Ulcerative Colitis Treatment: Medication
The most common medication option is anti-inflammatory drugs. These can be used orally or topically to reduce inflammation of the colon and rectum.
Treating ulcerative colitis is a highly individualized process. At Johns Hopkins, we tailor your treatment to your specific needs and alter the medication as necessary. Your specific medication regimen will depend largely on the severity of your condition.
Other medications include:
-
Immunosuppressive medications: These drugs slow your immune system to stop the immune response that is causing the colon and rectum to swell.
-
Biologics: Like immunosuppressive medications, biologics target the immune system, but biologics act on specific immune system proteins that encourage inflammation.
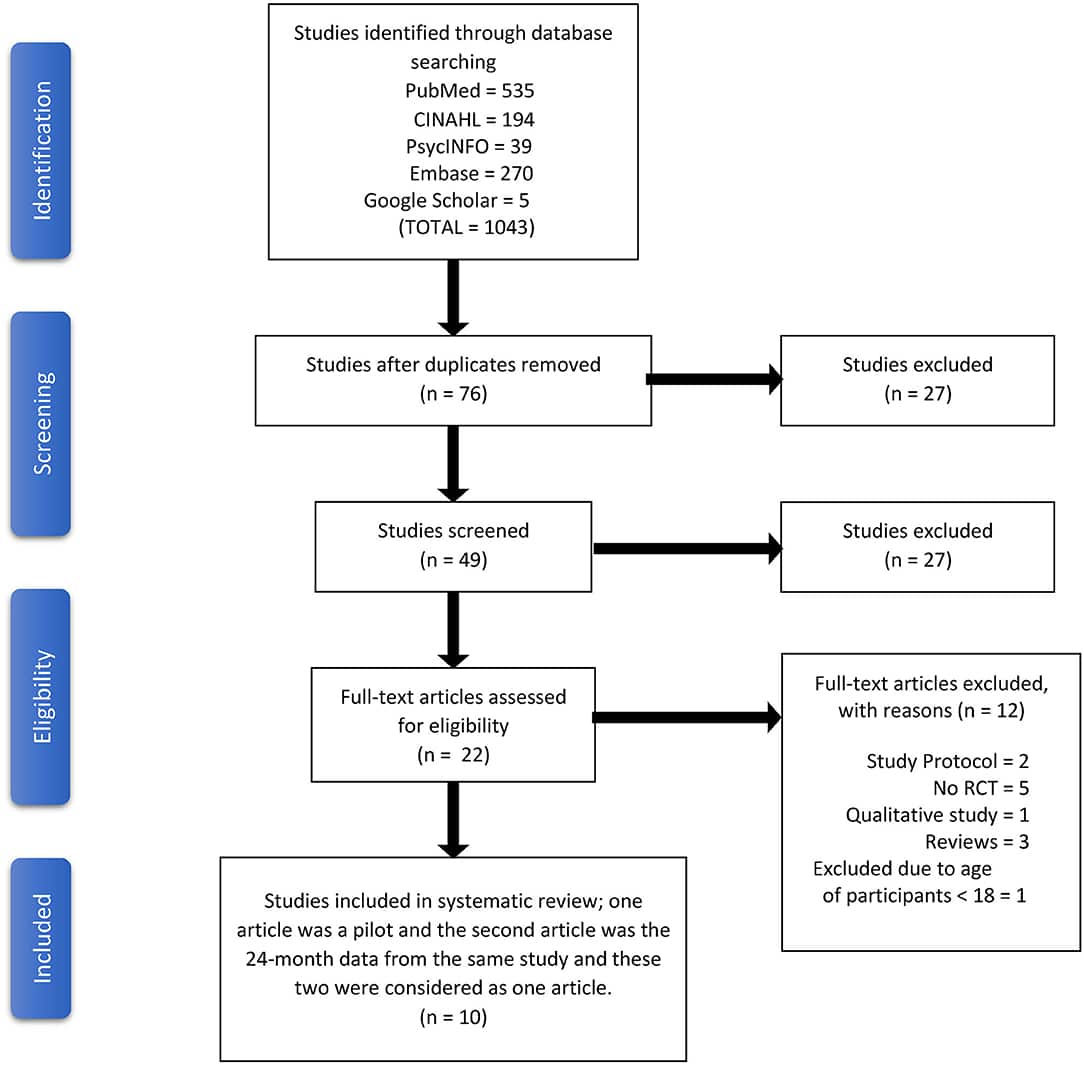
Characteristics Of Included Studies
All of the selected studies reported a control group. The design of these control groups varied among the studies. Four of the selected studies had waitlist control groups and two of them had attention control groups. Control group participants were taught about IBD and its management and the influence of stress on sleep, psychological and physical health was the subject for teaching by Jedel et al. . Three of the studies used standard care as the control group. Lastly, one study used a combination of attention control and waitlist control groups.
