When To See A Dermatologist
Diabetes can cause many other skin problems. Most skin problems are harmless, but even a minor one can become serious in people who have diabetes. A board-certified dermatologist can recognize skin problems due to diabetes and help you manage them.
Are all dermatologists board certified?
No. See what it takes to become board certified.
ImagesImage 1: Image Courtesy of Clark C. Otley, MD. All Rights Reserved
Images 3, 7, 8, 9: Used with permission of the American Academy of Dermatology National Library of Dermatologic Teaching Slides.
Image 2 from DermNetNZ
Some images used with permission of Journal of the American Academy of Dermatology
ReferencesCohen Sabban, EN. Cutaneous manifestations of diabetes mellitus from A to Z. Focus session presented at: 74th Annual Meeting of the American Academy of Dermatology March 4-8, 2016 Washington D.C.
Duff M, Demidova O, et al. Cutaneous manifestations of diabetes mellitus. Clinical Diabetes. 2015 33:40-8.
Kalus AA, Chien AJ, et al. Diabetes mellitus and other endocrine disorders. In: Wolff K, Goldsmith LA, et al. Fitzpatricks Dermatology in General Medicine . McGraw Hill Medical, New York, 2008:1461-70.
McKinley-Grant L, Warnick M, et al. Cutaneous manifestations of systemic disease. In: Kelly AP and Taylor S. Dermatology for Skin of Color. . The McGraw-Hill Companies, Inc. China, 2009:481-4.
Morgan AJ and Schwartz RA. Diabetic dermopathy: A subtle sign with grave implications. J Am Acad Dermatol. 2008 58:447-51.
What Are My Treatment Options
Treatment will depend on many factors, including the reason for the condition and your health status and history. Other factors your doctor will consider are:
- Your specific symptoms.
- How severe your condition is.
- How well you can tolerate medications or procedures.
The most common treatment for venous insufficiency is prescription-wear compression stockings, she says. These special elastic stockings apply pressure at the ankle and lower leg. They help improve blood flow and can reduce leg swelling.
You also can improve blood flow by keeping your legs elevated whenever possible, which means keeping them uncrossed when you are seated and by exercising regularly.
If you need medication, the most commonly prescribed include:
- Diuretics. These medications draw extra fluid from your body through your kidneys.
- Anticoagulants. These medications thin the blood.
- Pentoxifylline . This medication helps improve blood flow.
Healthcare Advice For Leg Ulcers
There are some lifestyle changes you can make that will help boost healing:
- Maintain a healthy weight
- Eat a well-balanced diet that includes 5 portions of fruit and vegetables a day and protein rich foods such as eggs, fish, chicken or pulses
- Take light to moderate exercise such as cycling or walking for about thirty minutes at least three times a week
- Avoid standing or sitting for long periods of time
- Put your feet up elevate your legs above your heart.
- Every so often, move your feet around in circles, then up and down. This helps blood circulate and get back to your heart
Don’t Miss: How To Self Treat An Ulcer
Referral To A Specialist
In some cases, your GP or nurse may decide to refer you to a specialist in conditions affecting the blood vessels .
For example, you may be referred to a vascular specialist if your GP or nurse is unsure about your diagnosis, or if they suspect your ulcer may be caused by artery diseases, diabetes or rheumatoid arthritis.
After taking your medical history and examining you, the vascular specialist may need to arrange further investigations to plan your treatment.
