Chronic Leg Ulcers: Epidemiology Aetiopathogenesis And Management
Shubhangi Vinayak Agale
1Department of Pathology, Grant Govt Medical College, Byculla, Mumbai 400008, India
Academic Editor:
Abstract
Chronic leg ulcer is defined as a defect in the skin below the level of knee persisting for more than six weeks and shows no tendency to heal after three or more months. Chronic ulceration of the lower legs is a relatively common condition amongst adults, one that causes pain and social distress. The condition affects 1% of the adult population and 3.6% of people older than 65 years. Leg ulcers are debilitating and greatly reduce patients’ quality of life. The common causes are venous disease, arterial disease, and neuropathy. Less common causes are metabolic disorders, hematological disorders, and infective diseases. As many factors lead to chronic lower leg ulceration, an interdisciplinary approach to the systematic assessment of the patient is required, in order to ascertain the pathogenesis, definitive diagnosis, and optimal treatment. A correct diagnosis is essential to avoid inappropriate treatment that may cause deterioration of the wound, delay wound healing, or harm the patient. The researchers are inventing newer modalities of treatments for patients with chronic leg ulceration, so that they can have better quality life and reduction in personal financial burden.
1. Introduction
2. Epidemiology
3. Aetiopathogenesis
| Vascular |
4. Pathogenesis of Chronic Leg Ulcers
4.1. Venous Ulcers
4.2. Arterial Ulcers
4.3. Diabetic Foot Ulcer
What Are Foot And Toe Ulcers
An ulcer is a wound or open sore that is either difficult to heal or keeps returning after it heals. Although there are several possible causes, youre more likely to get an ulcer on your foot or toe if you have diabetes specifically a complication called neuropathy that causes you to lose sensation. A scrape, cut or puncture can develop into an ulcer, but if you cant feel it you might not know its there.
Ulcers can lead to infections, and sometimes infections can lead to the amputation of a toe or foot. About 15% of diabetics will get a foot or toe ulcer. Around 14% to 24% of diabetes patients in the United States need an amputation after they get an ulcer.
Ulcers are sometimes painful, sometimes not. You may also experience:
- Burning.
What Is The Finest Cream For Leg Ulcers
Additionally, creams containing urea may be beneficial, since urea is a good moisturizer. Around a leg ulcer, the skin may get macerated and damaged, particularly if the lesion is actively oozing. A barrier film, such as Cavilon barrier film or LBF , protects and assists in the healing of the peri-wound skin.
Don’t Miss: Signs And Symptoms Of Peptic Ulcer
What Causes Diabetic Wounds
- Elevated blood glucose: When blood sugars reach levels higher than 200 the immune system lowers. This can contribute to the formation of wounds. A small cut that may normally heal without problems may actually become a larger, deeper ulcer due to the dysfunction of the immune system.
- Poor circulation: A common problem in patients with diabetes, is poor circulation. Elevated sugars in the blood can damage the small blood vessels, especially the ones to the foot and toes. When your foot or toes are lacking enough blood, they do not receive proper nutrients. The skin can begin to break down and an ulcer can form. This is similar to a plant that is not receiving proper water- the ends become brown, crisp and dry out.
- Neuropathy: Another common condition that can lead to diabetic ulcers, is neuropathy. Neuropathy is a loss of sensation or feeling, typically in the toes and the feet. You may step on something sharp and not feel it. This can result in a small cut that later becomes a deep wound. If you put a lot of pressure in the same place on your foot, daily, this can also result in a special type of ulcer called a pressure ulcer.
HOW CAN I PREVENT GETTING A DIABETIC WOUND?
HOW CAN I HEAL MY WOUND FASTER?
How Do I Take Care Of My Ulcers
Your healthcare provider may teach you how to care for your ulcers at home. Some instructions may include:
- Wash the affected area with mild soap.
- Keep the wound clean and dry.
- Change the bandages as directed.
- Take prescribed medications as directed.
- Drink plenty of fluids. Ask your healthcare provider how much water you should drink every day.
- Follow a healthy diet, as recommended by your healthcare provider.
- Exercise regularly, under your healthcare providers care.
- Wear appropriate shoes.
- Wear compression wraps as directed.
