What Are The Complications Of Skin Ulcers
Complications include:
- Infection. This may further slow the healing of the ulcer and make it more painful and smelly. It may affect the skin around it, making it red, and there may be a discharge of a gunky smelly material from the ulcer. If an infection is suspected, a swab is usually taken on a stick rather like a cotton bud and sent to the laboratory for analysis. The swab result can confirm the presence of germs and recommend the right antibiotic treatment.
- Infection can spread to the skin. This is called cellulitis.
- Infection can spread to the bone. This is called osteomyelitis.
- Occasionally infection can spread and become widespread, causing .
- Pain. This can usually be managed with suitable painkillers.
- Psychological problems. Depending on the severity and cause, ulcers can cause low mood, depression, anxiety, low self-esteem, being unable to work and loss of mobility
Ulcers Caused By Injury Or Pressure
- Injury. Most ulcers start off with an injury to the skin. Some are trivial a little scratch or bite for example, which doesn’t properly heal for some reason, such as a circulation problem as above. Others may be larger skin injuries, or injuries which extend more deeply to tissue under the skin.
- Neuropathic ulcers. Some injuries to the skin occur because there is a problem with the feeling in the skin. If you can’t feel your feet, for example, you may not be able to tell that a shoe is too tight, or the bath is too hot. So you end up with a blister or a burn, which can go on to become a skin ulcer, particularly if your circulation is not very good. Ulcers caused in this way are called neuropathic ulcers. Diabetes is the common cause. See the separate leaflet called Diabetes, Foot Care and Foot Ulcers.
- Pressure sores are a common type of skin ulcer. Areas of skin become damaged due to a continuous pressure on them, usually due to a person not being able to move well. See the separate leaflet called Pressure Sores.
Signs And Symptoms Of Leg Ulcers
The most common symptoms that accompany leg ulcers are as follows:
- Swelling of the ankles
- Irritated or flaky skin
- Skin begins to harden and scale around the ulcers
These symptoms often vary in their severity. Although most leg ulcers usually disappear in a few days, some may be non-healing. It is always better to try and heal leg ulcers as soon as you can to prevent further complications. For that, you need to diagnose them first. The following are a few most common techniques used to diagnose leg ulcers.
Also Check: How To Ease Mouth Ulcer Pain
What Are The Complications Of Leg Ulcers
People with nonhealing wounds are at risk for:
- Bone infections such as osteomyelitis, which may lead to limb loss .
- Cellulitis, a potentially severe bacterial infection of the skin and layers beneath the skin.
- , a potentially life-threatening bacterial infection.
- Skin cancers like squamous cell carcinoma.
Ulceration Due To Dermatitis Artefacta
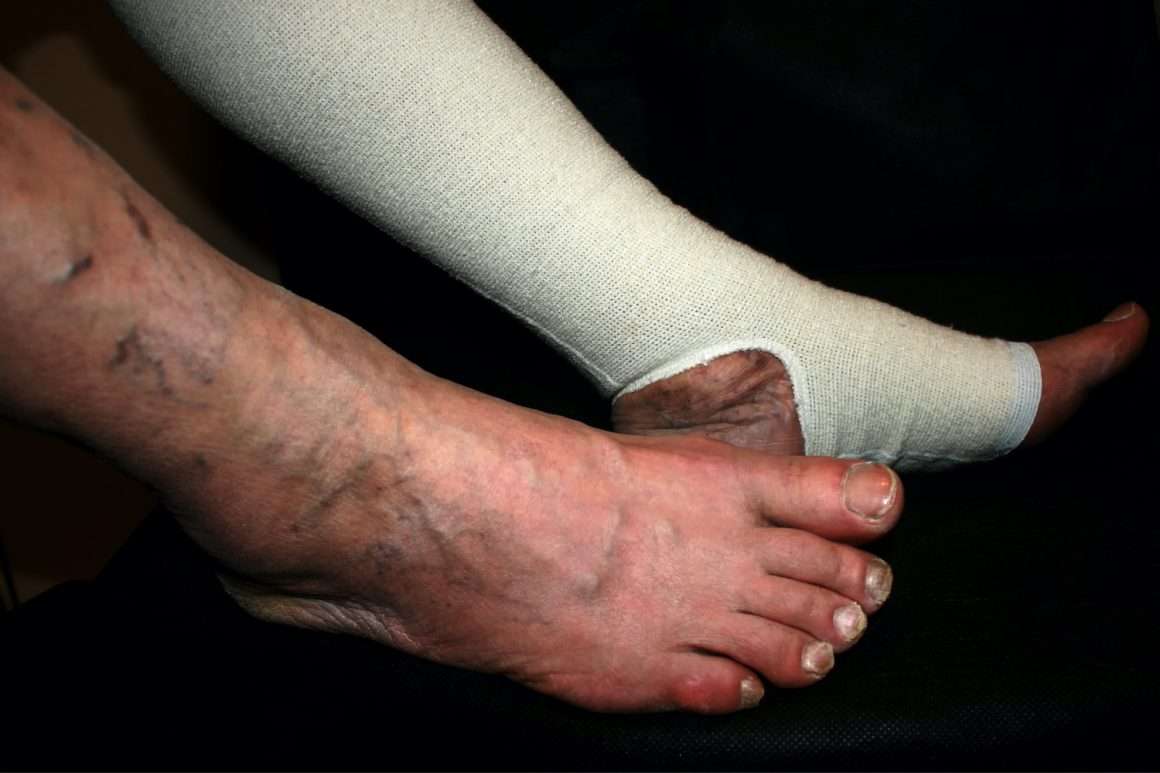
Ulceration secondary to artefact may be difficult to diagnose. Clinical suspicion might be raised by the following: unusual appearance, unusual site, after trauma at work with possible compensation issues, angulate shape or the apparent indifference of the patient to their ulcer and its implication to their life. If the ulcer tends to come and go, a skin biopsy may be necessary to show up out-side-in damage, that is, disproportionate damage to the epidermis compared with the dermis.
