When Should I Go To The Emergency Room
If you have a vascular ulcer, you should go to the emergency room if it becomes infected and you develop certain symptoms.
- Skin turning dark brown or black around the affected area, especially if this involves your toes.
- Fever or chills.
- A bad odor coming from a vascular ulcer.
- If a vascular ulcer starts to ooze or bleed more than before, especially if the fluid coming out is cloudy or yellow.
- If there is swelling, redness or the wound and its surrounding area are warm or hot to the touch.
A note from Cleveland Clinic
Vascular ulcers are generally a sign of an underlying chronic health condition. While these conditions are serious, it is possible to manage them and keep on enjoying your life. Your healthcare provider can offer you guidance, resources and more, all of which can help you do what it takes to keep chronic conditions from interfering with how you want to live your life.
What Causes Venous Insufficiency Ulcers
There are two important causes of venous insufficiency ulcers. One half to two-thirds of venous insufficiency ulcers result from progressive disease of the leg veins. The course of such disease is predictable: it starts with the development of varicose veins caused by refluxing of blood within the veins due to incompetent valvular structures. These varicosities may cause variable swelling and discomfort. As disease progresses, skin changes occur which eventually lead to the formation of a venous insufficiency ulcer. The course of the disease often culminates in ulcer formation in patients in their 60s and 70s.
Approximately one-third to one-half of venous insufficiency ulcers occur after the patient experiences DVT . DVTs may cause the process of ulcer formation to occur more quickly than in primary venous insufficiency as described above. Patients who have had a DVT may also present with hemosiderin staining, swelling and discomfort, making it difficult to distinguish post-phlebotic ulcer formation from ulcer formation stemming from venous insufficiency.
Other Types Of Leg Ulcer
Other common types of leg ulcer include:
- arterial leg ulcers caused by poor blood circulation in the arteries
- diabetic leg ulcers caused by the high blood sugar associated with diabetes
- vasculitic leg ulcers associated with chronic inflammatory disorders such as rheumatoid arthritis and lupus
- traumatic leg ulcers caused by injury to the leg
- malignant leg ulcers caused by a tumour of the skin of the leg
Most ulcers caused by artery disease or diabetes occur on the foot rather than the leg.
Page last reviewed: 11 January 2019 Next review due: 11 January 2022
Recommended Reading: Cpt Code For Ulcerative Colitis
How Can These Ulcers Be Prevented
Once an ulcer has developed, statistics show that another one will develop within 3-5 years. You know that preventing ulcers is well worth the effort if you have experienced the pain and frustration associated with healing wounds. Many patients will continue to wear some type of compression stocking every day while they are on their feet to help the circulation. While a Venous Stasis ulcer may have healed the poor circulation which caused the ulcer has not been corrected. Use AMERIGEL Care Lotion on your lower legs, particularly around the ankles daily. This helps the skin retain its natural moisture, promoting healthier skin that is less prone to problems.
AMERX Health Care Corporation164 Douglas Rd E, Oldsmar, FL 34677 | 448-9599 | AMERXHC.com
AMERX®, AMERIGEL®, HELIX3®, EXTREMIT-EASE®, Where Compression Meets Compliance®, Turn-Key DME®, and Oakin®, are registered trademarks of AMERX Health Care Corporation.
AMERX®, AMERIGEL®, HELIX3®, EXTREMIT-EASE®, Where Compression Meets Compliance®, Turn-Key DME®, and Oakin®, are registered trademarks of AMERX Health Care Corporation.
Elevation Of The Legs
The legs should be placed in an elevated position, ideally at 30 degrees to the heart, while lying down. This, again, helps in the movement of venous blood to the heart.This also prevents the build-up of liquid in the legs that leads to swelling. A cushion or any other object of comfort can be used to keep the toes above the level of the hip while sleeping.
Read Also: Bone Broth And Ulcerative Colitis
Making Healthy Lifestyle Choices
Maintaining a healthy lifestyle has a direct impact on vein health. A nutritious diet, regular exercise, maintaining a healthy weight, and following the recommendations of your health care provider can slow the progression of vein disease, ensure the successful outcome of vein treatment, and promote healing.
