Stasis Dermatitis And Ulcers
We include products we think are useful for our readers. If you buy through links on this page, we may earn a small commission. Heres our process.
What is stasis dermatitis?
Stasis dermatitis is skin inflammation that develops in people with poor circulation. It most often occurs in the lower legs because thats where blood typically collects.
When blood collects or pools in the veins of your lower legs, the pressure on the veins increases. The increased pressure damages your capillaries, which are very small blood vessels. This allows proteins to leak into your tissues. This leakage leads to a buildup of blood cells, fluid, and proteins, and that buildup causes your legs to swell. This swelling is called peripheral edema.
People with stasis dermatitis usually experience swollen legs and feet, open sores, or itchy and reddish skin.
One theory is that a protein called fibrinogen may be responsible for the changes you see in your skin. When fibrinogen leaks into your tissues, your body converts it to the active form of the protein, which is called fibrin. As it leaks out, the fibrin surrounds your capillaries, forming what are known as fibrin cuffs. These fibrin cuffs may prevent oxygen from entering your tissues. And when your cells dont receive enough oxygen, they can become damaged and die.
The symptoms of stasis dermatitis include:
- skin discoloration
You may also experience symptoms of venous insufficiency, including:
What Causes A Stasis Ulcer
Stasis ulcers are a complication of venous insufficiency, which is a health condition that affects the veins. Healthy vein valves normally help blood return to the heart, but the vein valves in people with venous insufficiency are damaged or weakened. This can lead to blood pooling in the legs instead of flowing back toward the heart. The resulting fluid buildup beneath the skin can damage the skin layer, causing a stasis ulcer to develop.
Managing Venous Stasis Ulcers
Venous disease, which encompasses all conditions caused by or related to diseased or abnormal veins, affects about 15% of adults. When mild, it rarely poses a problem, but as it worsens, it can become crippling and chronic.
Chronic venous disease often is overlooked by primary and cardiovascular care providers, who underestimate its magnitude and impact. Chronic venous insufficiency causes hypertension in the venous system of the legs, leading to various pathologies that involve pain, swelling, edema, skin changes, stasis dermatitis, and ulcers. An estimated 1% of the U.S. population suffers from venous stasis ulcers . Causes of VSUs include inflammatory processes resulting in leukocyte activation, endothelial damage, platelet aggregation, and intracellular edema. Preventing VSUs is the most important aspect of CVI management.
Treatments for VSUs include compression therapy, local wound care , dressings, topical or systemic antibiotics for infected wounds, other pharmacologic agents, surgery, and adjunctive therapy. Clinicians should be able to recognize early CVI manifestations and choose specific treatments based on disease severity and the patients anatomic and pathophysiologic features. Management starts with a full history, physical examination, and risk-factor identification. Wound care clinicians should individualize therapy as appropriate to manage signs and symptoms.
Recommended Reading: Ulcer Pain Relief At Night
How Is Venous Insufficiency Treated
To reduce swelling and relieve pain caused by venous insufficiency, you can wear compression stockings. They are tighter at the ankles than at the top of the legs. They also can help venous skin ulcers heal. But there are different types of stockings, and they need to fit right. So your doctor will recommend what you need.
You also can try to:
- Get more exercise, especially walking. It can increase blood flow.
- Avoid standing still or sitting for a long time, which can make the fluid pool in your legs.
- Try not to sit with your legs crossed at the knee.
- Keep your legs raised above your heart when you’re lying down. This reduces swelling.
If these treatments don’t work, you may need medicine or a procedure to help relieve symptoms. Procedures might be done to close the vein, to remove the vein, or to improve blood flow.
