Dr Alejandro Trujillo Rodriguez Cape Coral
Ulcerativecolitis is a type of inflammatory bowel disease. It’s caused by a malfunction in the body’s immune system. Normally, the immune system protects against bacteria and other foreign invaders. But in people with ulcerativecolitis, it mistakenly attacks the rectum and intestines, causing them to swell up and thicken. .
Your child was in the hospital because they have ulcerative colitis . This is swelling of the inner lining of the colon and rectum . It damages the lining, causing it to bleed. Ulcerative colitis is a form of inflammatory bowel disease and colitis, a disease of the colon , that includes… | Explore the latest full-text research PDFs, articles.
You were in the hospital because you have ulcerativecolitis. This is a swelling of the inner lining of your colon and rectum . It damages the lining, causing it to bleed or ooze mucus or pus. You probably received fluids through an intravenous tube in your vein. You may have received a blood transfusion.
2022. 8. 4. ·You were in the hospital because you have ulcerative colitis. This is a swelling of the inner lining of your colon and rectum . It damages the lining,. Questions? Call: 228-3344. Questions? Call: 402-228-3344.
When To Get Medical Advice
You should see a GP as soon as possible if you have symptoms of ulcerative colitis and you have not been diagnosed with the condition.
They can arrange blood or stool sample tests to help determine what may be causing your symptoms.
If necessary, they can refer you to hospital for further tests.
If you have been diagnosed with ulcerative colitis and think you may be having a severe flare-up, contact a GP or your care team for advice.
You may need to be admitted to hospital.
If you cannot contact your GP or care team, call NHS 111 or contact your local out-of-hours service.
When To Contact A Doctor
A person living with UC should talk with their doctor if they notice symptoms associated with sacroiliitis, such as pain in the hips when walking or any other types of arthritis. A primary care physician may refer a person to a rheumatologist for diagnosis.
A person may want to consider a second opinion if their doctor does not refer them to a rheumatologist. Early referrals can help improve treatment outcomes. However, referral rates are low, according to a 2018 study .
If symptoms get worse during treatment or do not improve, a person should talk with a healthcare professional. A doctor can recommend additional therapies that may help improve symptoms of either UC or sacroiliitis.
As a person begins to better manage their UC symptoms, they will often notice an improvement in their sacroiliitis symptoms, too.
