What Is Ulcerative Colitis Skin Rash
Inflammatory Bowel Disease
IBD is an inflammation of the intestines , there are spectra of diseases that may fall into this broad category, but the main two are Ulcerative Colitis and Crohns Disease.
It behaves as the main umbrella term, Although an exact etiology is unknown, it is internationally believed to be caused by the abnormal activation of the immune system and is genetic . However, Caucasians and individuals of eastern European Jewish descent are more likely to develop ulcerative colitis .
Crohns Disease
Ulcerative Colitis
Ulcerative Colitis mainly affects the colon and rectum with continuous lesions and only affects the guts inner lining . The Col in Colitis refers to the colon, and -itis is defined as inflammation. Pretty cool, right?
Another interesting element is that the word ulcerative explains what is happening due to this inflammation. People with Ulcerative Colitis have inflammation caused by such ulcers that destroy the lining of the colon wall, leading to diarrhea and bleeding .
Irritable Bowel Syndrome and Ulcerative Colitis
IBD and IBS get confused however, understanding the difference is important- despite having many similarities. However, the cause of IBS is believed to be dysfunction of the nerves and muscles of the intestines.
What are the First Signs of Ulcerative Colitis Symptoms?
Ulcerative Colitis Review
Other Ulcerative Colitis Symptoms
Ulcerative Colitis Diagnosis
What Is Erythema Nodosum
Erythema nodosum, or EN, is a skin condition that shows as a lumpy red rash, usually on the lower legs. It is sometimes caused by an illness, but about half the time there is no reason for it.
While the rash can be painful, it is harmless in itself. It usually settles down without specific treatment over several weeks.
Skin Joint Or Eye Problems
When you have UC, the lining of your large intestine gets inflamed and sets off your symptoms. For some people, this inflammation also shows up in other body parts during a flare. Experts arent sure why.
You could have symptoms like:
Let your doctor know whenever you get new UC symptoms. That way, they can change your treatment plan if needed.
Recommended Reading: Over The Counter Remedies For Ulcers
Recommended Reading: Best Natural Cure For Ulcerative Colitis
Why Do Skin Rashes Appear During Flare
The inflammation in the body that causes UC can also affect the skin. This can lead to swollen and painful skin rashes.
According to a 2015 study, skin problems affect up to of people with IBD, which includes people with UC.
