What Are The Risk Factors For Ulcerative Colitis
The main risk factor for ulcerative colitis is having a family member with the condition.
While experts do not know the exact cause of UC, they believe that genetics may play a role in its development.
Age may also increase your risk of UC. It most commonly affects people between ages 15 and 30, though it can occur later in life.
Dietary And Lifestyle Modifications
As most nutrients are absorbed higher up in the digestive tract, persons with ulcerative proctitis generally do not have nutrient deficiencies however, other factors may influence an individuals nutritional state. Disease symptoms may cause food avoidance, leading to food choices that might not provide a balanced diet. If bleeding is excessive, then modifications to the diet will be necessary to compensate for this.
Better overall nutrition provides the body with the means to heal itself. It is important to follow Canadas FoodGuide, but some foods may irritate the rectum and increase symptoms, even though they do not affect the disease course. The customized recommendations of a registered dietitian can address your sensitive digestive tract.
How Is Acute Bacterial Dysentery Differentiated From Acute Onset Of Ischemic Colitis
The degree of bloody diarrhea is variable in patients with ischemic colitis, and it may be difficult to distinguish between the two diseases. Clinically, the patient with ischemic colitis complains of sudden-onset abdominal pain, and an acute abdominal series may show thumbprinting of the colonic mucosa.
Flexible sigmoidoscopy is the mainstay of diagnosis for ischemic colitis. The rectum is usually spared because of its collateral blood flow. Above the rectum, the mucosa becomes friable and edematous, and there may be hemorrhagic areas and ulcerations resembling those of Crohns disease. Angiography is not generally helpful in the evaluation of ischemic colitis ischemic colitis is a small-vessel disease compared with mesenteric midgut ischemia of the small bowel, which involves thrombosis or embolism in the superior mesenteric artery . A barium enema is contraindicated in patients with suspected ischemic colitis, because colonic expansion during barium instillation may promote further ischemia.
Glenn T. Furuta, in, 2004
Read Also: What Causes Ulcers In Your Stomach
Inflammatory Bowel Disease And Colitis
Ulcerative colitis and Crohns disease are the two types of inflammatory bowel disease that cause colitis. Crohns disease and ulcerative colitis are considered autoimmune diseases .
- Ulcerative colitis always begins in the rectum and may spread to the rest of the rest of the colon, spreading from the rectum to the sigmoid, descending, transverse, and finally the ascending colon and cecum in that order. Ulcerative colitis is considered an autoimmune disease, and symptoms include abdominal pain, and bloody, diarrheal bowel movements.
- Crohns disease may occur anywhere in the gastrointestinal tract , including the esophagus, stomach, small intestine, and colon. In Crohns disease, there may be skip lesions, that is, abnormal segments of the GI tract interspersed with normal segments.
Both Crohns disease and ulcerative colitis may have other organ systems involved in addition to the gastrointestinal tract.
Either collagen or lymphocytes infiltrate into the layers of the wall of the colon, presumably as a result of inflammation. This is an uncommon illness and maybe an autoimmune disease. Diarrhea often is watery, and no blood is present in the stool.
Can I Prevent Ulcerative Colitis
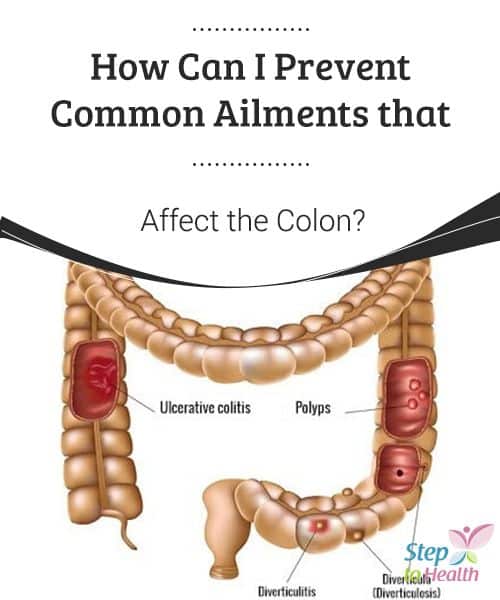
Because experts do not know the exact cause of ulcerative colitis , it may not be possible to prevent it.
