip-on style or Velcro® brand closure style . These models may be prescribed and are available from our online store. Please refer to the User Guide.
Please note: Our Bootees are sold individually
You May Like: Removing Colon Due To Ulcerative Colitis
Heel Pressure Ulcer Across The Entire Care Delivery Chain
Skin inspections were performed at different time points across the care delivery chain for the majority of the included patients ward day 1 n=168 ward day 3 n=100 and ward day 7 n=49 ). Heel pressure ulcer developed at different stages: 15 patients were identified with heel pressure ulcers at the ED, 18 patients at day 1, 12 patients at day 3 and nine patients at day 7. A total of 39 patients developed a heel pressure ulcer during their hospital stay. The heel pressure ulcer categories varied between 1 and 3 at the ED and between 1 and 4 at the ward. There were no statistically significant differences regarding the patients vital signs, measured in the ambulance and on admittance to the ED, between patients who developed heel pressure ulcer and those who did not .
Clinical Presentation Of Heel Pressure Ulcers
In the beginning, heel pressure ulcers may present with tenderness, discoloration of the skin and changes in skin temperature over the affected area. Heels that present with nonblachable erythema evidence decrease perfusion to the area, which may be due to friction or shearing forces, or injury related to pressure. Deep tissue injuries may be recognized as areas on the heel that are dark purple or reddish-purple in color, boggy or firm, and warmer or cooler to touch than surrounding tissue. The area will likely be tender and may develop blisters filled with blood or serum. As conditions deteriorate, the blisters may dry and become black in color an open wound may develop from the area. .
Read Also: I Think I Have An Ulcer What Should I Do
Three Heel Protectors That Effectively Grip The Limb
Available from Iskus Health in
- United Kingdom
- Republic of Ireland
The Prevalon Heel Protector was specifically designed to address the problem of patient movement and its negative effect on heel offloading. Prevalons unique dermasuede fabric interior gently grips the limb so it remains fully offloaded, even when the patient is moving.
Our specialized fabric and coating creates maximum grip control with the texture of fine velvet. This soft fabric contours to and cradles the leg, calf, ankle and foot to help prevent them from rotating within the boot or sliding out of the bootmaintaining effective heel offloading.
Dermasuede fabric holds the limb securely in place while preserving patient comfort. Its also a breathable material, so the limb remains cool while inside the heel protector.