Are You In Need Of An Experienced And Caring Podiatrist
If you’re experiencing an ulcer or sore on your foot or any type of foot pain, you should speak with an experienced podiatrist as soon as possible. Please contact us online to schedule your appointment or call one of our convenient El Paso offices directly. To reach our Sierra Tower Building podiatrist office, please call 915.533.5151. You can find driving directions here. To reach our George Dieter Drive podiatry office, please call 915.856.3331. Driving directions are available here.
|
Related Links: |
From Injury Or Blister To Ulcer
If a person with decreased sensation gets a blister or other injury, they may not notice it and it can develop into an ulcer.
Neuropathy:Neuropathy is a general term for nerve dysfunction. Peripheral neuropathy is the most common type of neuropathy in people with diabetes and typically affects the nerves of the feet, legs, and sometimes the arms and hands.
People with diabetes are at increased risk for peripheral neuropathy if they have a history of hyperglycemia and have had diabetes for a long time. Other risk factors for neuropathy include smoking and genetic predisposition.
Over time elevated blood sugar levels can affect nerve functioning and nerve signaling. Small nerve dysfunction results in the inability to feel pain, and large fiber dysfunction causes disturbances in balance, which can increase the risk of falls.
If a person has neuropathy and injures their foot without feeling it, they may not notice it until it gets much worse. Recurrent, unnoticed injuries to the foot can increase the risk of Charcot foot, in which progressive destruction of the bones and joints leads to foot deformity.
Autonomic neuropathy can cause a decrease in sweating, resulting in dry feet. Having dry feet can increase the risk of developing calluses. While calluses are healthy, if you have lost sensation, they can grow deeper cause damage to the skin surface known as breakdown, putting the foot at risk of blisters or ulcers.
How Do Diabetic Foot Ulcers Form
Ulcers form due to a combination of factors, such as lack of feeling in the foot, poor circulation, foot deformities, irritation , and trauma, as well as duration of diabetes. Patients who have diabetes for many years can develop neuropathy, a reduced or complete lack of ability to feel pain in the feet due to nerve damage caused by elevated blood glucose levels over time. The nerve damage often can occur without pain and one may not even be aware of the problem. Your podiatric physician can test feet for neuropathy with a simple and painless tool called a monofilament.
You May Like: Mouth Ulcer On Tongue Remedies
Find And Treat Cuts Scrapes And Other Wounds Immediately
If you treat new wounds right away, you can start caring for them before things get bad. So as soon as you find a cut or sore:
Of course, if you dont know you have a wound, you cant treat it quickly. So if you suffer from neuropathy, keep an eye out for new wounds. Check your hands and feet daily, and dont forget to check between your toes.
Wearing white socks can help, too. If you see a red spot or a place where your sock is sticking to your skin, check your foot to see if you have a wound thats new or not healing.
Diabetic Foot Ulcer Symptoms
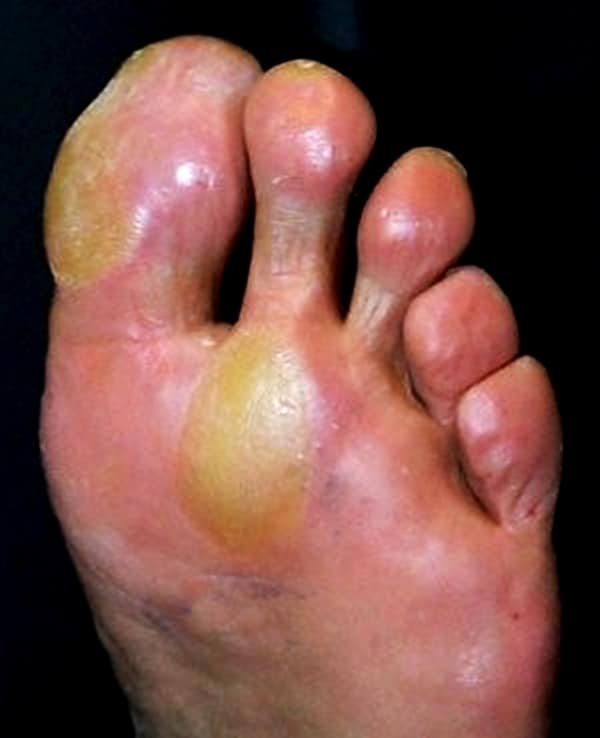
Normally a wound or sore on the skin would cause pain. But the same loss of feeling in the feet that often contributes to the development of a diabetic foot ulcer means that theres often no pain associated with the ulcer. This can make it difficult for people to realize that an ulcer is even there in the early stages, when treatment is most effective.
