Do Ulcerative Colitis Causes And Crohns Disease Causes Overlap
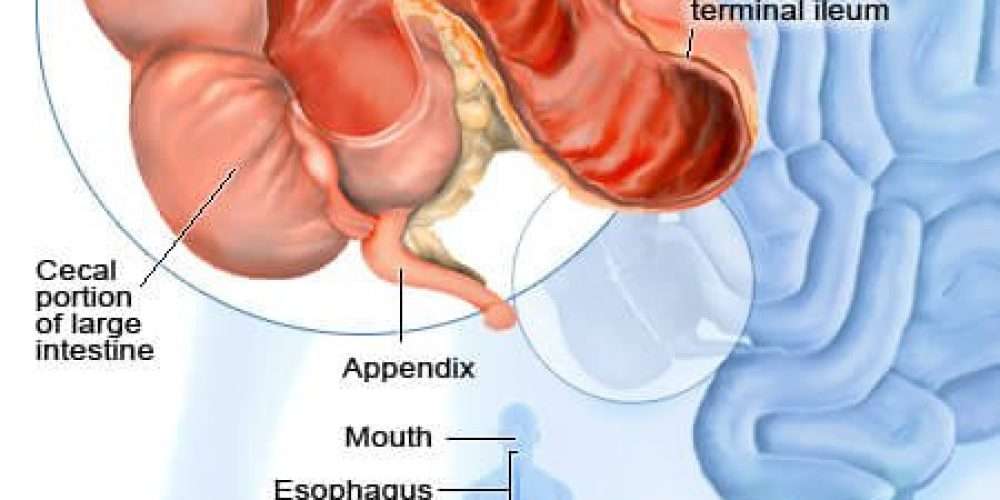
In Crohns disease, areas of your digestive tract become irritated and inflamed. This can lead to symptoms like cramping, diarrhea, and unintentional weight loss, which heavily overlap with those of ulcerative colitis. While ulcerative colitis only affects your colon, Crohns disease can impact any part of your digestive tract. The most commonly affected areas are the last part of your small intestine, called the ileum, and the first part of your colon.
Much like ulcerative colitis, the exact causes of Crohns disease remain unclear. Similar factors are believed to play a role, including a dysfunctional immune response and genetics.
According to the NIDDK, the risk factors for Crohns disease include family history, smoking cigarettes, and being between the ages of 20 and 29. Its also possible that eating a high-fat diet or using medications like NSAIDs, antibiotics, or birth control pills may also slightly increase the risk of Crohns disease.
Symptoms Of Colitis In Dogs
The most prominent symptom of colitis in dogs is diarrhea. Other canine colitis symptoms include:
- Difficulty and straining while defecating
- Pain and inflammation in the abdomen
- A sense of sudden urgency
- Increased defecation with small volume
- Fresh blood present in stool
- Mucus or slime present in stool
- Dehydration from loss of fluids
- Irregular eating habits
- Lethargy
Are There Different Kinds Of Canine Colitis
Colitis in dogs comes in two types. It can either be acute or chronic.
Acute colitis occurs suddenly. It is a one-off condition that can last a few days and afterwards, your dog will return to normal health. It is caused by some kind of short-term external trigger such as an undiagnosed infection, parasites, or by your dog eating something they shouldnt.
Read Also: Natural Ways To Heal Esophageal Ulcers
Is Ulcerative Colitis An Autoimmune Disease
Experts consider ulcerative colitis to be an autoimmune disease. An overactive immune response causes the immune system to attack healthy tissue in the gut, leading to inflammation of the large intestine.
Some medications people with ulcerative colitis take also compromise the immune system. However, this does not necessarily mean a person with ulcerative colitis has a higher risk of infection, including with the virus that causes COVID-19.
In this article, we look at the link between the immune system and ulcerative colitis, whether ulcerative colitis increases the risk of infection, and how treatments work to manage ulcerative colitis.
According to the Benaroya Research Institute, UC is an autoimmune disease.
An autoimmune disease happens when a persons immune system becomes overactive and attacks their healthy tissue.
In UC, the immune system attacks the intestines, causing inflammation in the large intestine.
Does Colitis Go Away
Acute colitis that is caused by a temporary infection, food intolerance or radiation exposure typically goes away by itself. Infections take about a week, while radiation colitis takes a few months. Some types of infection may need to be treated with antibiotics to go away, especially parasite infections. Allergic colitis goes away when the substance your child was allergic to has cleared from their body.
