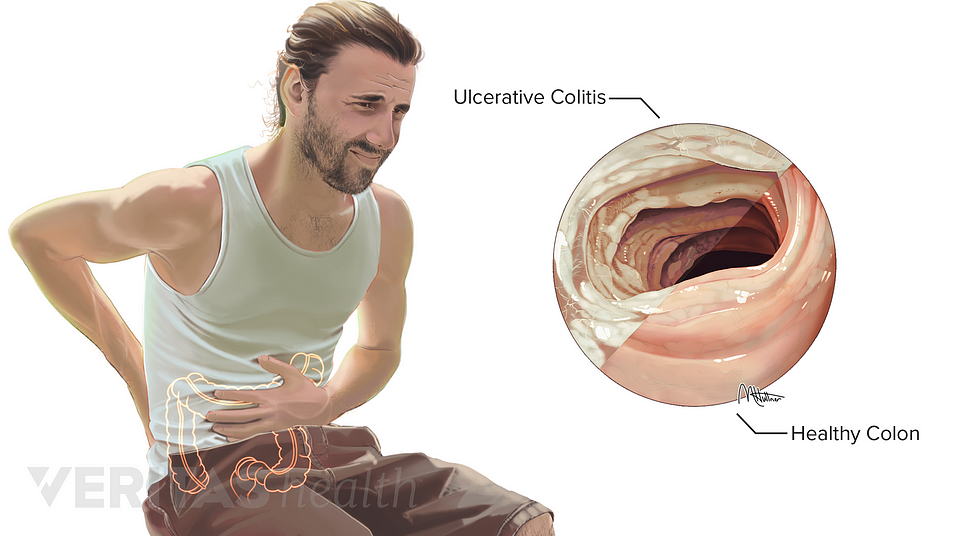
Can I Get Surgery For My Ulcerative Colitis
Surgery is an option if medications arent working or you have complications, such as bleeding or abnormal growths. You might develop precancerous lesions, or growths that can turn into colorectal cancer. A doctor can remove these lesions with surgery or during a colonoscopy.
Research shows that about 30% of people with ulcerative colitis need surgery sometime during their life. About 20% of children with ulcerative colitis will need surgery during their childhood years.
There are two kinds of surgery for ulcerative colitis:
Proctocolectomy and ileoanal pouch
The proctocolectomy and ileoanal pouch is the most common procedure for ulcerative colitis. This procedure typically requires more than one surgery, and there are several ways to do it. First, your surgeon does a proctocolectomy a procedure that removes your colon and rectum. Then the surgeon forms an ileoanal pouch to create a new rectum. While your body and newly made pouch is healing, your surgeon may perform a temporary ileostomy at the same time. This creates an opening in your lower belly. Your small intestines attach to the stoma, which looks like a small piece of pink skin on your belly.
After you heal, waste from your small intestines comes out through the stoma and into an attached bag called an ostomy bag. The small bag lies flat on the outside of your body, below your beltline. Youll need to wear the bag at all times to collect waste. Youll have to change the bag frequently throughout the day.
Impact Of Pain On Quality Of Life
When assessing the impact on quality of life 528 patients of the patients had an impact on the duties of daily life, with a median of 3/10 , 329 had no impact and 37 did not specify. 513 patients had an impact on their work with a median of 4/10 , 344 had no impact on work, 37 did not specify. The general quality of life was significantly lower in patients suffering of pain compared to those without pain p< 0.0001).
Questions To Ask Your Doctor
- How will my inflammatory bowel disease be treated?
- Will I need surgery? Are there other options?
- What lifestyle changes can I make to help inflammatory bowel disease?
- What are some medicines used to treat inflammatory bowel disease and what are the possible side effects?
- Are my children at risk of inflammatory bowel disease?
Also Check: Indian Diet For Ulcerative Colitis
How To Tell A Back Strain From A More Serious Medical Condition
So, how can you be sure that the pain in your back isnt the result of some weekend gardening but rather a more serious medical condition? Most of the time when Dr. Crooks sees patients, theyve had their medical issue diagnosed and theyre dealing with the secondary effects of that problem in their musculoskeletal system.
However, he has seen patients whove come to him for back pain only to find something on an imaging study MRI such as a kidney stone or even cancer, which is more unusual.
