Venous Leg Ulcers: 6 Things To Know When Treating Venous Disease
Lower extremity venous disease affects millions of Americans and may ultimately lead to open, draining wounds that adversely affect quality of life. However, there are exciting developments in early diagnosis, prevention and treatment of venous leg ulcers . On the treatment side, there are more choices now than ever before in compression products, which is greatly improving the patient experience. But proper treatment also comes from a better understanding of venous leg ulcers, and better understanding comes from more education. Luckily, were here to help provide education and support for you and your team, so here are six things to know when treating VLUs.
You May Like: Can Ulcers In The Colon Be Cancerous
Foam Dressings For Venous Leg Ulcers
Venous leg ulcers are a common and recurring type of chronic wound. Compression therapy is used to treat venous leg ulcers. Dressings that aim to protect the wound and provide a moist environment to aid ulcer healing are applied beneath compression devices. Foam dressings are one of several types of dressing available. We evaluated the evidence from 12 randomised controlled trials that either compared different types of foam dressings, or compared foam dressings with other types of wound dressings. We found no evidence to suggest that polyurethane foam dressings are significantly better or worse than hydrocellular foam dressings in venous leg ulcer healing. Similarly, we found no evidence to suggest that foam dressings are significantly better or worse than other types of dressings , for the healing of venous leg ulcers. We found insufficient evidence to draw any conclusions regarding: adverse events, quality of life, costs, pain, or dressing performance. Overall, the current evidence is of low or unclear methodological quality. This limits the making of any specific recommendations regarding the use of foam dressings. Further, good quality evidence is required before definitive conclusions can be made regarding the role of foam dressings in the management of venous leg ulcers.
You May Like: Best Treatment For Stage 2 Pressure Ulcer
What Causes A Venous Ulcer
Vein disease is the root cause of a venous ulcer. Vein disease develops when the one-way valves inside of a vein stop functioning correctly. The one-way valves are designed to push blood toward the heart however, sometimes the valves weaken and are unable to adequately return the blood to the heart. As a result, excess blood remains in the vein, which creates increased pressure on the vein wall. Further, the excess blood has nowhere to go, so it pools in the lower extremities. The pooled blood may seep out of the vein and into surrounding tissue, causing the skin to become discolored and tender. If left untreated, the excess blood and pressure can break down the skin from the inside out and create open, painful sores on the surface of the skin. Once a venous ulcer has developed, it can be challenging to treat and can take weeks, months or even years to heal.
Also Check: Stomach Ulcer Blood In Stool
Can Venous Leg Ulcers Be Prevented
There are several ways to help prevent a venous leg ulcer in people at risk, such as:
- wearing compression stockings
- losing weight if youre overweight
- exercising regularly
- elevating your leg when possible
This is particularly important if youve previously had a leg ulcer once a leg has suffered a venous ulcer, youre at risk of further ulcers developing within months or years.
Differentiating Lower Extremity Wounds
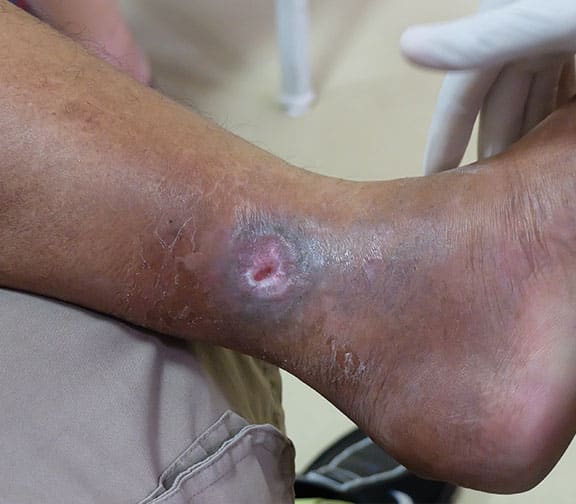
Understanding other lower extremity woundsarterial ulcers, neuropathic ulcers, and pressure injuriescan help nurses differentiate them from venous ulcers. A detailed clinical history and thorough assessment when evaluating lower extremity ulcers can aid diagnosis and guide treatment, which may differ depending on the type of ulcer.
