Who Gets Diabetic Foot Ulcer
Diabetic foot ulcer has an annual incidence of 26% and affects up to 34% of diabetic patients during their lifetime. Risk factors for developing a diabetic foot ulcer include:
- Type 2 diabetes being more common than type 1
- A duration of diabetes of at least 10 years
- Poor diabetic control and high haemoglobin A1c
- Being male
- A past history of diabetic foot ulcer.
How Can I Prevent Or Reduce My Risk Of Foot And Toe Ulcers
It may be possible to reduce your risk of getting ulcers, and even stop them from coming back. Try to:
- Manage your diabetes. If you have diabetes you should wear appropriate footwear and never walk barefoot.
- Every day, examine your legs as well as the tops and bottoms of your feet and the areas between your toes. Look for any blisters, cuts, cracks, scratches or other sores. Also check for redness, increased warmth, ingrown toenails, corns and calluses. Use a mirror to view your leg or foot if necessary, or have a family member look at the area for you. See a healthcare provider immediately if you notice any problems.
- Wear appropriate shoes and socks. Talk to your podiatrist about what you need.
Tips For Diabetic Foot Care
Proper foot care can prevent these common foot problems or treat them before they cause serious complications. Here are some tips for good foot care:
Dont Miss: How To Treat An Eye Ulcer
Read Also: Does Smoking Cause Ulcers After Gastric Bypass
Diagnosing A Diabetic Ulcer
An accurate diagnosis of a diabetic ulcer must be given by a medical health professional. Most doctors will first provide a physical examination of the patients foot. Should further tests be required, a doctor may recommend an X-ray or an MRI scan.
An X-ray can show any changes in foot alignment through a system of imaging. An X-ray image can show loss of bone mass and hormonal imbalances that can potentially relate to the diagnosis of diabetes.
MRI scans use three-dimensional images of the bodys soft tissue. If the extent of damage needs to be assessed, an MRI scan can use magnetic radio waves to reveal possible inflammation. This test can expose any significant infections in the foot.
One of the simplest tests a physician can use to diagnose an infectious diabetic ulcer is the blood test. This test is usually done by drawing blood at a doctors office so that the results can be sent to a lab for further information.
Diabetic Foot Ulcer Symptoms
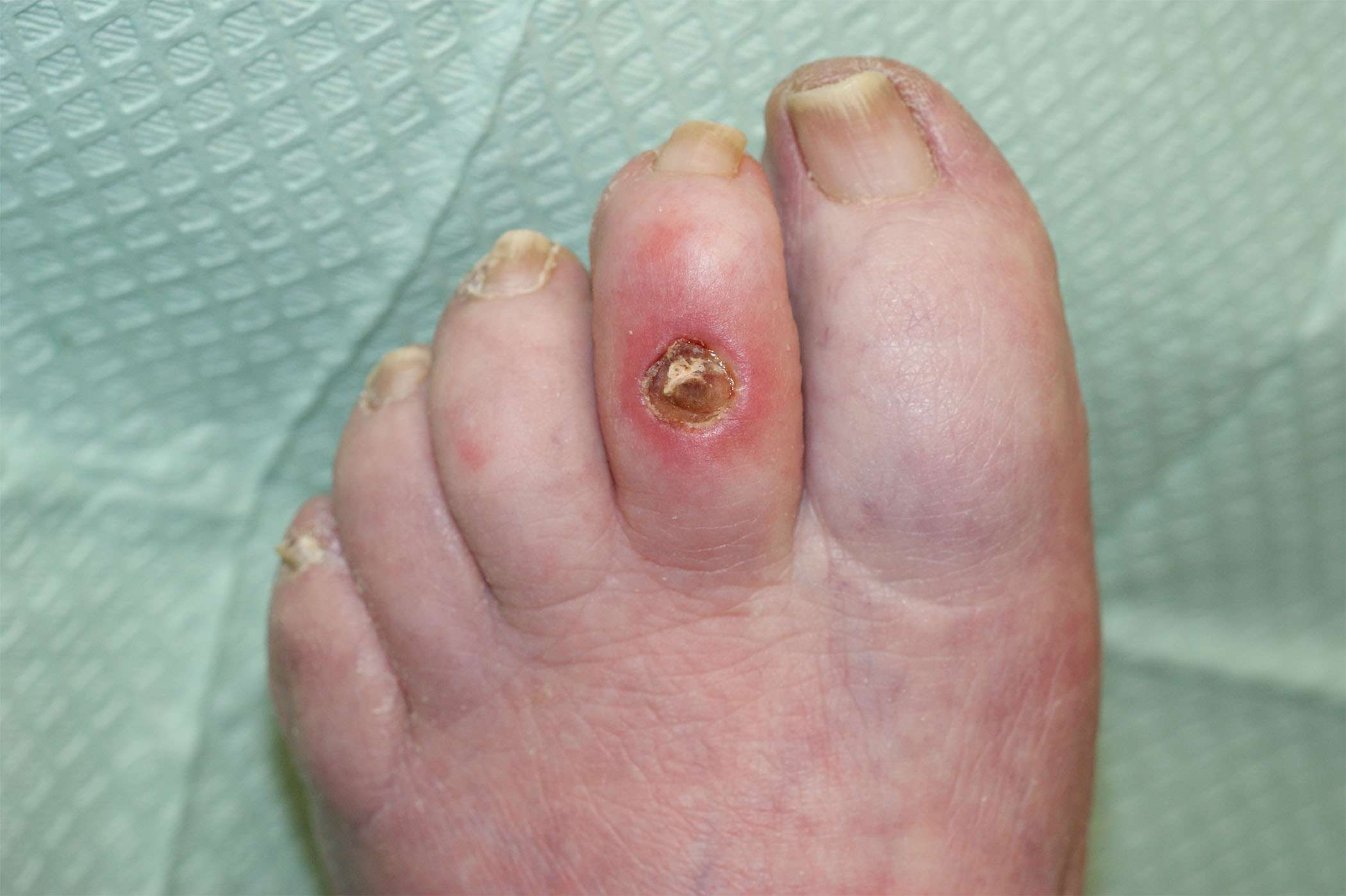
Normally a wound or sore on the skin would cause pain. But the same loss of feeling in the feet that often contributes to the development of a diabetic foot ulcer means that theres often no pain associated with the ulcer. This can make it difficult for people to realize that an ulcer is even there in the early stages, when treatment is most effective.