Ulcers Caused By Problems With Blood Circulation
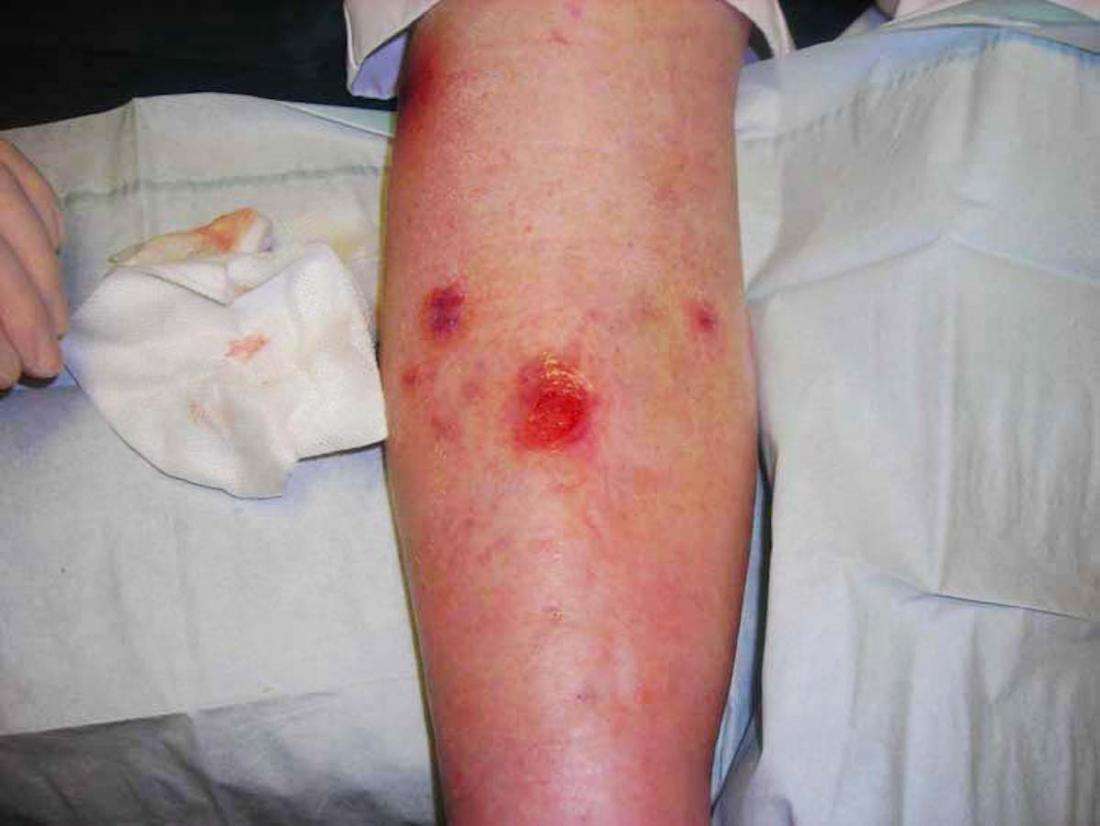
The blood supply coming to the skin is needed for the skin to heal after it has become broken or split for any reason. If there is a problem with circulation, the break in the skin does not heal, and may persist, leaving an ulcer. This may be a problem with the veins, the arteries, or the smaller blood vessels. The kinds of ulcers caused by circulation problems are:
- Venous ulcers. These ulcers and their treatment are described in the separate leaflet called Venous Leg Ulcers. They occur when the circulation in your legs is not working very well. Fluid tends to pool in the legs because the veins dont work well enough to pump the blood efficiently back to the heart . This type of ulcer is more common in people with varicose veins that have lead to associated skin problems such as varicose eczema. They are also more common if you are overweight or obese, or not very mobile for any reason. They can also occur when the circulation is damaged by a deep vein thrombosis .
- Arterial ulcers. These are caused by conditions affecting arteries see the separate leaflet called Peripheral Arterial disease.
- Vasculitic ulcers. These are caused by a number of conditions which cause blood vessels to become inflamed. This is called vasculitis.
Also Check: Corneal Ulcer Dog Home Remedy
What Are Venous Stasis Ulcers
Commonly located on the ankle or calf, venous stasis ulcers are painful and red in color but may be covered with a yellow, fibrous tissue and an irregular border.
Drainage and discharge are possible with venous stasis ulcers. This type of ulcer is common in patients with a history of leg swelling or varicose veins.
Treatment What Treatment Will I Be Offered For My Leg Ulcer
If your wound isnt healing because of venous hypertension and there are no problems with the blood supply to your legs, then you should be offered compression therapy.
Compression therapy improves blood supply by applying pressure to the leg. This can be done by bandaging the lower leg or by wearing supportive socks, stockings or tights. Compression therapy is very effective at reducing swelling, improving blood flow in the veins and healing or preventing sores or ulcers.
There are lots of different types of compression therapy so ask your nurse to find something that is right for you.
Compression can be a little uncomfortable when you first start treatment but should not cause you any pain. Any discomfort should reduce as the swelling goes down. If you do experience discomfort, talk to your nurse or doctor about it and they will advise you on ways of alleviating this.
In addition to the compression, your nurse should also advise you on wound care and dressings to keep your wound healthy.