You May Like: What Should You Not Eat With An Ulcer
Referral To A Specialist
In some cases, your GP or nurse may decide to refer you to a specialist in conditions affecting the blood vessels .
For example, you may be referred to a vascular specialist if your GP or nurse is unsure about your diagnosis, or if they suspect your ulcer may be caused by artery diseases, diabetes or rheumatoid arthritis.
After taking your medical history and examining you, the vascular specialist may need to arrange further investigations to plan your treatment.
What Does A Venous Leg Ulcer Look Like And What Causes Them
Venous leg ulcers are sores that develop between your knee and ankle, but they typically form inside the leg near or around the ankle. They are large, shallow ulcers with uneven edges that drain or weep a lot.
Youll likely see swelling in your leg, with red, itchy skin around the wound. You may also experience tightness in your calves, as well as aching, throbbing or a feeling of heaviness in your legs. Pooled and trapped blood often causes discolored splotches in the area.
The sores sometimes affect only the skin or they may sink deeper into the fat layer, muscle, tendon and bone, she says. Severe ulcers are more likely to become infected and take longer to heal.
Your veins carry blood back to your heart, and valves in the veins stop the blood from flowing backward. When your veins have trouble sending blood from your limbs to the heart, its known as venous insufficiency. In this condition, blood doesnt flow back properly to the heart, causing blood to pool in the veins in your legs.
Our veins are just like pipes, says Ehren. When theres persistently high blood pressure in the veins of the legs with a valve that doesnt work correctly, it causes damage to the skin, which eventually breaks down and forms an ulcer.
Other possible causes for venous leg ulcers include:
- Varicose veins.
- Cancer.
- Swelling of a superficial vein .
Read Also: What Does A Duodenal Ulcer Feel Like
Causes Of Venous Ulcers
Venous ulcers most often form around the ankles.
Venous ulcers typically occur because of damage to the valves inside the leg veins. These valves control the blood pressure inside the veins. They allow it to drop when you walk. If the blood pressure inside your leg veins doesn’t fall as you’re walking, the condition is called sustained venous hypertension. That increase in blood pressure causes ulcers to form on your ankles.
Venous ulcers may also be caused by other problems with your leg veins. These include:
-
Varicose veins. These are large, bulging leg veins. They occur when valves in the leg veins dont work well, allowing blood to collect in the lower leg.
-
Chronic venous insufficiency. Like varicose veins, this condition occurs when your leg veins cant pump blood back up to your heart. Blood then pools in your lower legs, causing your legs to swell. Since the blood can’t flow well in your legs, the swelling may be extreme. This extreme swelling can put so much pressure on your skin that venous ulcers form.
Biomechanical Treatment Options/pressure Relief
Several studies have confirmed the importance of pressure relief for the healing of diabetic ulcers . Patient education is also critical . The patient must understand that even a few weight-bearing steps on an ulcerated foot can delay healing. The effectiveness of the biomechanical approach is therefore highly dependent on patient compliance.
An important study about pressure relief demonstrated using hidden activity sensors in a double-shelled total-contact cast that the TCC was actually only worn on average for 28% of daily activities . Very good data are available for the non-removable cast or walker. They revealed outstanding healing rates using two non-removable relieving aids with no difference between a TCC and TCC with an additional fixed ready-made mobility orthosis .
Recommended Reading: List Of Foods To Eat When You Have An Ulcer
Why Do Diabetics Legs Darken
Diabetic dermopathy, also known as shin spots or pigmented pretibial patches, is a skin condition that most commonly affects the lower legs of diabetics. It is believed to be caused by changes in the small blood vessels that supply the skin and minor leakage of blood products into the skin from these vessels.
Side Effects Of Leg Ulcers
- Fever
- A green and foul-smelling discharge from the ulcers
- The skin around the ulcers begins to swell
- The sores become bigger
- Inflamed skin around the ulcers
The fear of developing these complications is enough for you to try and battle these nasty-looking sores at the earliest. Taking the necessary precautions and using the remedies mentioned above on a daily basis, without fail, should help heal leg ulcers pretty fast. Nevertheless, you must see your doctor immediately if the ulcers on your leg seem non-healing or worsen in their appearance. Try the remedies listed in the article and let us know if they worked for you.
