Glandular Gastric Ulcers In Horses
Glandular gastric ulceration occurs less frequently than squamous gastric ulceration, but has been found to be more common than previously thought. The two regions function differently. Unlike the upper third of the stomach which is highly susceptible to damage from stomach acid, the glandular section of the stomach is relatively impervious to it. However, when factors occur which cause the integrity of the mucosal lining to deteriorate, its natural defensive mechanisms to gastric acid are also challenged leading to the development of inflammation and lesions.
Scientists arent entirely sure what causes this breakdown. They theorize that high dosages or long-term use of non-steroidal anti-inflammatory drugs , such as Bute, may reduce the blood supply to the lining and so contribute. It has also been suggested that, similar to human gastric ulceration, a bacterial infection may also be at play. Despite ongoing investigation, though, that theory has yet to be confirmed.
Again, the symptoms of EGGUS are consistent with Skippys symptoms and also with those of ESGUS. But because EGGUS doesnt respond to the same treatment methods as ESGUS, you cant simply dose a horse up with omeprazole and assume hell recover.
Once an endoscopy has determined whether your horse has ESGUS, EGGUS or both its time for your next test: checking to see if he has colonic ulcers.
Equine 74 Gastric: 21 Typical Signs That Your Horse Has Stomach Ulcers Part 2
Which symptoms a stomach patient expresses and how he deals with his pain varies greatly from patient to patient. For example, some suffer more pain, suffer quietly with severe stomach ulcers and eat apparently only a little worse, while the other one clearly shows that he is not well even with a slight irritation of the stomach mucosa, for example, by frequently flehming, colic again and again or extremely tense and unridden.
Therefore it is important to always keep an eye on the expression behaviour of your horse and to seek advice from outsiders in case of uncertainty, because often creeping changes of behaviour do not attract attention at all or only late.
For your convenience we have allocated symptoms into categories. Simply click on the symptom you want to learn more about.
Feeding and watering behaviours
In the barn and out at pasture
- Difficulty lying down
- Wide placement of front and hind legs
- Defensive behaviour when being saddled
- Avoidance of other horses or increased aggression
Equine 74 Gastric counteracts the effects of constant stress-related acid problems with high mineral acid buffering. Learn more.
Often it is unclear which is first – the gastric ulcer or the cribbing behaviour, because both can be either cause or symptom.
However, it is often observed that horses with a tendency to cribbing will do so more often as a result of a gastric ulcer.
In this way the horse tries to stimulate salivary flow in order to alleviate stomach pain.
How Do Ulcers Develop
The horses stomach is divided into two distinct areas by a structure called the margo plicatus. The upper portion of the stomach is non-glandular and lined with squamous cells, while the lower portion is glandular. The latter produces mucus that coats the stomach lining to help prevent ulcers from the action of the gastric secretions, but the upper portion doesnt. Lesions and ulcers can develop in both portions of the stomach, but the mechanism of development and the predisposing factors are quite different.
The development of ulcers in the squamous portion of the stomach is directly related to intensity of training the more intense the training of the horse, the more likely the horse is to develop ulcers. These ulcers are extremely common up to 90 per cent of horses in some disciplines such as racing have ulcers, and even broodmares and pleasure horses can be affected by this condition. Researchers have proposed a new term to describe this problem: ESGUS .
Researchers havent identified the exact mechanism of ulcer development in the upper portion, but the link to training is well-established. While training, gastric acid normally contained in the glandular portion of the stomach may splash up to the non-glandular squamous cell portion that does not have the same protective mechanisms as the lower portion to prevent acid injury.
