Keeping Your Feet Healthy
Patients with diabetes must be diligent about wound prevention. The first step is properly managing the diabetes itself which includes maintaining a balanced diet and exercise routine, keeping blood glucose levels in the recommended range, avoiding alcohol and tobacco, and addressing any co-occurring disorder such as cardiovascular disease or obesity.
The next step is to commit to daily skin inspections, and especially your feet when sensation is impaired, Estocado said. This inspection should be thorough, and include the sole, sides and in between the toes. Even the smallest blister or scrape can escalate for diabetic patients, so call your doctor at the first discovery of any abnormality.
Wet To Dry Dressing Or Simple Saline
This dressing has a good debriding action and helps in wound bed preparation. Wet-to-dry dressings are described in the literature as a means of mechanical debridement. It is very absorptive as well as adherent and one of the cheapest dressings used throughout the world, but requires frequent dressing change based on wound severity. Dressings should be moistened before removal to minimize any chance of bleeding. A gentle cleanser will minimize wound irritation and discomfort. When treating a granulating or epithelizing wound one should soak the dressing thoroughly with normal saline for five minutes to prevent trauma and heavy bleeding.
How Do I Take Care Of My Foot And Toe Ulcers
Your healthcare provider might teach you how to care for your ulcers at home. You might be instructed to:
- Wash the affected area with mild soap.
- Keep the wound clean and dry.
- Change the bandages as directed.
- Take prescribed medications as directed.
- Drink plenty of fluids. Ask your healthcare provider how much water you should drink every day.
- Follow a healthy diet, as recommended by your healthcare provider.
- Exercise regularly, under your healthcare providers care.
- Wear appropriate shoes.
- Wear compression wraps as directed.
Don’t Miss: Do Probiotics Help Stomach Ulcers
Keep Your Wound Clean And Covered With The Right Dressings
Wounds heal best when they are clean and moist. So its important to get them clean and covered right away. If you have a new scrape or cut, a basic bandage and antibiotic cream should work just fine.
But if you have wounds that are infected, slow healing or more serious, make an appointment with a doctor to learn what the best wound care is for you. Your doctor will likely recommend different types of diabetic wound care dressings to protect the injury and promote healing.
Common types of dressings for diabetic wound care
- Foam dressings Extremely soft and absorbent, foam dressings are used for wounds that leak or ooze a lot. They also offer added cushioning which can help protect the wound against physical damage.
- Alginate dressing These types of dressings are primarily made from seaweed. They can hold up to twenty times their weight in moisture, making them a great choice for deep wounds and ones with discharge. Another advantage of alginate dressings is that they prevent the growth of new bacteria.
- Hydrogel dressings Hydrogel is a water-based gel designed to keep an area moist. If your wound is dry or covered in dead skin, your doctor may recommend a hydrogel dressing to provide moisture. This can help break down dead tissue and promote cell growth. These types of dressings usually arent used for infected wounds.
Quality Assessment Of Evidence Generated Using Direct Data
The overall quality of evidence surrounding estimates of effect using direct evidence only was assessed using GRADE . GRADE assessment focuses not on individual studies but on a body of evidence and considers issues wider than threats to interval validity, including imprecision, inconsistency, indirectness and publication bias. Problems in any category lead to the quality of the evidence being decreased . In reflecting the quality of an estimate drawn from multiple sources, GRADE aims to help the reader consider how confident we are that an effect estimate is correct . Quality of evidence can be rated as high, moderate, low or very low.
Direct and indirect data: MTC
Don’t Miss: Medications For Ulcers Over The Counter
Foot Care Tips To Prevent Diabetic Foot Ulcers
Along with controlling your blood glucose levels, these basic foot care tips can help reduce your risk of foot ulcers and improve your overall health.
1. Inspect your feet every day. You may not have the flexibility to see the bottoms of your feet, or you may not see well. If this is the case, have your spouse or a family member inspect your feet and shoes for cuts, bruises, cracks, blisters, redness, or other signs of an abnormality. Call your doctor if you notice even a small wound the earlier we can help, the better.
2. Show your doctor your feet. Remove your shoes and socks when you visit your primary care doctor. Ask them to examine your feet for nerve damage and circulation, even if they dont initiate the request.
Healing Tips For Diabetic Wound Care And Ulcers Of The Foot
Patients with diabetes can be at risk for diabetic foot ulcers, infections, and complications from those infections. Diabetic foot ulcers or wounds put patients at a higher risk of hospitalization and need for surgery or amputation. In fact, according to the CDC, there are 130,000 hospitalizations a year for amputations in those with diabetes. Up to 11.8% of those with diabetes have a wound and many may go on to need surgery. This means that wound care for diabetic foot ulcers as well as prevention is of the utmost importance.
