How Ulcerative Colitis Causes Nausea
Depending on the circumstances, nausea can be a , confrms Loretta Randolph, R.N., a clinical research nurse in digestive diseases at the University of Cincinnati in Cincinnati, OH. Although nausea can strike at any time, patients are most likely to experience it during a , she adds.
On the other hand, itself may also be to blame, says Randolph, since nausea can be a side effect of some oral UC medications.
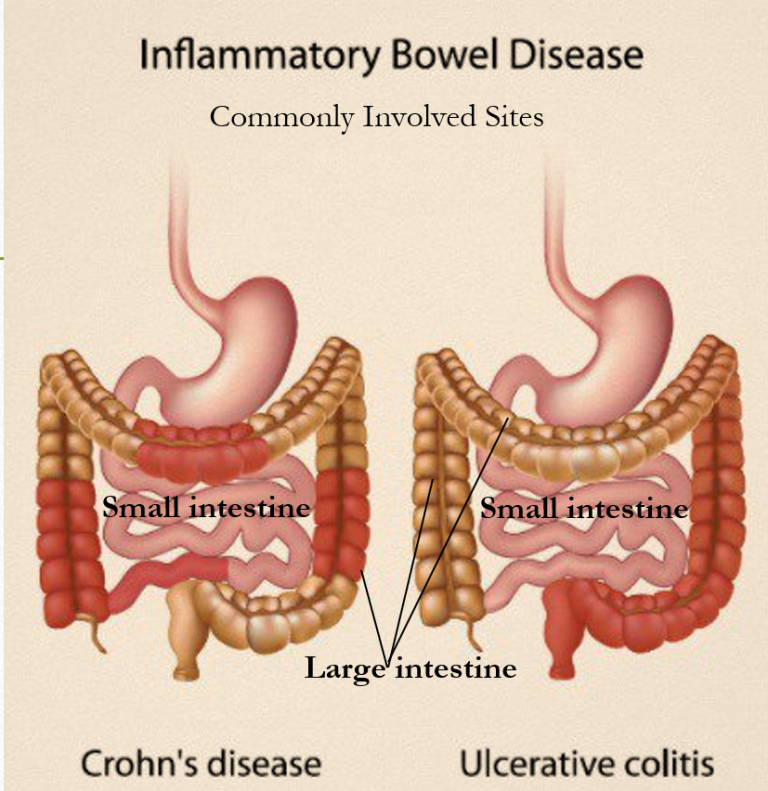
Disease severity and the location of your ulcerative colitis can also influence symptoms. According to the National Institute of Diabetes and Digestive and Kidney Diseases, nausea and vomiting are more likely to occur if your or affects more of your large intestine.
How Is Ulcerative Colitis Treated
Theres no cure for ulcerative colitis, but treatments can calm the inflammation, help you feel better and get you back to your daily activities. Treatment also depends on the severity and the individual, so treatment depends on each persons needs. Usually, healthcare providers manage the disease with medications. If your tests reveal infections that are causing problems, your healthcare provider will treat those underlying conditions and see if that helps.
The goal of medication is to induce and maintain remission, and to improve the quality of life for people with ulcerative colitis. Healthcare providers use several types of medications to calm inflammation in your large intestine. Reducing the swelling and irritation lets the tissue heal. It can also relieve your symptoms so you have less pain and less diarrhea. For children, teenagers and adults, your provider may recommend:
Children and young teenagers are prescribed the same medications. In addition to medications, some doctors also recommend that children take vitamins to get the nutrients they need for health and growth that they may not have gotten through food due to the effects of the disease on the bowel. Ask your healthcare provider for specific advice about the need for vitamin supplementation for your child.
You might need surgery that removes your colon and rectum to:
- Avoid medication side effects.
- Prevent or treat colon cancer .
- Eliminate life-threatening complications such as bleeding.
What Diet Is Best For Ulcerative Colitis
There is no specific diet or meal plan for ulcerative colitis , according to the U.K.s National Health Service . Some people may find that certain foods trigger symptoms or make them worse.
You may find that consuming a diet low in fiber during a UC flare may help ease your symptoms. Foods you can consume as part of a low fiber eating plan include:
Other meal plan tips for UC include:
- eating smaller meals more frequently rather than fewer larger meals
- drinking plenty of fluids
- taking food supplements at your doctors advice
- avoiding caffeine and alcohol, which can make diarrhea worse
- avoiding fizzy drinks, which can cause gas
- keeping a food diary to monitor which foods may be triggering your symptoms
Contact your doctor before making any significant changes to your eating habits. Your doctor may refer you to a dietitian or nutritionist to help make sure you get all of the nutrients you need while managing your symptoms.
