How Are Leg Ulcers Diagnosed
A vascular specialist a healthcare provider specializing in the circulatory system and knowledgeable about wound care can examine the ulcer. Your provider will examine your skin and the wound.
You may also get:
- Ankle-brachial index test, which uses ultrasound technology to measure blood pressure and blood flow in the legs.
- Biopsy to check skin cells and fluid from the wound for infections and skin diseases.
Referral To A Specialist
In some cases, your GP or nurse may decide to refer you to a specialist in conditions affecting the blood vessels .
For example, you may be referred to a vascular specialist if your GP or nurse is unsure about your diagnosis, or if they suspect your ulcer may be caused by artery diseases, diabetes or rheumatoid arthritis.
After taking your medical history and examining you, the vascular specialist may need to arrange further investigations to plan your treatment.
Causes Of Venous Ulcers
Venous ulcers most often form around the ankles.
Venous ulcers typically occur because of damage to the valves inside the leg veins. These valves control the blood pressure inside the veins. They allow it to drop when you walk. If the blood pressure inside your leg veins doesn’t fall as you’re walking, the condition is called sustained venous hypertension. That increase in blood pressure causes ulcers to form on your ankles.
Venous ulcers may also be caused by other problems with your leg veins. These include:
-
Varicose veins. These are large, bulging leg veins. They occur when valves in the leg veins dont work well, allowing blood to collect in the lower leg.
-
Chronic venous insufficiency. Like varicose veins, this condition occurs when your leg veins cant pump blood back up to your heart. Blood then pools in your lower legs, causing your legs to swell. Since the blood can’t flow well in your legs, the swelling may be extreme. This extreme swelling can put so much pressure on your skin that venous ulcers form.
Recommended Reading: Can Gluten Intolerance Cause Ulcerative Colitis
How We Vet Brands And Products
Healthlineonly shows you brands and products that we stand behind.
- Evaluate ingredients and composition:Do they have the potential to cause harm?
- Fact-check all health claims:Do they align with the current body of scientific evidence?
- Assess the brand:Does it operate with integrity and adhere to industry best practices?
What is stasis dermatitis?
Stasis dermatitis is skin inflammation that develops in people with poor circulation. It most often occurs in the lower legs because thats where blood typically collects.
When blood collects or pools in the veins of your lower legs, the pressure on the veins increases. The increased pressure damages your capillaries, which are very small blood vessels. This allows proteins to leak into your tissues. This leakage leads to a buildup of blood cells, fluid, and proteins, and that buildup causes your legs to swell. This swelling is called peripheral edema.
People with stasis dermatitis usually experience swollen legs and feet, open sores, or itchy and reddish skin.
The symptoms of stasis dermatitis include:
- skin discoloration
You may also experience symptoms of venous insufficiency, including:
- calf tenderness
- a dull ache or heaviness in your legs that gets worse when you stand
In the early stages of stasis dermatitis, the skin on your legs may look thin. Your skin may also itch, but try not to scratch it. Scratching can cause the skin to crack and fluid to seep out.