Read Also: Venous Leg Ulcer Dressing Treatment
Other Risk Factors And Management Practices To Consider
Besides nutrition, there are several other factors that affect the incidence of gastric ulcers in horses. For example, intense exercise and stress can increase the risk of ulcers. Racehorses, which are under very heavy exercise and stalled for long periods of time, have been found to have the highest incidence of ulcers. Increasing turnout time may decrease stress and provides horses with the opportunity to graze. Stress can also be caused by changes in management and routine or by transportation and competition. Avoid stressful situations when possible and talk with your veterinarian about medication options during transport and competition. Provide forage during travel and at competitions to encourage chewing and to decrease the risk of acid damage within the stomach. The long-term use of nonsteroidal anti-inflammatory drugs such as phenylbutazone and flunixin meglumine can also increase the risk of ulcers since these drugs also inhibit the secretion of the bicarbonate mucous within the stomach that protects itself from the acidic stomach environment. Avoid the long-term use of NSAIDs and talk to a veterinarian about alternative pain management strategies.
Squamous Gastric Ulcers In Horses
Equine Squamous Gastric Ulcer Syndrome refers to ulcerative lesions specifically affecting the squamous portion of the equine stomach, or roughly, the upper third of the stomach. An ulcer in the squamous region is believed to occur when the mucosal lining becomes damaged, likely by bacteria, parasites or a constant barrage of stomach acid. The squamous region is particularly susceptible to damage as it lacks the protective mechanisms of the glandular region to defend its mucosal lining from gastric acid.
Skippy may very well be suffering from ESGUS, as his current lifestyle and diet fit the typical profile of a horse likely to develop squamous ulcers. These risk factors often include:
- Limited turnout
- Intermittent feeding
Hes also displaying all of the classic symptoms, including loss of appetite, difficulty maintaining weight/weight loss, changes in hair coat, poor behavior, underperformance and wood chewing. If he is suffering from ESGUS, continuing his high-concentrate, low-roughage diet and intensive training schedule could make matters even worse for him.
Recommended Reading: Removing Large Intestine Ulcerative Colitis
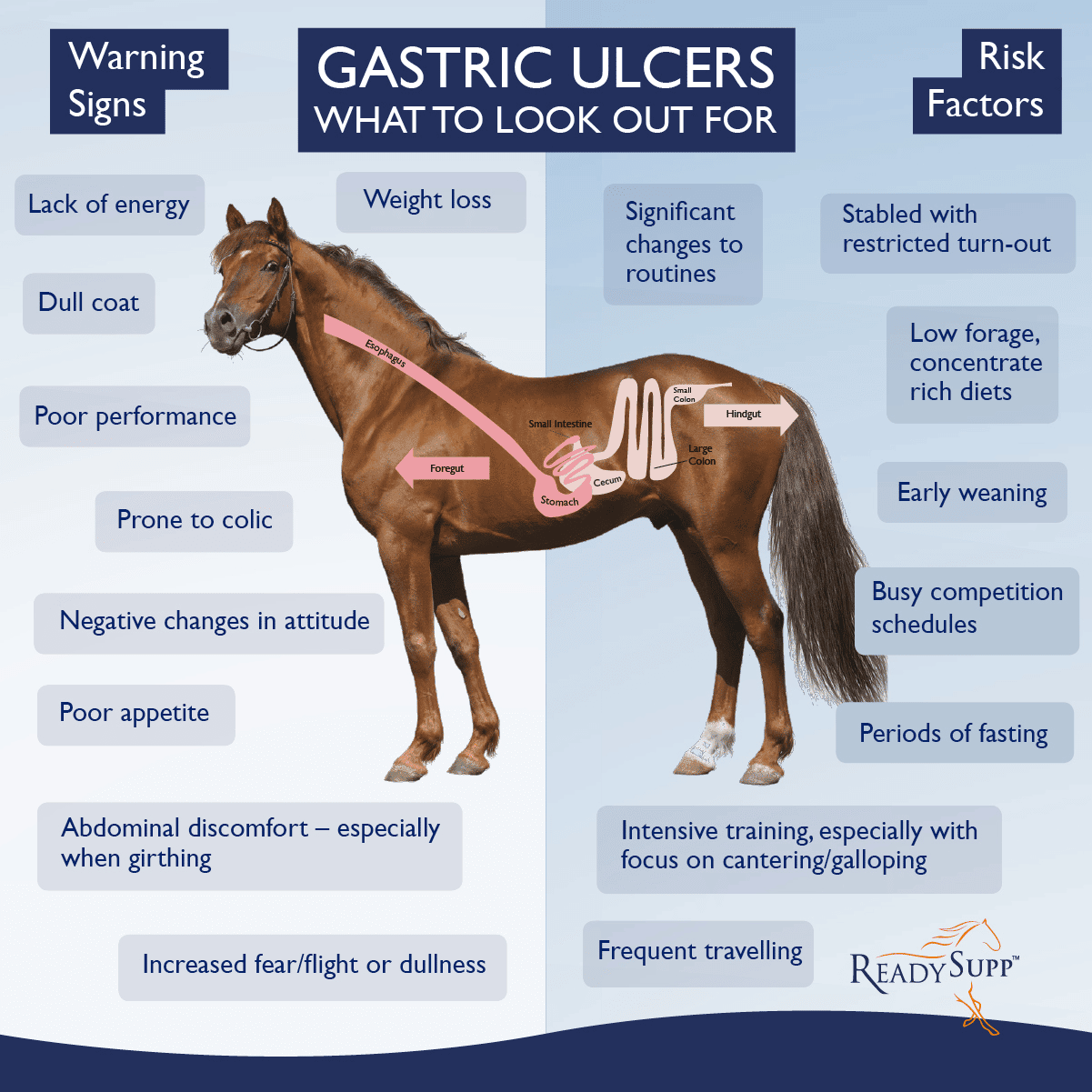
Signs That Your Horse Might Have An Ulcer
Ulcers in horses can be challenging to identify as they sometimes present with quite generic symptoms. Only veterinary diagnosis will confirm whether your horse has ulcers or not but what are the telltale signs that you should keep an eye out for? Read our handy guide and become better informed.