Don’t Miss: What Foods To Avoid With Ulcerative Colitis
What Is The Best Diet For Ulcerative Colitis
Theres no single diet that works best for ulcerative colitis. If the disease damages the lining of the colon, your body might not absorb enough nutrients from food. Your healthcare provider may recommend supplemental nutrition or vitamins. Its best to work with your provider and nutritionist to come up with a personalized diet plan.
Can I Get Surgery For My Ulcerative Colitis
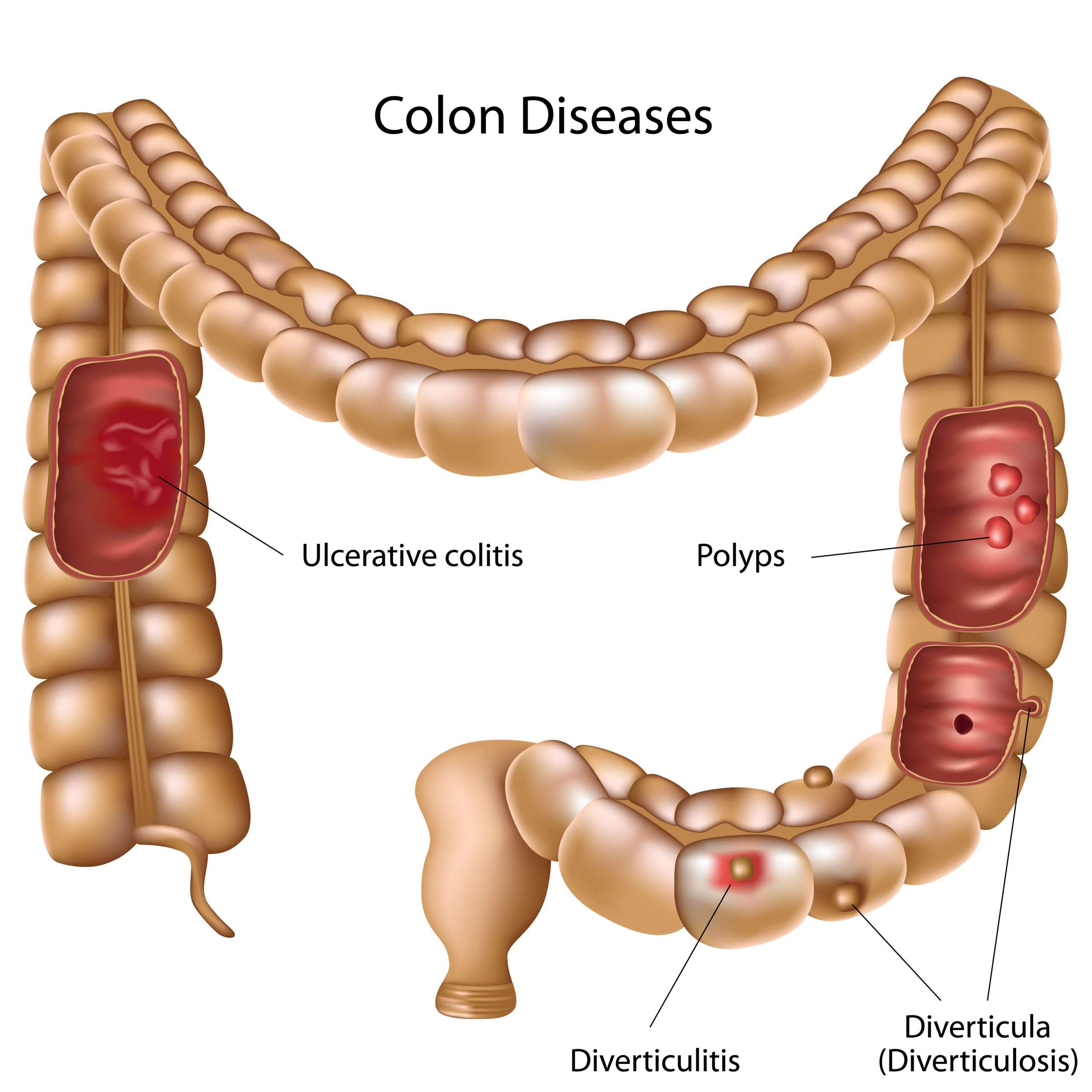
Surgery is an option if medications arent working or you have complications, such as bleeding or abnormal growths. You might develop precancerous lesions, or growths that can turn into colorectal cancer. A doctor can remove these lesions with surgery or during a colonoscopy.
Research shows that about 30% of people with ulcerative colitis need surgery sometime during their life. About 20% of children with ulcerative colitis will need surgery during their childhood years.
There are two kinds of surgery for ulcerative colitis:
Proctocolectomy and ileoanal pouch
The proctocolectomy and ileoanal pouch is the most common procedure for ulcerative colitis. This procedure typically requires more than one surgery, and there are several ways to do it. First, your surgeon does a proctocolectomy a procedure that removes your colon and rectum. Then the surgeon forms an ileoanal pouch to create a new rectum. While your body and newly made pouch is healing, your surgeon may perform a temporary ileostomy at the same time. This creates an opening in your lower belly. Your small intestines attach to the stoma, which looks like a small piece of pink skin on your belly.
After you heal, waste from your small intestines comes out through the stoma and into an attached bag called an ostomy bag. The small bag lies flat on the outside of your body, below your beltline. Youll need to wear the bag at all times to collect waste. Youll have to change the bag frequently throughout the day.
Recommended Reading: What Is Stomach Ulcer Pain Like
How Is Ulcerative Colitis Diagnosed
Colitis shares many symptoms with other common conditions, such as Crohns disease, irritable bowel syndrome, gastroenteritis and coeliac disease. Your doctor will examine you and take a detailed history of your symptoms to help rule these out.
There is no single test that can be used to diagnose UC, so a combination of tests is usually required:
- Blood tests help to rule out other medical conditions, and certain markers in the blood can indicate that inflammation is present.
- A stool sample may find other possible causes of diarrhoea and inflammation, such as an infection.