Signs And Causes Of Venous Ulcers
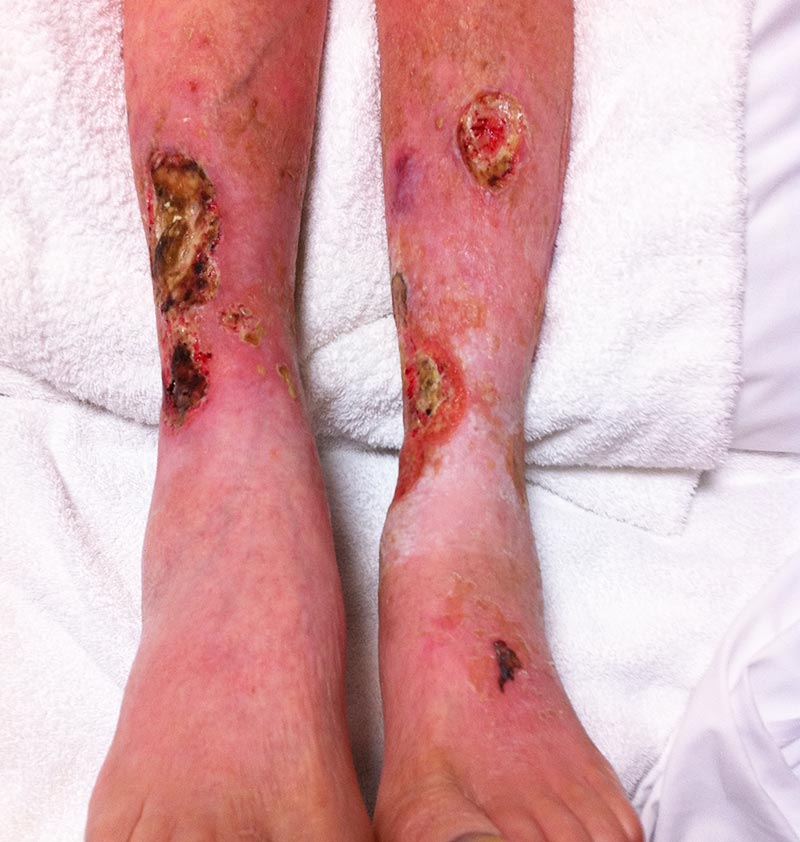
Venous ulcers are non-healing or slow-healing wounds that form as a result of blood pooling in the legs and feet. This happens when the walls or valves in the veins of the lower extremities dont work effectively. This is called venous insufficiency.
Venous ulcers are more common in women and older people. Several factors increase your risk of developing venous ulcers, including:
- Long periods of immobility, such as bed rest
You May Like: What Are The 4 Stages Of Pressure Ulcers
You May Like: Where Does It Hurt When You Have An Ulcer
What Are The Treatments For Poor Leg Circulation
Poor leg circulation is a common problem, especially as we age. Fortunately, there are simple habits and lifestyle changes you can make to reduce pain associated with poor circulation in legs. While its important to consult with your doctor, here are some ways you can improve circulation in your legs at home:
What Are Foot Ulcers
A foot ulcer is an open sore on the foot.
A foot ulcer can be a shallow red crater that involves only the surface skin. A foot ulcer also can be very deep. A deep foot ulcer may be a crater that extends through the full thickness of the skin. It may involve tendons, bones and other deep structures.
People with diabetes and people with poor circulation are more likely to develop foot ulcers. It can be difficult to heal a foot ulcer. In people with these conditions, even a small foot ulcer can become infected if it does not heal quickly.
If an infection occurs in an ulcer and is not treated right away, it can develop into:
- A spreading infection of the skin and underlying fat
- A bone infection
- Gangrene. Gangrene is an area of dead, darkened body tissue caused by poor blood flow.
Among people with diabetes, most severe foot infections that ultimately require some part of the toe, foot or lower leg to be amputated start as a foot ulcer.
Foot ulcers are especially common in people who have one or more of the following health problems:
- Peripheral neuropathy. This is nerve damage in the feet or lower legs. Diabetes is the most common cause of peripheral neuropathy. When nerves in the feet are damaged, they can no longer warn about pain or discomfort. When this happens, tight-fitting shoes can trigger a foot ulcer by rubbing on a part of the foot that has become numb.
In addition to diabetes, other medical conditions that increase the risk of foot ulcers include:
You May Like: Diet Plan For Ulcerative Colitis Flare Up
Are Other Venous Ulcer Treatments Available
Venous ulcers that are severe or not responding to standard therapies may require additional treatments such as:
- Growth factor therapy, injectable substances that attract healthy cells to ulcers.
- Hyperbaric oxygen therapy, a treatment in which you sit in a special, pressurized chamber and inhale pure oxygen.
- Lymphedema therapy, massage, skin care and bandaging techniques that clear fluid buildup.
- Skin graft, replacing diseased skin with healthy skin from another part of your body.
- Stem cell therapy, injections of bone marrow to generate healthy tissue.
- Venous disease treatment to correct blood pooling problems and improve circulation.
- varicose veins in the leg.
Manage Your Blood Sugar Levels
One of the most important things you can do to treat diabetic ulcers is to keep your blood sugar levels under control by monitoring them on a regular basis.
You can also help treat and prevent high blood sugar levels by following a healthy diet, exercising regularly, and taking any medication prescribed by your doctor.
