Choice Of Ileal Pouch Size And Type
Although most surgeons do not use the S pouch as the first option , the spout created in its construction provides an additional 3-5 cm in length to the entire ileal reservoir, as compared with the length of a J pouch.
Some still advocate straight ileoanal pull-through anastomosis without reservoir construction. Straight endorectal pull-through causes dilatation and compensation over time so that the pouch develops a reservoir function. In addition, length is generally not a problem with a straight pull-through. Thus, many pediatric surgeons perform this as their primary procedure. Good long-term outcomes and patient satisfaction are reported.
However, others have noted a need for revision of the straight pull-through configuration in 70% of cases. Construction of the ileal J pouchanal anastomosis is described below. One should keep in mind that the straight ileoanal pull-through is performed in essentially the same manner and uses less total length of small bowel.
In summary, the choice of pouch size and type involves a balance between increasing reservoir function to decrease stool frequency and the risk of developing pouchitis. All reservoirs have a tendency to enlarge over time. Consequently, most surgeons have opted for a smaller initial reservoir that depends on reservoir enlargement to gradually decrease stooling frequency while avoiding pouchitis.
Risk Of Cancer And Dysplasia
Compared to the general population, the risk of colorectal cancer is increased in patients with UC . Accordingly, a surveillance colonoscopy should be performed annually in patients with pancolitis and a disease duration 8 years. Patients with a left-sided or distal colitis should be submitted to surveillance colonoscopy every 1 or 2 year after a disease duration of 15 years .
In case of a histologically proven colitis-associated high-grade intraepithelial neoplasia /dysplasia a proctocolectomy is indicated after the diagnosis has been confirmed by an external pathologist. For resection of manifest colitis-associated cancer, the same principles apply as for the oncological resection of sporadic colorectal cancer.
In the presence of a low-grade IEN/dysplasia in flat mucosa – also confirmed by an external pathologist – either proctocolectomy or an endoscopic biopsy control within 3 months should be offered to the patient . The patient has to be informed of the risk of malignancy. In this situation, other centers and we advise the patient to undergo surgery because a sampling error’ represents a significant risk of missing a high-grade dysplasia or carcinoma in repeated colonoscopies.
Medical Versus Surgical Management Of Refractory Moderate
Reconstructive surgery may be offered to refractory and corticosteroid-dependent patients and improves quality of life despite the risk of early and late complications . Proctocolectomy with end-ileostomy is an alternative for some patients and has lower morbidity and comparable quality of life
Five systematic reviews were performed to define the risk of early and late complications after restorative proctocolectomy with IPAA. Early complications occurred in 965% of patients, and late complications occurred in 355% of patients., Systematic reviews indicate that the most frequent complications were pouchitis ,, wound infection ,,, bowel obstruction ,, ileus , sepsis ,, anastomotic leak ,, and fistula . The most common late complications were ileus , faecal incontinence , pouch loss ,, chronic pouchitis ,, Crohns-like disease of the pouch , and fistula . The overall mortality rate after surgery was 0.1%.
The studies that compared ileostomy with IPAA were all retrospective and revealed similar results, using a different QoL score. Occasionally the scores obtained in specific domains of health-related QoL differed significantly between the surgical techniques . Removing the diseased colon offers a good QoL when compared with medical treatment in UC patients, with a morbidity ranging between 20% and 25%.
Read Also: What To Take For An Ulcer Over The Counter
Children And Young People
Much of the information here will apply to children as well. However, there are some things to be aware of:
- Surgery on children and young people often takes place in specialist hospitals. This may mean you have to travel further for the surgery.
- Children cannot consent to treatment until they are 16 years old.
- The growth and development of a child or young person will be important in deciding if surgery is suitable for them.
- Children and young people may be given some specific instructions before surgery. For example, avoiding vaccinations in the few weeks before surgery.
CICRA has more information on surgery in children with Colitis.
I was only 10 so I spent some time wearing a bag pre surgery to get used to it on my tummy, sometimes we filled it with water to get used to the sensation of it being full, we also put a bag on my teddy bear.