As physicians, we have to use our resources and work with patients in order to heal diabetic foot wounds to prevent such complications. If a patient also has numbness in their feet, they may not feel a foot wound developing. Diabetic foot sores that start from a small scrap or cut can unknowingly form into a deep ulcer. Checking your feet and keeping your blood sugar
Whether you have diabetes or are caring for a loved one requiring foot diabetic wound treatment, Certified Foot and Ankle Specialists can effectively help your wound heal and prevent further complications. Here we will discuss diabetic foot care and how to minimize the traumatic consequences of ulcers.
How do we care for diabetic foot wounds and how does one clean a diabetic foot wound?
For proper wound care, clean the wound with saline, apply a topical gel or antibiotic ointment medication to the wound once a day, as recommended by your doctor.
Preventing diabetic wounds
Also Check: Foods To Eat To Help Ulcers
Can Diabetic Amputations Be Prevented
Absolutely. In fact, they are highly preventable. The best way to prevent an amputation is to prevent the diabetic foot ulcer from forming. There are steps that can be done at home, such as performing regular foot exams, engaging in daily movement to keep blood flowing, and wearing proper footwear.
Additionally, diabetic foot ulcers can be prevented by using thermometry. Thermometry will measure the temperature of the foot, recognizing changes that signal inflammation. When intervention occurs earlier on, most diabetic foot ulcers can be prevented â with the hope that amputation is not necessary.
Categories:
How To Help Prevent Diabetic Foot Ulcers:
- Inspect your feet daily, looking for ingrown, thick or odd colored toenails and toes that curl
- Use a mirror to look for any open areas in your skin and make sure to look between your toes
- Ask a family member or friend to help if you cannot thoroughly check your own feet
- Never cut corns or calluses yourself
- Never use store bought corn or callous removers, foot pads or arch supports
- Wash your feet daily, dry between your toes, and do not use powder
- If your feet become really dry, moisturize them but take care not to get the cream between your toes
- Dont use garters or elastics to hold up your stockings
- Dont use panty girdles that are tight around your legs
- Do not walk barefoot indoors or outdoors
Avoid getting your feet too hot or too cold:
- Dont walk barefoot on hot sand or pavement in summer
- Put sunscreen on your feet when in the hot sun
- Check the temperature of bath water with your hand before stepping in
- Do not use hot water bottles or heating pads to warm cold feet and wear loose socks at night in bed if your feet are cold
- Wear absorbent socks and change them during the day when needed
- Do not wear socks with holes in them
- Beware of car heaters on long trips
Recommended Reading: Best Natural Remedies For Stomach Ulcers
Take Pressure Off The Area
If a wound continues to reopen or experience damage, it wont heal quickly and may get much worse. So avoid putting stress, pressure and weight on wounds.
This can be tricky for some wounds like ones on your feet. If you need help, talk to your doctor about ways to protect your wounds while maintaining mobility. Special shoes and customized foot padding are common options.
How Can I Reduce My Risk Of Foot And Toe Ulcers
There are several things you can do to help reduce your risk of getting foot and toe ulcers. Sometimes, adopting these habits can even stop them from coming back. Try to:
- Manage your diabetes. If you have diabetes you should wear appropriate footwear and never walk barefoot.
- Examine your legs as well as the tops and bottoms of your feet and the areas between your toes every day. Look for any blisters, cuts, cracks, scratches or other sores. Also check for redness, increased warmth, ingrown toenails, corns and calluses. Use a mirror to view your leg or foot if necessary. If its difficult to see, ask a family member to look at the area for you. See a healthcare provider immediately if you notice any problems.
- Talk to your healthcare provider about ways you can stop smoking.
- Manage your blood pressure.
- Control your cholesterol and triglyceride levels by changing your diet. Limit salt in your diet.
- Care for your toenails frequently. Cut your toenails after bathing, when they are soft. Cut toenails straight across and smooth with a nail file. Take care of ingrown toenails.
- Exercise.
- Wear appropriate shoes and socks. Talk to your podiatrist about what you need.
Don’t Miss: Ulcerative Colitis Biologics Side Effects
How Are Foot And Toe Ulcers Treated
The treatment of all ulcers begins with careful skin and foot care. Inspecting your skin is very important, especially for people with diabetes. Detecting and treating foot and toe sores early can help you prevent infection and keep the sore from getting worse.
The goal of treating a foot or toe ulcer is to heal your wound and relieve any pain. Your treatment plan will be individualized based on what medical condition is causing your ulcers. If you cant correct the cause of your ulcer, its likely to come back after treatment.
There are both surgical and nonsurgical treatments for foot and toe ulcers. For early-stage foot and toe ulcers, nonsurgical treatments might work. More advanced ulcers especially ones that are infected might require surgery.