Recommended Reading: How To Stop Ulcerative Colitis Bleeding
When Should I See My Healthcare Provider About Foot And Toe Ulcers
If you have diabetes, its important to see a podiatrist regularly. Whether you have diabetes or not, you should see a healthcare provider immediately if you find an ulcer on your foot or toe. Left untreated, it could get infected, leading to complications like amputations.
A note from Cleveland Clinic
It can be distressing to discover an open sore on your foot or toe. You might not know what caused it, it might not be healing and, if you have neuropathy from diabetes, you might not even feel it. Keep in mind that your healthcare provider can successfully treat your ulcer, especially if its found early. If left untreated, an ulcer can lead to serious complications.
If you have neuropathy caused by diabetes, remember that its important to check your feet and toes on a regular basis. Check your toes and feet every time you shower or when you go to put on your shoes. Contact your healthcare provider right away if you find an ulcer.
How Can I Prevent Leg Ulcers
Leg ulcers commonly open up again after healing. These steps can lower the risk of getting a leg ulcer or a wound recurrence:
- Elevate your legs above your heart when youre sitting or sleeping.
- Maintain a healthy weight and stay physically active.
- Manage health conditions that affect blood circulation, including diabetes, high blood pressure, high cholesterol and Raynauds syndrome.
- Quit smoking and using tobacco products. Talk with your healthcare provider about ways to stop smoking.
- Use gentle cleansers, and apply moisturizing lotion to prevent dry skin.
- Wear compression stockings or bandages for an hour each day to improve blood flow to the legs.
Recommended Reading: How To Know If A Stomach Ulcer Is Bleeding
Cerave Lanolin And Fragrance Free Healing Ointment Skin Protectant With Petrolatum Ceramides
- You can return this item for FREE within the allowed return period for any reason and without any shipping charges. The item must be returned in new and unused condition.
- Extra 20% discount with code MC20. Discount by Amazon. Extra 20% discount with code MC20 when using MasterCard Credit cards at checkout. Please redeem the claim code only once. Discount by Amazon.
What Is A Venous Leg Ulcer
The cause of venous leg ulcers is venous insufficiency due to damage in the valves in the larger veins. Venous leg ulcers can be painless, but some are very painful. They can become infected. There is often an inflammation around the venous leg ulcer.
Competent and well functioning valves are necessary for:
- Fractionating blood flow
When you valves are damaged:
- Blood accumulates in the lower legs
- High blood pressure
This means that the veins or blood vessels by which the blood returns to the heart, are not functioning efficiently, which results in accumulation of the blood in peripheral blood vessels and increased pressure in lower leg veins. The consequence is fluid leackage from the veins beneath the skin. This results in swelling, thickening and damage to the skin. The damaged fragile skin may break down and form an ulcer.
Read Also: Janus Kinase Inhibitor Ulcerative Colitis
Side Effects Of Leg Ulcers
- Fever
- A green and foul-smelling discharge from the ulcers
- The skin around the ulcers begins to swell
- The sores become bigger
- Inflamed skin around the ulcers
Leg ulcers resemble sores that develop when bacteria enter underlying tissues through injured or broken skin. While skin injuries are the most common risk factor for leg ulcers, certain underlying medical conditions like diabetes, arterial disease, and venous disease may also lead to leg ulcers. Some common signs and symptoms that often accompany leg ulcers include irritated or flaky skin, swelling, heaviness, discoloration, and leg pain on prolonged standing. You may use natural ingredients like Gotu kola, turmeric, aloe vera, coconut oil, tea tree oil, and yarrow in home remedies to heal leg ulcers in mild to moderate cases.