Yet you may be able to take steps to reduce the severity of symptoms or to prevent relapse. Per the NHS, these include:
- avoiding foods that trigger your symptoms
- drinking plenty of fluids to stay hydrated
- getting enough regular exercise
- taking steps to reduce stress, such as relaxation techniques
Contact your doctor for more advice on ways to reduce the severity of your symptoms or to prevent relapse if you are in remission.
Recommended Reading: How To Apply Compression Bandages For Leg Ulcers
Managing Daily Life After Surgery
Flatulence is a common problem following surgery. People may need to avoid insoluble fiber foods, such as popcorn, olives, and vegetable skins, which can obstruct the stoma. Some pouching systems have filters that can help limit flatulence.
It is important to increase fluid intake, and include not only water but also broth, sports drinks, and vegetable juice to maintain appropriate levels of sodium and potassium.
Ileostomy and ileoanal anastomosis do not interfere with bathing or showering or most physical activity except for contact sports. As a rule, the surgeries do not impair sexual function.
What Tests Diagnose A Peptic Ulcer
To confirm a person has an ulcer a diagnostic imaging test will usually be ordered. The two most widely used tests are:
- Upper GI series : This is a type of X-ray. The patient is given a chalky liquid to drink that increases the contrast on the X-ray, making certain features easier to see. Because this liquid contains barium, this test is sometimes called a barium swallow.
- Endoscopy : An endoscope is a thin, flexible tube with a tiny camera at the end. The patient is given a mild sedative, and then the tube is passed through the mouth into the stomach. The doctor can see the lining of the stomach to diagnose a peptic ulcer. Tiny samples of the tissue will be taken , which are examined under a microscope.
If a diagnostic imaging test reveals an ulcer, the patient will most likely have a test to see if H pylori bacteria are present.
- It is important to be certain about this, because treatment of the H pylori is likely to heal the ulcer.
- Ulcers caused by H pylori are treated differently than ulcers caused by medications.
Three types of tests are available to detect H pylori.
Don’t Miss: How To Get Rid Of A Ulcer In The Mouth
Can Surgery Affect Nutritional Status
Removal of portions of the intestine can affect nutritional status. When sections of the small or large intestine are removed, surface area for absorption of nutrients is decreased. The following diagram illustrates where nutrients are absorbed. If certain portions of the intestine are severely inflamed, or have been removed, absorption of nutrients may be affected. Malnutrition and nutrient deficiencies can result.
If you have had or are planning to have surgery to remove intestines, talk to your doctor or registered dietitian about which vitamins and minerals you need to take.
You May Like: What Desserts Can I Eat With Ulcerative Colitis
What Alternatives Are There To Bread To Avoid Bloating
Switching to a different type of bread can often reduce or eliminate bloating, but not always.
For some, swapping to authentic sourdough bread can be enough. This is because the sourdough culture, together with the slow rise typical of an authentic sourdough loaf, breaks down many of the digestion-resistant components in breadsuch as the enzyme inhibitors. Even if a loaf of bread is not sourdough but has still been given a long proving time, it can be more tummy-friendly. Try buying your bread from a traditional bakery to see if this makes a difference.
Different kinds of wheat that are lower in gluten and enzyme inhibitors are another option. These include spelt, kamut, einkorn and emmer. Flours and breads made from these ancient grains are now available in many supermarkets.
Gluten-free breads are made from non-gluten containing flours, which dont carry the enzyme inhibitors and wheat germ agglutinin. But these products can contain emulsifiers and other additives that can affect your gut health, so its important to read the label carefully before choosing, or make your own.