Aside from pain, another sign to look for is discharge or drainage from the wound in the socks. Ulcers that have been present for some time and that have become infected may also cause an unpleasant odor.
Read Also: How To Detect A Bleeding Ulcer
Causes Of Foot Ulcers
Foot ulcers generally develop when the skin and tissues within the feet break down and then become infected. These ulcers are generally categorized into the following three types:
- Neurotropic ulcers Although these ulcers primarily affect people with diabetes, they can occur in anyone with a loss of sensation in their feet. They can develop anywhere on the foot but are generally located at pressure points along the bottom of the foot.
- Arterial ulcers These ulcers affect individuals with poor circulation. They often develop on the tips of the toes, in between the toes, on the heels or on bony protrusions.
- Venous ulcers These ulcers typically affect individuals who have a history of leg swelling, blood clots within the leg veins or varicose veins. They usually develop on the lower portion of the leg, between the ankle and the knee.
Treatment For Diabetic Foot Ulcers
If a diabetic foot ulcer does occur, its important to seek medical care as soon as possible this is not a wound you should attempt to treat at home on your own. The faster a foot ulcer is properly treated, the greater chance it will heal completely and without infection or complications.
A diabetic wound care specialist, such as the Wound Care Center at Harrington, can provide the most advanced and comprehensive diabetic wound treatment. Your primary care physician can provide a referral to the wound care center. Our Wound Care Center team will then continue working hand-in-hand with your doctor throughout the wound treatment process.
Our specialized diabetic wound treatment services include:
Read Also: How To Tell If Your Horse Has Ulcers
Getting Diagnosed With A Foot Ulcer
If you have a wound on your foot that is not healing, make an appointment at your GP practice or with a podiatrist. You may be given an appointment to see the nurse rather than the doctor as they are often responsible for caring for patients with leg and foot problems.
If you know you have diabetes and you have a wound on your foot, then you should seek advice from your healthcare professional urgently .
Make sure you remove any nail polish from your toenails before your appointment.
When you see the nurse, podiatrist or doctor, they should:
- Ask about your symptoms and how long you have had problems
- Examine your lower legs
- Do a special test called a Doppler Ultrasound. This test compares blood flow in your ankle with that in your arm to find out if there are blood flow problems in your lower leg. You may have to come back to have your Doppler test on another day or at another clinic but you should have this test within a few weeks of your first appointment
- Test how much sensation you have in your feet
You might also be offered some more tests to rule out other health problems that can affect your legs, including diabetes, anaemia, thyroid, kidney and cholesterol problems.
If your GP practice thinks you have problems with your arteries, they may refer you for further vascular tests at your local hospital or specialist clinic.
When Should I See My Doctor
See your GP if you think you might have an ulcer related to a mouth infection.
Also, see your GP if your child develops severe mouth ulcers with symptoms of general illness like:
- weight loss, stomach pain, unexplained fevers
- blood or mucus in their stool
- neck stiffness and tiredness
This may indicate conditions such as coeliac disease and inflammatory bowel disease.
Its also important to see your doctor or dentist for a mouth ulcer that lasts longer than 3 weeks and keeps coming back.
Although most mouth ulcers are harmless, a long-lasting mouth ulcer is sometimes a sign of mouth cancer. Its best to get it checked.