- A colonoscopy may be performed, where a thin, flexible tube that contains a tiny camera looks inside the bowel for ulcers, inflammation and bleeding.
- A biopsy may be taken from inside the bowel so a pathologist can examine it under a microscope to look for signs of disease.
Other types of imaging are sometimes used to help in the diagnosis and to help rule out other diseases.
Read Also: Mouth Ulcer Vitamin B Complex
Dietary And Lifestyle Modifications
As most nutrients are absorbed higher up in the digestive tract, those with ulcerative colitis generally do not have nutrient deficiencies however, other factors might influence your nutritional state. Disease symptoms may cause food avoidance, leading to food choices that might not provide a balanced diet. If bleeding is excessive, problems such as anemia may occur, and modifications to the diet will be necessary to compensate for this.
Generally, better overall nutrition provides the body with the means to heal itself, but research and clinical experience show that diet changes alone cannot manage this disease. Depending on the extent and location of inflammation, you may have to follow a special diet, including supplementation. It is important to follow Canadas Food Guide, but this is not always easy for individuals with ulcerative colitis. We encourage you to consult a registered dietitian, who can help set up an effective, personalized nutrition plan by addressing disease-specific deficiencies and your sensitive digestive tract. Some foods may irritate the bowel and increase symptoms even though they do not worsen the disease.
In more severe cases, it might be necessary to allow the bowel time to rest and heal. Specialized diets, easy to digest meal substitutes , and fasting with intravenous feeding can achieve incremental degrees of bowel rest.
Recommended Reading: Can You Eat Oatmeal With Ulcerative Colitis
Don’t Miss: What Can You Eat With A Peptic Ulcer
What Should You Eat When You Have Ulcerative Colitis
When it comes to food, theres no known dietary cause of ulcerative colitis, but different foods may aggravate or help limit symptoms of the disease.
Youre more likely to need to change your diet during periods of active disease , when eating soft, bland foods can help limit symptoms like cramping and diarrhea. With guidance from a doctor, a liquid meal replacement diet known as an elemental diet, can also help achieve remission from active disease.
During flares, you may also want to avoid or limit high-fiber and high-fat foods, as well as alcohol, dairy products, and spicy foods.
If youre losing nutrients and water in your diet due to diarrhea, you may need to focus on increasing your fluid intake and getting enough calories, protein, vitamins, and minerals from foods or supplements.
Editors Picks
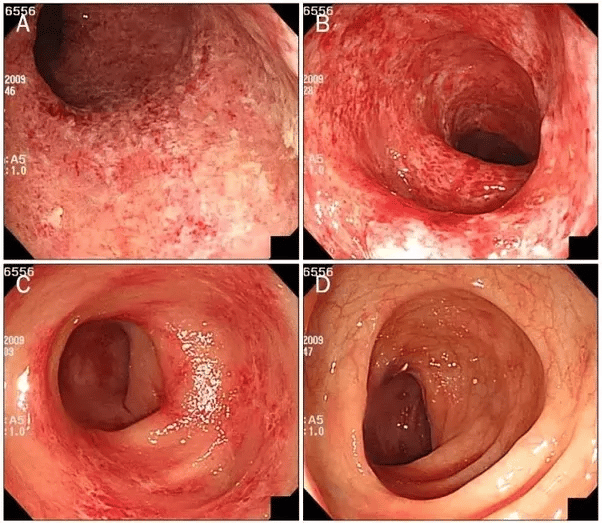
Correlation Between Disease Activity And Endoscopic Findings
There was a consensus that endoscopic findings would usually affirm patients own assessment of their level of disease activity.
Testing has always been pretty much a confirmation of how Im feeling at the time.
The colonoscopy reports and photos are basically, well, heres what this looks like and this looks like and heres the issue. So, theyre pretty in synch.
You May Like: Ulcer And High Blood Pressure
Living With Uc: Diet Changes
Diet doesn’t cause ulcerative colitis, but some foods may make your symptoms worse. Common ones include dairy, fatty foods, and foods with too much fiber, which can trigger diarrhea. It can help to keep a journal of what you eat and any symptoms you have. Look for links and avoid triggers. If you lose a lot of weight, you may need to work with a dietitian to come up with a healthy diet.