Clinical Features Of Venous Foot Ulcers
It is necessary to distinguish venous ulcers from other ulcer types as the management plan differs according to the etiology. The following characteristic clinical features can help clinicians diagnose venous ulcers:
- Shallow ulcers with irregular margins are present in the gaiter region. However, the location can be variable and ulcer might also be present on the lateral malleolus.
- Patients usually have a history of DVT or venous insufficiency.
- Red granulation tissue or exudate is present in the ulcer bed.
- Hemosiderin deposits leading to hyperpigmentation and “lipodermatosclerosis” around the ulcer wound are observed.
- Eczematous changes are seen in the skin near the ulcer edge.
Read Also: Foods For Gerd And Ulcers
Deterrence And Patient Education
Individuals affected with VLUs can have an impaired quality of life, mainly related to disability. Plus, heavy exudates can cause malodor, social isolation, and emotional disturbances that severely impact life quality. Compliance is essential to achieve a successful outcome.
Patients should be educated because VLUs are chronic processes that require lifelong evaluation and care, even after wound closure. Additionally, conformity to diet and lifestyle modifications may reduce the risk or recurrence, but evidence is lacking.
Why Is It Important To Seek Venous Ulcer Treatment
Venous ulcers dont heal on their own. The longer you live with them, the greater the likelihood of permanent tissue damage. The damage can spread or cause infections that can become life- or limb-threatening, such as gangrene.
In severe cases, it may be necessary to surgically remove your affected limb. Timely care from an experienced wound care provider significantly lowers this risk.
Also Check: Natural Ways To Heal Ulcerative Colitis
Is A Venous Ulcer A Pressure Ulcer
Asked by: Marguerite Goyette
Yes. Venous skin ulcers are caused by poor circulation in the legs caused by damaged valves that prevent blood from flowing the wrong way, allowing blood to pool in the legs. Pressure ulcers, on the other hand, are caused by sustained pressure on an area of the body, which cuts off blood flow.
What Types Of Venous Disease Cause Venous Stasis Ulcers
Chronic venous insufficiency is a common cause of valve dysfunction. It occurs when your valves are damaged or too weak to do their job.
Other venous ulcer causes include:
- High blood pressure , which damages blood vessel walls.
- Venous obstruction, a vein blockage thats sometimes due to blood clots.
- Venous reflux, when blood flows backward through weak or damaged valves.
Recommended Reading: Foods To Eat When You Have An Ulcer
Challenges Of Managing Stasis Ulcers
Stasis ulcers are a serious and chronic condition that can be difficult to treat. Infection is a frequent complication. If left unchecked, infection could progress to cellulitis or even septicemia, which in extreme cases could result in the need to amputate. There is also the risk of malignancy, most commonly squamous cell carcinomas.
It is essential that ulcers receive careful treatment and management, and that active steps are taken to prevent a recurrence. To reduce the risk of complications, patients are advised to seek treatment from a wound care specialist.
What You Need To Know
-
The cornerstone of treatment for venous leg ulcers is compression therapy, but dressings can aid with symptom control and optimise the local wound environment, promoting healing
-
There is no evidence to support the superiority of one dressing type over another when applied under appropriate multilayer compression bandaging
-
When selecting a dressing, look at the wound bed, edge and surrounding skin and decide on the goal of the dressing: for example, if there are signs of localised infection consider an antimicrobial dressing, if there is heavy exudate consider an absorbent dressing
A 65 year old man presents with a two month history of a wound in the gaiter area of his left leg. He has a history of a left leg deep vein thrombosis after a long flight but is otherwise fit and well. He had been self-managing with dressings bought over the counter, but the wound has gradually increased in size. The wound is not painful but is weeping serous fluid, causing irritation of the surrounding skin. Examination shows a 4×3×0.1cm wound above the left medial malleolus. There is haemosiderin deposition, venous flare, and moderate oedema in the limb. The ankle-brachial pressure index is normal at 1.0. He is diagnosed with a venous leg ulcer, which is managed with dressings and compression bandaging.