Donât Miss: Can Fatigue Cause Shortness Of Breath
Also Check: What Does A Foot Ulcer Look Like
When Nausea And Malnourishment Land You In The Hospital
Ulcerative colitis emergencies had me in and out of the hospital on numerous occasions. Since I was too nauseated to eat, I twice had a PICC line placed on the inside of my left arm so that I could receive TPN intravenously.
At home, my nausea was so crippling that I would take the food my dad would make for me and try to hide it in the trash. Even so, my father, a physician, was consistent and stern with his monitoring of my food intake. He knew I was always on the cusp of malnourishment, which meant another hospital stay and another PICC line.
Eventually, my condition became so severe that in 2013 I had an IPAA surgery series. During these procedures, a surgeon removes the colon and rectum and uses the end of the small intestine, known as the ileum, to form an internal pouch thats commonly shaped like a J. I have lived with a J-pouch for about five years.
Increased Appetite From Corticosteroid Use
Increased eating, weight gain, and a redistribution of fat to the face, neck, and abdomen are associated with the use of prednisone and other corticosteroids. Every time Im put on steroids, I find myself waking in the middle of the night with a raging hunger, a MyCrohnsAndColitisTeam member commented.
However, increased appetite due to corticosteroids is also associated with a reduction in lean body mass, including muscles and organs. For people with IBD, gastrointestinal discomfort means that an increase in appetite does not always correlate with an increase in eating, as many MyCrohnsAndColitisTeam members attest. Disordered eating may also lead to unhealthy eating that does not provide proper nutrition. Im always so hungry but cant eat much, since everything I eat upsets my stomach, one member wrote. Another member said, I am very hungry but have only been able to eat 600 calories today due to the cramping response.
Don’t Miss: Is Peppermint Tea Good For Ulcerative Colitis
Abdominal Pain And Bloating Can Be More Than Just A Stomach Ache
Its not unusual to experience the occasional stomach ache when food disagrees with you, or stress might trigger Irritable Bowel Syndrome. Its when you appear bloated more often than not, and are experiencing persistent abdominal pain and cramps, you need to consider colitis.
This is particularly the case when your pain and bloating coincides with significant weight loss, vomiting, and even painful joints.
What Can I Expect If I Have A Diagnosis Of Ulcerative Colitis

Ulcerative colitis is a lifelong condition that can have mild to severe symptoms. For most people, the symptoms come and go. Some people have just one episode and recover. A few others develop a nonstop form that rapidly advances. In up to 30% of people, the disease spreads from the rectum to the colon. When both the rectum and colon are affected, ulcerative symptoms can be worse and happen more often.
You may be able to manage the disease with medications. But surgery to remove your colon and rectum is the only cure. About 30% of people with ulcerative colitis need surgery.
Recommended Reading: Ulcerative Colitis And Night Sweats
Recommended Reading: What Can Help Stomach Ulcers
Lifestyle Changes To Treat Ulcerative Colitis
You can make dietary and lifestyle changes to help alleviate symptoms and lengthen time between flare-ups.
While there is no evidence that says certain foods cause ulcerative colitis, there are certain foods that can aggravate your symptoms. Limiting dairy products and avoiding problem foods may help improve your symptoms. Problems foods can vary for each person, but you should also avoid gassy foods such as beans, cabbage and broccoli, raw fruits and fruits, popcorn, caffeine and carbonated beverages. Experiment with fiber. For some, adding more high-fiber foods can help with bowel issues however, if you have an inflammatory bowel disease fiber may worsen your symptoms. Try eating five or six meals instead of two or three large ones and drink plenty of fluids, preferably water.
Avoiding stress is also a good way to alleviate your symptoms. Stress can aggravate your symptoms, so learning to better manage stress can help. Exercise, biofeedback, regular relaxation and breathing exercises are all ways you can manage stress.