Ulcers can present with a range of symptoms that can easily be attributed to other conditions. If you suspect something is wrong then your vet should evaluate your horse as it could be ulcers or a different issue. Ulcers rarely heal on their own without veterinary intervention. If your horse does have ulcers, your vet will need to determine which type they are as there are two different classifications:
- ESGUS Ulcers in the upper region of the horses stomach which is called the Squamous, really the lower end of the oesophagus lining and the most common of the two types of ulcer
- EGGUS Ulcers in the lower glandular region of the horses stomach
These are some of the symptoms a horse with ulcers can exhibit:
Are There Different Types Of Ulcers
There are three different types of ulcers that a horse can suffer from depending on whereabouts in their stomach the ulcer is.
- Equine Squamous Gastric Ulcer Syndrome Also known as a squamous ulcer, its more commonly associated with a lack of forage and access to water as well as a change in housing and lack of contact with other horses. It affects the area that covers the top third region of the horses stomach known as the squamous.
- Equine Glandular Gastric Ulcer Syndrome The lower two-thirds of the stomach, and in particular the end of the stomach known as the antrum, are affected by EGGUS . Theses ulcers are more commonly linked to prolonged use of drugs such as NSAIDs as well as bacteria infections.
- Colonic ulcer Sometimes referred to as right dorsal colitis , colonic ulcers form in the large intestine. Theyre not as common as the other types of ulcer but are similar in cause to EGGUS.
Also Check: Ulcerated Nodular Basal Cell Carcinoma
Don’t Miss: What Medicine Is Best For Stomach Ulcers
Should The Diet Of Every Horse Be Low In Starch And Sugar
A key concept to consider is that it isnt just the level of sugar and starch within a feed but also how much of the feed is fed and how quickly it is consumed that is important. Forages and pasture are consumed more slowly than the bucket feed so even though they contain relatively high levels of sugar, it is consumed throughout the day rather than in meals which the horses digestive system has evolved to cope with. Obesity, PPID, laminitis all change the ability of the horse to cope with sugar intake and in these situations 10-12% non-structural carbohydrate in forage is recommended. A typical value for grass hays is around 15-20% and a very high level would be 35%. As horses should be fed 1.5% minimum of forage per day to supply sufficient fibre to maintain normal gut function it makes a big contribution to the overall NSC intake.
