Assessment Of Nutritional Needs
Undernutrition is common among patients with pressure injuries and is a risk factor for delayed healing. Markers of undernutrition include albumin < 3.5 g/dL or weight < 80% of ideal. Protein intake of 1.25 to 1.5 g/kg/day, sometimes requiring oral, nasogastric, or parenteral supplementation, is desirable for optimal healing. Current evidence does not support supplementing vitamins or calories in patients who have no signs of nutritional deficiency.
Description Of The Condition
Pressure ulcers are an internationally recognised patient safety problem, estimated to affect 2.5 million people annually . The development of pressure ulcers in any patient is a serious complication resulting in pain, decreased quality of life and significant expenditure of both time and money for the healthcare industry . Also known as pressure injury, pressure sores, decubitus ulcers, or bedsores, pressure ulcers are a localised injury to the skin, underlying tissue, or both, usually occurring over a bony prominence, as a result of pressure, or pressure in combination with shear stress .
The main factors associated with the development of pressure ulcers are exposure of the skin to excessive pressure, and a reduced tolerance of the skin to pressure. Pressure is exerted on the skin, soft tissue, muscle, and bone by the weight of an individual or a device applied against the surface. Tissue tolerance is the ability of the skin and its supporting structures to tolerate the effects of pressure by distributing it and by the transfer of pressure loads from the skin surface to the skeleton . Tissues are capable of withstanding enormous pressures briefly, but prolonged exposure to pressure initiates a series of events that potentially leads to necrosis and ulceration of tissue.
When Should I Call The Doctor
If you suspect you have a pressure injury, speak with your doctor. A pressure injury is easier to heal if it is discovered in the early stages. It is important to prevent a wound from becoming infected. Healing is delayed in an infected wound and the infection could cause problems in other areas of the body.
Read Also: First Signs Of Ulcerative Colitis
How Can Pressure Injuries Be Prevented
The development of pressure injuries can be prevented through careful observation of the skin and frequent repositioning in those who canât turn themselves. Tips to prevent pressure injuries include:
- Keeping the skin clean and clear of bodily fluids.
- Moving and repositioning the body frequently to avoid constant pressure on bony parts of the body.
- Using foam wedges and pillows to help relieve pressure on bony parts of the body when turned in bed.
- Maintaining a healthy diet to avoid malnutrition and to assist in wound healing.
What Types Of Wound Dressing Can Be Used On Bed Sores
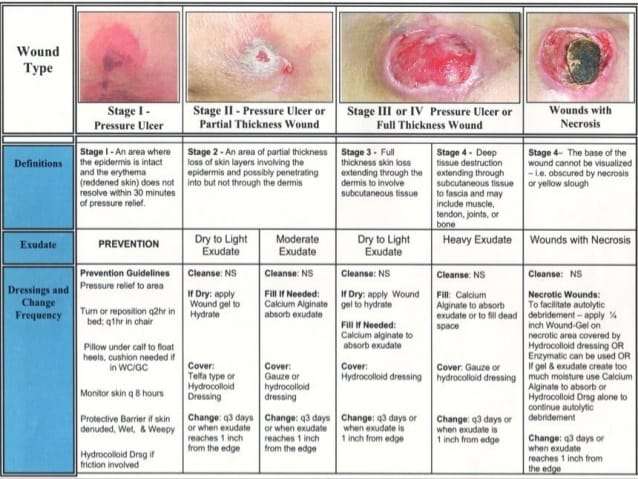
By Nursing Home Law Center
In order for bed sores to heal, attention must be paid to the removing dead tissue and protecting the wound from infection causing bacteria. Dressings are usually applied to help the body heal itself. The type of dressing and the frequency with which it is to be changed is ordered by a physician with the application and changes carried out by nurses.
Many patients with bed sores suffer additional harm when the staff responsible for caring for them fails to follow medical orders with respect to the frequency with which dressings are to be changed. If dressings are not changed according to orders set forth by a physician, the healing of the bed sores may be delayed and perhaps become infected.
The most commonly used dressings used to treat bed sores include:
Absorptive Dressings: These dressings are either applied directly to the wound or on top of other primary dressings. Absorptive dressings are intended to remove the drainage from the bed sore that may impede healing. Most absorptive dressings are changed on a daily basis. However, excessive drainage from a bed sore may require more frequent dressing changes.
Common types of Absorptive dressings include: Medipore, Silon Dual Dress, Aquacel Hyrofiber Combiderm, Absorbtive Border, Multipad Soforb, Iodoflex, Tielle, Telefamax, Tendersorb, Mepore and Exu-dry.