You May Like: What To Avoid Eating With Ulcerative Colitis
How Should I Treat A Leg Infection
The most appropriate treatment for a leg infection depends on the particular type of infection. Some affect a persons skin cells while others may involve the bone or lymph nodes. If a person suspects he has an infected leg, he should see a doctor for a diagnosis and treatment recommendation. Some seemingly minor infections can become severe if left untreated or if theyre treated with the wrong types of medication.
One type of infection that may affect a persons leg is called cellulitis. This infection involves the cells right below the skins surface, causing inflammation in the affected area. It develops when the skin is broken, such as because of a cut, broken blister or animal bite. The broken skin allows bacteria to enter the body, which leads to the infection. There are many types of bacteria that cause cellulitis, but those in the strep family are the most common.
Oral antibiotics are usually used to treat a cellulitis leg infection and usually cure it within a week or so. A patient may return to his doctor after about a week to check whether it has gone away entirely. In a severe case, a person may need to be hospitalized and treated with intravenous antibiotics.
Dont Miss: Will Doctors Prescribe Antibiotics Over Phone
What Is A Venous Stasis Ulcer
Venous ulcers are open, non-healing wounds that occur on the legs or ankles. They often develop when blood is not circulating properly and begins to pool in these regions. This accumulation of blood accounts for over 80 percent of all ulcers.
Venous leg ulcers can lead to serious medical problems like infection and skin discoloration.
Recommended Reading: Low Dose Aspirin Ulcerative Colitis
Venous Ulcer Diagnosis And Treatment
Doctors at Vascular surgeons at UPMC’s Heart and Vascular Institute use duplex ultrasound, a noninvasive test, to diagnose abnormal veins that cause venous ulcers. Part of the UPMC difference is that we actively look for the causes of the ulceration to treat venous pathology and keep the ulcer healed.
After an evaluation of your veins, we recommend a treatment plan based on your needs:
- Compression
- Compression of the leg is vital to healing venous wounds.
- Compression stockings are most commonly used for this treatment.
- The pressure from the compression dressing counteracts the pressure from the veins of the leg and allows skin to heal.
Signs And Symptoms Of Venous Ulcers
Symptoms may show up even before an ulcer forms, such as:
- Swelling, heaviness or cramping in the legs
- Hardening or thickening of the skin
- Dark red, purple or brown discoloration
Signs and symptoms of venous ulcers include:
- Sore on the inside of the leg or just above the ankle. The base of the wound is red and is sometimes covered by yellow tissue. The edges of the ulcer may be unevenly shaped.
- Skin around the wound is shiny, warm or hot, tight and discolored.
- Pain in the leg.
Also Check: Is Kimchi Good For Ulcerative Colitis
What Type Of Treatment Is Given For Leg Ulcers
The type of treatment that you are given will depend upon the severity of the ulcer. If the ulcer hasnt completely formed and a sore hasnt broken out, you may only need to use compression stockings and keep the leg elevated. This will help reduce swelling and prevent the ulcer from forming.
If an open sore has developed on the lower leg, the treatment that is recommended will be more intense. Treatment for severe ulcers includes antibiotics to fight infections, surgery to clean the wound, and dressing to protect the wound. If it is determined the ulcer is caused by venous insufficiency, your doctor may recommend you seek treatment from a vein specialist to treat the problem.
Schedule an appointment at Vein911 to discuss treatment options for leg ulcers and vein insufficiency.