What Do Stasis Ulcers Look Like
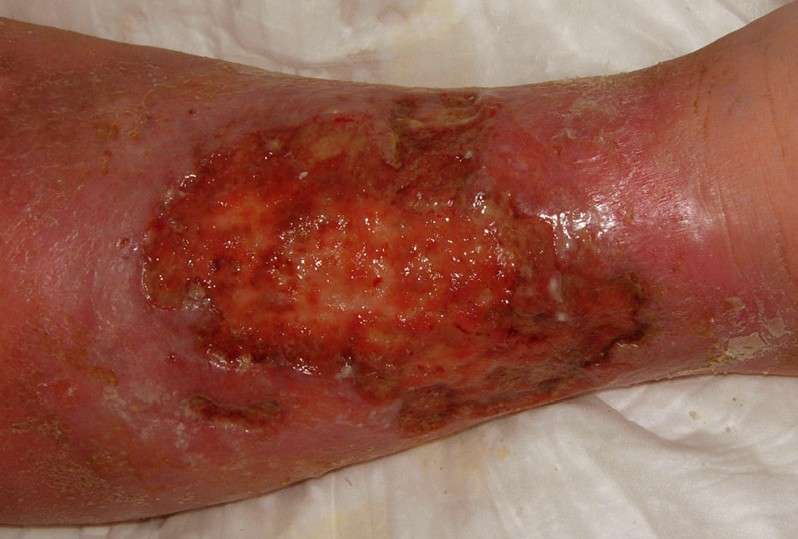
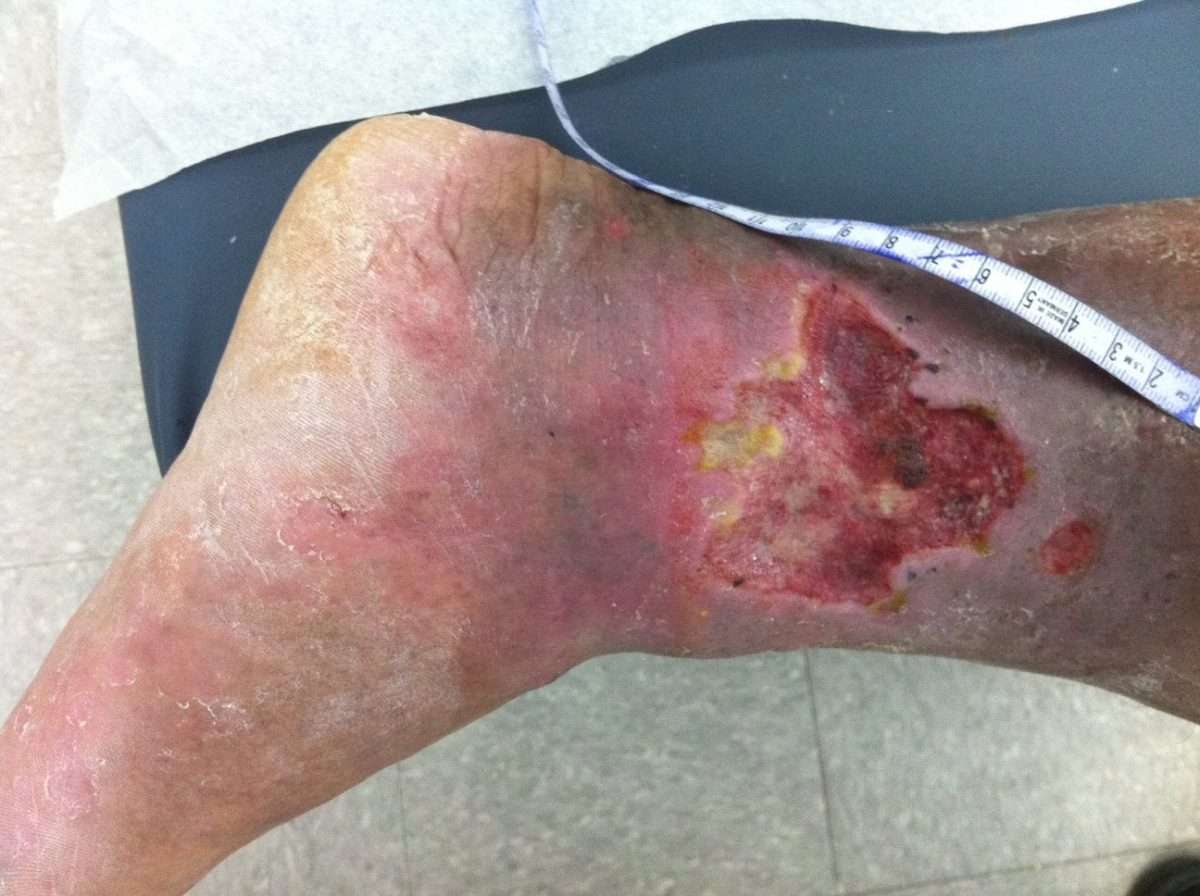
Stasis ulcers are commonly located on the lower legs, usually just above the ankles. They are shallow, open wounds with uneven borders, and they can vary in size and shape. The base of the sore will be red, sometimes with an overlay of yellow tissue. The surrounding skin may discolor , and it may also be shiny, tight, swollen, and warm to the touch. Often, the whole leg will become swollen.