Find out more about foods that can affect UC. You can also learn more about meal planning with UC.
Also Check: Ulcerative Colitis Lower Back Pain
What Are The Symptoms Of Ulcerative Colitis
Ulcerative colitis symptoms often get worse over time. In the beginning, you may notice:
- Diarrhea or urgent bowel movements.
- Abdominal cramping.
- Loss of fluids and nutrients.
Symptoms are similar in pediatric ulcerative colitis and may also include delayed or poor growth. Some ulcerative colitis symptoms in children can mimic other conditions, so it is important to report all symptoms to your pediatrician.
Connect With Others Who Understand
Have you experienced nausea with IBD? Its a frustrating symptom, but it can be helpful to know youre not alone.
MyCrohnsAndColitisTeam is the social network for people with IBD and their loved ones. More than 157,000 members come together to share their stories, ask questions, and let others know what has helped them manage IBD symptoms including nausea.
If youve found a way of managing your nausea with IBD, share your tips with others! Join MyCrohnsAndColitisTeam today and connect with others in the comments below or by starting a new conversation thread.
You May Like: Foods Bad For Ulcerative Colitis
What To Eat For Acid Reflux
Whether its a chronic condition or a newfound symptom of stressful days, heartburn happens! Avoiding spicy, acidic and fried foods as well as cutting back on alcohol and chocolate can help douse the flames and there are some foods you should gravitate towards to help reduce the discomfort. Heres what you can eat to help keep heartburn symptoms from being too upsetting.
Symptoms That May Indicate You Are Suffering From Colitis
posted: Mar. 01, 2019.
Colitis literally means inflammation of the colon, and it happens when the lining of your digestive tract has become damaged, causing it to become inflamed and sore. There are a few reasons this damage might occur, including infection, food poisoning, restricted blood flow to the colon, and as a side-effect of cancer treatment.
Colitis can also be because of inflammatory bowel disease, such as Crohn’s disease or the most common form, ulcerative colitis. Inflammatory bowel disease affects over 1.6 million Americans , but you might not know you have anything more than the occasional stomach ache or digestive issue.
There are four particular symptoms that indicate you may suffer from colitis. If you recognize any of these signs, book a consultation to come and see the Hawaii Gastroenterology Specialists.
Read Also: How Long Do Ulcerative Colitis Flare Ups Last
Symptom No : Rectal Bleeding
Solution: Stay calm. It probably looks worse than it actually is. If hemorrhoids are the cause, the bleeding will be minimal and can be treated with sitz baths, soluble fiber supplements, or medication, such as steroid suppositories, Dr. Vaughn says. If its caused by an uptick in inflammation, though, you and your doctor may need to adjust your treatment plan.
Until you figure out whats behind your bleeding, consider wearing a sanitary pad or incontinence underwear.
The Worst Foods For Those With Ulcerative Colitis
Ulcerative colitis is an inflammatory chronic disease of the colon and rectum where ulcers develop inside the lining of the large intestine. It is an inflammatory bowel disease along with Crohns Disease which causes a multitude of painful and unpleasant symptoms. Since dietary habits can contribute to ulcerative colitis symptoms, lets look at the worst foods for those with ulcerative colitis.
Don’t Miss: Stomach Ulcer Treatment Over The Counter
Diet And Meal Management
Some people successfully manage their IBD symptoms by adjusting their dietary and meal-management plans. Foods that trigger IBD symptoms vary from person to person, so keeping a food diary can help you identify whats helping or worsening your nausea.
UCSF Health recommends these approaches to help manage IBD symptoms during a flare:
- Lower the amount of sugar you consume
- Lower your alcohol consumption
- Try adding omega-3 fatty acids to your diet
Changing when you eat and your behavior around meals may help, too. Crohns and Colitis Canada recommends the following:
- Eat small meals and snacks so your stomach is never empty.
- Eat slowly, so your stomach is not filled up too quickly.
- Drink beverages 30 to 60 minutes before or after you eat instead of during your meal.
- Avoid lying down for at least one hour after eating.
Ask your doctor to refer you to a dietitian, who may also help you find the diet that works well for you.