Who Gets Foot And Toe Ulcers
Foot and toe ulcers can happen to many people but might be more common in Black, Native American and Hispanic people. If you have an eye, kidney or heart disease related to diabetes, youre also at a higher risk. About 15% of people with diabetes will get an ulcer, typically on the bottom of their foot. Some of those people will be hospitalized because of complications.
Youre also at a higher risk of getting foot and toe ulcers if you have any of the following conditions:
- Blood circulation issues.
- Grey.
- Black.
If your ulcer is black, that means cells in the tissues have died. This is called necrosis .
Recommended Reading: Best Things To Eat With Ulcerative Colitis
After The Ulcer Has Healed
Once you have had a venous leg ulcer, another ulcer could develop within months or years.
The most effective method of preventing this is to wear compression stockings at all times when you’re out of bed.
Your nurse will help you find a stocking that fits correctly and you can manage yourself.
Various accessories are available to help you put them on and take them off.
Page last reviewed: 11 January 2019 Next review due: 11 January 2022
Clinical Use Of Honey
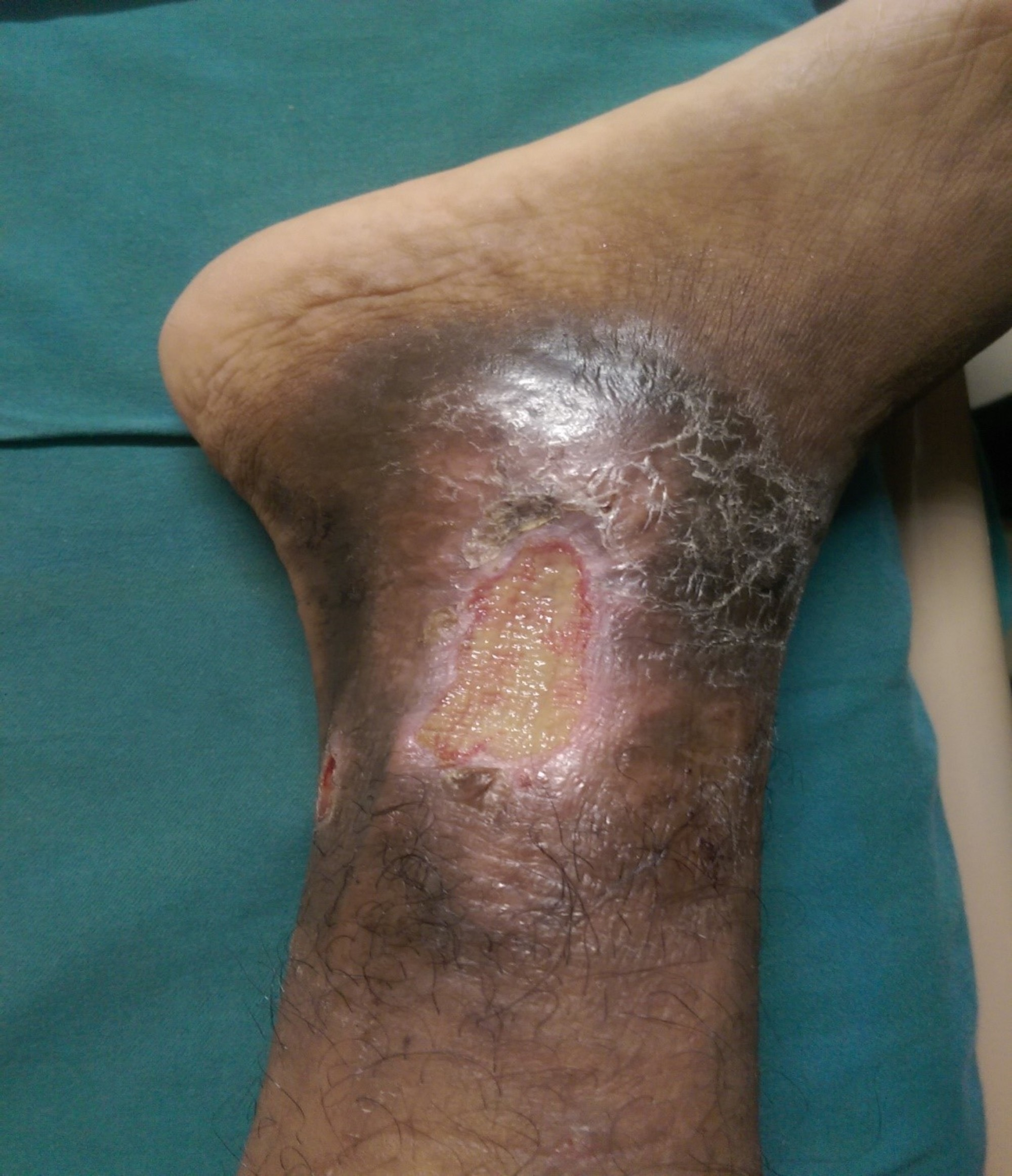
Several studies have proven that local honey is beneficial for wounds, cuts, minor burns, bed sores and even leg ulcers. But, this does not mean you can simply dab honey as much as you want on the affected area.