Don’t Miss: What To Eat When You Have A Stomach Ulcer
How Do I Get Athletes Foot
Athletes foot commonly spreads through skin-to-skin contact or contact with a flake of skin. It spreads in areas used by large groups of people, like locker rooms, swimming pools and saunas.
It can also spread through contact with an infected surface. You can get athletes foot by sharing towels, socks or shoes with someone who has athletes foot.
You May Like: What Foods Are Good For Stomach Ulcers
When To Seek Emergency Care
There are some instances in which you should go straight to the emergency room. Don’t hesitate to go to the ER if:
- You have severe pain or swelling
- You are unable to put any weight on your foot or walk
- You have numbness or loss of sensation
- The pain or tingling comes on suddenly
- You feel burning or tingling in your feet after being exposed to toxins
- You had a flu or other infection in the days or weeks before your pain began, which could indicate Guillain-Barré syndrome
- You have an open wound, or your wound has signs of infection, such as pus, redness, or red streaks leading from it
Don’t Miss: Over The Counter Ulcerative Colitis
What Causes A Foot Ulcer
Patients with diabetes are prone tomajor foot problems. This is because the foot expresses many of the underlying effects of diabetes, including neuropathy, vascular disease, and diminished response to infection.
As a result of the neuropathy, the foot can develop an ulcer. This happens for two reasons. The first is that the neuropathy causes paralysis of small muscles in the foot, which results in clawing of the toes. Clawing of the toes causes prominence of the metatarsal heads on the bottom of the foot as well as the knuckles on the dorsum of the foot.
Neuropathy also causes diminished sensation. As the prominent metatarsal heads on the plantar of the foot are subjected to increased pressure, the skin will begin to enlarge and become callused. The callused skin can be subjected to shear forces that cause a separation between the layers of the skin. The layers can fill with fluid, which can then become contaminated and infected. The pressure also can cause primary breakdown of the skin in these areas, causing a foot ulcer. Once the initial breakdown and contamination occurs, the foot may develop more significant problems because of infection.
Cysts Or Benign Soft Tissue Tumors
Benign cysts or soft tissue tumors, such as lipomas, can spontaneously develop on the bottom of the feet. These growths generally are not harmful.
Benign cysts or soft tissue tumors usually do not require treatment but may need to be surgically removed if they compress surrounding nerves or ligaments.
Recommended Reading: How To Heal Stage 3 Pressure Ulcer
Wound Care And Dressings
Care for your wound as instructed by your provider. Other instructions may include:
- Keep your blood sugar level under good control. This helps you heal faster and helps your body fight infections.
- Keep the ulcer clean and bandaged.
- Cleanse the wound daily, using a wound dressing or bandage.
- Try to reduce pressure on the healing ulcer.
- Do not walk barefoot unless your provider tells you it is OK.
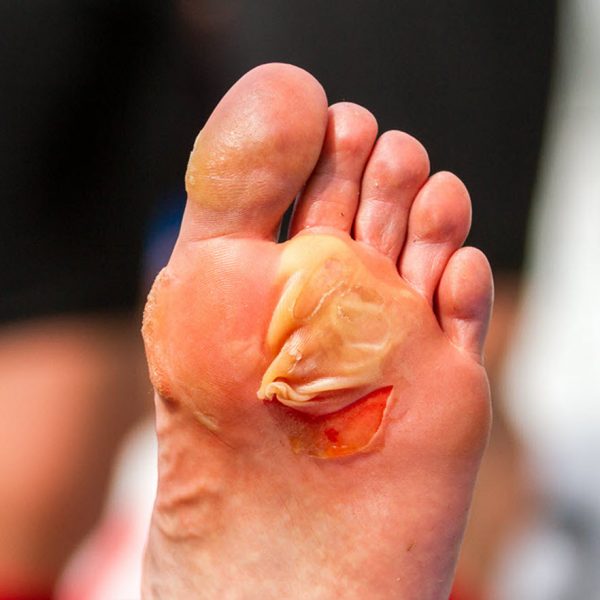
Metatarsal Heads And Sores
According to certain medical study, One of the most common areas for blisters is under the ball of the foot. This includes big or little toe knuckles. Actually, this is where metatarsal heads occur. This is weight-bearing bones that are usually subjected to high pressure.