Here are the most common medical conditions that can mimic musculoskeletal back pain and how you can help tell the difference:
Breast Lung Abdomen Colon Pancreas Gallbladder
These types of cancers can metastasize to the spine and cause back pain. Also with abdominal cancers, pancreatic and gallbladder cancers, you can get the referred visceral pain even before they metastasize, says Dr. Crooks. When cancers do spread to the spine, you can have severe spinal pain.
Depending on the type of cancer, treatments like intrathecal pain pumps can deliver medicine like an anesthetic, nerve pain medicine, or a narcotic in small doses straight to the spine without negative effects like tolerance, addiction, and overdose. Stimulation to the spinal nerve root and spinal blocks are also effective treatments for spinal pain.
Wheres the pain? Depending on the type of cancer, back pain can be in the upper, mid, or lower spine
What are the other possible symptoms? Fatigue that doesnt improve with rest, unexplained weight loss or gain, loss of appetite, nausea, vomiting, swelling or lumps, skin changes, hoarseness, persistent cough, change in bowel habits, vision or hearing problems, headache, and others
What does it feel like? Back pain can range from mild to severe depending on the type of cancer and location and may not respond to OTC pain relievers
While your primary care doctor or specialist helps keep your medical issue in check, a pain specialist can improve chronic musculoskeletal pain that stems from inflammation and overstimulated nerves that can occur when you have one of these conditions.
Read Also: Symptoms Of Crohn’s Vs Ulcerative Colitis
What Should I Ask My Doctor
If you have ulcerative colitis, you may want to ask your healthcare provider:
- How much of my large intestine is affected?
- What risks or side effects can I expect from the medication?
- Should I change my diet?
- Will ulcerative colitis affect my ability to get pregnant?
- What can I do at home to manage my symptoms?
- What are my surgical options?
Also Check: Will Aleve Help Back Pain
Back Pain Often Comes Directly From Back Or Spinal Structures But Sometimes Its A Sign Of A Medical Condition Elsewhere In Your Body Heres What Else Could Be Causing Your Back Pain
Heres a scene that plays out every day, all over the world: Someone thinks they have a little back strain. Perhaps they lifted something wrong or moved the wrong way. It was just a twinge, so they waited it out a few days for the pain to go away. It doesnt, so they head to their doctor. Turns out, they hadnt lifted anything wrong at all. It was the start of a kidney infection, or a UTI, or pancreatitis.
Heres how to tell the difference between a back strain and something more serious going on.
How do you know when the root cause of back pain is elsewhere in your body? There are two types of pain we look at, explains Matthew Crooks, MD, a pain specialist at Pinnacle Pain and Spine in Scottsdale, Arizona: visceral pain and somatic pain. Visceral pain is pain from an organ or internal pain that can radiate to the spine with conditions like pancreatitis, ulcerative colitis or Crohns disease, gall stones, cancers, kidney pain, and urinary tract infection, says Dr. Crooks.
Whats more, thanks to aging, injury, or a sedentary lifestyle, almost everyone has some wear and tear in the spine and pain in the musculoskeletal system . When you do develop visceral pain, it can flare up your somatic pain. And thats separate from the pain thats radiating from an organ, says Dr. Crooks. It can be activated from overall inflammation and the stress of the body dealing with the medical issue. Its the BOGO special that you never want.
Don’t Miss: Succeed For Horses With Ulcers
How Is Ulcerative Colitis Diagnosed
To diagnose ulcerative colitis in children, teenagers and adults, your healthcare provider has to rule out other illnesses. After a physical exam, your provider may order:
- Blood tests: Your blood can show signs of infection or anemia. Anemia is a low level of iron in your blood. It can mean you have bleeding in the colon or rectum.
- Stool samples: Signs of infection, parasites , and inflammation can show up in your poop.
- Imaging tests: Your healthcare provider may need a picture of your colon and rectum. You may have tests including a magnetic resonance imaging scan or computed tomography scan.
- Endoscopic tests: An endoscope is a thin, flexible tube with a tiny camera. Specialized doctors can slide the endoscope in through the anus to check the health of the rectum and colon. Common endoscopic tests include colonoscopy and sigmoidoscopy.