The medication that a person might take to control their UC symptoms may also cause skin problems.
People with UC often experience skin problems during flare-ups, so the best way to manage skin conditions related to UC is to manage UC itself.
A doctor can help a person with UC find the best methods for their symptoms and lifestyle.
When flare-ups occur, the following may help to reduce skin problems:
- taking corticosteroids to reduce inflammation
- eating a well-balanced diet to promote skin health
- keeping the affected skin clean to reduce infection risk
- covering the affected area with bandages
- taking over-the-counter pain relievers
Ulcerative Colitis Rash And Skin Irritation
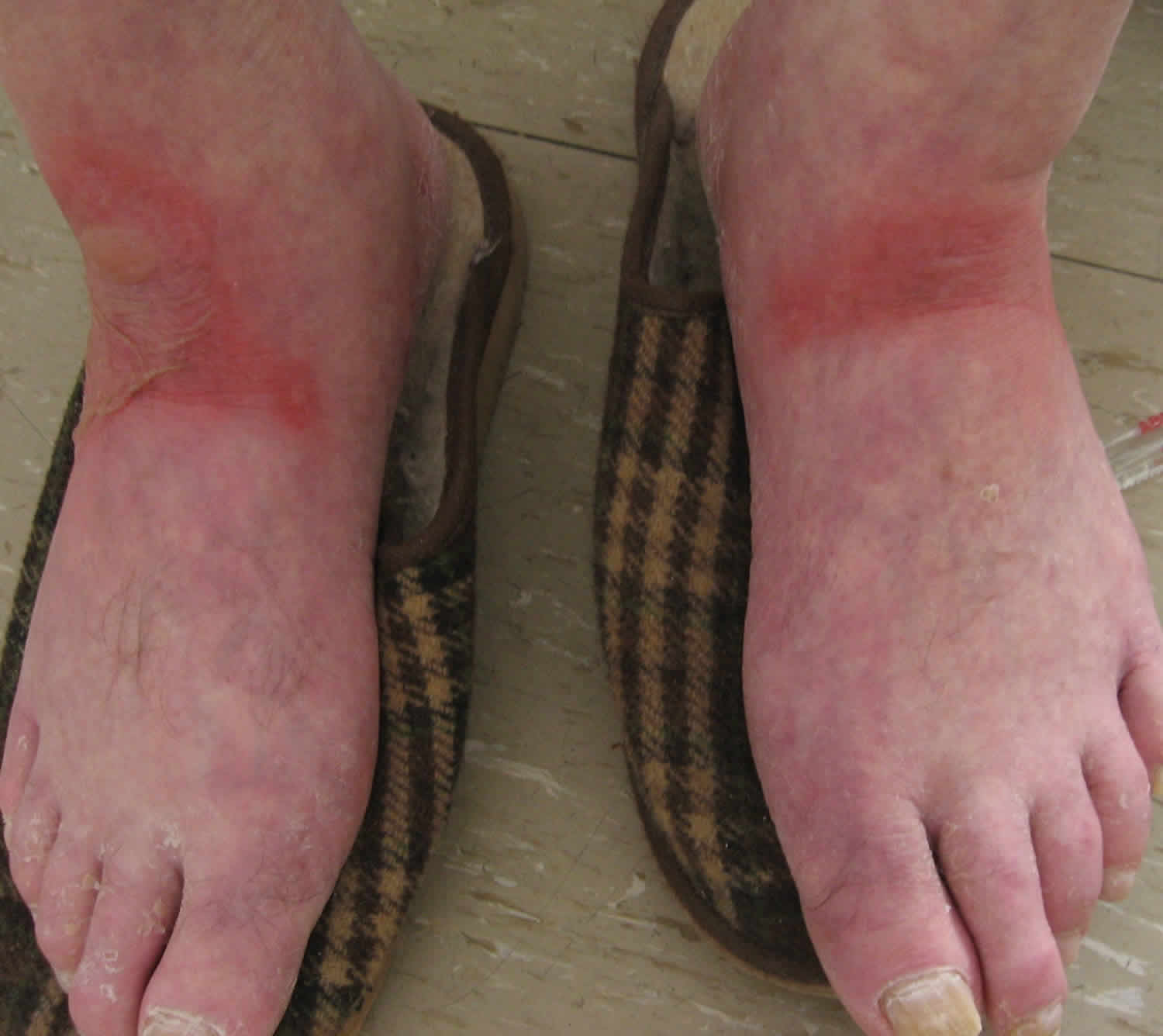
Ulcerative Colitis is marked by inflammation that presents through several gastrointestinal symptoms, as well as in other areas of the body including the skin, joints, mouth, and eyes. Swollen and painful areas of skin are common and affect up to 15 percent of individuals with UC. In general, skin irritation and rashes will get worse during a flare and resolve during periods of remission. These rashes oftentimes fluctuate in-line with the inflammation throughout your entire body.
While most skin irritation and rashes are caused by Ulcerative Colitis inflammation, general UC symptoms do not always cause the irritation and rashes. Ulcerative Colitis medications may cause skin issues as a side effect. Additionally, lack of nutrients may present as skin irregularities. It is important to work with your medical team to determine the cause of your skin problems.
Also Check: Ulcer Of Esophagus Without Bleeding
Symptoms Of Ulcerative Colitis
The main symptoms of ulcerative colitis are:
- recurring diarrhoea, which may contain blood, mucus or pus
- needing to empty your bowels frequently
You may also experience extreme tiredness , loss of appetite and weight loss.
The severity of the symptoms varies, depending on how much of the rectum and colon is inflamed and how severe the inflammation is.
For some people, the condition has a significant impact on their everyday lives.
Skin Disorders Associated With Ulcerative Colitis
Below are six skin conditions that people with ulcerative colitis can be at increased risk of developing.
1. Erythema Nodosum The most common skin condition associated with ulcerative colitis, erythema nodosum is a rash that consists of painful, raised bumps and is usually found on the legs.
It tends to develop when ulcerative colitis is active, notes Dr. Hagan. You may also run a fever, have joint pain, and generally feel ill, according to Medline Plus.