You May Like: In Order To Prevent Pressure Ulcers
Chronic Leg Ulcers: Epidemiology Aetiopathogenesis And Management
Shubhangi Vinayak AgaleAcademic Editor: Received
Abstract
Chronic leg ulcer is defined as a defect in the skin below the level of knee persisting for more than six weeks and shows no tendency to heal after three or more months. Chronic ulceration of the lower legs is a relatively common condition amongst adults, one that causes pain and social distress. The condition affects 1% of the adult population and 3.6% of people older than 65 years. Leg ulcers are debilitating and greatly reduce patients’ quality of life. The common causes are venous disease, arterial disease, and neuropathy. Less common causes are metabolic disorders, hematological disorders, and infective diseases. As many factors lead to chronic lower leg ulceration, an interdisciplinary approach to the systematic assessment of the patient is required, in order to ascertain the pathogenesis, definitive diagnosis, and optimal treatment. A correct diagnosis is essential to avoid inappropriate treatment that may cause deterioration of the wound, delay wound healing, or harm the patient. The researchers are inventing newer modalities of treatments for patients with chronic leg ulceration, so that they can have better quality life and reduction in personal financial burden.
1. Introduction
2. Epidemiology
3. Aetiopathogenesis
4. Pathogenesis of Chronic Leg Ulcers
4.1. Venous Ulcers
4.2. Arterial Ulcers
4.3. Diabetic Foot Ulcer
4.4. Pressure Ulcer
5. Management of Chronic Leg Ulcers
5.1. Clinical Assessment
Medical History And Examination
Your GP or practice nurse will ask whether you have any other symptoms associated with venous leg ulcers, such as:
- swelling in your ankles
- discoloured or hard skin
They’ll try to determine the cause of the ulcer by asking about underlying conditions or previous injuries, such as:
Read more about how venous leg ulcers are treated.
Recommended Reading: Does Smoking Cause Ulcers After Gastric Bypass
Diagnosis Of Leg Ulcers
- examine the wound
- perform some tests to measure the blood flow in your lower leg, such as the ankle-brachial index. This test compares blood pressure readings taken at the ankle and at the arm using a device called a Doppler machine
- recommend an angiogram for an arterial ulcer, to find out if the artery needs surgery to clear the blockage.
What Causes Leg Ulcers
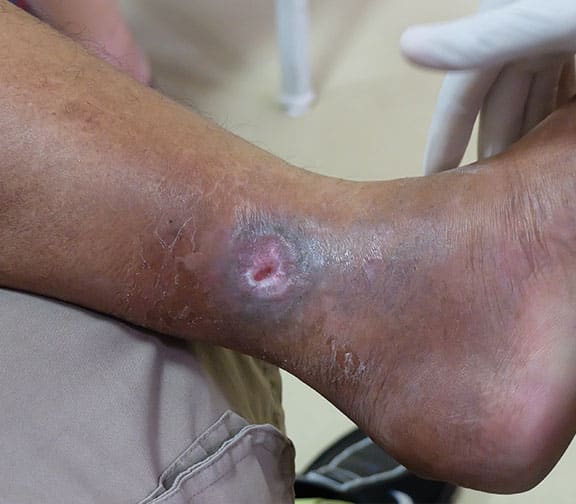
Causes of leg ulcers include:
- Chronic venous insufficiency: Chronic venous insufficiency occurs when faulty valves in leg veins allow blood to flow backward into the leg where it pools. If you develop high blood pressure in the leg veins, tiny blood vessels can burst, causing inflammation, itching and dry skin. Leg ulcers develop when the skin breaks open.
- Diabetes: High blood sugar levels from diabetes can cause fat deposits to form inside blood vessels, causing them to narrow. Reduced blood flow can cause nerve damage or diabetic neuropathy. With these nerve problems, you may not be able to feel a leg ulcer or know its there. Diabetes also slows the wound healing process.
- Peripheral artery disease : This condition causes plaque to build up in the arteries . The blood vessels in the leg become narrow, leading to poor blood circulation. The reduced blood flow slows the healing of leg ulcers. People with diabetes are more likely to develop PAD.