Twelve articles were excluded. Five were not RCTs . Two were study protocols . Three were reviews , along with one qualitative study and one study which included participants < 18 years of age .
All of the selected studies reported exclusion or inclusion criteria and included both men and women only one study was double-blinded . Three of the articles demonstrated adequate sample size by reporting the power analyses. Only one study informed the details of blinding procedures. Objectives, outcomes, details of the intervention, and statistical outcomes were clearly addressed in all studies. Sample sizes ranged from 11 to 51 in experimental groups and 1266 in control groups. The selected studies were from Spain, Australia, Netherlands, United Kingdom , New Zealand, Israel, United States , and Germany.
When To Get Treatment
An increase in inflammation causes a flare, and the nature of inflammation means that you should treat it as quickly as you can. Inflammation grows exponentially, because inflammation itself causes an increase in inflammation. The longer you leave it untreated, the worse it will get. In addition, untreated inflammation not only leads to the symptoms associated with ulcerative colitis, it can also increase your risk of developing complications such as colorectal cancer down the line. Pay attention to your symptoms, and visit your physician if you notice that they change or increase even a small amount.
Also Check: Over The Counter Medication For Ulcerative Colitis
Vitamin And Mineral Supplements
People with IBD often have vitamin or mineral deficiencies because digestive dysfunction prevents the body from absorbing important nutrients. These include iron, folate, vitamin D, and vitamin B12. As part of treatment at NYU Langone’s Inflammatory Bowel Disease Center, nutritionists may recommend dietary changes. They may also advise supplementing your diet with vitamins and minerals to boost your digestive health.
Management Of Active Uc
Symptoms of new onset UC or recurrent flare-ups usually consist of abdominal pain, bloody and/or mucous diarrhea. Severe cases present with weight loss, tachycardia, fever, anemia and bowel distension. Before starting medical treatment other etiologies of colitis/enteritis such as infections , toxic reactions , mesenteric ischemia or intestinal malignancies should be ruled out. Opportunistic infections need to be excluded prior to medical therapy escalation, especially in patients under immunosuppressive therapy with a corticosteroid-refractory course.
Although there is no gold standard, minimal diagnostic workup for UC includes medical history, clinical evaluation , full blood count, erythrocyte sedimentation rate , C-reactive protein , stool microbiology, ultrasound and endoscopy with mucosal biopsies. If there is any doubt about the diagnosis in the acute setting, endoscopic and histological confirmation should be repeated after a period of time has passed .
The choice of treatment depends on the degree of activity, distribution , course of disease, frequency of relapses, extraintestinal manifestations, previous medications, side-effect profile and the patient´s individual wishes.
Distribution patterns depend on the part of the colon involved and are designated according to the Montreal classification as proctitis , left-sided colitis or extensive colitis . A graphical treatment algorithm is shown in Figure Figure11.
You May Like: Signs Of Gastric Ulcers In Horses
Current Myths About Ulcerative Colitis
Oh boy there are some real doozies out there.
Foods donttrigger UC.
Just like you dont need a special diet to control UC.
Vegan, gluten, lactoseall BS.
The acid in your stomach is just below that of battery acid! Anything you digest will get processed by that acid. A piece of Wonder Bread loaded with gluten is not going to trigger UCit may give a sugar rush though
That acid though, is PRETTY caustic. That acid isnt too far from the colon. It can also attack the body..see where this is going?