Aside from pain, another sign to look for is discharge or drainage from the wound in the socks. Ulcers that have been present for some time and that have become infected may also cause an unpleasant odor.
Recommended Reading: How Does One Get Ulcerative Colitis
Diabetic Foot Pain And Ulcers: Causes And Treatment
Diabetic foot pain is common amongst diabetic patients and can become severe when left untreated. Diabetic foot ulcers are the sores that are usually seen on the foot pad and it occurs in around 15% of the diabetic patients. The risk of lower-extremity amputation is increased once the ulcer develops.
Ways To Treat Foot Ulcers
If you are currently experiencing a foot ulcer or think you have a foot wound while diabetic, then its important to seek professional care as soon as possible. This is not a normal wound you can treat at home as foot ulcers go past skin level where you need a professional Podiatrist to treat the wound and see if there are any complications such as infection. The faster you get professional help, the more chances you have in treating your wound. Regular family doctors will usually refer patients with foot ulcers to a professional wound care center where they specialize in foot wounds such as a foot ulcer. A diabetic wound care specialist in California, such as the Wound Institute of America, can provide the most advanced diabetic wound treatment with the latest wound care technology. Your primary doctor can provide a referral for your treatment to be continued at a professional center.
Read Also: Alternative Medicine For Ulcerative Colitis
Evaluation And Treatment Of Diabetic Foot Ulcers
Ingrid Kruse, Steven Edelman Evaluation and Treatment of Diabetic Foot Ulcers. Clin Diabetes 1 April 2006 24 : 9193.
Diabetic foot problems, such as ulcerations, infections, and gangrene, are the most common cause of hospitalization among diabetic patients. Routine ulcer care, treatment of infections, amputations, and hospitalizations cost billions of dollars every year and place a tremendous burden on the health care system.
The average cost of healing a single ulcer is $8,000, that of an infected ulcer is $17,000, and that of a major amputation is $45,000. More than 80,000 amputations are performed each year on diabetic patients in the United States,and 50% of the people with amputations will develop ulcerations and infections in the contralateral limb within 18 months. An alarming 58% will have a contralateral amputation 3-5 years after the first amputation. In addition, the 3-year mortality after a first amputation has been estimated as high as 20-50%, and these numbers have not changed much in the past 30 years,despite huge advances in the medical and surgical treatment of patients with diabetes.