Call Toll-Free for a No Obligation ConsultationCall Toll-Free for a No Obligation Consultation
Related Information
Also Check: How To Heal Stage 4 Pressure Ulcer
Appendix 2 Glossary Of Nma Terms
Armspecific outcomes/armlevel data: raw outcome data or risk) for each arm of the trial .
Assumptions for NMA: in common with all metaanalysis, the true treatment effect across trials is assumed to be described by a fixedeffect or randomeffects model. Additionally, transitivity is assumed and, concurrently, exchangeability and consistency.
Baseline risk: the absolute risk of the outcome in the ‘control’ group. This is affected by the presence of prognostic factors. Some authors have used the baseline risk as a proxy effect modifier, but in general the effect estimate is independent of the baseline risk on the other hand, the absolute risk difference depends on baseline risk.
Bayesian approach: the explicit quantitative use of external evidence in the design, monitoring, analysis, interpretation of a healthcare evaluation. In the Bayesian paradigm, prior beliefs about parameters in the models are specified and factored into the estimation. Posterior distributions of model parameters are then derived from the prior information and the observed data. In NMA, it is common to use noninformative priors for effect estimates.
Coherence/consistency: the direct effect estimate is the same as the sum of the indirect effect estimates.
Contrast/comparison/studylevel data: outcome data for the comparison .
Credible interval : the 95% credible interval is the range within which the mean value lies with posterior probability of 95%.
Studylevel data: see contrast.
Analysis
Nursing Home Abuse & Neglect Resources
Common Cases:
Client Reviews
Nursing Home Law Center, LLC is not a law firm. It is an organization that concentrates solely on helping provide nursing home patients and their families the legal help they need. NHLC LLC has a network of recognized attorneys located across the country who have experience representing clients in all types of nursing home injury cases. References to “NHLC attorneys” or “our attorneys” are references to attorneys within NHLC’s network, and not employees, agents, or partners of NHLC. Please consult the disclaimer page for further information concerning NHLC. All information on this site shall be considered ‘attorney advertising’ and not construed as legal advice. Prior case results should not be relied on when retaining a lawyer.
Also Check: Turkey Tail Mushroom For Ulcerative Colitis
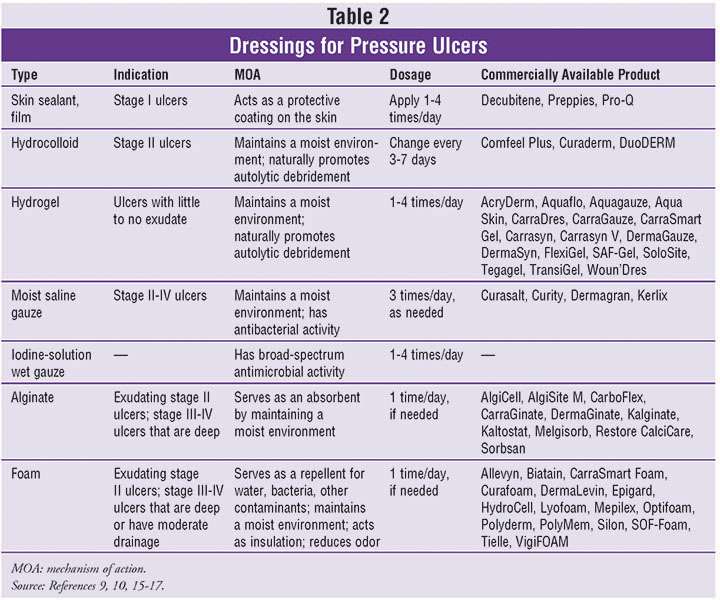
Alginate Dressings For Treating Pressure Ulcers
What are pressure ulcers, and who is at risk?
Pressure ulcers, also known as bedsores, decubitus ulcers and pressure injuries, are wounds involving the skin and sometimes the tissue that lies underneath. Pressure ulcers can be painful, may become infected, and so affect people’s quality of life. People at risk of developing pressure ulcers include those with spinal cord injuries, and those who are immobile or who have limited mobility – such as elderly people and people who are ill as a result of short-term or long-term medical conditions.
In 2004 the total annual cost of treating pressure ulcers in the UK was estimated as being GBP 1.4 to 2.1 billion, which was equivalent to 4% of the total National Health Service expenditure. People with pressure ulcers have longer stays in hospital, and this increases hospital costs. Figures from the USA for 2006 suggest that half a million hospital stays had ‘pressure ulcer’ noted as a diagnosis the total hospital costs of these stays was USD 11 billion.