About 1% of the adult population in Westernised countries are affected by venous ulcers on the leg or foot.2 The prevalence increases with age to 1.7% in
Read Also: How To Cure Mouth Ulcer Permanently
Types Of Compression Therapy
Compression therapy can speed up wound healing, as well as reduce swelling and pain. This type of therapy may be needed for months until the wound is fully healed. Ongoing use of compression therapy can also reduce the risk that an ulcer will come back.
Several types of compression therapy are available, including:
- Inelastic. This increases pressure on the wound while a person is walking or contracting the leg muscles, but not while at rest. The most common type of inelastic compression therapy is a moist bandage which hardens after drying. Because it is stiff, the dry bandage will not change when the size of the leg changes, which can be uncomfortable.
- Elastic. This type of compression therapy increases pressure on the wound both while moving and at rest. Both compression stockings and bandages can be used for this. Unlike inelastic compression therapy, this type can be removed at night, washed and easily replaced.
- Intermittent pneumatic compression. With this therapy, a pump is used inflate and deflate sleeves on the foot or leg. As the sleeve inflates, the pressure increases. Because the equipment is expensive and bulky, it is more commonly used for patients who are bedridden.
Who Gets Stasis Ulcers
Stasis ulcers affect 1% of the population, so they are not uncommon. A variety of medical problems and lifestyle factors have been linked to their development. These include:
- Increasing age
- Previous deep venous thrombosis
- Obesity
- Lower limb fracture, surgery or injury
- Immobility
- Standing upright for long periods
- Multiple previous pregnancies
Stasis ulcers account for at least 4050% of chronic lower limb ulcers and contribute to a further 20% of mixed arterial and venous ulcers.
Also Check: Why Do I Have Ulcerative Colitis
Evaluation Of Venous Ulcers
Venous ulcers are large and irregularly shaped with well-defined borders and a shallow, sloping edge. Slough with granulation tissue comprises the base of the wound, with moderate to heavy exudate. Patients typically experience no pain to mild pain in the extremity, which is relieved with elevation. Venous ulcers are most frequently located on the lower legs, such as above the lateral or medial malleolus with a medial and circumferential presentation.
Common symptoms include edema that worsens throughout the day, pruritus, pain that improves with elevation, and heaviness of the affected limb. Assessment frequently finds abnormally dilated veins around the foot and ankle, atrophic white scarring, and an inverted champagne bottle appearance of the extremity.
Are Other Venous Ulcer Treatments Available
Venous ulcers that are severe or not responding to standard therapies may require additional treatments such as:
- Growth factor therapy, injectable substances that attract healthy cells to ulcers.
- Hyperbaric oxygen therapy, a treatment in which you sit in a special, pressurized chamber and inhale pure oxygen.
- Lymphedema therapy, massage, skin care and bandaging techniques that clear fluid buildup.
- Skin graft, replacing diseased skin with healthy skin from another part of your body.
- Stem cell therapy, injections of bone marrow to generate healthy tissue.
- Venous disease treatment to correct blood pooling problems and improve circulation.
You May Like: Homeopathic Medicine For Ulcerative Colitis
Venous Insufficiency And Venous Ulcers
Venous insufficiency, also called venous reflux, is a debilitating leg issue in which the blood cant flow up through the veins toward the heart. Healthy veins contain a number of specialized, one-way valves that open to allow blood to flow upward and close to prevent blood from flowing back down. When these valves are damaged or malfunctioning, venous insufficiency occurs.
As the valves deteriorate, the blood flows backwards and increases the pressure in the vein, dilating it. Blood stagnates, or pools, in the veins of the lower legs, putting pressure on the venous wall and causing inflammation and discomfort.
