Skin Grafts For Diabetic Ulcer Treatment
When a diabetic ulcer does not improve after conservative treatment, your podiatrist may use a skin graft as a sort of bandage. Skin grafts close wounds and help them heal. Traditionally, skin grafts are done in a hospital setting under general anesthesia. However, diabetic ulcers can often be treated with biosynthetic skin substitutes that are grown in a lab and applied on an outpatient basis.
When you come to the office, your doctor will first clean the ulcer and then debride the wound, which means cutting off all the dead skin with surgical tools to make sure no infection remains and the wound is clean.
The doctor will then apply the biosynthetic skin, which looks a bit like a square of tissue paper. While it might not look like much, this miraculous bit of bioengineering covers and protects your wound, bonds to your skin, and promotes healing.
Finally, the doctor will bandage the area in gauze to keep it clean. It can take several treatments before your ulcer is completely healed, and you may also wear a boot during that time to help keep pressure off the ulcer.
How Do You Treat A Diabetic Ulcer
by kevdev | Feb 12, 2019 | Podiatry Issues
An ulcer is a condition that can occur in any patient with diabetes. Diabetic ulcers are sores which occur typically on the foot or ankle. The ulcer is caused secondary to friction which leads to a breakdown in skin. Diabetic patients will typically have a loss of feeling in their foot and legs, so they do not feel the repetitive irritation that leads to a wound. I typically will see patients that have wounds that are caused by improper shoes, trauma, or a foot deformity that causes excess pressure over a bone. Decreased blood flow can also lead to an ulcer and makes healing the ulcer more difficult.
How do you treat a diabetic ulcer?
I treat diabetic ulcers through a multi-pronged approach. On your first evaluation we will take a detailed history of the wound and perform a thorough exam of your foot/ankle. We then will develop a treatment plan to address the following issues:
Pressure: We must remove pressure which causes the breakdown of the skin. The constant pressure causes injury to the cells which are trying to fill the wound with healthy tissue and skin. We offload the wound with special padding, shoe modification, wearing special boots, or using crutches/wheel chairs to keep all weight from the foot.
How To Prevent Diabetic Foot Ulcers
The first line of defense in preventing diabetic wounds is to follow the guidelines recommended to keep the disease itself under control:
- Maintain healthy blood sugar levels through a healthy diet and by taking medications as instructed by your doctor.
- Keep your blood pressure within a healthy range.
- Avoid alcohol and tobacco.
You should also take measures to avoid causing sores or wounds on the feet:
- Never walk barefoot.
- Wear shoes that fit properly and dont rub the skin.
- Wash your feet daily with mild soap and lukewarm water to prevent the buildup of bacteria on the skin, which can cause infection even in the tiniest skin breaks.
Because a loss of sensation in the feet may mean theres no pain felt even when an ulcer is present, its also extremely important for those with diabetes to regularly check for any foot sores or skin irritation. This way, the ulcer can be properly treated as early as possible.
You May Like: Ulcerative Colitis And Kidney Stones
How Can I Reduce My Risk Of Foot And Toe Ulcers
There are several things you can do to help reduce your risk of getting foot and toe ulcers. Sometimes, adopting these habits can even stop them from coming back. Try to:
- Manage your diabetes. If you have diabetes you should wear appropriate footwear and never walk barefoot.
- Examine your legs as well as the tops and bottoms of your feet and the areas between your toes every day. Look for any blisters, cuts, cracks, scratches or other sores. Also check for redness, increased warmth, ingrown toenails, corns and calluses. Use a mirror to view your leg or foot if necessary. If its difficult to see, ask a family member to look at the area for you. See a healthcare provider immediately if you notice any problems.
- Talk to your healthcare provider about ways you can stop smoking.
- Manage your blood pressure.
- Control your cholesterol and triglyceride levels by changing your diet. Limit salt in your diet.
- Care for your toenails frequently. Cut your toenails after bathing, when they are soft. Cut toenails straight across and smooth with a nail file. Take care of ingrown toenails.