What Causes Ulcerative Colitis
The exact cause isn’t clear. But researchers think your immune system — which defends you from germs — is involved. When you have UC, your immune system may not react like it should to bacteria in your digestive tract. Doctors aren’t sure whether this triggers the condition or results from it. Stress and your diet can make your symptoms worse, but they don’t cause ulcerative colitis.
Don’t Miss: What Foods Should You Avoid If You Have Ulcerative Colitis
Ulcerative Colitis Vs Crohns Disease Vs Irritable Bowel
Other gut diseases can have some of the same symptoms.
- Ulcerative colitis affects only your large intestine and its lining.
- Crohnâs disease causes inflammation, but it affects other places in your digestive tract.
- Irritable bowel syndrome has some of the same symptoms as UC, but it doesnât cause inflammation or ulcers. Instead, itâs a problem with the muscles in your intestines.
Recommended Reading: Is Aloe Vera Good For Ulcerative Colitis
Food As Trigger Of Flare
Participants frequently discussed the possibility that certain foods could trigger flares, but had great difficulty in identifying common themes across participants.
I never could figure out what triggers it. When Ive got a flareup going, I mean, its always, I eat, and then half an hour later Im in the bathroom.
I know until I kept a food journal, I had no concept of what would or wouldnt trigger it. I just its hard to isolate.
Don’t Miss: Ulcerative Colitis And Anxiety Attacks
Its Time For Some Potty Talk Because What You Find In Your Toilet Bowl Can Reveal A Lot About Your Uc
by Health Writer
Consistency, liquidity, shape, smell, frequency. Whether or not youre living with , chances are those words immediately make you think about poop. But if you do have UC, an inflammatory bowel disease that causes painful intestinal cramping and frequent bathroom runs, those five worlds just might be your mantra.
Everybody poops, but anyone with IBD can attest to how big of a role bowel movements can play in daily life. Truth is, your poopand how often nature callscan reveal a lot about your disease and whether a flare of your worst is on the horizon. So much so that its worth taking a look in the toilet bowl every now and then.
Here, we talk to top poop experts, who break down what your bodys waste can reveal.
How Is Acute Bacterial Dysentery Differentiated From Acute Onset Of Ischemic Colitis
The degree of bloody diarrhea is variable in patients with ischemic colitis, and it may be difficult to distinguish between the two diseases. Clinically, the patient with ischemic colitis complains of sudden-onset abdominal pain, and an acute abdominal series may show thumbprinting of the colonic mucosa.
Flexible sigmoidoscopy is the mainstay of diagnosis for ischemic colitis. The rectum is usually spared because of its collateral blood flow. Above the rectum, the mucosa becomes friable and edematous, and there may be hemorrhagic areas and ulcerations resembling those of Crohns disease. Angiography is not generally helpful in the evaluation of ischemic colitis ischemic colitis is a small-vessel disease compared with mesenteric midgut ischemia of the small bowel, which involves thrombosis or embolism in the superior mesenteric artery . A barium enema is contraindicated in patients with suspected ischemic colitis, because colonic expansion during barium instillation may promote further ischemia.
Glenn T. Furuta, in, 2004
Also Check: How To Tell If I Have Stomach Ulcer
How Is Ulcerative Colitis Diagnosed In A Child
Your child’s healthcare provider will ask about your child’s health history. He or she will also give your child an exam.
Your child will have blood tests. These tests can tell if your child has anemia. They can also tell if your child has a high white blood cell count. This can be a sign of inflammation. Your childs healthcare provider may also do other tests.
Key Points About Ulcerative Colitis In Children
-
Ulcerative colitis is an inflammatory bowel disease. In this condition, the inner lining of your childs large intestine and rectum gets inflamed.
-
This inflammation causes diarrhea or frequent emptying of the colon. Your child may also have stomach pain and diarrhea.
-
Treatment may include avoiding foods that cause symptoms, taking medicine, and having surgery.
-
Children with this condition need long-term care. Your child may have times when symptoms go away. But symptoms usually come back.