What’s The Link Between Uc And As
Both UC and AS are inflammatory diseases. UC inflames the intestine, while AS inflames the spine.
A faulty immune response triggers inflammation in both diseases. Gene changes might be behind the immune misfire. People with IBD often have family members with AS. Scientists have found a few genes that might trigger both diseases, including HLA-B27. But just because you have the HLA gene doesn’t mean you’ll get AS.
There’s also a strong link between the gut and the joints. Scientists have found that bacteria and immune cells from the intestine can travel to the joints and cause inflammation there.
Don’t Miss: Are Beets Good For Ulcerative Colitis
Ankylosing Spondylitis And Ulcerative Colitis
When fusion occurs, axial spondyloarthritis progresses into ankylosing spondylitis. AS is a specific type of axial arthritis that causes inflammatory back pain and limits range of motion. If a person has AS that causes significant fusing in their vertebral column and affects their rib movement, they may also struggle to take deep breaths.
According to the University of Washington, ankylosing spondylitis symptoms generally dont present alongside gastrointestinal symptoms in people with UC. Although doctors arent entirely sure what causes AS, some research suggests a genetic component contributes to the diseases development. Bowel or urinary tract infections are also believed to trigger the onset of AS in genetically susceptible people.
Axial Arthritis And Ulcerative Colitis
Although more common in people with Crohns disease, axial arthritis can also affect those with UC. Over time, axial arthritis causes pain and stiffness in the lower spine and sacroiliac joints, which connect the lower spine and pelvis.
The main symptoms of axial arthritis are stiffness and pain in the lower back, hips, and buttocks that persist for three or more months at a time. Flare-ups typically come on slowly, gradually worsening over a period of several weeks or months. Symptoms tend to be at their worst in the morning and wear off with time and exercise. Prolonged rest or inactivity can make joint pain worse.
I can’t bend or twist like I used to, wrote one MyCrohnsAndColitisTeam member. It hurts too bad. Being up and about helps, but getting up for those first few steps after sitting a while is so painful, and I can’t fully stand upright sometimes for a minute or so. It’s frustrating.
Also Check: Can You Donate Blood If You Have Ulcerative Colitis
Poor Growth And Development
Ulcerative colitis, and some of the treatments for it, can affect growth and delay puberty.
Children and young people with ulcerative colitis should have their height and body weight measured regularly by healthcare professionals.
This should be checked against average measurements for their age.
These checks should be carried out every 3 to 12 months, depending on the person’s age, the treatment they’re having and the severity of their symptoms.
If there are problems with your child’s growth or development, they may be referred to a paediatrician .
Gi Issues Caused By Kidney Stones
Normally, kidney stones cause symptoms such as pressure and pain in your lower back, fever, frequent urination, discomfort urinating, and bloody or discoloured urine. However, sometimes kidney stones can cause gastrointestinal symptoms such as nausea, vomiting, and stomach discomfort.
If youre experiencing sudden low back pain and gastrointestinal discomfort, dont ignore the possibility that it might be kidney stones.
Also Check: Advil For Lower Back Pain
You May Like: Venous Leg Ulcer Dressing Treatment
Study Design And Data Collection
All IBD patients with and without self-reported joint/back pain, who signed informed consent, were seen at the JOINT outpatient clinic at study inclusion and at 1 year follow-up. During the 12-month study period, patients were asked to complete monthly questionnaires assessing IBD disease activity and spine and/or peripheral joint scores. When no response was received within 1 week, a reminder email or letter was sent out, followed by a telephone call.
Following the baseline assessment, patients were categorised into two study groups:
Patients with joint/back pain: CBP for 3 months and/or pJTC currently or during the previous year.
Patients without joint/back pain: no back pain or pJTC during the previous year.
Routine Screening To The Rescue
When the physician turned 60, he scheduled a colonoscopy, a recommended test to screen asymptomatic individuals over 50 for colon cancer. He had one at 50 it was completely normal. When it was time for his next exam, the doctor who did it the first time had retired, so he asked a friend, Dr. Erick Chan, a gastroenterologist, to perform the test.