Treatments for some types of wounds may be harmful for others. For example, if compression therapy is applied to a limb with arterial insufficiency that resulted in an arterial ulcer, blood flow can be reduced further, potentially leading to amputation.
Arterial ulcers
Arterial ulcers are small, have an irregular shape, and appear punched-out with a deep base. Typically, necrotic tissue is present with low exudate unless the wound is infected. The ulcers usually are located over the pretibial area, the lateral malleolus , or on the toes or heel.
Most patients report severe pain thats relieved when the extremity is placed in a dependent position and increased when the extremity is elevated. Assessment findings include abnormal distal pulses, cold extremities, and prolonged venous filling time. Arterial ulcers may be caused by tissue ischemia resulting from atherosclerosis.
Arterial vs. venous ulcer
The following table compares venous and arterial ulcers, which can occur as a result of peripheral vascular disease.
| Arterial |
Pressure injuries
Don’t Miss: Side Effects Of Bleeding Ulcer
How Soon After Treatment Will I Feel Better / How Long Does It Take To Recover From This Treatment
Vascular ulcers can take weeks or even months to heal under normal circumstances. However, if cared for properly including closely following the treatment plan provided to you wounds should heal faster than expected. Your provider can tell you what to expect based on your specific wound issue and can help you track your progress along the way.
Treatment For Venous Stasis Ulcer
Compression therapy and direct wound management are the standard of care for VLUs. For wound closure to be effective, leg edema must be reduced. Treatment for venous stasis ulcer should usually include:
- Compression therapy. The most practical, efficient, and economical intervention for the treatment of VLUs is compression therapy. This calls for the use of various hosiery or bandages, which may be single- or multi-layered, elastic or inelastic, etc.
- Wound management. Cleaning, debridement, infection control, dressing application, and topical medication are all direct ulcer interventions. To minimize harm to the live tissue, cleaning should be done with a non-toxic substance. Debridement is possible and highly advised by surgically removing non-viable tissue. To lessen discomfort, the anesthetic may be applied topically or intravenously. Enzymatic drugs, larval therapy, and autolytic dressings are non-invasive debridement alternatives, albeit recovery times may be prolonged.
- Debridement. For new tissue to the surface, dead and necrotic tissues must be surgically removed. For larger wounds, reconstructive surgery may also be necessary, and flaps will be used to cover the wounds.
- Wound dressing. Dressings promote granulation and re-epithelialization, maintain a sufficient moisture level, and provide physical protection. To treat dry, exudative, and infected wounds, respectively, a variety of absorbent , and moisture-retaining .
Recommended Reading: What Do Doctors Prescribe For Ulcers
Prevention Of Venous Stasis Ulcer
The following lifestyle changes must be implemented to increase circulation and lower the risk of developing venous stasis ulcers:
- Antihypertensive medications. Maintain the course of treatment for persistent ailments like high blood pressure that have an impact on vein health.
- Maintain a healthy weight. High pressure in the leg veins brought on by being overweight might harm the skin.
- Quit smoking. Smoke-damaged veins result in chronic venous insufficiency, a condition marked by continuously inadequate blood flow. The legs may swell, cramp, and develop skin ulcers as a result.
- Anticoagulants. If prescribed, take anticoagulants to prevent blood clots.
- Be physically active by doing regular exercise. Regular exercise and a healthy, balanced diet are advised to aid with weight loss.
- Wear compression stockings. Because of their unique design, these stockings will compress the legs, increasing circulation.
- Elevate the legs. An extended time standing or sitting should also be avoided. Every time this happens, elevate the patients legs unless contraindicated.
What Causes Sacral Pressure Ulcers
Pressure ulcers occur when there is prolonged pressure to the skin, usually over bony areas such as the elbows, spine, or sacral area .