Nonsurgical treatments include:
- Topical wound care.
- Reconstructive surgery using skin grafts.
How Can I Tell If Im Getting An Ulcer On My Foot Or Toe
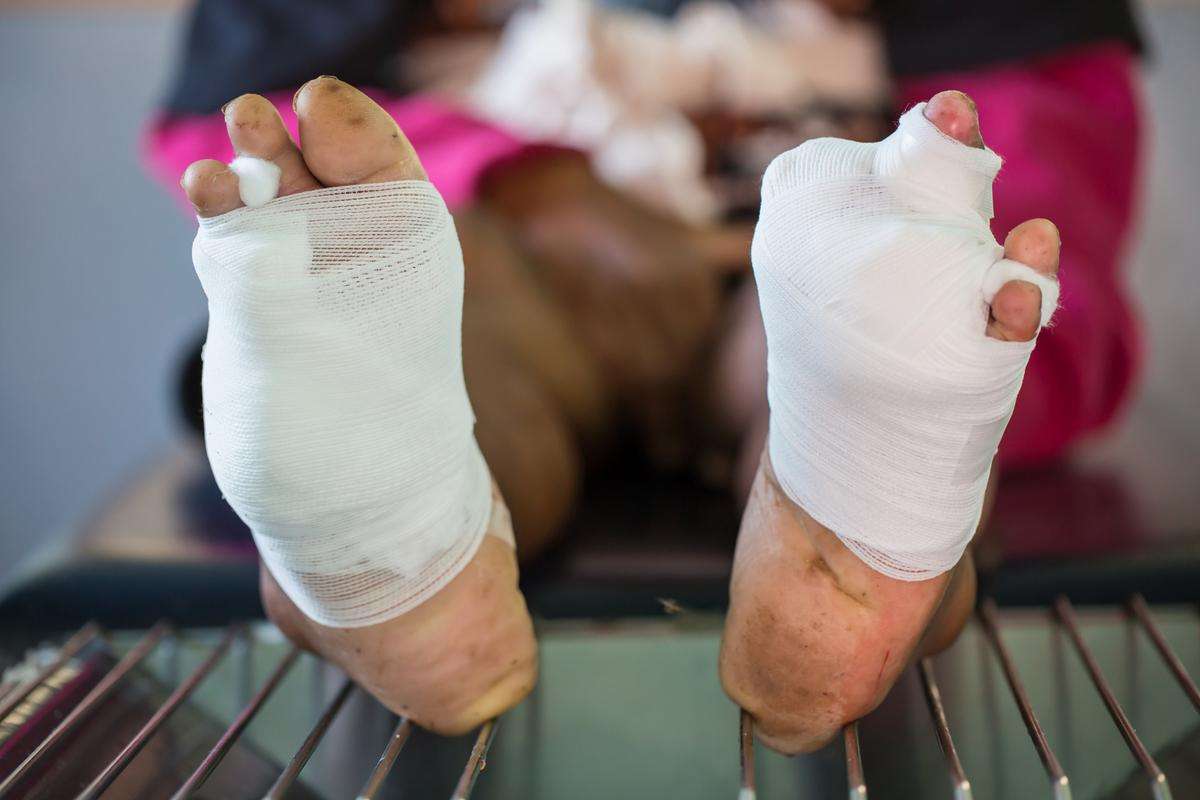
When an ulcer is starting to develop on your foot or toe, you might notice changes in your skin like:
- Dry skin.
- Redness.
- Rashes.
As the ulcer gets worse, it can get wider, and longer and deeper sometimes down to the bone. In advanced stages you might see:
- A callus.
- A halo around the center of the wound that feels harder than the skin around it.
- Drainage , which is a sign that you might have an infection.
- A brown discoloration.
Don’t Miss: What Do You Take For An Ulcer
Effectively Dressing Diabetic Foot Ulcers
Creating an optimal environment is essential to ensuring rapid healing and preventing complications. However, it can be challenging to effectively dress wounds located on the foot, particularly in cases of deformity or disease such as Charcot foot. To dress these wounds appropriately, health care professionals must often use non-traditional methods. Using best practices and more effective medical adhesive products can allow dressings to stay secure longer, even in unusual locations.2,4
Infection Control Infection in DFUs can lead to inflammation, delayed wound healing, gangrene, and amputation. To reduce the risk of infection and improve outcomes, health care professionals can use dressings that control bacterial load in the wound. Antibacterial agents such metronidazole gel and sisomicin can help control pathogens in the wound area.5
Wound Protection Because DFUs are located on the foot, they are more susceptible to additional injury than wounds in a less exposed location. This makes it important to choose a dressing that provides some amount of mechanical protection. Dressings that are secure and substantial can protect the wound area from additional damage. Using offloading techniques such as total contact casts and removable cast footwear can also help provide support the foot and prevent repetitive trauma.5
When You Need More Treatment
If your wound doesnât heal in about a month or becomes an infection that spreads to the bone, you may need other treatments. These can include surgery and hyperbolic oxygen therapy, which involves breathing pure oxygen in a special room in order to help your body heal.