Treatment options include pain-relieving medication, steroids , and a potassium iodide solution to clear up the bumps.
A cool compress can also help alleviate discomfort and reduce inflammation, says Kally Papantoniou, MD, a dermatologist in private practice in Melville, New York. She also recommends elevating your legs to help lessen swelling and tenderness.
Compression stockings can also be helpful, but have your doctor evaluate you for vascular disease before using them, cautions Dr. Papantoniou.
Symptoms of erythema nodosum usually go away within three to six weeks, but the residual bruises may last for months. In about 20 percent of cases, the rash comes back.
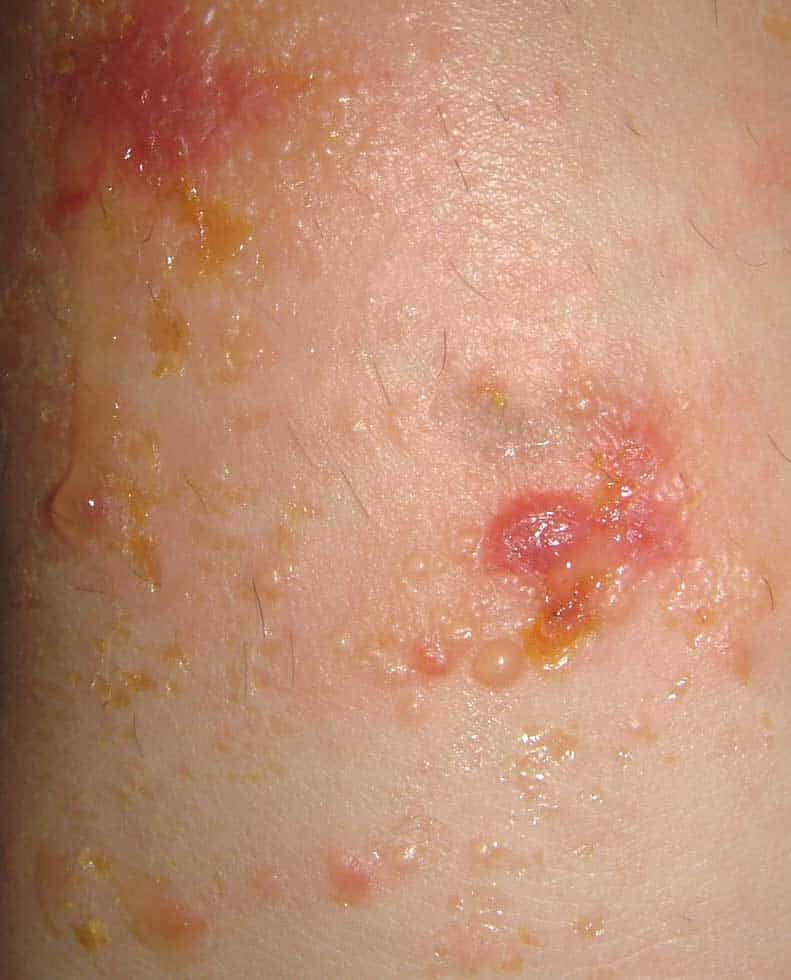
2. Pyoderma Gangrenosum This is a severe and debilitating condition that starts as a rash made of red or purple bumps or blisters, and then quickly spreads. These blisters eventually join together and form deep open sores , according to the Crohn’s& Colitis Foundation.
Pyostomatitis vegetans is the same condition, but it occurs in the mouth, Brieva says.
Read Also: Is Oatmeal Ok To Eat With Ulcerative Colitis
Skin Rashes Linked To Ulcerative Colitis
Inflammatory bowel diseases, including Crohns disease and ulcerative colitis , are chronic conditions that affect the digestive tract. While inflammation is the most common symptom associated with these diseases, some patients with Crohns and UC also experience skin issues, including painful skin rashes. In fact, over 15% of all individuals with different types of inflammatory bowel diseases are also affected by skin issues. While some skin rashes may be associated with Crohns or UC-related inflammation within the body, others may derive from the medications used to treat UC. 10 of the most common skin rashes linked to UC include the following:
To view this video please enable JavaScript, and consider upgrading to a web browser thatsupports HTML5 video
How Does Ibd Affect Other Parts Of The Body
IBD can also cause problems outside the gut. Some people with IBD develop conditions affecting the joints, eyes or skin. These can be known as extraintestinal manifestations and often occur during active disease, but they can develop before any signs of bowel disease or during times of remission. Many of these are not very common.