Medical Management Of Asuc
Intravenous corticosteroids as the initial standard treatment for adult patients with ASUC are recommended, as this treatment induces clinical remission and reduces mortality
The only randomised controlled trial including placebo in the setting of ASUC is the paramount work by Truelove and Witts, who observed that steroids induced clinical remission and decreased mortality without increasing serious adverse events., Risk of bias led to downgrading of the evidence level from 2 to 3. No conclusions could be drawn about the need for surgery, as the authors included derivative ostomies and colectomies without distinguishing the type of surgery in the report. Since the results of this pivotal study, placebo-controlled trials to clarify these and other aspects would be unethical.
Either infliximab or cyclosporine should be used in adult patients with steroid-refractory ASUC. When choosing between these strategies, centre experience and a plan for maintenance therapy after cyclosporine should be considered
There is currently insufficient evidence to determine the optimal regimen of infliximab rescue therapy in patients with ASUC refractory to corticosteroid therapy
A retrospective cohort study did not reveal differences in short-term or long-term colectomy rates between ASUC patients treated with accelerated- or standard-dose infliximab.
Recommended Reading: How To Treat Peptic Ulcer Disease
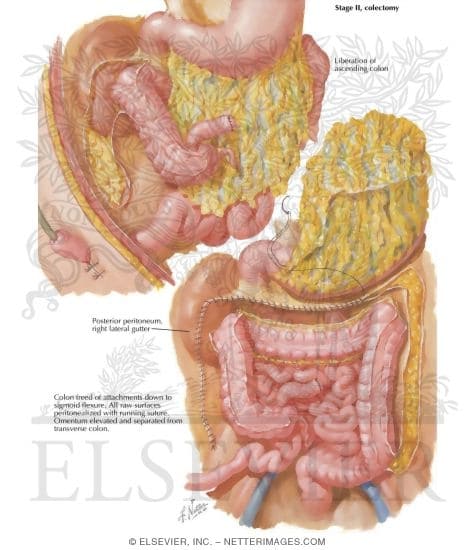
Surgical Treatment Of Ulcerative Colitis
Submitted: February 6th, 2011Published: November 2nd, 2011
DOI: 10.5772/26268
There are two ways to cite this chapter:
There are two ways to cite this chapter:
Total Chapter Downloads on intechopen.com
Silvestro Canonico
*Address all correspondence to:
Management Of Ulcerative Colitis
Management of ulcerative colitis involves first treating the acute symptoms of the disease, then maintaining remission. Ulcerative colitis is a form of colitis, a disease of the intestine, specifically the large intestine or colon, that includes characteristic ulcers, or open sores, in the colon. The main symptom of active disease is usually diarrhea mixed with blood, of gradual onset which often leads to anaemia. Ulcerative colitis is, however, a systemic disease that affects many parts of the body outside the intestine.
Recommended Reading: Foods That Affect Ulcerative Colitis
Ulcerative Colitis Treatment: Surgery
If you did not respond to a medication regimen or you developed complications of colitis, you may be a candidate for surgery to treat ulcerative colitis.
Colectomy may be used in children with ulcerative colitis who experienced growth retardation. In all patients, elective colectomy can be a cure for ulcerative colitis. Almost always, the procedure is a total colectomy, meaning the entire colon is removed.
Surgical procedures include:
-
Total proctocolectomy with Brooke ileostomy. Removal of your entire colon and rectum. Your doctor will perform an ileostomy, which brings out your small intestine through the abdominal wall. Waste collects in an ileostomy bag. An ileostomy can be temporary or permanent.
Colitis Coming Back After Surgery
Colitis cant come back if the whole large bowel has been removed. However, some people still have symptoms outside of the gut, such as in their joints or eyes.
For most people, removing the large bowel should mean:
Colectomy with ileo-rectal anastomosis is a type of surgery where your rectum is not removed. If you have surgery that leaves your rectum inside, you could still get inflammation in your rectum. Medicines such as 5-ASAs may be able to help control this inflammation.
Colitis is different for everyone, and the risks and benefits of each treatment will vary from person to person. Having any type of surgery will carry some risks. These include a risk of infection and risks linked to having a general anaesthetic such as having an allergic reaction to the anaesthetic.