Wet To Dry Dressing Or Simple Saline
This dressing has a good debriding action and helps in wound bed preparation. Wet-to-dry dressings are described in the literature as a means of mechanical debridement. It is very absorptive as well as adherent and one of the cheapest dressings used throughout the world, but requires frequent dressing change based on wound severity. Dressings should be moistened before removal to minimize any chance of bleeding. A gentle cleanser will minimize wound irritation and discomfort. When treating a granulating or epithelizing wound one should soak the dressing thoroughly with normal saline for five minutes to prevent trauma and heavy bleeding.
Also Check: Ulcerative Colitis Flare Up Foods
Where Does An Ulcer Appear
There are many different kinds of ulcers. While peptic ulcers form in the stomach or upper intestine lining, ulcers can also occur almost anywhere on the body.
Ulcers that are found outside the body can include leg and foot ulcers. These ulcers are generally swollen or tender and can cause itchiness or pain. Skin discoloration and changes in texture are also common in ulcers found outside the body.
Whether they are found inside or on the skin’s surface, ulcers are sores that are often slow to heal. Once they have disappeared, ulcers can return if not treated properly. Depending on the cause of the ulcers, they can require different treatment options.
How To Treat Diabetic Ulcers
While prevention plays an integral part in managing physical health conditions, diabetic ulcers can occur even if diabetes is properly managed. Treatment options can vary depending on the symptoms and individual but generally consist of medicine or natural ointments.
Diabetic ulcers are generally slow to treat. Taking pressure off the foot is crucial during the healing process. Contact casting or therapeutic boots are often recommended to reduce swelling and irritation from the ulcer. Bandages and other types of wound dressing can usually be found in local pharmacies.
Medications are sometimes used for diabetic ulcers to normalize glucose and heal any potential infection. Hyperbaric oxygen therapy is one method of treatment that can be used as well as surgical debridement. By removing dead tissue, certain diabetic ulcers can be treated by medical professionals.
Natural ointments are also used for certain types of diabetic ulcers. Since homeopathic treatments that reduce inflammation can help with pain reduction, this can be a beneficial treatment for healing while allowing the individual a level of comfort.
Recommended Reading: How To Treat Skin Ulcer On Leg
Diabetic Wound Care: 6 Ways To Treat Diabetic Foot Ulcers
Neuropathic ulcers, often caused by diabetes, are slow to healeven more so as patients age, if they have longer-term diabetes, or if theyre smokers. Other factors that may stall healing include hypertension, hypercholesterolemia, and abnormal blood sugar levels, often associated with diabetes.