Too much exercise doesnt cause it. In fact exercise is one of the best things to prevent it.
Before you start wasting money on special foods, read my treatment below.
Incorporate Cardiovascular Exercise Into Your Routine
Regular physical activity is good for all of us, but it has especially important benefits if you have IBD. Researchers have looked at the impacts of both walking and running if you have IBD, and both forms of exercise came out winners. Even walking just 30 minutes, at 60% of your effort, three times a week improved heart health, general well-being, quality of life, and perceived stress.
You May Like: Stomach Ulcer Pain Relief Medicine
Take Vitamins And Minerals
If you are living with IBD, you are at risk for micronutrient deficiencies such as calcium, vitamin D, B6, B9, iron, magnesium, and zinc. If you are not getting enough of these micronutrients, you may experience bone disease, cognitive decline, anemia, poor growth or other complications. Your doctor or dietitian can provide an assessment to let you know if you are deficient. You can go here for recommended vitamin and mineral replacement amounts.
Get Regular Exercise To Reduce Uc Inflammation
Snider says exercise is useful in managing many of the complications associated with ulcerative colitis, including decreased bone density, a weakened immune system, emotional health problems, stress, and weight gain.
“Try to engage in a moderate-intensity exercise like swimming or biking, three or four days per week,” he says. A review published in August 2016 in Pharmacological Reports noted that moderate exercise releases protective myokines such as irisin from working skeletal muscles, which promotes healing and helps with inflammatory bowel disease inflammation.
Snider also strongly recommends yoga as a natural treatment for ulcerative colitis, as it promotes relaxation and targets the digestive system, flooding the area with oxygen and nutrition for healing. Find what type and frequency of exercise works for you and take it slow: Too much exercise can cause mild systemic inflammation.
Research indicates that stress plays a role in inflammatory bowel diseases such as ulcerative colitis. Researchers analyzed data on 2,007 adults in a Swiss IBD study and found a relationship between depression and anxiety and disease symptoms. The results were published in June 2016 in Clinical Gastroenterology and Hepatology.
Counteract stress with relaxation techniques such as meditation, deep breathing, and progressive muscle relaxation to help your body relax.
You May Like: Is Ulcerative Colitis A Serious Disease
Synthesis Of Two Studies
Findings of three of the selected studies were synthesized narratively due to insufficient quantitative data for meta-analysis for the outcomes of anxiety and depression. The interventions implemented were multicomponent regimens , CBT and solution-focused therapy . Both CBT and solution-focused therapy significantly reduced depression . However, only CBT was effective in reducing anxiety which was persistent at 12 months after the intervention . No statistically significant change in anxiety or depression scores was noted among the participants of the multicomponent regimen .
The Best And Fastest Treatment For Ulcerative Colitis
The SYMPTOMS are NOT in your head. They are very real.
What is causing them though are the THOUGHTS on your head.
Thoughts?yup.
Ulcerative colitis is caused by a threat that your subconscious mind is facing and CANNOT defend itself any longer.
Your subconscious mind is crying out for help with a threat it is seeing every day all day long.
What is that threat?a thought that it perceives as life threatening.
When you eat some bad food, or drink too much alcohol what does your body do? It automatically protects itself by throwing it back up.
Well you are eating a bad thought or thoughts and it has no way to throw them back up. So it is going to get your attention in other ways.
Like blood in the toilet.
Whoa, that got your attention right? That was the purpose.
Your subconscious mind makes up about 95% of your brain power. It handles EVERYTHING your body needs to function properly.
Conscious mind vs subconscious mind EXAMPLE:
You used your subconscious mind to learn how to drive a car.
Today you drive your car using your subconscious mind.
You learned how to do it, or you programmed your mind. You now drive without thinking. It has become a habit.
Well right now there is a thought or two in your subconscious mind that you programmed as a threat. And you SM is trying to throw it up.
You need to REPROGRAM your subconscious mind. Now this is NOT the same as law of attraction!
You cannot eliminate a bad thought, you can REPLACE it with one that is positive.
You May Like: Can Stomach Ulcers Be Cancerous
Ulcerative Colitis Treatment: Surgery
If you did not respond to a medication regimen or you developed complications of colitis, you may be a candidate for surgery to treat ulcerative colitis.