Why use alginate dressings to treat pressure ulcers?
Dressings are one treatment option for pressure ulcers. There are many types of dressings that can be used these can vary considerably in cost. Alginate dressings are a type that is highly absorbant and so can absorb the fluid that is produced by some ulcers.
What we found
This plain language summary is up-to-date as of June 2014.
Causes Of Pressure Ulcers
Pressure ulcers are caused by sustained pressure being placed on a particular part of the body.
This pressure interrupts the blood supply to the affected area of skin. Blood contains oxygen and other nutrients that are needed to help keep tissue healthy. Without a constant blood supply, tissue is damaged and will eventually die.
The lack of blood supply also means that the skin no longer receives infection-fighting white blood cells. Once an ulcer has developed, it can become infected by bacteria.
People with normal mobility do not develop pressure ulcers, as their body automatically makes hundreds of regular movements that prevent pressure building up on any part of their body.
For example, you may think that you are lying still when asleep, but you may shift position up to 20 times a night.
Pressure ulcers can be caused by:
- pressure from a hard surface such as a bed or wheelchair
- pressure that is placed on the skin through involuntary muscle movements such as muscle spasms
- moisture which can break down the outer layer of the skin
The time it takes for a pressure ulcer to form will depend on:
- the amount of pressure
- how vulnerable a person’s skin is to damage
Grade 3 or 4 pressure ulcers can develop quickly. For example, in susceptible people, a full-thickness pressure ulcer can sometimes develop in just 1 or 2 hours. However, in some cases, the damage will only become apparent a few days after the injury has occurred.
You May Like: How Do You Prevent Pressure Ulcers
How Are Pressure Injuries Treated
Pressure injuries can be treated in many ways depending on the stage. Once the stage and severity of the wound is determined, it must be cleaned, usually with a saline solution. After the wound is cleaned, it needs to be kept clean, moist, and covered with an appropriate bandage. There are several different types of bandages your doctor may use to dress the wound. These include:
- Water-based gel with a dry dressing
- Foam dressing
- Hydrocolloid dressing
- Alginate dressing
Sometimes debridement is needed. This is a process of ridding the wound of dead tissue. Debridement is an important part of the healing process. It changes the wound from a long-lasting one to a short-term wound. There are several types of debridement. These methods include:
- Ultrasound: Using sound waves to remove the dead tissue.
- Irrigation: Using fluid to wash away dead tissue.
- Laser: Using focused light beams to remove the dead tissue.
- Biosurgery: Using maggots to eliminate bacteria from the wound.
- Surgery: Using surgery to remove the dead tissue and close the wound.
- Topical: Medical-grade honey or enzyme ointments.
Contributions Of Editorial Base:
Nicky Cullum: edited the protocol advised on methodology, interpretation and protocol content. Approved the final protocol prior to submission. Sally BellSyer: coordinated the editorial process. Advised on methodology, interpretation and content. Edited the protocol. Ruth Foxlee: designed the search strategy and edited the search methods section.
You May Like: What Not To Eat With An Ulcer
Thin Flexible And Versatile
Designed to reduce the risk of further skin breakdown due to friction.
DuoDERM® Extra Thin Dressing can be used as a primary hydrocolloid dressing for dry to lightly exuding wounds.
It can be used as a secondary dressing to secure an AQUACEL® Dressing or an AQUACEL® Ag Dressing.
The European Pressure Ulcer Advisory Panel and The National Pressure Ulcer Advisory Panel guidelines recommend the usage of hydrocolloids for the management of pressure ulcers.1
DuoDERM® Extra Thin Dressing can be used to manage stage I and stage II pressure ulcers.
Overall Completeness And Applicability Of Evidence
The network is sparse, in terms of the total number of participants, the total number of wounds healed, the number of studies per contrast, the size of the constituent studies and the duration of followup: 21 of 27 direct contrasts were informed by only one study and the average number of events per mixed treatment contrast was around four. The median study size was 41 and several studies had zero events. The duration of followup was relatively short for most studies : only 3/39 studies in the network had a followup duration of 16 weeks or more.
In parallel we conducted a second NMA, grouping together some classes of dressings. We had hoped that the group network would provide more power in the analysis, but in practice too many data were excluded from the network, and the network was also unbalanced, being dominated by the advanced dressing versus basic dressing contrast, which involved about 55% of the participants in the group network. The group network provided equally uncertain evidence and the findings are not discussed further here, but are reported in Appendix 5 for the interested reader.