Diabetic ulcers typically occur below the ankle at any site of pressure, friction, shear, or trauma. The wound is likely to be round, with margins often characterized by a periwound callus. The presence of diabetes increases the risk for infection.
Treating neuropathic/diabetic ulcers can be challenging, so be sure to take the following steps to simplify the process and help improve outcomes:
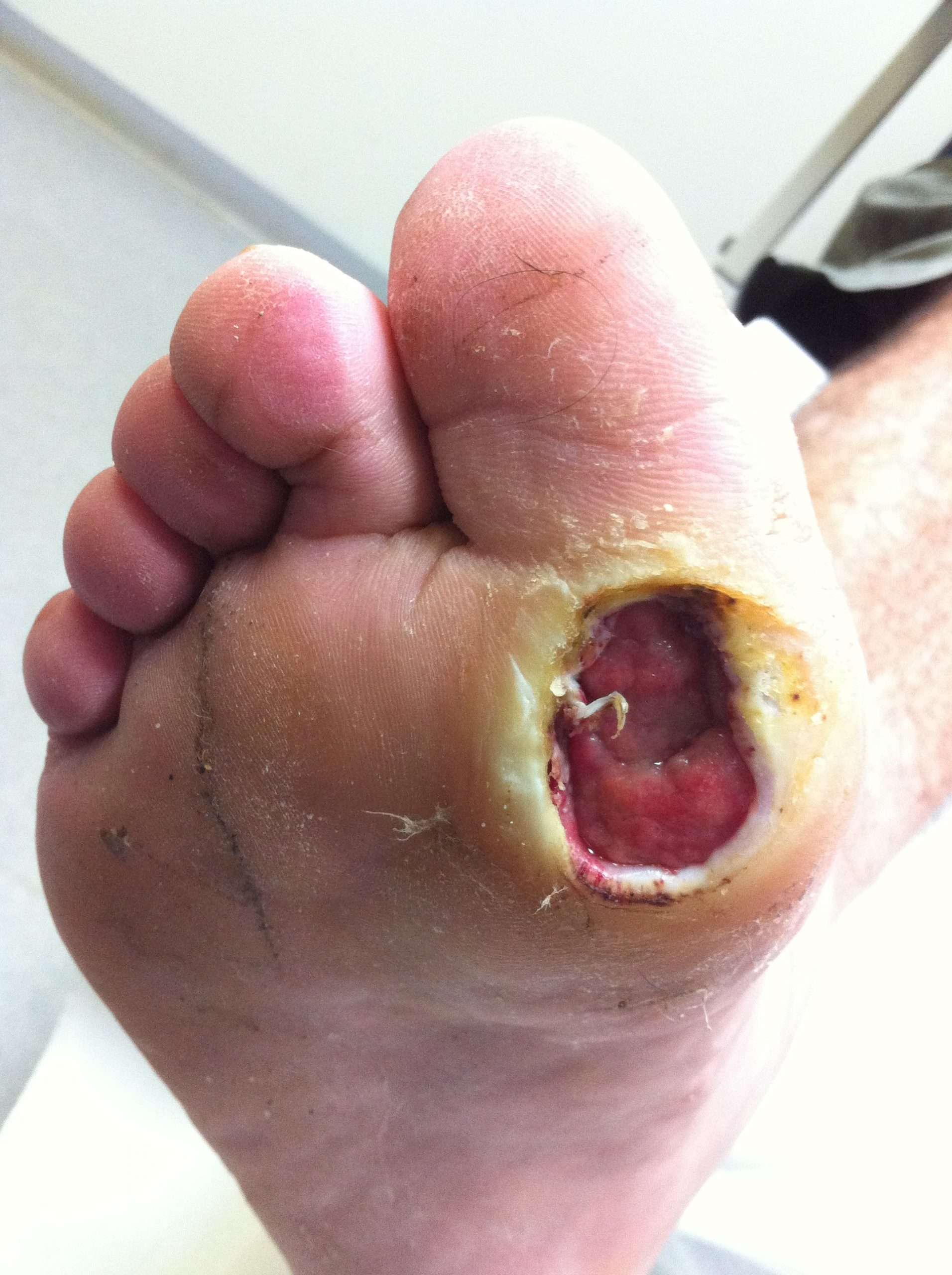
Are You At Risk For A Foot Ulcer
-
Do you have a foot deformity? If so, you may have a higher than average risk of a foot ulcer.
-
Do your shoes rub the wrong way? Poorly fitting shoes are a leading cause of foot ulcers.
-
Can you feel your feet? Diabetes can cause nerve damage to the feet, making it difficult to feel cuts or scratches.
-
Do you have high blood pressure? You may not realize it, but controlling your blood pressure could actually help protect your feet as well as your heart.
-
Have you had a foot ulcer before? If so, youre at higher risk of having another one. Check your feet daily and call your doctor at the first sign of an injury.
-
Do you go barefoot? Wearing shoes both inside and outside can help protect your feet from injury.
-
Can you see your feet? People who are overweight or have diabetic eye disease should ask a family member or caretaker to examine their feet every day.
-
Do you smoke? Ask your doctor for help quitting. Your feet will thank you.
Also Check: Is Kimchi Good For Ulcerative Colitis
How To Treat Diabetic Foot Ulcers
When treating these, the majority of healthcare professionals focus on the actual ulceror the wound itself. However, treating the wound alone is simply addressing a problem with the skin. If you think about it, you have skin all over your foot. Whats the difference between the skin where there is no ulcer versus the skin where there is an ulcer? The answer is, Nothing. It is not that the skin is weaker where the ulcer is. It is just that the pressure or forces in the specific location of the ulcer are stronger. Clearly, the wound needs to be treated but failure to address the pressure or force that caused the ulcer in the first place, is shortsighted and doomed to fail.
2. Our patients have a lower recurrence rate of diabetic foot ulcers.
Since most practitioners rarely address the cause of the problem the recurrence rate of diabetic foot ulcers is anywhere from 30-70% in as little as one year.This is true with or without special diabetic shoes. If you have a foot ulcer and nothing is done to address the shear forces or pressure forces that caused the ulcer in the first place, the risk of having another foot ulcer, or never healing the original ulcer in the first place, is incredibly high. This is why some people have foot ulcers for years.