If your ulcer develops gangrene and your tissue dies, your doctor may have to amputate that area of your body.
Also Check: Urgent Care For Stomach Ulcer
Could You Have Nerve Damage
Anyone with diabetes can develop nerve damage, but these factors increase your risk:
- Blood sugar levels that are hard to manage
- Having diabetes for a long time, especially if your blood sugar is often higher than your target levels
- Being overweight
- Having high cholesterol
Nerve damage, along with poor blood flowanother diabetes complicationputs you at risk for developing a foot ulcer that could get infected and not heal well. If an infection doesnt get better with treatment, your toe, foot, or part of your leg may need to be amputated to prevent the infection from spreading and to save your life.
When you check your feet every day, you can catch problems early and get them treated right away. Early treatment greatly reduces your risk of amputation.
What Causes A Diabetic Foot Ulcer
Diabetic foot ulcers can be caused from a number of factors and often from a combination of them. Here are some of the most common factors that cause diabetic foot ulcers: poor blood circulation or vascular disease, high blood sugar or hyperglycemia, diabetic neuropathy , foot deformities, irritations to the foot, previous woot wounds, poor hygiene, and poorly fitting shoes.
Any of these factors can lead to inflammation of the foot, which precedes a diabetic foot ulcer. Before the wound forms, the area may rise in temperature signaling inflammation. This change is too subtle for patients to notice on their own. Many donât realize the foot ulcer is coming until it begins to show physical symptoms like blackening of the surrounding flesh, numbness, and abscesses.
Recommended Reading: Best Anti Diarrhea Medicine For Ulcerative Colitis
How Does A Diabetic Foot Ulcer Lead To A Diabetic Amputation
The worst scenario for a diabetic foot ulcer is that it progresses past the point of treatment and requires a lower extremity amputation. This can happen due to infection of the wound, or simply because time has passed and the ulcer wasnât identified early on, due to complex factors like neuropathy or vascular disease. If there is nerve damage, a wound like a foot ulcer can go unnoticed because it wonât cause any pain.
Itâs also difficult for many people to examine the bottom of their feet regularly. Some patients may have caretakers that can perform regular foot exams, but many do not.
In addition, many patients have diabetic retinopathy. This condition leads to vision impairment, making it even harder to see any changes to the foot. Even if foot exams are done regularly, it can be hard to determine if a foot ulcer is forming.
Diabetic amputation of lower extremities should be a last resort, only taken once the foot ulcer has progressed significantly. If the tissue is damaged beyond repair, it might be the best option for the patient. Their doctor will also consider quality of life, risk of additional foot complications, and other criteria to make their decision.
How The Intervention Might Work
Animal experiments conducted over 40 years ago suggested that an acute wound heals more quickly when its surface is kept moist, rather than left to dry and scab . A moist environment is thought to provide optimal conditions for the cells involved in the healing process, as well as allowing autolytic debridement , which is thought to be an important part of the healing pathway . The desire to maintain a moist wound environment is a key driver for the use of wound dressings. Different wound dressings vary in their level of absorbency, so that a very wet wound can be treated with an absorbent dressing to draw excess moisture away from the wound to avoid skin maceration, whilst a drier wound can be treated with a more occlusive dressing to maintain a moist environment. Alginate dressings contain sodium, or sodium and calcium, salts of alginic acid. These alginate salts are highly hydrophilic and can absorb large volumes of wound exudate.
Recommended Reading: What Does An Ulcer Feel Like In Your Stomach
What The Start Of A Foot Ulcer Looks Like
It can be difficult for a person with diabetes to realize that they have a diabetic foot ulcer until it has already progressed. The reason for this is that many people with diabetes do not have feeling in their extremities due to poor circulation and peripheral neuropathy, so they may not feel the pain of a cut or wound.
One of the first signs of a diabetic foot ulcer that a person with diabetes may notice is drainage from the wound that stains their socks. Irritation, swelling, or an unpleasant odor may also be some of the first signs that a diabetic foot ulcer is present.
In more severe cases, a person may notice discoloration around the wound , or the skin around the wound may be callused or painful to the touch.
If these symptoms are present, immediately seek medical care, ideally with a podiatrist, to prevent the wound from getting any worse and begin treatment as needed.