- The amount of local honey required on the wound relates to the amount of fluid exuding from the wound diluting it.
- It is recommended to apply honey to an absorbent dressing prior to application. When applied directly to a wound, the honey may run off before the application of a dressing to hold it in place.
- Honey may not soak readily into absorbent dressings. To facilitate soaking, warm the honey to body temperature. You can also add 1 part water to 20 parts honey to make the honey more fluid.
- To treat cavity wounds, a blister of honey can be held on a wound using an adhesive film dressing.
- As infection may lie in the tissues underlying the wound area, honey dressings may be needed beyond the inflamed area surrounding a wound.
Read Also: Ulcerative Colitis And Colon Cancer Statistics
Causes Of Venous Leg Ulcers
A venous leg ulcer is the most common type of leg ulcer. They are caused by diseases of the leg veins such as varicose veins or as a complication of a DVT .
Venous leg ulcers can develop after a minor injury. It can happen where persistently high pressure in the veins of the legs has damaged the skin.
Natural Treatment For Diabetic Leg Ulcers
Of course, a proper diabetes diet and blood sugar control are essential to preventing leg ulcers. For any existing, open ulcers, cleaning and dressing the wound is essential. You may want to consider coating the wound with honey as a natural antibiotic to supplement your immune systems own efforts to prevent infection. Supplemental zinc and vitamin C will speed up the healing process. As one more option, phototherapy offers a promising alternative medicine treatment for diabetic leg ulcers.
I have this Ulcer on my right leg., . Being a tropical ulcer, it weeps and defuses bad odor where ever I went., Thus making it harder for me to travel in public vehicles.., its also very painful and caused inflammation to my right leg, that walking short distance is avoided.., into the third week of this misery a good friend of mine came for a visit and saw me in this misery., that friend suggested using Coconut Activated Charcoal therapy., and he advised me how to build a simple Charcoal Kiln and process the Activated Charcoal,, now Im on this therapy and Im satisfied with the results.., the oozing had stop and almost 95% of the odour is gone,, currently Im on the mend, after 3 days of consumption and sprinkling the the charcoal onto the ulcer.
Baby Aspirin for Diabetic Leg Ulcers
Within days, the ulcers started healing, and now a month later, theyre completely gone, no trace!
You May Like: How To Cure Gastritis And Ulcers Naturally
Ways To Treat Venous Leg Ulcer And Its Symptoms
Venous leg ulcer is a sore that develops on the leg and heals very slowly, typically due to poor circulation through the limb. The sore may persist for only a few weeks, or it may last for years.
There are preventative steps you can take to keep from getting them. Venous leg ulcers can cause more serious issues if theyre untreated.
The condition occurs when the veins in your leg fail to send blood adequately back to your heart. The built-up backflow of blood increases the pressure at the end of your leg, which weakens this skin.
In turn, its more difficult for a scrape or cut to heal. These ulcers often occur on bony areas like the ankle.
Venous And Arterial Leg Ulcers
A leg ulcer occurs when skin breaks down, usually on the lower leg area, just above the ankle. Leg ulcers affect about 1 in 1000 people in Europe and are more frequent in elderly people: about 20 out of 1000 people are affected by the time they reach their eighties.
The majority of leg ulcers, about 80%, are caused by venous disease , about 20% are of arterial or mixed origin. If not treated correctly, a leg ulcer can become a chronic wound which requires longer healing time , and they have a tendency to reoccur.
Don’t Miss: Side Effects Of Ulcerative Colitis
Can Leg Ulcers Be Prevented
To prevent and promote healing of ulcers:
- Avoid injury, particularly when pushing a supermarket trolley. Consider protective shin splints.
- Walk and exercise for at least an hour a day to keep the calf muscle pump working properly.
- Lose weight if you are overweight.
- Stop smoking.