There is also a risk of developing blood clots after surgery. And this risk is higher in people with Colitis. Your surgical team will assess your risk of blood clots before you have surgery and will put measures in place to reduce this risk.
Some surgeries for Colitis carry other risks. Your surgical team can tell you more about these complications, how common they are, and how they are usually treated. They include:
Recommended Reading: Ozanimod Phase 2 Ulcerative Colitis
How Long Your Surgery Will Take
This will depend on the type of surgery youre having, whether it is keyhole or open surgery and if youve had surgery on your tummy before. If youve had surgery on your tummy before you may have scar tissue called adhesions. Adhesions can sometimes make surgery more complicated, so it can take longer. Your surgical team can tell you how long they expect your surgery to take.
After surgery youll be moved to a recovery ward. This is a small ward where nurses will monitor you as you wake up properly. The medicines that put you to sleep take a couple of hours to fully wear off. You may not remember waking up, or the first couple of hours after you wake up.
The medicines used during surgery can make you feel sick. You may also have a sore throat. This is usually because of the tube thats put into your throat to help you breathe during surgery. This tube is taken out when you wake up. If you feel unwell, let the nurses know and theyll be able to help you.
What Are The Benefits Of Ulcerative Colitis Surgeries
If the entire colon and rectum are removed, ulcerative colitis is cured. This should put an end to the diarrhea, abdominal pain, anemia, and other symptoms.
In addition, this surgery prevents colon cancer. Overall, an estimated 5% of ulcerative colitis patients will get cancer. Removing the colon cancer threat is especially significant for people who have ulcerative colitis that affects the entire colon. In these cases, as opposed to cases of ulcerative colitis that affect only the lower colon and the rectum, the cancer risk without surgery could be up to 32 times the normal rate.
Also Check: Best Probiotic Brand For Ulcerative Colitis
Meet Your Uc Surgeons And Team
Most people who have surgery for ulcerative colitis are referred from their gastroenterologist. The surgeon that will complete the surgery is most often a colorectal surgeon, who specializes in surgery of the digestive system.
An enterostomal therapy nurse will be helpful before and after surgery to place an ileostomy. An ET nurse will help decide where the stoma will be placed and will make suggestions on which type of appliance will work best.
Ulcerative Colitis Surgery Cost
As surgery for ulcerative colitis requires at least one and possibly three hospital stays, it comes at a higher cost than procedures that can be done as outpatient surgery. Ileostomy surgery may cost approximately $39,000, while j-pouch surgery may cost $50,000.
Check with your insurance provider to find out how much will be covered and what co-pays may be required. Using a hospital and surgical team in your plan’s network is key to preventing any unexpected charges.
Also Check: How Do You Heal A Bleeding Ulcer
Sudden Severe Ulcerative Colitis
This complication is the main cause of emergency surgery in patients with ulcerative colitis. With sudden, severe ulcerative colitis, medications and intravenous steroids, are unable to control the symptoms.
-
Uncontrolled bleeding can occur from deep ulcerations in the colon, though that is rare.
-
Severe, sudden ulcerative colitis can lead to toxic megacolon, a potentially life-threatening complication caused by severe inflammation.
-
Toxic megacolon leads to rapid enlargement of the colon. Symptoms include pain, distension or swelling of the abdomen, fever, rapid heart rate, constipation, and dehydration.
-
Toxic megacolon requires immediate treatment and surgery.
Proctocolectomy With Brooke Ileostomy
Description of procedure
Indications
Most patients are suitable candidates for this operation irrespective of age. The choice of this operation is often appropriate for patients who wish to avoid the problems associated with ileoanal pouch procedure or those who are not suitable candidates for a resortative procedure, especially in elderly patients and those with poor sphincter function.
Contraindications
IPAA is now the surgical procedure of choice in most patients with UC .