You May Like: How To Heal Mouth Ulcers
Will Ulcerative Colitis Affect Me Over Time
The effects of ulcerative colitis vary considerably from person to person, based on the nature and severity of their disease. In many cases, the condition does not have much impact on daily life, the ability to work or to enjoy an active social life but does take some getting used to. When it is at an active stage, symptoms such as diarrhoea and abdominal pain often require time away from work, college etc. and can make it difficult to cope going out or even being at home. However, treatment usually makes the symptoms better within days or weeks so normal quality of life can be restored quite quickly. Some severe cases of ulcerative colitis, however, can have a significant impact on peoples lives. This can be due to a weak response to treatment which makes symptom-free remission difficult to achieve and can involve frequent flare ups.
What Role Does Diet And Nutrition Play In Ulcerative Colitis
Diet does not cause the development of ulcerative colitis nor can any special diet cure the disease. However, the foods you or your child eat may play a role in managing symptoms and lengthening the time between flareups.
Some foods may make symptoms worse and should be avoided, especially during flareups. Foods that trigger symptoms are different from person to person. To narrow down what foods affect you, keep track of what you eat each day and how you feel afterward .
Problem foods often include:
- High sugar foods and drinks.
- Carbonated beverages.
- High-fiber foods.
In addition to the problem foods listed above, infants, children and teenagers can also experience issues with:
- Dairy products.
Keep a careful eye on your childs diet and nutrition. Their appetite may decrease during a flareup and they might not eat enough to stay healthy, and grow. Also, the inflammation caused by ulcerative colitis may keep their digestive tract from absorbing enough nutrients. This can also affect your childs health. For these reasons, you may have to increase the amount of calories your child consumes.
Its best to work with your provider and nutritionist to come up with a personalized diet plan if you or your child has ulcerative colitis.
Don’t Miss: Ulcerative Colitis And Lower Back Pain
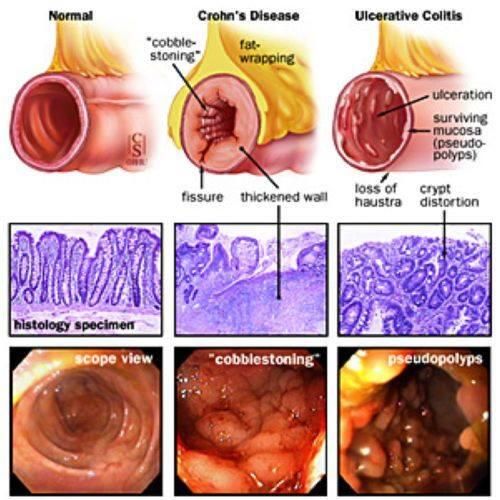
How Is Ulcerative Colitis Different From Crohns Disease
Ulcerative colitis is different from other inflammatory bowel diseases like Crohns disease. Crohns can affect any area of the gastrointestinal tract, including the small intestine and colon. Ulcerative colitis, on the other hand, affects only the colon. The inflammation involves the entire rectum and extends continuously up the colon. There are no normal areas of the intestine between the areas of ulceration. In Crohns, the inflamed areas are scattered and can affect the entire thickness of the bowel wall.
Vitamin And Mineral Supplements For Ibd
A person with IBD who eats a healthy, varied diet does not usually need to take vitamin supplements. But if they have a dietary deficiency, they may need tablets or occasional vitamin B12 injections. For example, a person on a low-fibre diet may need extra vitamin C and folic acid because they dont eat enough fruit and vegetables.A person with Crohns disease who experiences steatorrhoea may need calcium and magnesium supplements. Most children with IBD should take supplements to help them grow and develop normally.
You May Like: What Is Peptic Ulcer Pain Like
Feeling Comfortable With Your Doctor
Its not always easy to talk about your bowel habits. Talking about poop can be embarrassing, and many people may not be ready to open up to their doctor about it.
Others may ignore the changes to their stool or think that nothing is wrong. However, ignoring symptoms will only make things worse.
Your doctor has studied the gastrointestinal tract along with all that it does and produces. They have seen and heard it all. Nothing you say about your bowel symptoms is going to offend or shock them.
Its part of their job to know about any changes in your symptoms. Your doctor is there to help you, not to judge you.
You dont have to know any fancy medical terms when talking with your doctor about your symptoms. Share your concerns and any changes in your bowel habits you have noticed. Talking with them about changes in your stool can only help get you closer to resolving the problem.