The Old Understanding Of Venous Leg Ulcers
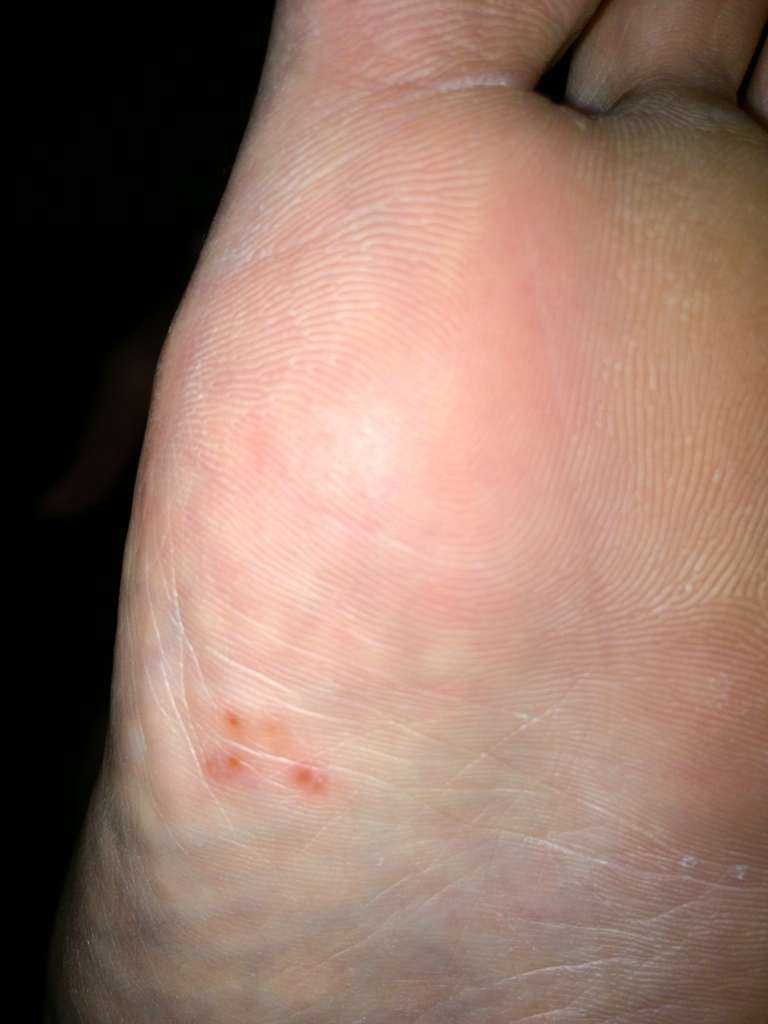
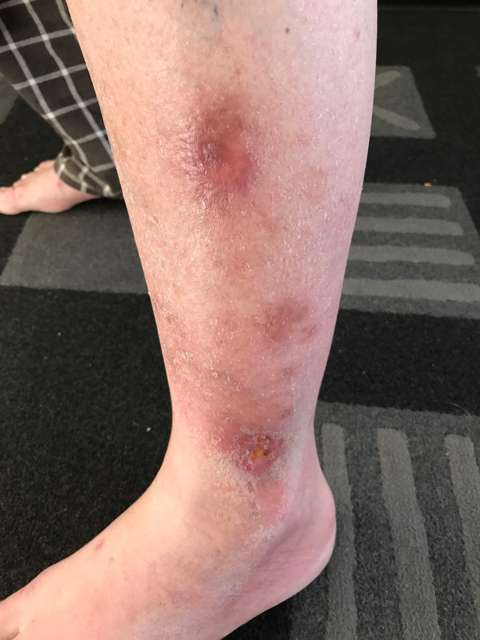
Until the 1980s, most doctors and nurses had a clear understanding of the difference between venous leg ulcers and varicose veins.
Unfortunately, it turned out that they were wrong!
When valves failed in the superficial veins, they swelled on the surface causing varicose veins.
They believed that the deep veins could not be treated and so the only way to treat venous leg ulcers was to wrap the leg in compression bandages and dressings.
They also believed that the superficial veins caused no inflammation. Although they could be treated by varicose vein surgery, there was no need to do so as varicose veins were only cosmetic.
They believed in only 2 systems of veins in the legs the deep and superficial systems. The deep veins were in the muscles. The superficial veins in the fat under the skin.
When valves failed in the deep veins, this resulted in inflammation at the ankles. After a time, this inflammation would accumulate until the ankles swelled, the skin turned brown and leg ulcers appeared.
It is a great pity that many doctors and nurses still believe this, as it is totally incorrect.
This error has resulted in patients with leg ulcers failing to get the right treatment and ending up in compression for years. It also resulted in patients with varicose veins being left untreated, deteriorating towards complications such as leg ulcers in the future.
Don’t Miss: Rice Recipes For Ulcerative Colitis
Diagnosis Of Leg Ulcers
- examine the wound
- perform some tests to measure the blood flow in your lower leg, such as the ankle-brachial index. This test compares blood pressure readings taken at the ankle and at the arm using a device called a Doppler machine
- recommend an angiogram for an arterial ulcer, to find out if the artery needs surgery to clear the blockage.
What Is The Treatment For Leg Ulcers
Where possible, treatment aims to reverse the factors that have caused the ulcer. As an ulcer is often the result of both arterial and venous disease, careful assessment is needed first.