- Exercise.
- Wear appropriate shoes and socks. Talk to your podiatrist about what you need.
What Is The Treatment For Diabetic Wounds
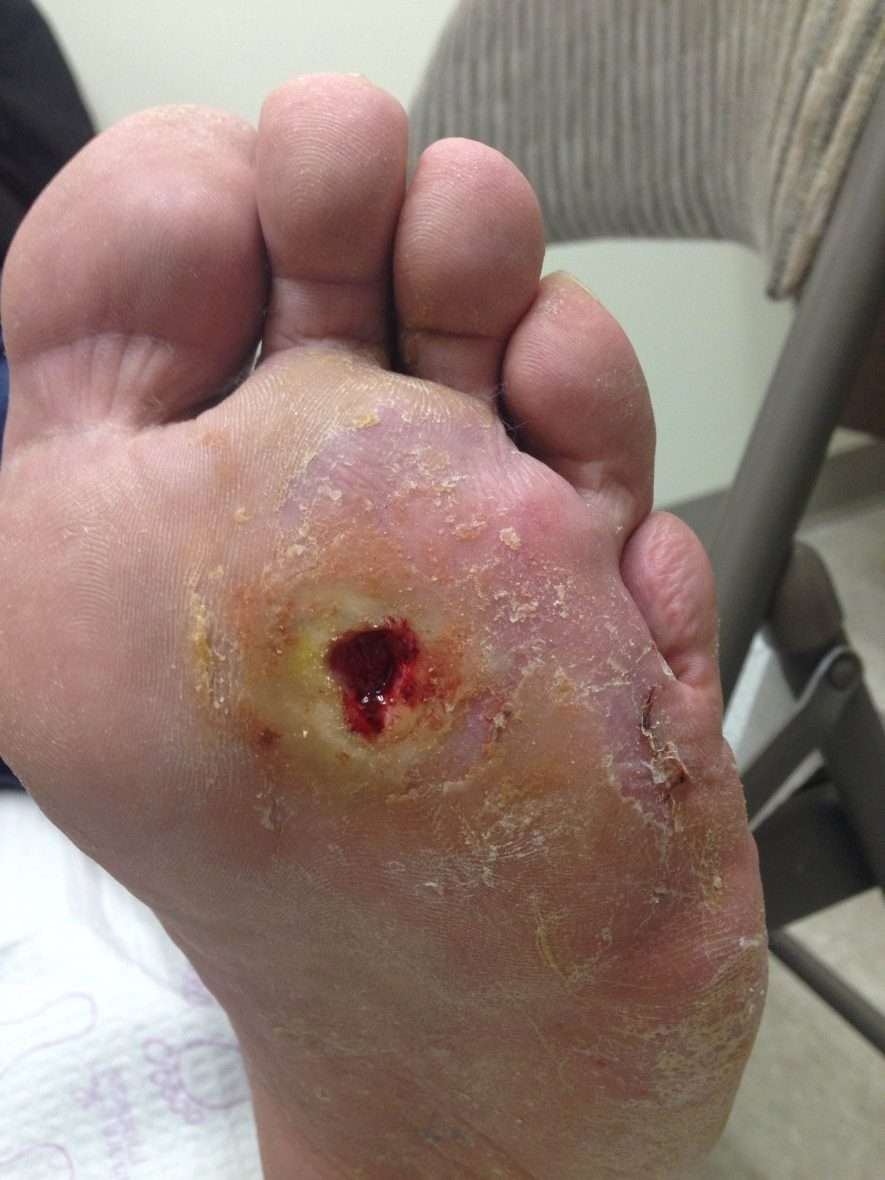
The management of diabetic foot ulcers requires offloading the wound, daily saline or similar dressings to provide a moist wound environment, débridement when necessary, antibiotic therapy with or without surgical intervention if osteomyelitis or soft tissue infection is present, optimal control of blood Oct 15, 2020.