What Can You Do To Help
Also Check: How To Cure Ulcerative Colitis With Diet
Taking Care Of Your Hair
For some people, simple dermatologist-recommended practices to increase scalp and follicle health may do the trick. These practices include:
- Limiting the use of heated styling tools, such as curling irons and hair straighteners
- Blow-drying infrequently or on low heat
- Avoiding chemical treatments, such as coloring and relaxing
- Using gentle or naturally derived hair products
- Avoiding hairstyles that tug on the hair follicles, such as tight ponytails
- Being gentle when combing or styling your hair
Connect With Others Who Understand
Have you experienced nausea with IBD? Its a frustrating symptom, but it can be helpful to know youre not alone.
MyCrohnsAndColitisTeam is the social network for people with IBD and their loved ones. More than 157,000 members come together to share their stories, ask questions, and let others know what has helped them manage IBD symptoms including nausea.
If youve found a way of managing your nausea with IBD, share your tips with others! Join MyCrohnsAndColitisTeam today and connect with others in the comments below or by starting a new conversation thread.
Recommended Reading: Low Fodmap Diet Ulcerative Colitis
What Causes Ulcerative Colitis
Researchers think the cause of ulcerative colitis is complex and involves many factors. They think its probably the result of an overactive immune response. The immune systems job is to protect the body from germs and other dangerous substances. But, sometimes your immune system mistakenly attacks your body, which causes inflammation and tissue damage.
Causes Of Stomach Pain After Eating
If you experience gastrointestinal discomfort frequently after eating food, it may be something serious that needs professional help. A gastroenterologist can help you find out more about the causes of stomach aches and even recommend an effective treatment plan based on your symptoms.
Following are the most common causes of stomach pain after eating:
Don’t Miss: Whipworm Therapy For Ulcerative Colitis
How Is Ulcerative Colitis Treated
Theres no cure for ulcerative colitis, but treatments can calm the inflammation, help you feel better and get you back to your daily activities. Treatment also depends on the severity and the individual, so treatment depends on each persons needs. Usually, healthcare providers manage the disease with medications. If your tests reveal infections that are causing problems, your healthcare provider will treat those underlying conditions and see if that helps.
The goal of medication is to induce and maintain remission, and to improve the quality of life for people with ulcerative colitis. Healthcare providers use several types of medications to calm inflammation in your large intestine. Reducing the swelling and irritation lets the tissue heal. It can also relieve your symptoms so you have less pain and less diarrhea. For children, teenagers and adults, your provider may recommend:
Children and young teenagers are prescribed the same medications. In addition to medications, some doctors also recommend that children take vitamins to get the nutrients they need for health and growth that they may not have gotten through food due to the effects of the disease on the bowel. Ask your healthcare provider for specific advice about the need for vitamin supplementation for your child.
You might need surgery that removes your colon and rectum to:
- Avoid medication side effects.
- Prevent or treat colon cancer .
- Eliminate life-threatening complications such as bleeding.
A Food Allergy Or Intolerance

Food allergies and intolerances are the most common reason behind stomach pain after eating. Symptoms such as gas, bloating, unusual burps, cramping, and diarrhea indicate that you have eaten something that has not digested well in your stomach.
Allergies occur when the body mistakes some food for a harmful foreign invader, and your immune system releases antibodies to fight it. This immune response can cause an array of symptoms. Common allergens include:
Food intolerance occurs when the digestive system gets irritated by a particular food or cannot digest it properly. Unlike an allergy, there is no immune system response involved in food intolerance which results when your stomach cannot process specific foods or ingredients.Foods that are known to cause intolerance include:
- Lactose sensitivity to milk or dairy products
- Gluten a protein that is present in grains such as wheat, barley, and others
- FODMAPs sensitivity to foods that contain different types of fermentable carbohydrates
If these intolerances are not significant, these conditions can go undiagnosed for years. If you notice signs of stomach pain every time you consume a specific food item, it may be coming from an allergy or intolerance and must be tested by a doctor.
Read Also: Can I Eat Oatmeal With Ulcerative Colitis