Venous leg ulcer, in the absence of arterial disease, is usually treated with exercise, elevation at rest, and compression. Compression must not be used if there is significant arterial disease, as it will aggravate an inadequate blood supply. Surgery, ultrasound-guided sclerotherapy or endovascular laser treatment of superficial and perforator leg veins may also help, particularly if the deep venous system is intact. Venous-return assisted calf compression devices may be of additional benefit.
A vascular surgeon should also assess patients with arterial leg ulcers as they may require surgery to relieve the narrowing of the arteries. Revascularisation is particularly important if the ABPI is less than 0.5.
It is also very important to treat underlying diseases such as diabetes and to stop smoking.
You May Like: Is Ensure Good For Ulcerative Colitis
How Should We Define Wound Infection
Virtually all open wounds are colonized with microorganisms, but this usually has no clinical consequences, because they show no evidence of infection and heal as expected . Some wounds are clearly infected they have purulent secretions or some of the cardinal manifestations of inflammation that have classically defined the host response to tissue damage caused by pathogenic and invasive microorganisms . The likelihood that a wound will become infected is related directly to the inoculum size and virulence of the colonizing organisms and inversely related to local and systemic host resistance . But some wounds occur in patients with neuropathy , ischemia , or venous insufficiency . Because these conditions limit the expression of inflammation, some define infection by secondary signs of local infection, . A Delphi approach by an international group of 54 wound care experts produced consensus on criteria they deemed common to infection in all chronic wounds: cellulitis, malodor, pain, delayed healing, deterioration or breakdown, and increased exudate . Some of these criteria have purportedly been validated by studies of various wounds in several settings, but the findings are limited by the fact that they compare the clinical criteria to inadequately validated microbiological definitions of infection . Furthermore, the additional evidence of infection likely varies for different types of chronic wounds .
Read Also: Best Foods To Eat When You Have A Stomach Ulcer
Controlling Pressure In The Leg Veins
Controlling swelling is essential for patients with venous leg ulcers. Leg elevation, with the feet at or above the level of the heart, several times throughout the day and while sleeping, can help reduce swelling. Compression wraps or bandages are often applied to the legs. These can be changed as often as multiple times a day or as infrequently as once a week, depending on the amount of fluid draining from the ulcer. Once the leg ulcer is smaller or nearly healed, elastic compression stockings may be recommended. Compression stockings are sized to fit the legs and are typically put on in the morning and worn throughout the day. A venous pump may be prescribed for patients with severe swelling.
Recommended Reading: Do Tums Help Ulcerative Colitis
Swelling In The Legs And Ankles
Venous leg ulcers are often accompanied by swelling of your feet and ankles , which is caused by fluid. This can be controlled by compression bandages.
Keeping your leg elevated whenever possible, ideally with your toes at the same level as your eyes, will also help ease swelling. You should put a suitcase, sofa cushion or foam wedge under the bottom of your mattress, to help keep your legs raised while you sleep.
You should also keep as active as possible and aim to continue with your normal activities. Regular exercise, such as a daily walk, will help reduce leg swelling. However, you should avoid standing or sitting still with your feet down. You should elevate your feet at least every hour.
What Are The Symptoms
Skin ulcers look like round, open sores. They range in severity and are usually minor injuries on the skin.
In severe cases, ulcers can become deep wounds that extend through muscle tissue, leaving bones and joints exposed.
The symptoms of skin ulcers include:
- discoloration of the skin
People can develop the following types of skin ulcer:
Read Also: Can You Eat Cheese With Ulcerative Colitis
Symptoms Of Leg Ulcers
- that they are commonly found on the lower leg and ankle
- a sunken, asymmetrically shaped wound
- the edges of the ulcer are clearly defined from the surrounding skin
- the surrounding skin is intact, but inflamed
- the surrounding skin may be pigmented, hardened or calloused
- yellowish-white exudate
- varicose veins in the leg.
What Are Little White Worms Coming Out Of My Dogs But
A tapeworm body consists of multiple parts, or segments, each with its own reproductive organs. Tapeworm infections are usually diagnosed by finding segmentswhich appear as small white worms that may look like grains of rice or seedson the rear end of your dog, in your dogs feces, or where your dog lives and sleeps.
Don’t Miss: Signs Of A Bleeding Stomach Ulcer