Also Check: What To Eat With Stomach Ulcer
Symptoms Of Stomach Ulcers
Although the most common symptom of a stomach ulcer is a burning or gnawing pain in the centre of the abdomen . Not all stomach ulcers are painful.
Some people experience:
Speak to your GP immediately if:
- your symptoms persist
- youre vomiting blood the blood can appear bright red or have a dark brown, grainy appearance like coffee grounds
- youre passing dark, sticky, tar-like stools
- you feel a sudden, sharp pain in your tummy that gets steadily worse
These could be a sign of a serious complication.
Also Check: How To Treat Mouth Ulcers
How Do You Treat A Diabetic Foot Ulcer
If a patient suspects they have a diabetic foot ulcer, they should seek treatment from a podiatrist immediately. Because diabetes and diabetic neuropathy can slow healing, itâs critical to be seen as soon as possible. Their doctor may do a number of things to treat the diabetic foot ulcer, including: âoffloadingâ or taking pressure off of the foot, âdebridementâ where dead skin and tissue is removed, wound care like medications and dressing, early administration of antibiotics to prevent infection.
Read Also: What Are The Early Signs Of An Ulcer
S To Prevent Diabetic Foot Ulcers
What Are The Causes Of Peptic Ulcers
The most common causes of peptic ulcers has been found to be Helicobacter pylori infection which invade the intestinal lining and damage it while proliferating. Also, indiscriminate use of NSAIDs has found to precipitate peptic ulcers.
Alcohol & tobacco intake as well as consumption of oily, spicy foods may worsen the condition of peptic ulcers, but has not been found to cause them. The most common, first line treatment for ulcers is administration of antacids and proton pump inhibitors which dilute the concentration of acid secretions in the stomach or reduce the acid production respectively.
Also Check: Over The Counter For Ulcers
Also Check: What Is An Infusion For Ulcerative Colitis
How Is Gastroparesis Treated
Gastroparesis is a chronic condition. This means that treatment usually doesnt cure the disease, but you can manage it and keep it under control. People who have diabetes should try to control their blood glucose levels to reduce the problems of gastroparesis.
Some people may benefit from medications, including:
- Reglan: You take this drug before you eat, and it causes your stomach muscles to contract to help move food out of your stomach. Reglan also helps cut down on vomiting and nausea. Side effects include diarrhea and, rarely, a serious neurological disorder.
- Erythromycin: This is an antibiotic that also causes stomach contractions and helps move food out. Side effects include diarrhea and development of resistant bacteria from taking the antibiotic for a long time.
- Antiemetics: These are drugs that help control nausea.
Surgery for gastroparesis
People with gastroparesis who still have nausea and vomiting even after taking medications may benefit from surgery. One type of surgery for gastroparesis is gastric electrical stimulation, which is a treatment that sends mild electric shocks to your stomach muscles. In this procedure, your provider inserts a small device called a gastric stimulator into your abdomen. The stimulator has two leads that are attached to your stomach and provide mild electric shocks, which help control vomiting. Your provider can adjust the strength of the electric shocks. The device runs on a battery that lasts up to 10 years.
What Kinds Of Diabetic Ulcers Are There
There are several kinds of diabetic ulcers, but here we break them into three primary groups:
Neuropathic ulcers
There form in areas with peripheral diabetic neuropathy, but no ischemia caused by peripheral artery disease.
Neuroischemic ulcers
These can form in areas afflicted by both peripheral neuropathy and ischemia resulting from peripheral artery disease.
Ischemic ulcers
These form because peripheral artery disease is present without the involvement of diabetic peripheral neuropathy.
Don’t Miss: What Over The Counter Medicine Is Good For Ulcers
Preventing & Curing Diabetic Ulcers With Wellstar Wound Care
When someone is diabetic, a small wound can escalate into a major health issue and, in many cases, lead to an amputation. However, with proper wound care and accelerated healing with hyperbaric medicine, Wellstar patients are partnering with providers to treat wounds like diabetic foot ulcers.