Types Of Horse Ulcers
Horse ulcers often develop in the stomach, though they can also form in the colon. Ulcers in the stomach are referred to generally as Equine Gastric Ulcer Syndrome, but a veterinarian will provide a specific diagnosis after examining your horse. The two possible diagnoses refer to the region in which the stomach ulcers appear.
- Equine Glandular Gastric Ulcer Syndrome : The glandular is the lower part of your horses stomach. EGGUS is a rare form of Equine Gastric Ulcer Syndrome because the glandular lining can withstand harsh acids and is less susceptible to developing a sore or lesion. EGGUS occurs more often in racehorses than endurance horses.
- Equine Squamous Gastric Ulcer Syndrome : The squamous is the upper part of your horses stomach. Its thought of as an extension of the esophagus lining. Research has shown that ESGUS is far more widespread than EGGUS. In fact, of the horses that show symptoms of Equine Gastric Ulcer Syndrome, 60 to 80 percent of them are diagnosed with ESGUS.
Ulcers in your horses stomach can also lead to the development of hindgut or colonic ulcers. More than 50 percent of performance horses, for example, have both gastric and colonic ulcers. Hindgut ulcers are harder to diagnose, which is why veterinarians may suggest a treatment for them as a precaution.
You May Like: Bone Broth For Stomach Ulcer
How Can I Diagnose Ulcers In My Horse
There are three ways to further investigate the likelihood that your horse has ulcers. A great first step is to perform a focused acupressure point test to determine if there is sensitivity. Another option is to perform a therapeutic trial with drug therapy and/or digestive support supplementation. The most costly procedure is to have your veterinarian perform an endoscopy.
A simple, non-invasive indicator of possible digestive tract ulceration involves palpating acupuncture points near the horses girth area. These points are closely associated with the digestive tract, and start just behind the withers, run down along the horses barrel and cross the sternum. If the horse reacts with pain or sensitivity, it is very likely that your horse has an ulcer. You may also notice a defensive or reactive response when saddling or brushing this area. Severe acidosis and un-diagnosed ulcers cause often very sensitive withers or chronic sore backs.
A therapeutic trial consists of basing your diagnosis on the results of treatment with a proper drug or effective supplement. For example, if you feed your horse a digestive health supplement for one to two weeks and see improvement in symptoms, you have correctly identified the problem. Natural digestive support supplements are a fantastic way to perform a therapeutic trial, as there are no negative side effects.
Clinical Findings Of Gastric Ulcers In Horses
Foals with gastric ulcers are often 26 months of age, and EGUS in foals has been divided into four clinical syndromes: subclinical , clinical , perforating, and gastric outflow obstruction. Most foals have absent or vague clinical signs . However, when gastric ulcers become widespread and severe, classic clinical signs in foals include lethargy, colic, an unthrifty appearance, diarrhea, poor or interrupted nursing, dorsal recumbency, bruxism, ptyalism, frothing or drooling of milk from the mouth, and tongue rolling. Bruxism and ptyalism are signs of esophagitis and esophageal ulceration, which in most foals are secondary to gastric outflow obstruction and gastroesophageal reflux. In addition, esophageal obstruction and Candida spp infection should be considered if these clinical signs are observed in foals.
Importantly, when a foal has clinical signs, the ulcers are typically severe and should be evaluated and treated immediately. Complications related to gastric ulcers are most frequent and severe in foals these include delayed gastric emptying, gastroesophageal reflux and esophagitis, megaesophagus, and acute perforation. Sudden gastric perforation without prior clinical signs occurs sporadically in foals.
Also Check: Ulcerative Colitis Nausea After Eating
Treatment Of Squamous Ulcers
GastroGard is the only medication on the market in the United States that is FDA approved to treat squamous ulcers in horses. Omeprazole works to reduce the production of stomach acid by inhibiting a proton pump within the stomach that is responsible for secretion of stomach acid. It is not just a buffer for stomach acid. Usually, a 28-day treatment with this medication is prescribed by a veterinarian. This medication can also be given at half dose to aid in the prevention of ulcers. It is important to use GastroGard and not medication intended for human ulcers when treating ulcers in horses because GastroGard has a special coating to ensure that it is not degraded by the time it reaches the small intestine where it is absorbed. While GastroGard is effective, successful treatment and particularly prevention of future ulcers requires nutritional changes as well.