You May Like: What To Eat When You Have Ulcerative Colitis
What Are The Types Of Ulcers
There are two types of ulcers that can affect your feet and toes:
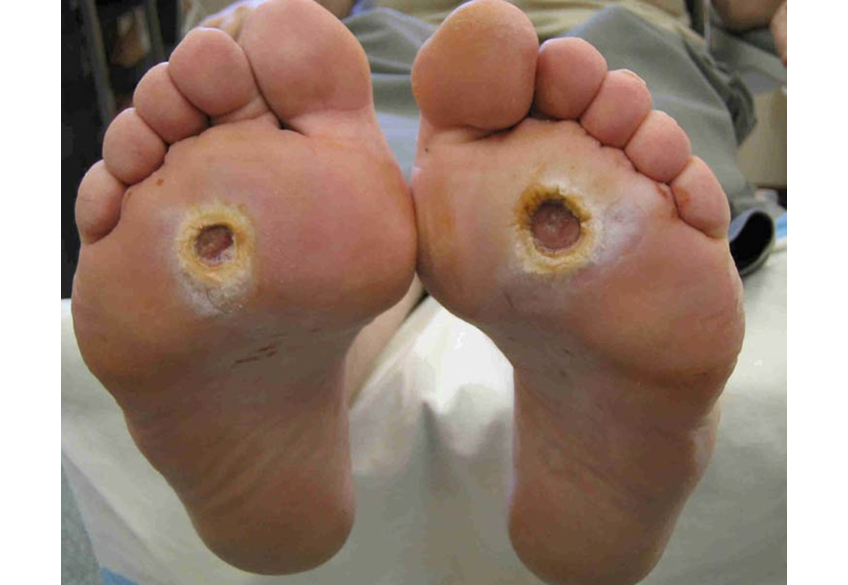
- Neurotrophic ulcers.
- Arterial ulcers.
Diabetics can get neurotrophic ulcers. Neurotrophic ulcers can be found anywhere on your feet, but theyre usually on pressure points on the bottoms of your feet. The base, or middle of the ulcer, can look different from person to person. It changes because the appearance depends on your circulation. A neurotrophic ulcer can appear pink, red, brown or black or a combination of these colors. The borders of the ulcers are punched out while the surrounding skin is often calloused.
Anyone can get an arterial ulcer. The word arterial means relating to arteries. Arteries are blood vessels that transport blood from your heart to the rest of your body, including your feet and toes. Arterial ulcers appear on your heels, the tips or your toes, between your toes where they rub against one another and anywhere your bones may protrude and rub against bed sheets, socks or shoes. They also occur commonly in the nail bed if your toenail cuts into the surrounding skin or if you had recent aggressive toenail trimming or an ingrown toenail removed.
Diagnosis And Treatment Of Venous Ulcers
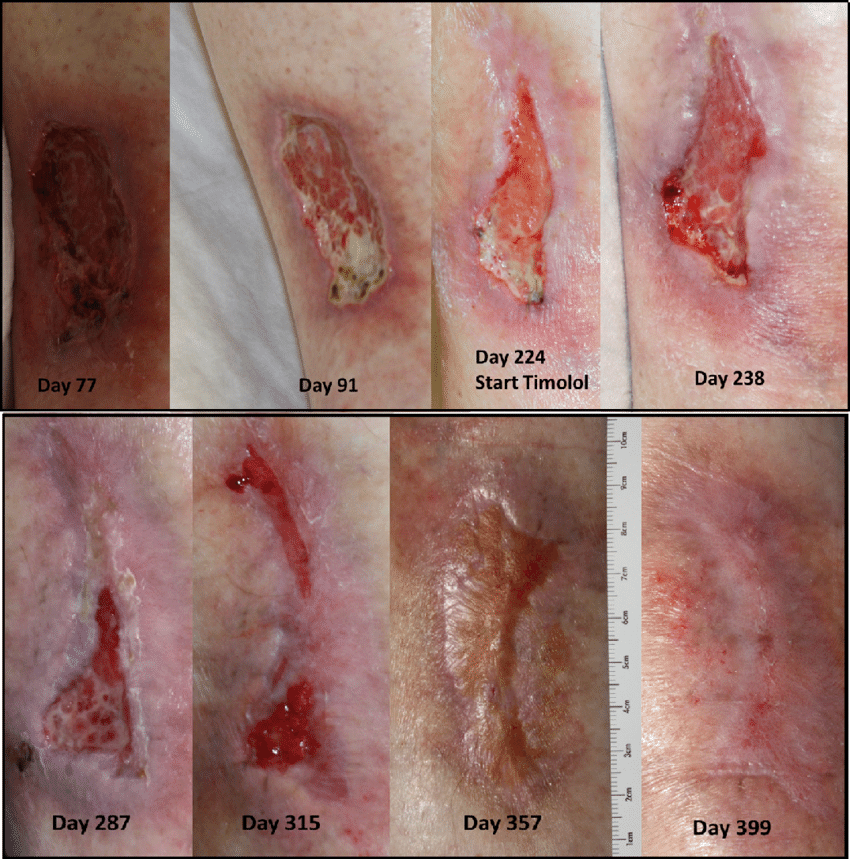
LAUREN COLLINS, MD, and SAMINA SERAJ, MD, Thomas Jefferson University Hospital, Philadelphia, Pennslyvania
Am Fam Physician. 2010 Apr 15 81:989-996.