Diabetic foot ulcers can develop if diabetes is not well-managed, and some causes of ulcers include poor circulation and high blood sugar. Ulcers may go unnoticed at first because many people with diabetes are also affected by neuropathy and do not have feeling in their feet, said Dr. Ricardo Duran, Medical Director of the Wound Care and Hyperbaric Medicine Department at Wellstar North Fulton Hospital.
Also, if a diabetic person gets a wound, it may not heal as quickly, as people with diabetes are more likely to also experience poor circulation, immune system deficiencies and elevated blood sugar levels.
When you combine the lack of sensation in the foot with the lack of healing, that leads to even more damage, Dr. Duran said.
Foot ulcers should be taken seriously when a diabetic person has an open wound, their five-year mortality rate increases by about 32%, according to Dr. Duran.
Praise For Emuaid From Satisfied Customers
We are very thankful for the early arrival of your fine product. My sister, in less than 24 hours, is now completely Pain free. Very, very grateful,*
Dennis L F
I use Emuaid for my skin condition that causes constant itching. Since using Emuaid the itching is completely gone. Its a great product!*
Theresa S.
Emuaid max is a great product that I have bought several times.I am diabetic and it is slow healing but it does help alot*
Anonymous Customer
I am so glad I found this cream to help my husband, in one week I could see a big different. Today we had a Doctor appoinment , she was so surprise how it got better, she took me to the computer to show me the picture from last week and now what a different, I just have to tell her about your cream, she said , she never heard about this cream. I strongly recomend r*
David J
It is the only meds that i have ever found that totally works. the shopping exp, was awesome thanks*
Maggie T.
This stuff is so good. I got the extra strength this time. I am assured that it will work as well or better. Nothing I have tried before worked until I discovered this product. Its a miracle in a jar.*
Paul
Show/Hide all customer reviews +
D. G.
My order came within the promised time and my sore parts were better in 2 days. I cant wait to try it on other skin issues to test its effectiveness. When I talk to my Dr. again I am going to suggest he recommend this to his patients with any skin ailment.*
ElizabethLucyRalphAliceRolandAlbieFred
You May Like: What Is The Best Medicine For Mouth Ulcer
How Are Foot And Toe Ulcers Diagnosed
Your healthcare provider can tell what type of ulcer you have based on four observations:
- The appearance of the ulcer.
- Location of the ulcer.
- The appearance of the borders.
- The appearance of the surrounding skin.
Your primary healthcare provider can diagnose an ulcer, but they might send you to a specialist for treatment. You might see a podiatrist, a provider who works with feet, or a wound specialist. For more complicated cases that require surgery, you might also see a plastic surgeon, anesthesiologist, orthopedic surgeon and/or vascular surgeon.
Healing Tips For Diabetic Wound Care And Ulcers Of The Foot
Patients with diabetes can be at risk for diabetic foot ulcers, infections, and complications from those infections. Diabetic foot ulcers or wounds put patients at a higher risk of hospitalization and need for surgery or amputation. In fact, according to the CDC, there are 130,000 hospitalizations a year for amputations in those with diabetes. Up to 11.8% of those with diabetes have a wound and many may go on to need surgery. This means that wound care for diabetic foot ulcers as well as prevention is of the utmost importance.
As physicians, we have to use our resources and work with patients in order to heal diabetic foot wounds to prevent such complications. If a patient also has numbness in their feet, they may not feel a foot wound developing. Diabetic foot sores that start from a small scrap or cut can unknowingly form into a deep ulcer. Checking your feet and keeping your blood sugar
Whether you have diabetes or are caring for a loved one requiring foot diabetic wound treatment, Certified Foot and Ankle Specialists can effectively help your wound heal and prevent further complications. Here we will discuss diabetic foot care and how to minimize the traumatic consequences of ulcers.
How do we care for diabetic foot wounds and how does one clean a diabetic foot wound?
For proper wound care, clean the wound with saline, apply a topical gel or antibiotic ointment medication to the wound once a day, as recommended by your doctor.