Read Also: What Should I Eat If I Have An Ulcer
Treating And Preventing Pressure Ulcers
Treatment for pressure ulcers includes the use of dressings, creams and gels designed to speed up the healing process and relieve pressure. Surgery is sometimes recommended for the most serious cases.
For some people, pressure ulcers are an inconvenience that require minor nursing care. For others, they can be serious and lead to life-threatening complications, such as blood poisoning or gangrene.
Read more about the complications of pressure ulcers.
Pressure ulcers can be unpleasant, upsetting and challenging to treat. Therefore, a range of techniques is used to prevent them developing in the first place. These include:
- regularly changing a person’s position
- using equipment to protect vulnerable parts of the body such as specially designed mattresses and cushions
Read about treating pressure ulcers and preventing pressure ulcers for more information.
Unfortunately, even with the highest standards of care, it’s not always possible to prevent pressure ulcers in particularly vulnerable people.
Agreements And Disagreements With Other Studies Or Reviews
We have been unable to identify any network metaanalyses directed at healing pressure ulcers and incorporating both dressings and topical agents. The AHRQ guideline reviewed the evidence for dressings in a series of pairwise comparisons and stated that overall, they did not find substantial evidence to support certain local wound applications over others . The most recent NICE guideline on the prevention and management of pressure ulcers considered all RCT evidence on dressings and separately all RCT evidence on topical agents. NICE recommendations are to not use saline gauze dressings and for the health professional and adult to discuss the type of dressing to use, taking into account pain and tolerance, position of the ulcer, amount of exudate and frequency of dressing change. These recommendations rely heavily on consensus decisions, weakly supported by the evidence, and as such, agree with the findings of this review.
Also Check: Entyvio Dosing For Ulcerative Colitis
What Are The Stages Of A Pressure Injury
There are four stages that describe the severity of the wound. These stages include:
- Stage 1: This stage is discolored skin. The skin appears red in those with lighter skin tones and blue/purple in those with darker skin tones. The skin does not blanch when pressed with a finger.
- Stage 2: This stage involves superficial damage of the skin. The top layer of skin is lost. It may also look like a blister. At this stage, the top layer of skin can repair itself.
- Stage 3: This stage is a deeper wound. The wound is open, extending to the fatty layer of the skin, though muscles and bone are not showing.
- Stage 4: This stage is the most severe. The wound extends down to the bone. The muscles and bone are prone to infection, which can be life-threatening.
Summary Of Findings For The Main Comparison
NMA evidence for individual network: proportion with complete healing interventions versus saline gauze
1Majority of evidence at high risk of bias imprecision: very wide CI .2Imprecision: very wide CI .3Majority of evidence at high risk of bias imprecision: wide CI and direct evidence on collagenase from three studies, 11 events .4Majority of evidence at high risk of bias : imprecision: wide CI and direct evidence on dextranomer from one study, seven participants and four events .5Majority of evidence at high risk of bias imprecision: wide CI .6Majority of evidence at high risk of bias inconsistency: heterogeneity in direct evidence imprecision: wide CI .7Majority of evidence at high risk of bias inconsistency: significant difference between direct and indirect estimates imprecision: very wide CI .8Imprecision: wide CI .9Majority of evidence at high risk of bias : imprecision: wide CI and direct evidence on tripeptide copper gel from one study, six participants and five events .
In this section, we present the results for the individual NMA. Results for the group network are given in Appendix 5.
Interventions and comparisons
The individual network comprised 21 interventions: 13 eligible dressings six topical agents and two supplementary linking interventions .
Risk of bias for the individual network
We report risk of bias in three ways :
Network metaanalysis results
Ranking of treatments
Rankograms for each intervention individual network
Also Check: How To Heal Mouth Ulcers Quick
Symptoms Of Pressure Ulcers
The parts of the body most at risk of developing pressure ulcers are those that are not covered by a large amount of body fat and are in direct contact with a supporting surface, such as a bed or a wheelchair.
For example, if you are unable to get out of bed, you are at risk of developing pressure ulcers on your:
- shoulders or shoulder blades
- knees, ankles, heels or toes
- spine
- tail bone
If you are a wheelchair user, you are at risk of developing pressure ulcers on:
- your buttocks
- the back of your arms and legs
- the back of your hip bone
Bone And Joint Infection
Infection can also spread from a pressure ulcer into underlying joints and bones .
Both of these infections can damage the cartilage, tissue and bone. They may also affect the joints and limbs.
Antibiotics are required to treat bone and joint infections. In the most serious of cases, infected bones and joints may need to be surgically removed.
Recommended Reading: Exercising A Horse With Ulcers