- High blood pressure: Chronic, poorly controlled high blood pressure can cause an extremely painful ulcer on the lower leg called a Martorell ulcer. High blood pressure causes the capillaries in the skin to become narrow, cutting off the blood supply to the skin. The skin can die, forming a leg ulcer.
Also Check: Medications Used To Treat Ulcerative Colitis
What Are The Symptoms
Skin ulcers look like round, open sores. They range in severity and are usually minor injuries on the skin.
In severe cases, ulcers can become deep wounds that extend through muscle tissue, leaving bones and joints exposed.
The symptoms of skin ulcers include:
- discoloration of the skin
People can develop the following types of skin ulcer:
Cleaning And Dressing The Ulcer
The first step is to remove any debris or dead tissue from the ulcer and apply an appropriate dressing. This provides the best conditions for the ulcer to heal.
A simple, non-sticky dressing will be used to dress your ulcer. This usually needs to be changed once a week. Many people find they can manage cleaning and dressing their own ulcer under the supervision of a nurse.
Also Check: How To Tell If I Have Stomach Ulcer
What Is Poor Leg Circulation
Poor leg circulation, or peripheral artery disease , is a circulatory problem in which narrowed arteries reduce blood flow to your limbs. While it commonly occurs in the legs, peripheral artery disease can also affect the peripheral arteries to the stomach, arms, and head. The arteries harden due to plaque buildup in the arteries and blood vessels, and this blocks the normal blood flow through the vessels and results in poor circulation in the legs.
While it isnt a condition in itself, poor leg circulation may be a sign of larger health issues. If youre experiencing the associated symptoms of poor blood circulation, its important to consult with your doctor, who can check for other health complications that may worsen over time. These can include obesity, diabetes, high blood pressure or cholesterol, and various heart and arterial conditions.
Symptoms Of Venous Leg Ulcers
Venous leg ulcers are open, often painful, sores in the skin that take more than a month to heal. They usually develop on the inside of the leg, just above the ankle.
If you have a venous leg ulcer, you may also have:
- discolouration and darkening of the skin around the ulcer
- hardened skin around the ulcer, which may make your leg feel hard or even resemble the shape of an upside-down champagne bottle
- a heavy feeling in your legs
- aching or swelling in your legs
- red, flaky, scaly and itchy skin on your legs
- swollen and enlarged veins on your legs
- an unpleasant and foul-smelling discharge from the ulcer
Don’t Miss: What Are The Symptoms Of A Stomach Ulcer Uk
Arterial & Venous Ulcers
Skin ulcers are wounds that develop on your skin due to poor circulation of blood. When blood flow is blocked, the overlying skin and tissues dont receive oxygen. This damages the tissue and causes the area to form an open wound.
There are different types of ulcers:
- Arterial ulcers. These occur when you have artery disease, such as peripheral artery disease , and are usually on your feet and toes. These are less common than venous ulcers.
- Diabetic foot ulcers. Diabetes can cause nerve damage, which can lead to a loss of feeling in your feet. This can result in unnoticed sores that can become serious foot ulcers.
- Venous ulcers. These are caused by damaged valves in your lower-leg veins, which disrupt normal blood flow and allow blood to flow backward. The abnormal blood flow causes the veins to get overfilled, and fluid seeps out into the surrounding tissues.
Foods Rich In Omega 3s
Omega 3s are known to promote blood circulation and increase circulation.
Fatty Fish
Salmon and mackerel provide a tremendous dose of omega-3 fatty acids. Omega 3 fats promote the release of nitric acid, which works to dilate blood vessels and improve blood flow. They also reduce the risk of blood clots by preventing blood platelets from clumping.
Don’t Miss: Does Stelara Work For Ulcerative Colitis
Home Remedies For Blisters Or Leg Ulcers
- Garlic improves blood circulation. One should take 3 to 4 garlic cloves every day. Cut raw garlic into tiny pieces and put the minced pieces at the blister area for few days. Garlic powder is also available which can be sprinkled twice a day on that area.
- Vitamin C also helps in improving blood circulation and healing of leg blisters and ulcers. Richest source are guavas, red sweet peppers, parsley, turnip greens, broccoli, brussels sprouts and all fresh fruits and vegetables, especially green leafy.
- Take a full multivitamin supplement.