3. Our podiatrists educate the patients and utilize a wide range of treatments.
Most important thing to remember:
Praise For Emuaid From Satisfied Customers
We are very thankful for the early arrival of your fine product. My sister, in less than 24 hours, is now completely Pain free. Very, very grateful,*
Dennis L F
I use Emuaid for my skin condition that causes constant itching. Since using Emuaid the itching is completely gone. Its a great product!*
Theresa S.
Emuaid max is a great product that I have bought several times.I am diabetic and it is slow healing but it does help alot*
Anonymous Customer
I am so glad I found this cream to help my husband, in one week I could see a big different. Today we had a Doctor appoinment , she was so surprise how it got better, she took me to the computer to show me the picture from last week and now what a different, I just have to tell her about your cream, she said , she never heard about this cream. I strongly recomend r*
David J
It is the only meds that i have ever found that totally works. the shopping exp, was awesome thanks*
Maggie T.
This stuff is so good. I got the extra strength this time. I am assured that it will work as well or better. Nothing I have tried before worked until I discovered this product. Its a miracle in a jar.*
Paul
Show/Hide all customer reviews +
D. G.
My order came within the promised time and my sore parts were better in 2 days. I cant wait to try it on other skin issues to test its effectiveness. When I talk to my Dr. again I am going to suggest he recommend this to his patients with any skin ailment.*
ElizabethLucyRalphAliceRolandAlbieFred
Read Also: Does Apple Cider Vinegar Help Ulcerative Colitis
Preventing Diabetic Foot Ulcers
There are several ways to prevent a foot ulcer. In addition to daily checks of your feet for any signs of an ulcer or other abnormality, the following can be done to help with prevention:
- Never walk barefoot, and always wear socks to protect your feet
- Wear shoes that fit properly and do not rub
- Keep your blood sugar under control and monitored
- Eat a healthy diet
- Avoid alcohol and tobacco products
- Seek immediate medical attention if you have a foot wound that is not healing
A Note From Cleveland Clinic
Foot and toe ulcers take longer to heal the longer theyre ignored. If you dont get treatment for your ulcer, it may get bigger and deeper, get infected or cause you to be unable to use your feet correctly. Remember that ulcers can return after treatment. In fact, you have a 50% chance of getting another one within three years of the first. See a podiatrist for your ulcer as soon as possible.
Also Check: Ulcerative Colitis Surgery J Pouch
Types Of Diabetic Ulcers
There are several types of diabetic foot ulcers
- Neuropathic ulcers occur where there is peripheral diabetic neuropathy, but no ischemia caused by peripheral artery disease.
- Ischemic ulcers occur where there is peripheral artery disease present without the involvement of diabetic peripheral neuropathy.
- Neuroischemic ulcers occur where the person has both peripheral neuropathy and ischemia resulting from peripheral artery disease.
Arriving at the correct diagnosis and identifying the cause of a diabetic ulcer is critical since it affects the treatment plan.
What Causes Diabetic Foot Ulcer
People with diabetes have an increased chance of developing foot ulcers because you are more likely than other people to damage the skin on your feet. This is because diabetes can cause nerve damage, so you don’t notice if your foot is injured or sore. Diabetes also causes blood vessel damage so your skin can’t heal easily.
You May Like: Sample Meal Plan For Ulcerative Colitis
When You Need More Treatment
If your wound doesnât heal in about a month or becomes an infection that spreads to the bone, you may need other treatments. These can include surgery and hyperbolic oxygen therapy, which involves breathing pure oxygen in a special room in order to help your body heal.
If your ulcer develops gangrene and your tissue dies, your doctor may have to amputate that area of your body.