Colectomy may be used in children with ulcerative colitis who experienced growth retardation. In all patients, elective colectomy can be a cure for ulcerative colitis. Almost always, the procedure is a total colectomy, meaning the entire colon is removed.
Surgical procedures include:
-
Total proctocolectomy with Brooke ileostomy. Removal of your entire colon and rectum. Your doctor will perform an ileostomy, which brings out your small intestine through the abdominal wall. Waste collects in an ileostomy bag. An ileostomy can be temporary or permanent.
Crohn’s Disease Treatment Options

A combination of treatment options can help you stay in control of your disease and help you to lead a full and rewarding life. Remember that there is no standard treatment that will work for all patients. Each patients situation is different and treatment must be followed for each circumstance.
Treatment for Crohns disease and other IBD varieties can include the use of medication, alterations in diet and nutrition, and sometimes surgical procedures to repair or remove affected portions of your GI tract.
You May Like: Foods To Eat With Peptic Ulcer Disease
What Is A Flare
When you have ulcerative colitis, your physician will try to find the right medications to control your symptoms. However, since there is no cure, the systemic disease is always there. When the symptoms arent present, you are in remission. If the symptoms return, especially if they are worse than before, it is a flare. This is why it is important to continue taking any medications your doctor prescribes, even if you feel better. If you stop taking your medication, then you can increase your chance of experiencing a flare and progression of the disease. Infections, stress, and taking antibiotics or NSAIDs can also make you more susceptible to a flare.
Future Aspects In The Management Of Ibd
CD and UC are complex disorders which need complex therapeutic strategies and a continuous development of treatment managements, new drugs and alternative measures. Despite the high prevalence of mental health co-morbidities in IBD, psychological illness remains largely under treated, with studies showing that 60% of IBD patients experiencing mental health problems do not receive adequate help. Therapeutic approaches must always be chosen in agreement with the patients to increase the patients compliance.
Due to the complexity of the disease a collaboration of medical specialists is necessary to cover all complications and to improve treatment success.
A new scoring system for CD, the Lémann score, is developed to allow a better identification of patients with severe epithelial damage and those with rapid progression of damage. This system monitors the cumulative damage. It measures cumulative structural bowel progression at a specific time point, based on medical and disease history, by endoscopy and other imaging methods. This instrument can also be used to assess the effect of various medical therapies on the progression of bowel damage.
Another point in therapeutic care in IBD is a harmonization between different countries and centers. Two retrospective cross sectional studies from 2009 describe country and care-setting specific therapeutic variations. The impact on outcome is not yet clear.
Don’t Miss: Can Ulcerative Colitis Cause Bladder Problems
Medication Options For Ulcerative Colitis
Medication is the first line of treatment for ulcerative colitis. Your doctors recommendation for which medication will work best for you is based on the severity of your disease, your overall health, and other individual factors.
There are six major classes of medication used to treat ulcerative colitis.
Physical Activity And Exercise
Reduced cardiovascular capacity, impaired muscle function, and secondary osteoporosis has been reported in patients with IBD. Limited physical activity, particularly with CD, due to fatigue may partially explain these negative outcomes. Conversely, regular physical activity seems to improve disease activity and fatigue in patients with IBD. For example, regimented exercise has been shown to improve disease activity and QOL, as well as cardiovascular and bone health. The best available evidence for PA/E for IBD is described below.
Recommended Reading: Alternative Medicine For Ulcerative Colitis
Oral Vs Rectal Treatments
Most physicians prescribe ulcerative colitis patients oral versions of 5-ASAs or corticosteroids, since this is a patient-preferred delivery method of medication. However, even if they have a specially designed release mechanism, they might not reach and treat the area where the disease is most active.
For example, when you apply sunscreen to your skin, you need to make sure that you cover every exposed part to protect it from the sun. Similarly, when applying these treatments to your rectum and lower colon, you need to make sure that the product covers all of the inflamed areas.