JOINTS
Inflammation of the joints, often known as arthritis, is a common complication of IBD.
It is most common in those with Crohns Colitis and also affects about one out of 10 people with UC.
The inflammation usually affects the large joints of the arms and legs, including the elbows, wrists, knees and ankles. Fluid collects in the joint space, causing painful swelling, although pain may occur without obvious swelling. Symptoms usually improve with treatment of intestinal symptoms, and there is generally no lasting damage to the joints. A few people develop swelling and pain in the smaller joints of the hands or feet. This may be longer lasting and persist even when the IBD is in remission.
Sometimes, the joints in the spine and pelvis become inflamed a condition called ankylosing spondylitis . This can flare-up independently of IBD. It often causes pain over the sacroiliac joints, on either side of the lower part of the spine. Stiffness and pain in the spine itself may eventually lead to loss of flexibility.
SKIN
MOUTH
EYES
BONES
KIDNEYS
LIVER
Some complications are related to the liver and its function.
BLOOD CIRCULATION
ANEMIA
You May Like: Best Protein Shakes For Ulcerative Colitis
How To Treat Pain
There are various treatment options for UC, and the best approach for a person will depend on the severity of their symptoms. Over-the-counter medications can sometimes help relieve the pain that UC can cause. However, severe cases require stronger pain relievers.
Medications for the treatment of UC include:
Also Check: What Makes Ulcerative Colitis Worse
What Are The Causes And Risk Factors Of Ulcerative Colitis
Ulcerative colitis is believed to be caused by an abnormal response by your bodys immune system.
Your immune system is supposed to defend you against harmful invasive bacteria and viruses. But in some people, the immune system mistakenly attacks the bodys own tissue.
While we dont know exactly what causes ulcerative colitis, there are two leading theories:
Experts believe that ulcerative colitis develops because of a combination of environmental factors and genetic predisposition.
Fatty cold-water fish such as mackerel, tuna, salmon, sardines, and herring are rich sources of omega-3 fatty acids.
Editorâs Picks
Also Check: Nanda Nursing Diagnosis For Ulcerative Colitis
Secondary Cutaneous Manifestations Due To Adverse Effects Of Ibd Treatment
Skin manifestations from adverse effects can result in a broad range of secondary cutaneous manifestations, such as drug eruptions, urticaria, angioedema, hair loss, lichen planus, erythema multiforme, bullous dermatosis/reaction, StevensJohnson syndrome, acne, psoriasis and so on . The following are examples of drugs used in IBD treatments that can cause secondary cutaneous complications: 5-ASA, metronidazole, ciprofloxacin, azathioprine, 6-MP, methotrexate, cyclosporine, steroids, anti-TNF- agents, etc. .
Anti-TNF- agents have been used successfully in the treatment of IBD and psoriasis, but when treating IBD, anti-TNF- agents such as infliximab and adalimumab can paradoxically induce psoriasis lesions after the third or fourth infusion . The psoriasis lesions regressed after withdrawing the anti-TNF- agents in 16 out of 17 patients . Although there have only been 18 reported cases of anti-TNF induced psoriasis in the IBD population, but clinicians should still be aware of this potential side effect . It has been suggested that inhibition of TNF- induces over-expression of cutaneous IFN- which then causes predisposition to psoriasis . The treatment of psoriasis induced by anti-TNF- agents is cessation of the offending agents and topical steroid therapy .