Patient information: See related handout on venous ulcers, written by the authors of this article.
Venous ulcers, or stasis ulcers, account for 80 percent of lower extremity ulcerations.1 Less common etiologies for lower extremity ulcerations include arterial insufficiency prolonged pressure diabetic neuropathy and systemic illness such as rheumatoid arthritis, vasculitis, osteomyelitis, and skin malignancy.2 The overall prevalence of venous ulcers in the United States is approximately 1 percent.1 Venous ulcers are more common in women and older persons.36 The primary risk factors are older age, obesity, previous leg injuries, deep venous thrombosis, and phlebitis.7
Venous ulcers are often recurrent, and open ulcers can persist from weeks to many years.810 Severe complications include cellulitis, osteomyelitis, and malignant change.3 Although the overall prevalence is relatively low, the refractory nature of these ulcers increase the risk of morbidity and mortality, and have a significant impact on patient quality of life.11,12 The financial burden of venous ulcers is estimated to be $2 billion per year in the United States.13,14
You May Like: Psc Liver Disease Ulcerative Colitis
Don’t Miss: Is Okra Good For Ulcerative Colitis
Healthcare Advice For Leg Ulcers
There are some lifestyle changes you can make that will help boost healing:
- Maintain a healthy weight
- Eat a well-balanced diet that includes 5 portions of fruit and vegetables a day and protein rich foods such as eggs, fish, chicken or pulses
- Take light to moderate exercise such as cycling or walking for about thirty minutes at least three times a week
- Avoid standing or sitting for long periods of time
- Put your feet up elevate your legs above your heart.
- Every so often, move your feet around in circles, then up and down. This helps blood circulate and get back to your heart
Can Venous Leg Ulcers Be Prevented
There are several ways to help prevent a venous leg ulcer in people at risk, such as:
- wearing compression stockings
- losing weight if you’re overweight
- exercising regularly
- elevating your leg when possible
This is particularly important if you’ve previously had a leg ulcer once a leg has suffered a venous ulcer, you’re at risk of further ulcers developing within months or years.
Read more about preventing venous leg ulcers.
Read Also: What Foods To Avoid With Ulcerative Colitis
What Are The Causes Of A Venous Leg Ulcer
Venous leg ulcers develop because of problems with the blood circulation in your leg veins. Valves in your legs help to push blood from your legs and feet back up towards your heart. If these valves become damaged, the blood pools in the leg veins, causing pressure symptoms and skin changes.
Often an ulcer will develop after a minor injury to your leg, and because of blood circulation problems, the wound fails to heal.
Youre more at risk of developing a venous leg ulcer if you:
- are overweight
- have a history of deep vein thrombosis
- have had a previous venous leg ulcer
- are aged over 60.
What Can Cause Leg Ulcers
Venous hypertension / insufficiency the most common cause of poor healing on the lower leg is venous hypertension. This is when the veins struggle to take the blood back up the leg, so the blood can pool at the ankle creating pressure in your veins
Peripheral arterial disease another reason why our lower leg wound might not be healing is because not enough blood is getting down to our feet to heal the wound. This is then the opposite of the problem described above with veins.