Turn Your Horse Out To Pasture More Frequently

In addition to this important step in treatment, there are several more actionable steps we can take to hasten your horses healing. If at all possible, turn your horse out more frequently. Remember, the horses stomach is small and produces acid continually. Consuming small meals more frequently helps to regulate this. 4. Stop or Drastically Reduce the Use of NSAIDs
If you extensively use NSAIDS on your horse, your vet will direct you to reduce their use or eliminate them drastically. That is because NSAIDs are well known to irritate the stomach lining.
You May Like: Home Remedies For Leg Ulcers
Signs Of Horse Ulcers
You rely on your veterinarian to determine if your horse has a gastric or colonic ulcer, but they depend on you to recognize the signs. Its crucial to know the symptoms of horse ulcers so that you can contact your vet and begin treatment as soon as possible.
EGGUS, ESGUS and colonic have identical symptoms, which include:
- Sporadic lameness in the hind end
- Reluctance to bend, extend or collect
- Increased periods of laying down
- Lack of energy or stamina
Experienced riders, owners and stable managers often recognize these signs early, especially when an attitude change or lethargy lasts several days. Some horse ulcer symptoms, however, are easier to miss or overlook.
If you suspect your horse isnt feeling well but are unsure why, dont hesitate to contact your veterinarian. An early diagnosis lets you start treatment sooner so that your horse can begin feeling better.
How Are Esophageal Ulcers Caused
The main causes of esophageal ulcers are:
Exposure to stomach acid: This causes chronic inflammation and irritation of the esophagus, allowing ulcers to develop. Stomach acid exposure most often occurs in people with other gastrointestinal conditions. These can include hiatal hernias and GERD, or gastrointestinal reflux disease, more commonly referred to, as severe heartburn.
Medications: Certain drugs, including aspirin, ibuprofen, bisphosphonates, and some antibiotics, can cause esophagitis, or inflammation of the esophagus, and esophageal ulcers.
Infection: Ulcers caused by infection are less common, but the fungal infection known as candida, herpes, and the human papillomavirus have all been linked to esophageal ulcers.
Caustic injury: Esophageal ulcers may be caused by ingesting a corrosive substance. This type of injury mostly affects children, but it can also occur in adults who experience psychosis, suicidal tendencies, or who are abusing alcohol.
Certain types of gastric surgery or foreign bodies can also cause esophageal ulcers.
Early intervention is key to preventing complications from esophageal ulcers.
In cases of acid reflux, treatment may include:
- Medication, such as antacids, H-2-receptor blockers, and proton pump inhibitors .
- Dietary and lifestyle changes, to aid digestion.
- Surgery, for severe cases. Types of surgeries include to tighten the LES valve near the top of the stomach or to insert a magnetic device to help the LES valve function.
Don’t Miss: What Is Severe Ulcerative Colitis
S To Diagnose Equine Corneal Ulcers
If you have ever tried to pry your horses eyelids open when they wish to keep them closed, you understand how difficult that can be. To allow a full eye inspection, and reduce the amount of pressure applied to the eye during the exam, Dr. Pierce will inject a local anesthetic in several locations around your horses eye. This allows him to hold your horses eyelids open to check for foreign material, view the cornea with a handheld microscope, and apply fluorescein and/or rose bengal dye to the eye. The fluorescein dye will attach only to areas of disrupted cornea, and can be used to delineate the location, size, and shape of the ulcer, should one be present, and the rose bengal dye can help detect early fungal ulcers. Depending on the ulcers appearance, Dr. Pierce may also collect corneal cells for laboratory examination or culture, to diagnose and effectively treat bacterial or fungal infections.