In many patients, untreated superficial venous reflux leads to the deposition of red blood cells in the tissues. Hemoglobin, the protein in red blood cells that carries oxygen, and hemosiderin, the accumulation of iron from the breakdown of hemoglobin , leaves deposits in the skin in the form of dark staining.
In severe cases, chronic, untreated venous insufficiency can cause open sores to develop on the skin, known as venous ulcers. These ulcers occur at the site where blood pools, due to the swelling that prevents the movement of nutrients and oxygen to the tissues.
Venous insufficiency can also cause varicose veins, a condition in which the superficial veins, or the veins closest to the surface of the leg, enlarge, twist, or bulge. In addition to being unsightly, varicose veins can cause pain, discomfort, or the development of venous ulcers.
Foam Dressings For Venous Leg Ulcers
Venous leg ulcers are a common and recurring type of chronic wound. Compression therapy is used to treat venous leg ulcers. Dressings that aim to protect the wound and provide a moist environment to aid ulcer healing are applied beneath compression devices. Foam dressings are one of several types of dressing available. We evaluated the evidence from 12 randomised controlled trials that either compared different types of foam dressings, or compared foam dressings with other types of wound dressings. We found no evidence to suggest that polyurethane foam dressings are significantly better or worse than hydrocellular foam dressings in venous leg ulcer healing. Similarly, we found no evidence to suggest that foam dressings are significantly better or worse than other types of dressings , for the healing of venous leg ulcers. We found insufficient evidence to draw any conclusions regarding: adverse events, quality of life, costs, pain, or dressing performance. Overall, the current evidence is of low or unclear methodological quality. This limits the making of any specific recommendations regarding the use of foam dressings. Further, good quality evidence is required before definitive conclusions can be made regarding the role of foam dressings in the management of venous leg ulcers.
You May Like: Best Treatment For Stage 2 Pressure Ulcer
Read Also: Ulcerative Colitis Increased Risk Of Colon Cancer
How Soon After Treatment Will I Feel Better / How Long Does It Take To Recover From This Treatment
Vascular ulcers can take weeks or even months to heal under normal circumstances. However, if cared for properly including closely following the treatment plan provided to you wounds should heal faster than expected. Your provider can tell you what to expect based on your specific wound issue and can help you track your progress along the way.
Wound Dressing And Care