Recommended Reading: Can Ulcerative Colitis Cause Back Pain
How Are Stasis Ulcers Diagnosed
Stasis ulceration is usually a clinical diagnosis, made on the basis of the patient’s history and examination findings, and includes the presence of risk factors for venous stasis, that is, congestion and slowing of venous circulation, and the characteristic features of the wound and surrounding tissues.
- Duplex ultrasonography is used to confirm venous obstruction or valvular incompetence prior to saphenous vein ablation surgery
- Concomitant arterial disease is identified using the ankle-brachial index
Other investigations to evaluate venous insufficiency and provide haemodynamic information may include:
- Intravenous ultrasonography
- Ascending or descending venography/phlebography
- Venous air plethysmography
- Haematological studies of the coagulation system.
Risk Factors And Symptoms
The incidence of venous insufficiency rises with age, and is also linked to a family history of varicose veins, a sedentary lifestyle, or to jobs that require people to spend many hours on their feet. Venous insufficiency can also be caused by a partial blockage of the veins, for example by a blood clot .
The most common early symptom of venous insufficiency is chronically swollen ankles the feet and calves may also swell. The swelling can be accompanied by a dull aching, cramping, or feeling of heaviness in the legs and feet that becomes worse after prolonged standing.
As the condition progresses, people with venous insufficiency develop brown patches and deteriorating skin around the ankles. If venous insufficiency is not treated, venous ulcers may develop on the lower legs.
Doctors use an imaging test called a duplex ultrasound to determine if there is structural damage in the veins.
Read Also: Is Burping A Sign Of An Ulcer
Prompt Proper Care Will Help Reduce Complications And Improve Quality Of Life
Venous ulcers are the most common lower extremity wounds in the United States. Patients experience poor quality of life as a result of pain and immobility, and they require advanced levels of wound care. Any delay in care increases the risk of infection, sepsis, amputation, skin cancers, and death. Patients who develop complications may require frequent care visits, dressing changes, and recurrent hospitalizations. In addition, they may experience loss of productivity, significant discomfort, or disability.
Many patients with venous ulcers struggle with adherence to rigorous treatment regimens, and the COVID-19 pandemic has added to that challenge because of treatment delays. For example, risk of complications increases when venous reflux goes undertreated or untreated, increasing the incidence of venous ulcers, which can be costly for the healthcare system and detrimental to patients lives.
Targeted nursing education is essential to improve the assessment and management of venous leg ulcers. In addition, empowering patients to care for themselves can help bridge care gaps.
Pandemic impact on wound care
A multidisciplinary approach in collaboration with a wound care center is the most beneficial for addressing wound care. However, during the height of the pandemic, the availability of expert care from a wound center was limited. The situation has eased in some geographic regions, but remains problematic in others.
About Venous Leg Ulcers
A leg ulcer is a long-lasting sore that takes more than 4 to 6 weeks to heal. They usually develop on the inside of the leg, just above the ankle.
The symptoms of a venous leg ulcer include pain, itching and swelling in the affected leg. There may also be discoloured or hardened skin around the ulcer, and the sore may produce a foul-smelling discharge.
See your GP if you think you have a leg ulcer, as it will need specialist treatment to help it heal.
Your GP will examine your leg and may carry out additional tests to rule out other conditions.
Read more about how a venous leg ulcer is diagnosed.
Don’t Miss: Is Ulcerative Colitis And Colitis The Same Thing
Implications For Future Practice
Improving venous ulcer care requires increasing nurse wound care knowledge across settings and ensuring nurses work at the top of their scope of practice. For example, barring exclusion from a states nursing practice act, training in debridement of venous ulcers can be taught to nurses in many settings to facilitate care outside of wound care centers. In addition, nurses and patients can use monofilament devices for mechanical debridement.