Contraindications
Operative factors
The ileal pouch is constructed using one of the several pouch designs, which include the J-pouch, S-pouch and W-pouch. The ultimate choice of pouch design is largely the surgeon’s preference, studies to date suggesting that J and W produce similar results. The S pouch is considered an inferior design, especially when there is a long exit spout, as this can cause obstructive defecation problems which at times require intubation of the pouch to empty it . The J-pouch design is the most commonly used in part due to the ease of construction.
Complications
Bowel obstruction is common following all types of surgery for UC. The annual risk for patients following IAPP is 1 in 25, 1 in 49 for a Kock pouch, 1 in 66 for a proctocolectomy and Brooke ileostomy, and 1 in 71 for colectomy and ileorectal .
Outcome
You May Like: Does Ulcerative Colitis Make You Tired
Refractory Course And Corticosteroid Resistance
A treatment-refractory course, despite the use of immunosuppressive drugs including biologicals, represents an absolute indication for surgery. Similarly, the patient should be operated on if corticoid dependence is obvious, i.e. the corticoid medication cannot be lowered below the Cushing threshold of 7.5 mg of prednisolone equivalent daily. From this course of the disease, which comprises weeks or months, the intractable fulminant flare must be distinguished which cannot be controlled even by high doses of corticosteroids and requires emergency surgery.
Things To Think About Before Having Surgery
- Transport how will you get to and from hospital?
- Next of kin who should the hospital contact with updates about your hospital stay? Are they ok with being contacted?
- Work and volunteering will you need to take time off and who should you talk to about this?
- Caring responsibilities do you care for anyone, such as children, a relative, or a partner? Any pets? Who will be looking after them whilst you are in hospital and whilst you recover at home?
- Pre-hospital instructions did your surgical team give you any instructions on what to do before coming in, like stopping medicines?
- Going home will somebody be able to help you when you go home? Can you get food delivered?
- Hospital visiting policy when can people come to visit you?
Also Check: Foods To Avoid With Bleeding Ulcer
Technical Aspects Of Surgical Approaches For Refractory Moderate
IPAA may be constructed using either a stapled or a handsewn technique, with comparable functional outcomes. Thus, the type of anastomosis should be left to the surgeons discretion
Overall, stapled and handsewn IPAAs seem to result in comparable complication rates, functional outcomes, and QoL. In a meta-analysis of four randomised controlled trials including 184 patients , no significant differences were observed in terms of functional outcomes, sphincter resting pressure, or squeeze pressures. Based on low-quality evidence, the stapled technique may be more likely to achieve perfect continence compared with the handsewn approach. Despite slightly better functional outcomes after stapled anastomosis, overall QoL appears equivalent between the two groups.,
Due to a paucity of high-quality data, no recommendations can be made with regards to sexual function, strictures, and septic complications between stapled and handsewn techniques, although stapled IPAA is likely associated with a higher rate of cuffitis.,
Laparoscopic surgery is the preferred approach to patients with medically refractory UC, as it is associated with lower intra- and postoperative morbidity, faster recovery, fewer adhesions and incisional hernias, shorter hospital length of stay, improved female fecundity, and better cosmesis
Feeling Better After Surgery
When you feel better will be different for each person. When you first get home, youll probably feel quite weak and tired. You may not feel like doing much.
You should avoid any strenuous exercise for at least a few weeks after your surgery. This is so your wounds can heal properly. This means avoiding any heavy lifting or housework. You may struggle to go up stairs for a short time after surgery.
I couldn’t even lift a full kettle when I was first home. When I had to be on my own, my dad would make a flask of tea for me to have throughout the day, as this was easier for me to lift and pour. I also found it very useful to wear loose long T-shirts or nightgowns so that clothing didn’t pull on my stomach which was very sore for the first few days.
NiaLiving with Colitis
As time goes on youll notice your strength coming back. After a few weeks, you should be able to gradually introduce exercise into your daily routine. A gentle exercise programme may help speed up your recovery and you will likely be given advice on this by your surgical team.
You should be able to start going back to your normal daily activities. Its important to listen to your body and only do as much as feels comfortable. Everybody is different, so try not to put too much pressure on yourself to get back to normal life straight away.
Living with Colitis
Read Also: Pressure Ulcer Cream Over The Counter