During the time when the metatarsal skids over the skin and moves backward, the skin is stretched and compressed. Though this is normal to shear here, excessive shear may become unbearable. If this occurs near the surface of the skin, skin blisters may form at the bottom.
The best solutions are to resolve to cushioned insoles, ENGO blister patches, donut pads, etc. For severe conditions please see you GP.
Recommended Reading: Healing Ulcerative Colitis With Plant Based Diet
What To Expect After Treatment With Cvm
At the Center for Vascular Medicine, our mission is to help patients with their vascular diseases in a cost-effective and compassionate manner. We specialize in the diagnosis and treatment of venous and arterial diseases in the legs, feet, and pelvis. Our world-class providers are the most experienced in the specialty and work with patients to develop a treatment plan that is custom-tailored to their unique situation.
Typically, this process involves an initial consultation and ultrasound scan at one of our accredited facilities. After reviewing the results of your scan and obtaining a thorough medical history, our providers will discuss the results with you and help you decide on the next steps.
Our health care providers use several diagnostic tests to help determine what vascular diseases may be causing your symptoms. Our initial evaluations utilize ultrasound because this non-invasive imaging modality helps us verify our suspicions on whether your symptoms are caused by underlying vascular disease.
Foot Ulcer that will not heal Foot ulcer that healed for the first time after the procedure
The venous stent procedure was conducted by Dr. Satwah, physician for the Center for Vascular Medicine.
What Does A Diabetic Foot Look Like
The foots appearance will provide some tell-tale signs of diabetic foot. A physical examination is, therefore, the usual starting place for doctors.
A diabetic foot may become discoloured . One or both feet may also develop:
-
A deformed appearance or abnormal shape
-
Loss of hair on the dorsum of the foot
-
Staining on socks
Recommended Reading: Can Stomach Ulcers Cause Blood In Your Stool
Pus Or Fluid Drainage
You may notice draining of fluid or pus from your infected foot if you have an abscess. An infected ingrown toenail can cause a pus-filled pocket to form under your skin at the side of your toenail.
Foot infections usually develop after an injury or wound to the foot. Having certain medical conditions also increases your risk of foot infections.
How To Prevent Diabetic Foot Ulcers
The first line of defense in preventing diabetic wounds is to follow the guidelines recommended to keep the disease itself under control:
- Maintain healthy blood sugar levels through a healthy diet and by taking medications as instructed by your doctor.
- Keep your blood pressure within a healthy range.
- Avoid alcohol and tobacco.
You should also take measures to avoid causing sores or wounds on the feet:
- Never walk barefoot.
- Wear shoes that fit properly and dont rub the skin.
- Wash your feet daily with mild soap and lukewarm water to prevent the buildup of bacteria on the skin, which can cause infection even in the tiniest skin breaks.
Because a loss of sensation in the feet may mean theres no pain felt even when an ulcer is present, its also extremely important for those with diabetes to regularly check for any foot sores or skin irritation. This way, the ulcer can be properly treated as early as possible.
Don’t Miss: Do Stomach Ulcers Cause Back Pain
Diabetic Foot Ulcers: Surgery Options To Treat And Prevent Podiatric Emergencies
Diabetic foot ulcers open wounds on the feet are all too common in patients with uncontrolled blood sugar levels. In fact, 15% of people with diabetes will experience a foot ulcer, and 1 in 5 of those will be hospitalized for the condition.
Two of the most common disease processes that affect the feet in people with diabetes are diabetic peripheral sensory neuropathy and peripheral arterial disease.
Peripheral arterial disease involves damage to the medium and small arteries that supply blood and oxygen to nourish foot tissue.