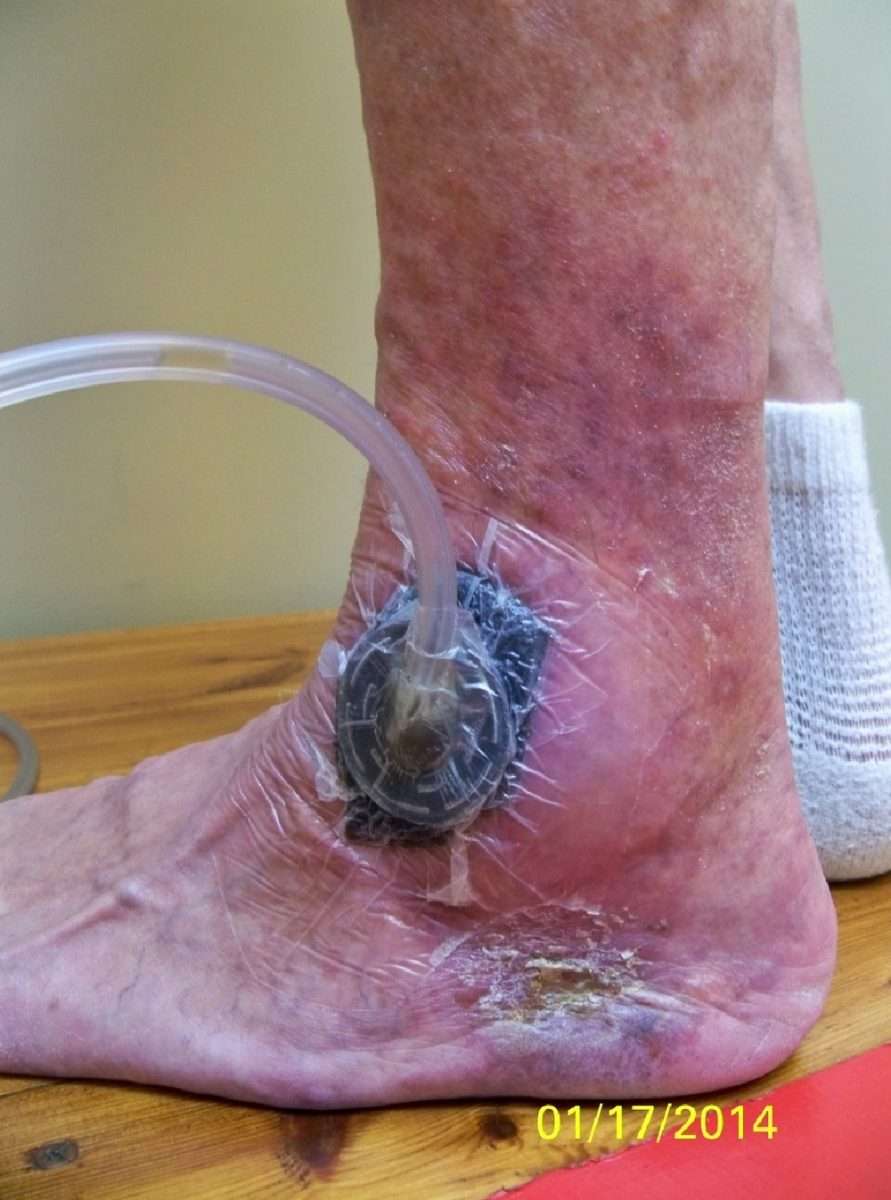
A venous leg ulcer is an open sore that can catch an infection from microbes very quickly. It is important to keep it clean at all times. Advanced Wound Care Dressings can help keep them free from infection as well as aid in faster wound healing. After dead tissue is removed and the wound is cleaned, it should be covered with a light, wound healing dressing. This can be easily done at home by following the instructions of a wound specialist regarding the method of cleaning and the number of dressings required.
Read Also: How To Get Rid Of Tongue Ulcers
Looking After Yourself During Treatment
The following advice may help your ulcer heal more quickly.
- Try to keep active by walking regularly. Sitting and standing still without elevating your legs can make venous leg ulcers and swelling worse.
- Whenever you’re sitting or lying down, keep your affected leg elevated.
- Regularly exercise your legs by moving your feet up and down, and rotating them at the ankles. This can help encourage better circulation.
- If you’re overweight, try to reduce your weight with a healthy diet and regular exercise.
- Stop smoking and moderate your alcohol consumption. This can help the ulcer heal faster.
- Be careful not to injure your affected leg, and wear comfortable, well-fitting footwear.
You may also find it helpful to attend a local healthy leg club, such as those provided by the Lindsay Leg Club Foundation, for support and advice.
Venous Leg Ulcers: 6 Things To Know When Treating Venous Disease
Lower extremity venous disease affects millions of Americans and may ultimately lead to open, draining wounds that adversely affect quality of life. However, there are exciting developments in early diagnosis, prevention and treatment of venous leg ulcers . On the treatment side, there are more choices now than ever before in compression products, which is greatly improving the patient experience. But proper treatment also comes from a better understanding of venous leg ulcers, and better understanding comes from more education. Luckily, were here to help provide education and support for you and your team, so here are six things to know when treating VLUs.
You May Like: Can Ulcers In The Colon Be Cancerous
Read Also: What Are Ulcers Caused From
Who Gets Foot And Toe Ulcers
Youre at higher risk for foot and toe ulcers if you are:
- Native American.
- Male.
- Elderly.
If you have an eye, kidney or heart disease related to diabetes, youre also at a higher risk. About 15% of people with diabetes will get an ulcer, typically on the bottom of their foot. Around 6% of that 15% will have to be hospitalized because of complications.
Youre also at a higher risk of getting foot and toe ulcers if you have any of the following:
- Problems with circulation.