Symptom No : Abdominal Cramps
Solution: Try to pinpoint your triggers. Stomach cramps are often caused by gas or spasms in the gut. Common culprits include foods high in fiber or fat, which can impact gas production, says , an assistant professor of medicine at the University of Minnesota Medical School in Minneapolis and director of their inflammatory bowel disease program. Foods that are high in insoluble fiber especially cruciferous vegetables, such as broccoli and cauliflower can be particularly hard to digest, according to the Crohns & Colitis Foundation.
Medications, such as a recent course of antibiotics or nonsteroidal anti-inflammatory medications ibuprofen, naproxen, aspirin can also trigger abdominal pain, he says.
Also Check: Can Alcohol Cause Stomach Ulcers
What Causes Ulcerative Colitis
Researchers think the cause of ulcerative colitis is complex and involves many factors. They think its probably the result of an overactive immune response. The immune systems job is to protect the body from germs and other dangerous substances. But, sometimes your immune system mistakenly attacks your body, which causes inflammation and tissue damage.
What Is The Outlook For Someone With Ulcerative Colitis
Ulcerative colitis can be managed with treatment. It generally wont alter the life expectancy of most people.
Most people with UC experience acute flares of symptoms during their lifetime. But with treatment, the disease can enter remission, during which symptoms go away.
Remission may last for weeks or even years. The longer the period of remission, the better a persons general health becomes.
Dr. Saurabh Sethi is a board certified physician specializing in gastroenterology, hepatology, and advanced interventional endoscopy. In 2014, Dr. Sethi completed his gastroenterology and hepatology fellowship at Beth Israel Deaconess Medical Center at Harvard Medical School. Soon after, he completed his advanced endoscopy fellowship at Stanford University in 2015. Dr. Sethi has been involved with multiple books and research publications, including over 30 peer-reviewed publications. Dr. Sethis interests include reading, blogging, traveling, and public health advocacy.
Read Also: What To Put On Leg Ulcers
What Causes Ulcerative Colitis Flareups
When youre in remission from ulcerative colitis, youll want to do everything you can to prevent a flareup. Things that may cause a flareup include:
- Emotional stress: Get at least seven hours of sleep a night, exercise regularly and find healthy ways to relieve stress, such as meditation.
- NSAID use: For pain relief or a fever, use acetaminophen instead of NSAIDs like Motrin® and Advil®.
- Antibiotics: Let your healthcare provider know if antibiotics trigger your symptoms.
This Gastrointestinal Disease Is Known For Its Stabbing Pain And Cramping But An Upset Stomach Is Often Not Far Behind
by Health Writer
If youre dealing with ulcerative colitis , you know all about the desperate sprints to the bathroom and finding yourself doubled over in pain from abdominal cramps. Another symptom thats less discussed? That feeling like you are on a rocky boat in the middle of the ocean, about to lose your lunch. isnt as commonly associate with nausea, but when it hits it can be debilitating.
Like many , nausea can be caused by many things beyond your chronic condition. As such, it take some investigating to be sure that the queasiness you feel is related to your ulcerative colitis and not another cause. We asked the experts for indicators that nausea may be due to this gastrointestinal disease, plus ways to get your gut back on track so you can feel your best.
You May Like: Medihoney For Stage 1 Pressure Ulcer
Stomach And Back Pain At The Same Time
For most of us, its not uncommon to have an occasional stomachache or acute back pain. But what does it mean if both are happening at the same time? This could be a coincidence, but it may also be concerning to notice two disconnected symptoms. The combination of pains may make daily activities difficult or be distracting. If the pain reaches this level, it may be a good idea to visit an Atlanta MRI center to rule out any serious conditions that could cause both problems at the same time.
If your stomach ulcers caused by a Helicobacter pylori bacterial infection, youll be given:
- a course of antibiotics
- a medication called a proton pump inhibitor
This is also recommended if its thought your stomach ulcers caused by a combination of an H. pylori infection and non-steroidal anti-inflammatory drugs .
Read Also: What Can I Do For Mouth Ulcers
How It Affects Daily Life
The diagnosis of UC usually comes before an individual reaches 35 years old. However, theres another time in life when UC is most frequently diagnosed at around 60 years old. An estimated 12 percent of those with UC are diagnosed in the decades before and after this age.
Regardless of when the disease is diagnosed, UC can take a significant physical and emotional toll on those living with this chronic condition.