Colitis that is an acute reaction to a chronic condition needs treatment to go away. Ischemic colitis resulting from intestinal ischemic syndrome wont go away until blood flow is restored to your colon. Diversion colitis in people with colostomies wont go away until the colostomy is reversed and the full use of your colon is restored . In some people, these solutions arent possible.
Chronic colitis that is caused by inflammatory bowel disease is a lifelong condition. It wont go away forever, but it can go away for a while. This is called remission. Treatment for IBD is focused on improving your symptoms and making remission last as long as possible. This is also true if your colitis is caused by another condition that cant be cured. In some cases, surgery can make it go away.
Read Also: How Do You Get Ulcers In Your Colon
Allergic Colitis In Infants
Allergic colitis is a condition that can occur in some infants who are breastfeeding. The only symptom thats usually found is blood in the stool.
This condition may result from a food allergy, but the cause is not well understood. Tests such as endoscopy arent usually done but the diagnosis is based on the occurrence of bloody stools.
The bloody stools normally resolve on their own, but the possibility of a food allergy should be looked into. This includes removing foods from the breastfeeding parents diet. Usually this begins with removing dairy products for several weeks and seeing if that makes any difference.
Other foods that commonly cause allergies might also be stopped if the bloody stools dont improve. In some cases, a special formula might be recommended for feeding.
Does Ulcerative Colitis Make You Immunocompromised
Ulcerative colitis doesnt make you immunocompromised. Some of the medicines that treat it may change the way your immune system responds. This change is different for each medication. Some of these changes may increase the risk of certain infections or other issues. A discussion with your health care team before starting a medication is the best way to understand these risks and ways to prevent them.
Don’t Miss: How To Treat Peptic Ulcer Disease
How Can I Care For Myself
- Drink liquids to help prevent dehydration. Ask your healthcare provider how much liquid to drink each day and which liquids are best for you. You may need to drink an oral rehydration solution . An ORS contains a balance of water, salt, and sugar to replace body fluids lost during diarrhea. Ask what kind of ORS to use, how much to drink, and where to get it.
- Do not take medicine to stop your diarrhea. These medicines may make your symptoms last longer.
The Influence Of Sex: Boys Develop Crohn’s Disease More Easily Than Girls While Men Develop Ulcerative Colitis And Women Develop Crohn’s Disease When Infected With Map
It is commonly known that infant males are more prone to infectious diseases than infant females, probably due to weaker immune systems . This weaker immune response might cause boys to develop Crohn’s disease more often than ulcerative colitis when infected with MAP, because they probably have a weaker immune response to the MAP organism. It has been postulated that Crohn’s disease is not an autoimmune disease, a disease of excessive or over reactive immunity, but an immune deficiency disease . Individuals with Crohn’s disease have a less active response to the MAP organism, in contrast with individuals with ulcerative colitis, who have a more active response, as proposed above.
In contrast to children, adult females seem slightly but consistently more likely to develop Crohn’s disease and adult males to develop ulcerative colitis when infected with MAP. While purely speculative, this difference might be due to the differing effects of testosterone versus estrogen on blood and lymphatic vessels, to the greater effects of smoking on females than males , or to the increase in oral contraceptive use, with its known vascular complications .
Read Also: What Are The First Signs Of A Stomach Ulcer
What Are The Clinical Signs Of Colitis
Most dog owners report seeing frequent, small volumes of semi-formed to liquid feces. Many dogs will exhibit straining during and after defecation, and small amounts of bright red blood will often be passed near the end of defecation. Mucus or fat is seen in many cases of chronic colitis. Most dogs with colitis will exhibit a sense of urgency and need to defecate frequently. Vomiting occurs in less than a third of the cases of colitis or large bowel diarrhea. Weight loss is rare.
What Are The Causes Of Colitis
As colitis can either be acute or chronic, it can be caused by a sudden trigger or an existing long-term condition. Diagnosing colitis is best done by a trained veterinary professional.
Some of the common causes of colitis in dogs include:
- Eating something disagreeable
- Pre-existing health conditions
You May Like: How Do You Diagnose A Stomach Ulcer
Who Diagnoses Ulcerative Colitis
If you have symptoms of ulcerative colitis, your regular healthcare provider will probably refer you to a specialist. A gastroenterologist a doctor who specializes in the digestive system should oversee the care for adults. For young patients, a pediatric gastroenterologist who specializes in children should manage the care.
What Causes Ulcerative Colitis Flareups

When youre in remission from ulcerative colitis, youll want to do everything you can to prevent a flareup. Things that may cause a flareup include:
- Emotional stress: Get at least seven hours of sleep a night, exercise regularly and find healthy ways to relieve stress, such as meditation.