Preventing diabetic wounds
Don’t Miss: Diabetic Foot Ulcer Treatment Guidelines
What Are Peptic Ulcers
Peptic ulcers, also called as stomach ulcers, are characterized by the occurrence of an open sore on the inner lining of the stomach. The sore may be on the proximal, middle or distal part of the stomach or in the duodenum, the initial part of small intestine, following the stomach.
Diseases of the gastro-intestinal tract such as peptic ulcers and dyspepsia are quite common among the urban population today due to improper eating habits and erratic lifestyle adopted due to the influence of technology. People today have chosen jobs involving prolonged hours of sitting in front of the PC and often skipping meals, which is quite common due to busy working hours.
Irregular meal timings combined with having large meals at a time all play a role in disturbing the functioning of the normal digestive system. Paying proper attention to regularizing meal timings & minding the portion size of meals can help reverse gut disorders such as peptic ulcers.
Ulcers are often the result of inadequate presence of the bicarbonate ions in the stomach lining. Hence, on account of inadequate bicarbonate ions to neutralize the H+ ions in the acidic secretions of the gut, the stomach acid has the capacity of corroding the stomach lining. This gives rise to ulcers.
Foot Care Tips To Prevent Diabetic Foot Ulcers
Along with controlling your blood glucose levels, these basic foot care tips can help reduce your risk of foot ulcers and improve your overall health.
1. Inspect your feet every day. You may not have the flexibility to see the bottoms of your feet, or you may not see well. If this is the case, have your spouse or a family member inspect your feet and shoes for cuts, bruises, cracks, blisters, redness, or other signs of an abnormality. Call your doctor if you notice even a small wound the earlier we can help, the better.
2. Show your doctor your feet. Remove your shoes and socks when you visit your primary care doctor. Ask them to examine your feet for nerve damage and circulation, even if they dont initiate the request.
Don’t Miss: What Pain Reliever Is Safe For Stomach Ulcer
Complications Of Untreated Diabetic Ulcers
If a diabetic ulcer is not adequately treated, the risk of infection can significantly increase. Abscesses, the spread of disease, gangrene, and eventual amputation are all possible outcomes of poorly treated or neglected diabetic ulcers.
Diabetic foot ulcers can quickly become severe conditions. By treating them as soon as possible, the condition can be remedied before the chance of infection. Serious wounds will not go away on their own and will require prompt attention.
Fortunately, diabetic ulcers can be easily detected. Unlike ulcers that form on the inside of the body, these wounds can be seen and felt. A diabetic ulcer’s symptoms include foot pain, discoloration or numbness, and a deepening wound that will not heal with time. Diabetic ulcers occur in those who have diabetes. The diagnosis of diabetes combined with painful wounds on the bottom of the feet is a good indication that a diabetic ulcer needs treatment.
What Can Caregivers And Loved Ones Do To Contribute To Prevention
Education and instruction on the proper process for general foot care should be available to the patient and family, especially anyone who carries the most responsibility for daily care. General foot care steps include:
- Daily foot washing
- Drying the feet thoroughly
- Proper moisturization
If the patients feet are not sweating or visibly dirty, a little means a lot when it comes to soap. Older patients already have reduced natural body oil, so it is necessary to preserve the moisture that is there. Moisturizing soaps are recommended. If bedside bathing is necessary, a few drops of baby oil can be added to the water for extra moisturization followed by moisturizing lotion after the body has been patted dry. Getting dressed for the day after moisturizing is important, as the clothing will easily slide over the lotioned limbs.
Do not apply moisturizer between the toes of the foot, as this can promote fungal growth. If excessive feet sweat is an issue, roll-on antiperspirant can be applied to the soles of the feet before putting on socks.
Socks and shoes should always be worn whether the patient is in a wheelchair or not. Footwear is not for walking, but for protection, in diabetics. Shoes are barriers between toes and items a patient may kick accidentally and a support structure. Footrests should be kept on wheelchairs. When the patient is pushed, they may be dragging their feet and not even realize it, and an injury can be sustained.
You May Like: What Not To Eat With Bleeding Ulcers