The urgent need to use a bathroom multiple times a day can interfere with your social activities and your ability to work. Diarrhea can be unpredictable, highly inconvenient, and potentially embarrassing. In addition to physical symptoms, people living with UC may experience:
- elevated stress
Your doctor may be able to pinpoint some potential triggers. You may also find it helpful to keep a daily journal to track what you eat, your physical activities, and stressful events. In time, you may be able to identify a pattern that leads to diarrhea.
Read Also: Aloe Juice For Ulcerative Colitis
In My Shoes: 24 Hours With Crohns Or Colitis App
In My Shoes is an immersive experience that allows anyone to find out first-hand what its like to have Colitis.
From low energy levels to managing pain, from rushing to the toilet to juggling work and a social life, the app will allow friends, family and anyone you want, to see first-hand how the condition can affect every part of your body, and every aspect of your life.
We have information for friends and family, employers, and colleagues. Find all our information online.
We have around 50 Local Networks across the UK that bring local people affected by Crohns and Colitis together. They are run by volunteers and host a range of events, from educational talks to socials. Check our website or call our Helpline to find your nearest Local Network.
You May Like: Icd 10 Stage 3 Pressure Ulcer Sacrum
What Are The Risk Factors Of Ulcerative Colitis
The cause of ulcerative colitis is unclear, but its thought that a combination of genetics and environmental factors are at play. Up to 20 percent of people with ulcerative colitis have a parent, sibling or child with the disease.
Ulcerative colitis is more common for people living in urban, industrialized areas compared to undeveloped countries, which indicates that highly refined diets may play a role. Although all ethnic groups are affected, the problem is most common among Caucasians and people of Eastern European Jewish descent.
Lastly, there appears to be a connection to nonsteroidal anti-inflammatory medications. Its not that these medications cause the disease but, because they inflame the bowel, they can worsen symptoms. This category of medication includes ibuprofen , naproxen sodium and diclofenac sodium .
Also Check: Can Ulcers Cause Chest Pain And Shortness Of Breath
Managing Vomiting With Ibd
People living with IBD may experience vomiting for the same reasons they have nausea. For adults with IBD, vomiting greenish-yellow fluid called bile can be normal or a sign of an obstruction of the intestines.
While managing vomiting at home, avoid eating solid food and anything besides clear liquids until the vomiting episode is over. Be aware of the symptoms of dehydration like confusion, dark yellow urine, and excessive thirst.
People living with IBD should consider contacting their health care providers about vomiting sooner than those without the condition because of the risk of serious complications such as bowel obstruction with Crohns disease. Adults should seek medical attention after one to two days of vomiting or if they have any of the following symptoms with the vomiting:
- Blood in your stool or vomit
- Fever over 101 degrees Fahrenheit
- Severe cramping or belly pain
- Severe headache
If youre caring for a child with IBD who is vomiting, bring them to medical professionals quicker than if they were an adult, as they are at higher risk for complications like dehydration.
People Describe How They Were Diagnosed With Ulcerative Colitis
Ulcerative colitis, or UC for short, is a form of inflammatory bowel disease that affects portions or all of your large intestine and rectum. The Centers for Disease Control and Prevention estimates that 3.1 million Americans have IBD, which also includes Crohn’s disease .
UC is a chronic conditionthat can cause long-term inflammation and ulceration, severe diarrhea, abdominal pain, blood and mucous in your stool, urgency, nausea, joint paint, fever, weight loss, and fatigue. UC is also a risk factor in colorectal cancer, according to the Mayo Clinic. And while there’s no known cure for ulcerative colitis, removal of the colon and rectum in a procedure called a proctocolectomy can eliminate the disease.
Other treatment options include corticosteroids, anti-inflammatory drugs called 5-aminosalicylates, immunosuppressant biologics , and bowel resection or removal. Patients can also manage symptoms with pain medication, anti-nausea medication, and antidiarrheals, though all medications should be taken under the care of a doctor. IBD is often confused with irritable bowel syndrome , a disorder that causes pain and cramping of the large intestine. But unlike IBD, IBS doesn’t cause long-term damage to your intestinal tissue or increase your risk of colorectal cancer.
Managing UC is a complex puzzle of treatment options and unpredictable symptoms. We spoke with nine women to find out what life is like with the disease.
Related:
Recommended Reading: Does Ulcer Pain Come And Go
Complications Of Ulcerative Colitis
Complications of ulcerative colitis include:
- primary sclerosing cholangitis where the bile ducts inside the liver become damaged
- an increased risk of developing bowel cancer
- poor growth and development in children and young people
Also, some of the medications used to treat ulcerative colitis can cause weakening of the bones as a side effect.