- NSAID use: For pain relief or a fever, use acetaminophen instead of NSAIDs like Motrin® and Advil®.
- Antibiotics: Let your healthcare provider know if antibiotics trigger your symptoms.
Don’t Miss: Crohn’s Disease And Ulcerative Colitis Differences
Whats The Difference Between Ulcerative Colitis And Colitis
Colitis refers to inflammation of the inner lining of the colon. Colitis causes symptoms such as abdominal pain and cramping, bloating, and diarrhea.
An inflamed colon can be caused by several conditions. UC is one possible cause. Other possible causes of colitis include:
- infection
- Crohns disease
- an allergic reaction
To diagnose the cause of colitis, a doctor will order a series of tests. These tests will help them understand what other symptoms youre experience and rule out conditions based on what youre not experiencing.
Treatment for colitis will depend on the underlying cause and other symptoms you have.
General Recommendations: Healthy Practices
There are preventive actions you can take to protect yourself from exposure to the virus and prevent the spread of the disease. The CDC recommends the following ways to limit your risk of infection:
- Avoid having close contact with people who are sick.
- Do not touch your nose, eyes, and mouth if you have not washed your hands.
- Wash your hands with soap and water for at least 20 seconds. To ensure you wash for the appropriate amount of time, sing Mary Had a Little Lamb or another short song two to three times to reach 20 full seconds.
- If soap and water are not available to you, use a hand sanitizer that contains at least 60% alcohol. Check the label to confirm the amount of alcohol.
-
Many communities have implemented social distancing measures including canceling public events and encouraging remote work. Please follow the specific guidance being issued by your local health department.
Here are some other actions to take if you are feeling ill or you think you may have been exposed COVID-19:
- Stay home if you are feeling sick
- Cover your cough or sneeze with a tissue, and throw it in the trash
- Clean and disinfect frequently touched objects
- Contact your doctor
- If you are feeling unwell and are not at high-risk , monitor symptoms, and contact your doctors via phone or telemedicine.
- If you need an in-person visit at the office, ER or Urgent Care, please call ahead. This will allow the office/ER to take measure to prevent any possible spread of infection.
Don’t Miss: Offloading The Diabetic Foot For Ulcer Prevention And Healing
How Does Colitis Spread
- Contagious types of colitis are spread from person-to-person, but non-contagious types of colitis are not.
- Contagious types of colitis are usually spread by direct person-to-person contact, usually by the hands , but others may be spread by contaminated food or fluids, and for some types, indirectly by contact with contaminated items like clothing, utensils, or toothbrushes.
How Does Ulcerative Colitis Affect The Body
To understand the possible ulcerative colitis causes, its important to first understand a little bit about the structure of your colon, which is your large bowel or large intestine.
Mucus coats the colons walls to not only serve as a lubricant for stool moving through your bowels but to also help keep germs and harmful substances away from the cell layer that lines the colon. The scientific name for this layer of cells is the epithelium. The epithelium itself is an important barrier to potentially harmful substances and is fortified by tight connections between each cell. Located below the epithelium is an area called the lamina propria, which is made up of connective tissue and is home to several types of immune cells, according to a 2016 study published in the journal Inflammatory Bowel Diseases.1
In ulcerative colitis, the barriers provided by mucus and the epithelium are dysfunctional. This means that the epithelial cells and nearby immune cells are increasingly exposed to bacteria and potentially other substances, like yeast, that are found in the colon.
Because the immune response is abnormal, this can have several damaging effects in the colon and throughout the body, such as an expanded presence of immune cells that attack the lining of the colon, increased inflammation, and further disruption of the colons lining, Nicole Fay, Ph.D., an immunotherapeutics researcher and a director of pharmacology at Nutcracker Therapeutics, tells SELF.
You May Like: Where Are Stomach Ulcers Located
How Is Crohn’s Disease Treated
Initial treatment is almost always with medication. There is no “cure” for Crohn’s disease, but medical therapy with one or more drugs provides a means to treat early Crohn’s disease and relieve its symptoms. The most common drugs prescribed are corticosteroids, such as prednisone and methylprednisolone, and various anti-inflammatory agents.