- Check your feet and legs regularly. Look for cracks, sores or changes in colour. Moisturise after bathing.
- Wear comfortable well-fitting shoes and socks. Avoid socks with a tight garter or cuff. Check the inside of shoes for small stones or rough patches before you put them on.
- If you have to stand for more than a few minutes, try to vary your stance as much as possible.
- When sitting, wriggle your toes, move your feet up and down and take frequent walks.
- Avoid sitting with your legs crossed. Put your feet up on a padded stool to reduce swelling.
- Avoid extremes of temperature such as hot baths or sitting close to a heater. Keep cold feet warm with socks and slippers.
- Consult a chiropodist or podiatrist to remove a callus or hard skin.
- Wear at least Grade 2 support stockings if your doctor has advised these. This is particularly important for the post-thrombotic syndrome, leg swelling or discomfort, and for long-distance flights.
- Have a vascular ultrasound assessment and consult a vascular surgeon to determine whether any vein treatment should be carried out.
- Horse chestnut extract appears to be of benefit for at least some patients with venous disease.
How Are Foot And Toe Ulcers Diagnosed
Your healthcare provider can tell what type of ulcer you have based on four observations:
- The appearance of the ulcer.
- Location of the ulcer.
- The appearance of the borders.
- The appearance of the surrounding skin.
Your primary healthcare provider can diagnose an ulcer, but they might send you to a specialist for treatment. You might see a podiatrist, a provider who works with feet, or a wound specialist. For more complicated cases that require surgery, you might also see a plastic surgeon, anesthesiologist, orthopedic surgeon and/or vascular surgeon.
You May Like: Best Protein Shakes For Ulcerative Colitis
What Questions Should I Ask My Healthcare Provider
You may want to ask your healthcare provider:
- What caused the leg ulcer?
- What is the best treatment for me?
- What changes can I make to heal the wound and prevent future ulcers?
- Should I look out for signs of complications?
A note from Cleveland Clinic
Leg ulcers can be painful, unsightly and difficult to treat. Chronic leg ulcers need specialized wound care to prevent infection and aid healing. Your healthcare provider may recommend other treatments like medicines or procedures to improve blood flow to the leg. Even after they heal, leg ulcers can break open again. Your provider can offer suggestions on how to prevent a wound recurrence.
Last reviewed by a Cleveland Clinic medical professional on 06/23/2022.
References
What Causes Diabetic Ulcers

Alcohol, tobacco use, obesity, heart disease, and kidney disease are just a few factors that increase the risk of these ulcers. Poor-fitting shoes can also cause blisters on the toes and sole of the foot that can worsen quickly. High blood sugar suppresses immune response, so infection can create complications.
Also Check: How To Treat Gum Ulcers
What Are Neurotrophic Ulcers
Neurotrophic ulcers occur primarily in people with diabetes, although they can affect anyone who has impaired sensation in their feet. They can be found anywhere on your feet, but they usually develop on the parts of your feet and toes that are most sensitive to weight .
Neurotrophic ulcers dont cause pain. But they can be serious if they arent treated promptly or they dont respond to treatment.
A neurotrophic ulcer might be the following colors:
- Pink.
- Black.
- Any combination of those colors.
The thin borders of the ulcers are punched out, meaning that theyre taller than the surrounding tissues.
Ways To Treat Venous Leg Ulcer
Learn how to treat venous leg ulcers now.
1. Clean and Dress the Ulcer
One of the most important first steps is to clean and dress the ulcer. With any abrasion of the skin, you want to make sure the wound is cleaned.
Improper wound care can allow bacteria to gather in the wound, which then leads to infection. If your ulcer becomes infected, you might have to take antibiotics to kill the bacteria.
To clean the ulcer, run it under cold water with a damp washcloth before using an anti-infection cream. Since the wound breaks the skin, cover it with a bandage.
You should be able to find bandages and anti-infection creams at your local drugstore. Its also possible to make homemade bandages by taping down a pad of sterile gauze.
As the ulcer takes an increased amount of time to heal, be sure to intermittently replace the bandage and make sure the wound is still clean.
2. Compression Socks and Bandages
The most common treatments to address a venous leg ulcer are compression socks and bandages. Compression socks can also be found at your local drugstore.
These stockings gently compress the legs and narrow blood vessels, causing blood circulation to improve. It will also help decrease leg swelling. If you get a notice from your doctor that you have a medical reason for the compression socks, it may be possible to get a reimbursement from your insurance company.
3. Elevate the Legs
4. Moisturize to Reduce Itchy Skin
5. Stay Active Through Walking
Don’t Miss: How To Know If I Have Ulcerative Colitis