Who Gets Foot And Toe Ulcers
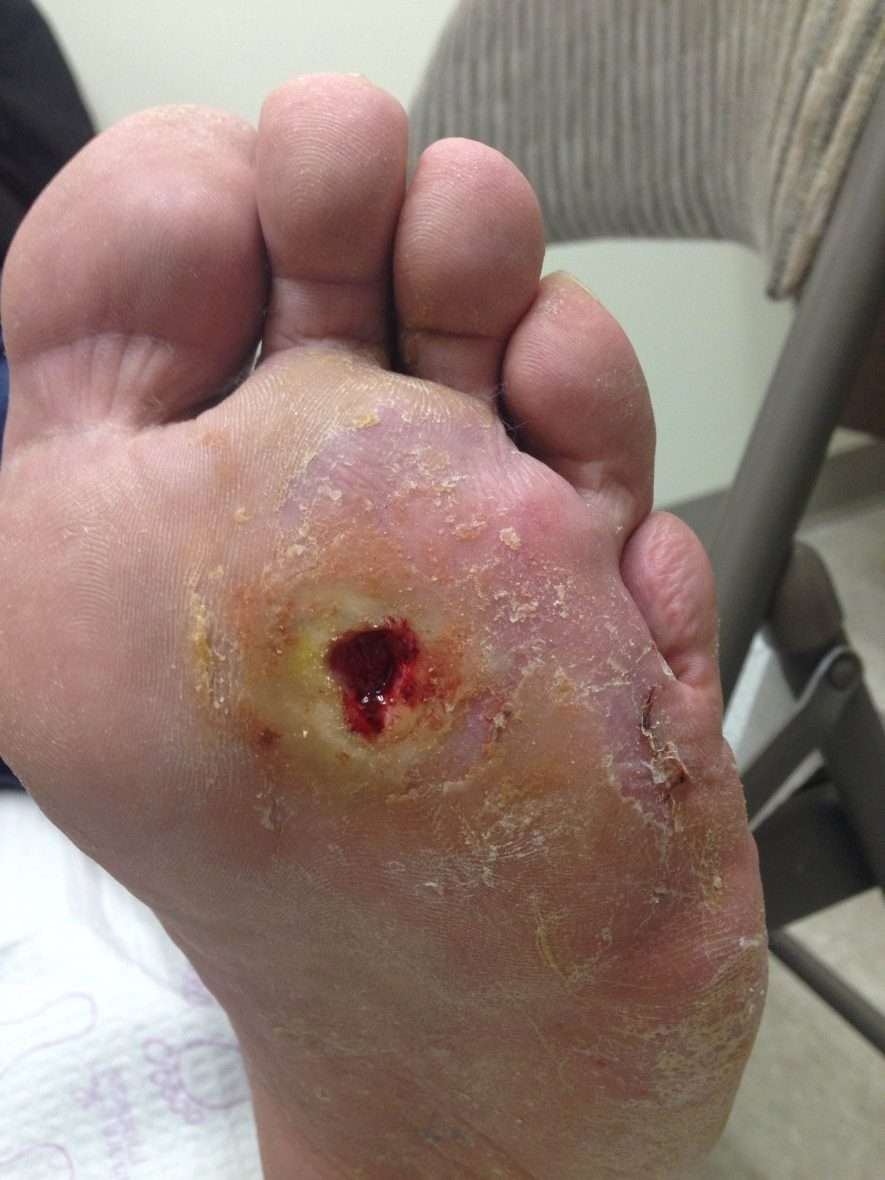
You’re at higher risk for foot and toe ulcers if you are:
- Native American.
- Male.
- Elderly.
If you have an eye, kidney or heart disease related to diabetes, youre also at a higher risk. About 15% of people with diabetes will get an ulcer, typically on the bottom of their foot. Around 6% of that 15% will have to be hospitalized because of complications.
Youre also at a higher risk of getting foot and toe ulcers if you have any of the following:
- Problems with circulation.
- A foot deformity like a bunion or hammertoe.
- Kidney disease.
- Use alcohol.
Recommended Reading: Is Omeprazole Good For Ulcers
Why Are Diabetics Prone To Foot Ulcers And Other Chronic Wounds
Diabetic patients are more prone to developing chronic wounds for a few reasons. Two of the most influencing factors are nerve damage and blood circulation issues that are common among diabetic patients.
Nerve damage, or neuropathy, tends to occur in patients who have a longer history with diabetes because elevated blood glucose levels damage nerves over time. Neuropathy causes patients to experience reduced, or lack of, sensation in the areas affected.
Many patients can sustain trauma or develop an infection without realizing it because theyre unable to feel pain in the area. Further, neuropathy commonly affects the feet, so a wound on the bottom of the foot can escalate quickly because the patient cannot feel or see the wound easily.
Blood circulation issues also can increase the risk for developing chronic wounds, as well as making the wounds more prone to infection. High blood glucose levels cause the narrowing of blood vessels, which constricts blood supply, Estocado said. Adequate blood supply is essential to normal wound healing. The secondary effect of impaired blood supply is a decrease in white blood cells, which are responsible for fighting infection and maintaining a strong immune system.