Other drugs occasionally used include 6-mercaptopurine and azathioprine, which are immunosuppressive. Metronidazole, an antibiotic with immune system effects, is frequently helpful in patients with anal disease.In more advanced or complicated cases of Crohn’s disease, surgery may be recommended. Emergency surgery is sometimes necessary when complications, such as a perforation of the intestine, obstruction of the bowel, or significant bleeding occur with Crohn’s disease. Other less urgent indications for surgery may include abscess formation, fistulas , severe anal disease or persistence of the disease despite appropriate drug treatment.
Not all patients with these or other complications require surgery. This decision is best reached through consultation with your gastroenterologist and your colon and rectal surgeon.
Smoking Increases The Risk Of Both Ulcerative Colitis And Crohn’s Disease But Nicotine Has Different Effects On Colonic Versus Small Bowel Inflammation
There are two commonly accepted beliefs about the relationship between smoking and Crohn’s disease and ulcerative colitis: smoking increases the risk of Crohn’s disease but protects an individual from developing ulcerative colitis, and smoking increases the severity of Crohn’s disease, but decreases the severity of ulcerative colitis. If ulcerative colitis and Crohn’s disease are both caused by MAP, how can these apparently dichotomous effects be explained? An excellent review article by Lakatos and colleagues helps elucidate the reasons for the different effects of smoking on these diseases.
First, in children, smoking increases the risk of developing both ulcerative colitis and Crohn’s disease. In a study of inflammatory bowel disease in Kentucky children , children who started smoking before 10 years of age were 7 times more likely to develop ulcerative colitis than nonsmokers, and over 3 times more likely to develop Crohn’s disease than nonsmokers. If they started smoking before age 15, they were over three times more likely to develop both diseases. Smoking increased the risk of developing both Crohn’s disease and ulcerative colitis, and in this one study increased the risk of ulcerative colitis more than it increased the risk of Crohn’s disease .
You May Like: How Effective Is Humira For Ulcerative Colitis
How To Prevent Colitis In Dogs
One of the best ways to prevent colitis in dogs is to be careful about what they eat. Keep your pet away from the trash and unfamiliar food items, including human food. Restricting their contact with potentially sick dogs in public places can also prevent your pet from getting sick. It is also helpful to teach your dog the leave it command or keep him on the leash to stop him from scavenging while out on walks.
In addition to these preventatives related to food, you should also make sure to keep your four-legged friend free of parasites by giving their scheduled de-worming medications and ensuring that he or she is current on all recommended vaccines.
Which Specific Infectious Microorganism Is Found In Patients With Crohn’s Disease And Ulcerative Colitis Map
MAP is an organism found in animal feces. It infects and causes clinical disease, called Johne’s disease, in a wide variety of animal species. Several meta-analyses and reviews of the literature have concluded that the MAP organism is consistently associated with Crohn’s disease :
…the MAP Crohn’s disease phenomenon has fulfilled at least four of the six epidemiological causal criteria outlined by Hill…the current epidemiological evidence strongly supports the conjecture that Crohn’s disease is caused by MAP .
There is an association between MAP and , across many sites, by many investigators, and controlling for a number of factors .
…our meta-analysis showed an association between MAP and Crohn’s disease that is robust and specific .
The studies attempting to identify the MAP organism in Crohn’s disease by a variety of techniques have often used ulcerative colitis as the “negative” control, under the assumption that MAP may cause Crohn’s disease, but not ulcerative colitis . When MAP is identified in both Crohn’s disease and ulcerative colitis, researchers conclude that MAP causes neither disease. If, however, the current body of research is looked at from the point of view that MAP might cause ulcerative colitis as well as Crohn’s disease, there is evidence to support this alternative position.
Read Also: Best Way To Treat Ulcers In Horses
Ulcerative Colitis Causes And Risk Factors Explained
Medically reviewed by Kerri Glassner, DO
If you find yourself shaking your fists at the sky, demanding to know the truth behind the causes of ulcerative colitis , youve probably had your fair share of less-than-pleasant bathroom time.
Ulcerative colitis is a type of inflammatory bowel disease , and its more common than you might think. The National Institute of Diabetes and Digestive and Kidney Diseases estimates that between 600,000 and 900,000 people in the United States live with this chronic condition, but its likely even more than that.
When you have ulcerative colitis, an abnormal immune response leads to an increase in inflammation in the colon, causing ulcers to appear on its inner lining. This ultimately leads to symptoms like bloody diarrhea, abdominal cramping, and the urge to go .
The good news is, with treatment, people diagnosed with ulcerative colitis often have periods of remission, where symptoms go away for a while. Remission can last for weeks or even for several years. If and when ulcerative colitis symptoms return, its called an ulcerative colitis flare-up or relapse.