Diabetes peripheral arterial disease is a known complication of diabetes, which can lead to developing a leg ulcer or diabetic foot ulcer.
Recommended Reading: Dog Skin Ulcer Home Treatment
How To Use Honey To Support Healing
Taking A Closer Look At Leg Ulcers
Leg ulcers arent something that you will wake up one day and instantly develop. They start off as a small wound that is often caused by an injury. That wound, which resulted in the breaking of the skin, is extremely slow to heal. Once the wound doesnt heal within the proper time frame, usually one to two weeks, it is no longer considered a minor injury and is then considered a leg ulcer.
Leg ulcers are classified as a chronic condition. This means if you do not seek proper medical treatment, the wound will never naturally heal and you could develop serious, potentially life-threatening health problems.
Don’t Miss: How Do You Get Rid Of Stomach Ulcers
Caring For Venous Ulcers
Venous ulcers need proper care and treatment to prevent infection and to heal. It’s important to have any venous ulcers checked right away by your healthcare provider.
Treatment may require focusing on the circulatory or vein problems that are causing the ulcers. Or it may mean removing some tissue around the wound. You may be asked to:
-
Clean the wound regularly
-
Apply a dressing to the ulcer
-
Avoid products that cause skin sensitivity
-
Wear compression stockings to prevent blood from pooling in the legs and to speed healing
-
Apply an antibacterial ointment or another topical medicine to prevent or treat an infection
-
Take oral antibiotic medicines to prevent or treat an infection
-
Have allergy testing done
Wearing a compression wrap to keep blood flowing back up to your heart can also help ulcers heal more quickly. In some cases, surgery or a skin graft is needed to close up the opening in the skin.
What Is The Treatment For Leg Ulcers
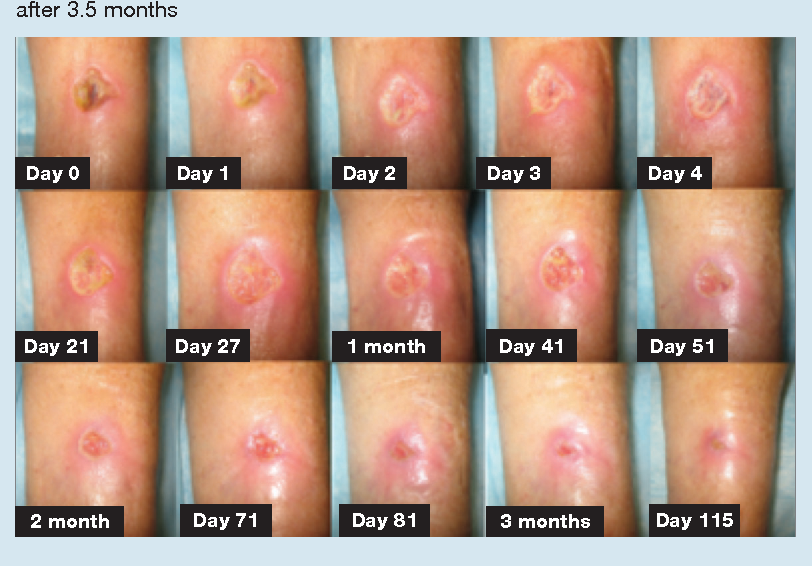
Where possible, treatment aims to reverse the factors that have caused the ulcer. As an ulcer is often the result of both arterial and venous disease, careful assessment is needed first.
Venous leg ulcer, in the absence of arterial disease, is usually treated with exercise, elevation at rest, and compression. Compression must not be used if there is significant arterial disease, as it will aggravate an inadequate blood supply. Surgery, ultrasound-guided sclerotherapy or endovascular laser treatment of superficial and perforator leg veins may also help, particularly if the deep venous system is intact. Venous-return assisted calf compression devices may be of additional benefit.
A vascular surgeon should also assess patients with arterial leg ulcers as they may require surgery to relieve the narrowing of the arteries. Revascularisation is particularly important if the ABPI is less than 0.5.
It is also very important to treat underlying diseases such as diabetes and to stop smoking.
Also Check: How Many People Have Ulcerative Colitis