Compression of the soft tissue causes blood vessels to collapse and reduces blood flow and oxygen delivery. This localized tissue damage usually happens when a person sits or lays for long periods of time in a chair, wheelchair, or bed.
Pressure ulcers begin forming under the skin, making them difficult to catch before a wound is actually visible. So its important to take these steps to help prevent sacral pressure ulcers from happening.
Also Check: Ulcer Pain Relief At Night
Read Also: Can You Get An Ulcer In Your Colon
How Long Does It Take For A Venous Leg Ulcer To Heal
Overview Venous leg ulcer. A leg ulcer is a long-lasting sore that takes more than 2 weeks to heal. They usually develop on the inside of the leg, just above the ankle. The symptoms of a venous leg ulcer include pain, itching and swelling in the affected leg.
When to see a doctor for a venous stasis ulcer?
These can take months to heal and, if not healed within a year, may never heal completely. Consult a doctor right away if you suspect you have a venous stasis ulcer. Thoroughly clean the ulcer with a sterile wound cleansing pad and apply a new sterile dressing every day.
How to speed up the healing time of an ulcer?
Talk to your doctor about whether taking aspirin may help your condition. You may take 300mg of aspirin daily, which is safe for most people. This may speed up your healing time if you also use your compression bandage. Consider surgery if your ulcer doesnt heal in six months. Most ulcers heal with proper treatment.
What Is A Venous Ulcer
Venous ulcers are open wounds around the ankle or lower leg.
They do not heal for weeks or months and sometimes longer.
Venous stasis ulcers are often on the ankle or calf and are painful and red.
A yellow, fibrous tissue may cover the ulcer and have an irregular border. Drainage and discharge are common with venous stasis ulcers.
This type of ulcer is common in people who have varicose veins or a history of leg swelling.
Don’t Miss: Bed To Prevent Pressure Ulcers
A Comparison Of The Efficacy And Cost Of Different Venous Leg Ulcer Dressings: A Retrospective Cohort Study
1North Cumbria University Hospitals NHS Trust, Cumberland Infirmary, Newtown Road, Carlisle, Cumbria CA2 7HY, UK
Abstract
Objective. To compare the efficacy and cost-effectiveness of simple nonadherent dressings with other more expensive dressing types in the treatment of venous leg ulcers. Study Design. Retrospective cohort study. Location. The leg ulcer clinic at the University Hospital of South Manchester. Subjects and Methods. The healing rates of twelve leg ulcer patients treated with simple nonadherent dressings were compared with an equal number of patients treated with modern dressings to determine differences in healing rates and cost. Main Outcome Measures. Rate of healing as determined by reduction in ulcer area over a specified period of time and total cost of dressing per patient. Results. Simple nonadherent dressings had a mean healing rate of 0.353cm2/week compared with a mean of 0.415cm2/week for more expensive dressings. This resulted in a one-tailed value of 0.251 and a two-tailed value of 0.508. Multiple regression analysis gave a significance of 0.8134. . The results indicate that the difference in healing rate between simple and modern dressings is not statistically significant. Therefore, the cost of dressing type should be an important factor influencing dressing selection.
1. Introduction
2.2. Alternative Hypothesis
Juzo Ulcer Pro Wound Care Compression
Product Description
The Juzo UlcerPro is a two-layered system that can be applied over top of wound dressings while providing therapeutic compression.
- Dual stretch zones for ease of donning & optimal fit
- Holds wound dressings in place
- Supports movement to encourage physical activity
If you would like to order compression garments online, please call the store at 630-355-6500 or send an email to . If you order without specifying the size or compression you need, we will contact you. We want to ensure that you get the right compression for your needs.
Need to get measured for compression garments? Stop by and have one of our certified fitters help you out! We measure every day from 9:00 to 11:00 AM. Call to schedule an appointment! 630-355-6500
Questions?