Oral tablets might not be the optimal way to reach the end of the colon, where stool and the fact that ulcerative colitis patients have diarrhea, might interfere with its effectiveness. Unfortunately, this is also the area in the colon where a flare usually starts. The best way to reach this particular area is by inserting the drug directly into the rectum.
Rectal preparations are particularly good at treating urgency and bleeding, symptoms that often are very bothersome. A positive response often occurs within days of treatment.
The 3 Key Goals Of Uc Treatment
There are treatments available that can help control excess inflammation in order to help you:
Controlling inflammation can help relieve UC symptoms such as frequent and urgent bowel movements, bloody stools, and abdominal pain.
Controlling inflammation can also help you achieve and maintain remission. This means you have achieved ongoing symptom relief and are able to prevent flares.
Controlling inflammation over time allows the lining of the colon to heal and can help you maintain remission.
Don’t Miss: What Is Good For Ulcers
Recommendations For Cancer Surveillance
Patient with UC have an elevated risk of developing colon cancer. After 8-10 years of colitis, annual or biannual surveillance colonoscopy with multiple biopsies at regular intervals should be performed . Detection of high grade dysplasia in flat mucosa has to be confirmed by a second pathologist and is an indication for colectomy .
The sensitivity of random biopsies is a matter of debate and uncertainty as dysplasia in flat mucosa can be easily overlooked. Implementation of advanced endoscopic imaging techniques such as high-resolution white-light endoscopy, autofluorescence and narrow-band imaging may help to better identify pathological lesions and optimize cancer surveillance in inflammatory bowel disease in the future.
Complementary Treatments And Therapies
You may consider these approaches in addition to what your doctor prescribes. But itâs important to talk to your medical team about any and all of them because some, like supplements, can interfere with treatments from your doctor. Letâs take a look at a few:
Mind-body therapies:Stress and anxiety are well-known triggers for many people with ulcerative colitis, so it is not surprising that mind-body relaxation techniques could help. These techniques help nurture a healthy connection between your mind and body as well as between you and the outside world. In some cases, they encourage behavior changes in your everyday life. They may be worthwhile if only to lessen anxiety and depression linked to UC and improve quality of life. In addition, there is some evidence that yoga, meditation, and gut-centered hypnotherapy could help with some physical symptoms or flare-ups of UC. Some of the techniques, like cognitive behavioral therapy and patient support groups, have been so successful that they have slowly become a part of mainstream treatment for IBD.
Keep in mind that the FDA doesn’t regulate supplements, so claims on packaging may not be accurate. Thatâs yet another reason why itâs important to talk to your doctor before you start taking any supplements for your UC.
Read Also: Oral Antibiotics For Leg Ulcers
Eat More Fruits Veggies And Soluble Fiber
According to Whitney Duff, Ph.D. the lead researcher on the 2018 study, diet is a key way to manage your IBD. We know that IBD is linked to alterations in the microbiota living in our gut. As scientists begin to understand the links between the gut microbiota and health, we learn that diet is a key player, she tells HealthCentral. Fiber is well studied and is known to support the growth of good bacteria. Many large studies demonstrate that those who consume a fiber-rich diet have a lower risk of developing IBD.
Medication For Inflammatory Bowel Disease
Gastroenterologists at NYU Langone’s Inflammatory Bowel Disease Center may prescribe one or more medications to reduce inflammation in the digestive tract caused by inflammatory bowel disease, or IBD. The goals of treatment are to improve symptoms and heal any damage to the intestines.
Our gastroenterologists develop a personalized treatment plan for you based on the type of IBD, the severity of the condition, and the results of diagnostic tests. These tests may have confirmed that you have Crohns disease, which can affect any part of the gastrointestinal tract, or ulcerative colitis, which only affects only the colon, or large intestine.
Medications work differently in different people, so your gastroenterologist closely monitors how well you respond to treatment. He or she adjusts the type or dose of medication as often as needed.
Medications for IBD can often reduce inflammation and promote healing in the intestines, resulting in remissionmeaning long-term symptom relief. However, for many people with IBD, the condition is chronic and treatment is lifelong. It is very important to follow up regularly with your gastroenterologist.
Don’t Miss: Low Carb Diet For Ulcerative Colitis