Toxic Shock Syndrome And Scalded Skin Syndrome
Staphylococcus aureus is the organism responsible for classic toxic shock syndrome and scalded skin syndrome. Toxic shock syndrome can present with hypotension, erythema, fever and multisystem dysfunction.3 Most cases of nonmenstrual toxic shock syndrome occur in the postoperative setting.1
Several different staphylococcal exotoxins have been implicated. The syndrome may result from infection, or it may occur because of simple colonization with S. aureus.3 Staphylococcal scalded skin syndrome occurs in infants, young children and adults with immunosuppression or renal impairment.1
The rash is usually diffuse and can present as bullous impetigo, scarlatiniform lesions or diffuse erythema . The mucous membranes are spared in most patients. During the physical examination, the physician should attempt to elicit Nikolsky’s sign .1,3,4
Read Also: Signs Of Having A Stomach Ulcer
Psoriasis In Patients With Uc
Approximately 5% of UC patients experience psoriasis.3 Some studies have shown that symptoms of psoriasis can occur up to 15 years prior to the symptoms of UC or other inflammatory bowel diseases.1 Psoriasis and UC both appear to be linked in how they affect the immune system, which seems to explain why they are linked.2 Psoriasis causes red, itchy, scaly patches on the skin, which are known as plaques.3 These patches are common on the joints , the scalp and the chest and stomach area, but can occur anywhere on the body. Psoriasis may also cause changes in nail growth. The most common treatments for Psoriasis include topical corticosteroids, topical salicylic acid, systemic immunosuppressive agents, and injectable biological therapies.3
What To Do During A Flare
Most skin issues associated with UC are best treated by managing the UC as much as possible, as many of these rashes can coincide with UC flare-ups. Others may be the first sign of UC in someone who hasnt been diagnosed yet.
Corticosteroids can help with the inflammation that often causes the skin issues associated with UC. Eating a well-balanced diet can help promote overall health and may aid in preventing skin issues.
When you do experience a flare-up of UC skin rash, there are several things you can try:
- Keep the lesion clean to prevent infections.
- See your doctor for prescription antibiotic ointment or pain medication if needed.
Read Also: What To Eat To Help Stomach Ulcers
Mechanisms Between Ibd And Skin Disorders
Mucosal T-cells are important in maintaining intestinal homeostasis, defined as the balance between the mucosal epithelium, intestinal microbes, and host immune response . Abnormal T-cell response to these microbial antigens can disrupt this equilibrium and is believed to be the mechanism that triggers the chronic inflammation and excessive secretion of cytokines that lead to the development of IBD . It has been proposed that some EIMs seen with IBD manifest also as a result of immune dysregulation resulting in a lymphocyte mediated destructive process. Adams and Eksteen proposed IBD patients with hepatic EIMs could be explained by mucosal T-cells in the gut aberrantly traveling to the liver, becoming exposed to hepatic antigens, and ultimately causing liver damage. This article suggested that a similar mechanism could possibly explain the pathogenesis of other EIMs in patients with IBD .
Studies have implicated several immune pathways in cutaneous disorders of IBD. In addition to the two established effector CD4 T-cells, the Th1 and Th2 , a third novel T-helper cell has been described. Termed Th17 cells for its ability to produce interleukin-17 , these cells have been described in various systemic, inflammatory, and autoimmune skin disorders including psoriasis, contact or atopic dermatitis, scleroderma, systemic lupus erythematosus , Bechets disease, and IBD . This discovery brings to light new treatment targets for dermatologic disorders in the IBD population.
Managing And Treating Skin Problems Caused By Ulcerative Colitis:
Shutterstock
All of the above skin issues are related to ulcerative colitis, so the best way to manage them is to treat the underlying condition. Most of the time, you get skin rashes only during ulcerative colitis flare-ups. It is best to keep the condition in control to avoid getting these associated skin issues.
Ulcerative colitis-related issues are diagnosed with a combination of X-rays, blood tests, and stool tests. Alternatively, various medical imaging tests, such as MRIs, CT scans, and MRIs, are conducted for diagnosis.
Usually, doctors prescribe corticosteroids to manage skin inflammation. During a flare-up, you can take these measures to avoid skin issues:
- Take the prescribed corticosteroid to reduce the inflammation.
- Keep your skin or the affected area clean to reduce the chances of infection.
- Follow a well-balanced diet. Vitamins and nutrients are essential for your skin health.
- Keep open wounds, lesions, or patches covered with bandages.
- Use a doctor-prescribed topical ointment or pain medication to manage discomfort.
Skin rashes and other complications associated with ulcerative colitis improve once the underlying causes are treated. Doctors may prescribe topical or oral steroids, antibiotics, and immunosuppressant medicines, depending on your condition.
To be prepared to deal with ulcerative colitis skin rashes, it is important to know who is prone to develop the condition. Read on to know more.