Peripheral sensory neuropathy affects more than half of people with diabetes. Neuropathy damages the nerves in the feet, so people experience numbness or tingling, or feel like they have a heavy stocking or mud caked on their foot. In some cases, people experience burning or shooting pains in their feet, which are often worse at night.
Sensory neuropathy also creates an environment in which people can injure their feet but not feel the injury. For instance, people with diabetic sensory neuropathy can burn their feet with bath water that is too hot or when they walk on hot pavement barefoot during the summer.
Foot ulcers develop when the skin is exposed to repetitive pressure on the bottom of the foot, or from friction from poorly fitting shoes. Normally, people would feel pain because their shoes are rubbing against their foot, but neuropathy masks the pain.
Diabetes And Your Feet
Get your feet checked at every health care visit.
If you have diabetes, heres a way to keep standing on your own two feet: check them every dayeven if they feel fineand see your doctor if you have a cut or blister that wont heal.
Theres a lot to manage if you have diabetes: checking your blood sugar, making healthy food, finding time to be active, taking medicines, going to doctors appointments. With all that, your feet might be the last thing on your mind. But daily care is one of the best ways to prevent foot complications.
About half of all people with diabetes have some kind of nerve damage. You can have nerve damage in any part of your body, but nerves in your feet and legs are most often affected. Nerve damage can cause you to lose feeling in your feet.
You May Like: Ulcerative Colitis And Lung Disease
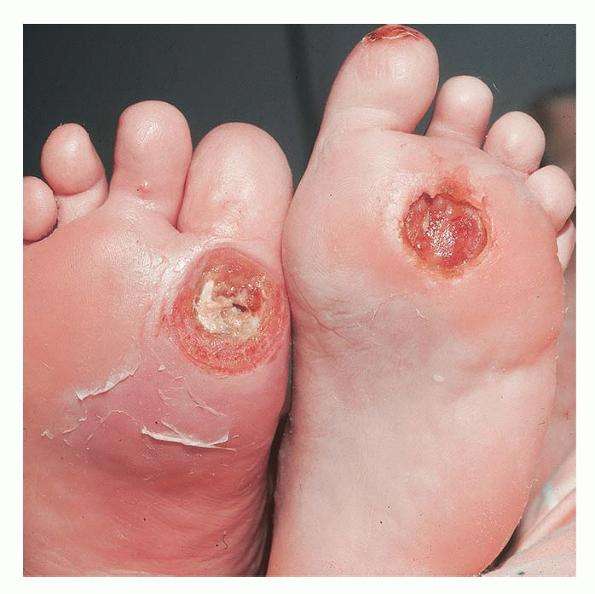
What Are The Symptoms Of Diabetic Foot Ulcers
It is not unusual for patients to have Diabetic foot ulcers for some time before presenting to doctors because they are frequently painless and therefore unaware that they. Symptoms of Diabetic ulcers include but are not limited to:
- Persistent pain
- Redness especially when surrounding a wound, or of abnormal rubbing of shoes or socks.
- Swelling of the feet or legs can be a sign of underlying inflammation or infection, improperly fitting shoes, or poor venous circulation.
- Localized warmth perhaps from wounds that wont heal or that heal slowly.
- Any break in the skin is serious and can result from abnormal wear and tear, injury, or infection.
- Drainage of pus from a wound is usually a sign of infection. Persistent bloody drainage is also a sign of a potentially serious foot problem.
- Fever or chills in association with a wound on the foot can be a sign of a limb-threatening or life-threatening infection.
People suffering from Diabetes should look for cuts, scratches, bruises and sores on the foot, changes to the toenail. Use a mirror if you cannot see under the foot. Tissue around the ulcer may become black due to the lack of healthy blood flow to the foot. In severe cases partial or complete gangrene may occur.
If you do notice any cuts, corns or callus on your feet have them checked out by a podiatrist. A medical pedicure is the best and safest way to have your feet assessed and treated to prevent any further problems.