The Centers for Medicare & Medicaid Services has paved the way for using telehealth during the pandemic, making it an ongoing viable option for helping patients adhere to treatment recommendations. It can be used for patient and family education and to perform screening and monitoring visits, effectively reducing barriers to care.
For more complex patients, home health nurses should be trained in advanced wound care to help reduce gaps in care during times of crisis and for patients unable to visit a wound care center. In addition, in-person or virtual patient self-care education is vital to ensure proper venous ulcer management if in-office or home health visits arent possible.
What Is The Best Treatment For Venous Ulcers
What is the recommended procedure for treating leg ulcers?
It depends on the cause. If the ulcers are due to varicose veins, then treatment of the varicosities can help significantly in conjunction with a wound care specialist. If due to deep venous reflux, compression stockings and wound care are the best choices.
It depends on the cause. If the ulcers are due to varicose veins, then treatment of the varicosities can help significantly in conjunction with a wound care specialist. If due to deep venous reflux, compression stockings and wound care are the best choices.
Correct any superficial venous reflux.
Correct any superficial venous reflux.
Venous stasis ulcers can be due to deep, superficial, and/ or perforatorvein incompetence deep vein thrombosis can also be involved in theetiology. Before recommending the best treatment, venous duplex scanning must be performed and acomprehensive history and physical must be taken by an expert in the field of complex venous disorders. Perforator vein surgery , superficial venous ablation, vein interruptions, or a combination of these treatments may be indicated.
The best treatment for venous ulcers consists of 2 parts, both applied assoon as possible. First, the underlying cause should be identified andtreated. Second, proper compression with edema reduction and specializedwound care is needed until the ulcer heals.
Don’t Miss: Can You Donate Blood If You Have Ulcerative Colitis
Do Not Hesitate Get Treatment
If you do suffer venous stasis ulcers, its critical that you get treatment immediately. Your doctor will clean the wound and may apply an antibiotic ointment to stave off an existing or potential infection. Other treatment options may include wearing of a special boot that helps to protect and more quickly heal the wound, time in a whirlpool, and ultrasound or physical therapy. While most patients respond well and heal with adequate wound care, extreme cases may require skin-grafting surgery.
It is very important to also treat the abnormal veins which caused the ulcer. If not the ulceration will usually reoccur.
If you have signs of venous statis ulcers, contact the St. Johns Vein Center at 877-640-VEIN and schedule a consultation today.
Dont Miss: Foam Dressing For Pressure Ulcer
Venous Ulcer Diagnosis And Treatment
Doctors at Vascular surgeons at UPMC’s Heart and Vascular Institute use duplex ultrasound, a noninvasive test, to diagnose abnormal veins that cause venous ulcers. Part of the UPMC difference is that we actively look for the causes of the ulceration to treat venous pathology and keep the ulcer healed.
After an evaluation of your veins, we recommend a treatment plan based on your needs:
- Compression
- Compression of the leg is vital to healing venous wounds.
- Compression stockings are most commonly used for this treatment.
- The pressure from the compression dressing counteracts the pressure from the veins of the leg and allows skin to heal.
Recommended Reading: How To Check A Horse For Ulcers
Best Practices For Venous Leg Ulcer Treatment
Venous leg ulcer treatment and management require frequent examination of at-risk patients and best practice wound care with a focus on prevention. Without effective treatment, venous leg ulcers can become extremely painful and result in cellulitis, osteomyelitis, and even death.1 To prevent these complications, health care professionals must actively work to identify venous leg ulcers, manage exudate, and choose wound dressings that enable an optimal healing environment. This can help promote rapid healing, reduce costs, and improve quality of life for patients.1
Identifying At-Risk Patients One of the most important components of venous leg ulcer management is prevention. Venous leg ulcers are caused by inflammatory processes that lead to endothelial damage, platelet aggregation, and intracellular edema. By taking steps to identify at-risk patients and regularly assessing them for signs of ulcers, health care professionals can reduce the incidence of the disease. Older adults, obese patients, those with mobility issues, and those who have previously had a venous leg ulcer are all significantly more likely to develop venous ulcers.1
Elevate Legs Leg elevation for 30 minutes three to four times a day can help reduce edema and thus may positively affect inflammation.1
Dress the Wound Dressings aid in the treatment of venous leg ulcers by protecting the wound, preventing adherence of compression bandages, and enabling an ideal healing environment.1,5
Articles On Types Of Dermatitis
Venous stasis dermatitis happens when there’s a problem with your veins, usually in your lower legs, that keeps blood from moving through very well. As more fluid and pressure build, some of the blood leaks out of your veins and into your skin.