Don’t Miss: Is Ulcerative Colitis A Serious Disease
What Are Other Common Skin Conditions Linked To Uc
Erythema nodosum is another common skin disorders in patients with inflammatory bowel diseases.1 EN may look like bruises, but they will feel like large raised bumps under the skin.2 They are usually warm to the touch, and very tender or even painful. EN is most commonly found on the legs, but it may occur in other places. Women tend to be more affected by EN than men, but there have been studies that show it happens equally in men and women.1 The treatment for EN is rest, oral corticosteroids, and in severe cases, immunosuppressive agents.3
Cutaneous Disorders Or Dermatosis Associated With Ibd
These disorders include hidradenitis suppurativa, phlebitis, erythema multiforme, urticaria, lichen planus, secondary amyloidosis, and various autoimmune skin disorders, such as acquired epidermolysis bullosa , bullous pemphigoid, linear IgA bullous dermatosis, vitiligo, and psoriasis . Rarely has IBD been reported to be associated with skin neoplasm such as Bowens disease and squamous cell carcinoma, which require surgical excision .
Read Also: Can You Get Ulcerative Colitis At Any Age
What Are The Most Common Skin Issues With Uc
Pyoderma gangrenosum is one of the most common skin disorders in UC patients.1 PG is often the immune system’s overreaction to minor trauma such as a needle stick or a surgical wound.2 It usually starts as a small bump or nodule under the skin which eventually becomes a deep, painful ulcer or crater-like hole in the skin. These ulcers are usually found at surgical sites but are also often found on the legs and feet.3 This condition is also supposed to be more common in women than men, but again, other studies have found that this can happen equally among both.1 PG is treated with oral and topical corticosteroids, immunosuppressive agents and injectable biological therapies as a last line of therapy.2
Diarrhea And Rectal Bleeding
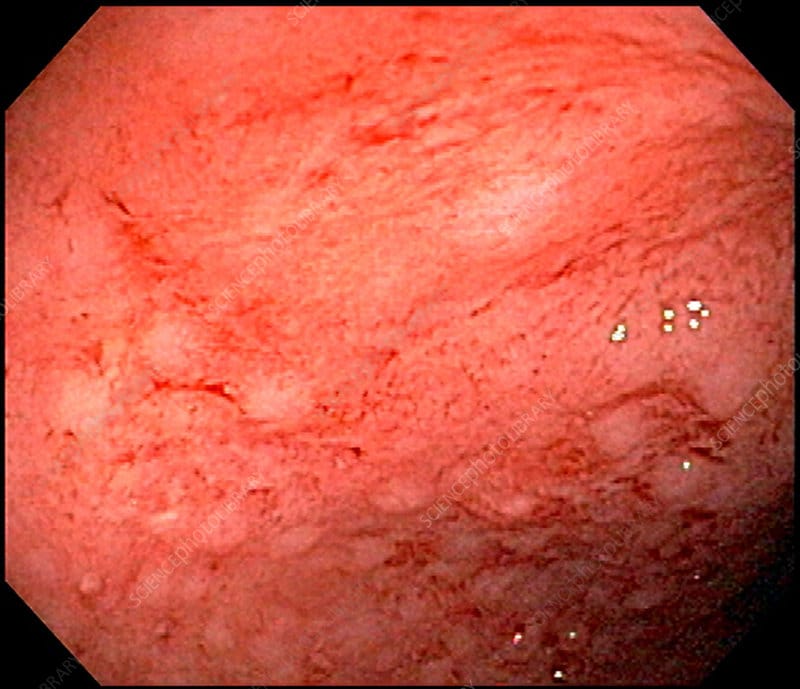
People with ulcerative colitis often experience watery diarrhea as well as frequent and sudden urges to have a bowel movement. For some people, the urge to have a bowel movement may occur so suddenly that it significantly disrupts their daily life. Some people need to have a bowel movement more than 10 times per day.
You may notice blood, pus, or mucus in your stools. You may also experience rectal bleeding if youre having a flare-up. Blood comes from ulcers along the surface of your rectum.
If you have uncontrollable diarrhea or notice blood in your stool, you should see a doctor. Diarrhea caused by ulcerative colitis can lead to medical emergencies like severe dehydration, a perforated colon, or .
Recommended Reading: Can You Take Tylenol With Stomach Ulcers