He was still a little foggy from the anesthesia when Chan came by with what the physician assumed would be the usual report of normal results. He was wrong. I took some biopsies, and well wait to see what they show, Chan said. But I have to tell you, it didnt look normal. The test had been routine until Chan got close to the spot where the colon and the small intestine connect, a structure known as the ileocecal valve. Chan noticed that the valve looked a little asymmetric.
As Chan advanced his scope, he could see that the valve was distorted by scar tissue so much so that the connection was too narrow for his instrument to enter. Bringing his scope as close to the opening as he could, he saw that the tissue on the other side was an angry red and dotted with ulcers. They would have to wait for the biopsies to come back, but Chan suspected Crohns disease. Thats impossible, the man responded. He had no G.I. symptoms at all. No pain, no diarrhea, no blood in his stools. How could he possibly have Crohns?
- Medical Author: Melissa Conrad Stöppler, MD
Reviewed on 10/9/2020
Dont Miss: Can O Positive Donate Kidney To Anyone
You May Like: Diabetic Ulcer On Big Toe
Who Gets Ulcerative Colitis
Anyone at any age, including young children, can get ulcerative colitis. Your chance of getting it is slightly higher if you:
- Have a close relative with inflammatory bowel disease .
- Are between 15 and 30 years old, or older than 60.
- Are Jewish.
- Use frequent nonsteroidal anti-inflammatory drugs like ibuprofen .
Pain As A Tool For Diagnosis
Because pain can come from different sources, and pain in the abdomen is particularly difficult to pinpoint, it is not a symptom that is normally used to diagnose IBD or a particular form of IBD.
Rather, the type and location of pain is more often used together with other signs and symptoms when diagnosing IBD or other conditions. In other words, it might be a starting point to help a healthcare provider know where to start looking for inflammation, but its only one part of the picture.
Also Check: Early Symptoms Of Ulcerative Colitis
He Had Recurring Pain For Nearly A Decade
- Read in app
The pain woke the 52-year-old physician from a dead sleep. It was as if all the muscles in his right leg, from those in the buttock down his thigh to the very bottom of his calf, were on fire. He shifted slightly to see if he could find a more comfortable position. There was a jag of pain, and he almost cried out. He glanced at the clock: 4 a.m. In just three hours he would have to get up. He had a full day of patients to see. Massage didnt help. He couldnt get comfortable lying flat, so finally he moved to the living room, to a recliner. Only then, and only by lying completely still, did he manage to get the pain to abate. He drifted off, but never for long. The searing pain in his leg and buttock slowly eased, and by the time his alarm went off, he could stand and walk though his muscles still ached and he had to baby his right leg, causing a limp.
Between patients, he arranged to see his own doctor. Hed had pain off and on in his buttocks, one side or the other, for more than a year. The pain was in the middle of each cheek and was worse when he was sitting and at the end of the day. Walking to and from his car on the way home was brutal. And then, as mysteriously as it came, it would disappear only to come back a week or two later.
When To Contact A Doctor
A person living with UC should talk with their doctor if they notice symptoms associated with sacroiliitis, such as pain in the hips when walking or any other types of arthritis. A primary care physician may refer a person to a rheumatologist for diagnosis.
A person may want to consider a second opinion if their doctor does not refer them to a rheumatologist. Early referrals can help improve treatment outcomes. However, referral rates are low, according to a 2018 study .
If symptoms get worse during treatment or do not improve, a person should talk with a healthcare professional. A doctor can recommend additional therapies that may help improve symptoms of either UC or sacroiliitis.
As a person begins to better manage their UC symptoms, they will often notice an improvement in their sacroiliitis symptoms, too.
You May Like: Pressure Ulcer Root Cause Analysis
Kidney Infections And Kidney Stones
Kidneys are the bean-shaped organs located in the posterior half of the body toward the middle of the back that filter waste products from the body, regulate bodily fluids, and perform other important functions. Its very easy for kidney infections and kidney stones to mimic a sprain or strain , says Dr. Crooks.
Wheres the pain? Mid or upper back
What are the other possible symptoms? Fever, nausea, and malaise, burning sensation when you urinate
What does the pain feel like? Pain may feel higher and deeper in the back vs. lower back pain. You can also have side and groin pain. Note, the pain typically doesnt go away when you shift positions, lie down or rest.
Kidney stones and kidney infections can cause back pain.