The condition is also called venous eczema or stasis dermatitis. It’s more common in people who are 50 or older. Women are more likely to have it than men.
Medical treatments can help, and you can do many things on your own to get the problem under control.
Read Also: Can Coffee Cause Ulcerative Colitis
Swelling In The Legs And Ankles
Venous leg ulcers are often accompanied by swelling of your feet and ankles , which is caused by fluid. This can be controlled by compression bandages.
Keeping your leg elevated whenever possible, ideally with your toes above your hips, will also help ease swelling.
You should put a suitcase, sofa cushion or foam wedge under the bottom of your mattress to help keep your legs raised while you sleep.
You should also keep as active as possible and aim to continue with your normal activities.
Regular exercise, such as a daily walk, will help reduce leg swelling.
But you should avoid sitting or standing still with your feet down. You should elevate your feet at least every hour.
Elevation Of The Legs
The legs should be placed in an elevated position, ideally at 30 degrees to the heart, while lying down. This, again, helps in the movement of venous blood to the heart.This also prevents the build-up of liquid in the legs that leads to swelling. A cushion or any other object of comfort can be used to keep the toes above the level of the hip while sleeping.
Also Check: How To Reduce Bloating With Ulcerative Colitis
Differentiating Lower Extremity Wounds
Understanding other lower extremity woundsarterial ulcers, neuropathic ulcers, and pressure injuriescan help nurses differentiate them from venous ulcers. A detailed clinical history and thorough assessment when evaluating lower extremity ulcers can aid diagnosis and guide treatment, which may differ depending on the type of ulcer.
Treatments for some types of wounds may be harmful for others. For example, if compression therapy is applied to a limb with arterial insufficiency that resulted in an arterial ulcer, blood flow can be reduced further, potentially leading to amputation.
Arterial ulcers
Arterial ulcers are small, have an irregular shape, and appear punched-out with a deep base. Typically, necrotic tissue is present with low exudate unless the wound is infected. The ulcers usually are located over the pretibial area, the lateral malleolus , or on the toes or heel.
Most patients report severe pain thats relieved when the extremity is placed in a dependent position and increased when the extremity is elevated. Assessment findings include abnormal distal pulses, cold extremities, and prolonged venous filling time. Arterial ulcers may be caused by tissue ischemia resulting from atherosclerosis.
Arterial vs. venous ulcer
The following table compares venous and arterial ulcers, which can occur as a result of peripheral vascular disease.
| Arterial |
Neuropathic ulcers
Pressure injuries
What Types Of Wounds Can Alginate Dressings Heal
Alginate dressings usually do best on wounds that are actively giving out bodily secretions as the gel forms a shield around the sore to help soak up the secretions while keeping all other foreign bodies out of the cut, which lowers risks of infections. Alginate is also useful for wounds that are bleeding profusely as there are calcium fibers in the bandages which can break down and help slow the bleeding of a sore is bleeding heavily. Alginate dressings have long been used to dress wounds including fissures, hyper granulating tissue, interdigital maceration, heloma mole, and other lesions. Alginate dressings have also successfully been used to cover wounds on the parts of the body that are utilized the most such as on the feet. When it comes to healing venous ulcers, more studies are needed to see if Alginate dressings are effective.
If you do have venous ulcers or varicose veins, take a look at our Vein Score tool! After entering your symptoms and zip code, you will receive and vein score and a list of local vein physicians.
Medically reviewed by Dr. Susanne Woloson on 5-01-2020.
*Disclaimer: We are a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for us to earn fees by linking to Amazon.com and affiliated sites.
Medically reviewed by Dr. Susanne Woloson on May 5, 2020
Also Check: Food For Ulcer Patient In Nigeria
Also Check: Foods To Eat During Ulcerative Colitis Flare Up