How Are Leg Ulcers Treated
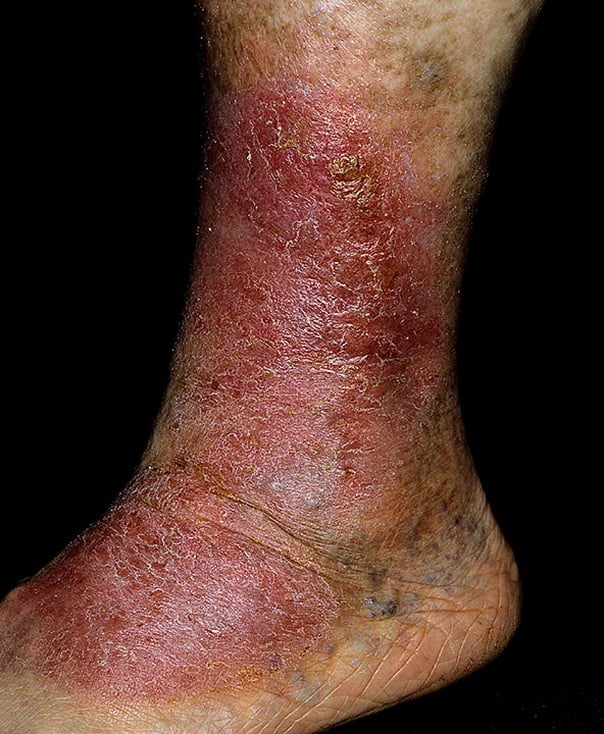
Leg ulcers can be challenging to eliminate. Even with treatment, wounds can persist for months or sometimes years.
Treatments vary depending on the ulcer type and cause. Your healthcare provider will focus on healing the wound, reducing swelling and preventing the ulcer from coming back as it heals.
Leg ulcer treatments include:
- Compression therapy with stockings or bandages to stimulate blood flow to the legs.
- Leg elevation above the heart for one hour a day for at least six days.
- Wound care, including debridement , topical antiseptics to prevent infection and regular bandage changes.
- Antibiotics to treat infections and medications to open blood vessels and improve blood flow .
- Hyperbaric oxygen therapy to get more oxygen into the blood and speed healing.
- Sclerotherapy or endovascular ablation to treat varicose veins.
- Surgery to remove, repair, replace or bypass a damaged vein.
- Skin grafts for wounds larger than 4 inches or ulcers that dont heal with other treatments.
Don’t Miss: Why Does Ulcerative Colitis Happen
Guide To The Causes Of Leg Ulcers
A leg ulcer an open wound or sore that develops on an individual’s leg. Symptoms include pus at the ulcer site, increasing wound size, enlarged veins, pain at the ulcer site, heaviness in the legs, and swelling in the legs. Medical history, physical examination, CT scan, MRI scan, vascular ultrasound, and x-rays may be used to diagnose leg ulcers. The main concern when it comes to leg ulcers is the risk of developing an infection in the wound that progresses to a life-threatening blood infection.
Thankfully, there are many leg ulcer treatment options out there. Patients may need compression bandages to treat their ulcers. Leg ulcer medication includes antibiotics for infections as well as medication for circulation, topical ointments, and pain medication. Leg ulcer wound care should also include natural treatments and home remedies for leg ulcers, such as diet changes and braces or orthotics. Overall, the best leg ulcer treatment can vary based on the underlying cause. Get to know the common causes now.
Home Care For An Ulcer
With the proper care, a leg ulcer can heal successfully on its own. However, it isnt a quick process and requires you to be diligent about your wound care.
If you have an ulcer, the best thing to do is to come to see Dr. Issa for an evaluation. He helps you understand what’s happening with your skin and gives you wound care instructions to enable your wound to heal.
Home care instructions given by Dr. Issa include:
- Clean the wound regularly
- Keep the skin around the wound dry
- Prop your feet up during the day
- Walk daily to improve blood flow
You must follow his wound care steps closely. Venous leg ulcers are complicated to eliminate and may become infected without the proper care.
If you notice that your wound isn’t healing correctly, contact the team right away. Dr. Issa may need to intervene in your care for a swifter recovery.
Read Also: Best Pain Relief For Leg Ulcers