Don’t Miss: What Not To Eat With An Ulcer
Venous Stasis Ulcer Risk Factors
Venous stasis wounds typically develop on the lower extremities, near bony and non-fleshy areas. These areas are vulnerable because of their proximity to certain risk factors.
A variety of factors can raise your risk of venous ulcers. They include:
- Family history of venous disease
- Sedentary lifestyle with limited physical activity
There are many signs of venous ulcers, including:
- Leg swelling and cramping.
- Dull ache or feeling of heaviness in the leg or calf.
- Itchiness and tingling, red-colored skin.
- Signs of pooling blood, including dark red, purple, and brown spots with hardened skin.
- The skin surrounding the ulcers may be shiny, tight, warm, or hot to the touch.
- The borders of the ulcers may be unevenly shaped.
Signs And Causes Of Venous Ulcers
Venous ulcers are non-healing or slow-healing wounds that form as a result of blood pooling in the legs and feet. This happens when the walls or valves in the veins of the lower extremities dont work effectively. This is called venous insufficiency.
Venous ulcers are more common in women and older people. Several factors increase your risk of developing venous ulcers, including:
- Long periods of immobility, such as bed rest
Don’t Miss: Can Ulcerative Colitis Lead To Crohn Disease
Proper Foam Dressing Application Instructions
The procedure for applying a foam dressing is as follows:
The flexibility of foam dressings allows for a wide variety of clinical applications with wounds that have from moderate to heavy exudate. Because they are easy to use and can be easily cut to fit irregular wound areas, they are a good dressing choice for many situations.
The views and opinions expressed in this blog are solely those of the author, and do not represent the views of IncontinenceSource, Kestrel Health Information, Inc., its affiliates, or subsidiary companies.
How Are Stasis Ulcers Diagnosed
Stasis ulceration is usually a clinical diagnosis, made on the basis of the patientâs history and examination findings, and includes the presence of risk factors for venous stasis, that is, congestion and slowing of venous circulation, and the characteristic features of the wound and surrounding tissues.
- Duplex ultrasonography is used to confirm venous obstruction or valvular incompetence prior to saphenous vein ablation surgery
- Concomitant arterial disease is identified using the ankle-brachial index
Other investigations to evaluate venous insufficiency and provide haemodynamic information may include:
- Intravenous ultrasonography
- Haematological studies of the coagulation system.
Also Check: How To Get Rid Of Ulcerative Colitis
Referral To A Specialist
In some cases, your GP or nurse may decide to refer you to a specialist in conditions affecting the blood vessels .
For example, you may be referred to a vascular specialist if your GP or nurse is unsure about your diagnosis, or if they suspect your ulcer may be caused by artery diseases, diabetes or rheumatoid arthritis.
After taking your medical history and examining you, the vascular specialist may need to arrange further investigations to plan your treatment.
Implications For Future Practice
Improving venous ulcer care requires increasing nurse wound care knowledge across settings and ensuring nurses work at the top of their scope of practice. For example, barring exclusion from a states nursing practice act, training in debridement of venous ulcers can be taught to nurses in many settings to facilitate care outside of wound care centers. In addition, nurses and patients can use monofilament devices for mechanical debridement.
The Centers for Medicare & Medicaid Services has paved the way for using telehealth during the pandemic, making it an ongoing viable option for helping patients adhere to treatment recommendations. It can be used for patient and family education and to perform screening and monitoring visits, effectively reducing barriers to care.
For more complex patients, home health nurses should be trained in advanced wound care to help reduce gaps in care during times of crisis and for patients unable to visit a wound care center. In addition, in-person or virtual patient self-care education is vital to ensure proper venous ulcer management if in-office or home health visits arent possible.
Also Check: Pressure Ulcers Are Most Likely To Develop
Nursing Care Plan For Venous Stasis Ulcer 5
Nursing Diagnosis: Impaired Peripheral Tissue Perfusion related to deficient knowledge of risk factors secondary to venous stasis ulcers as evidenced by edema, decreased peripheral pulses, capillary refill time > 3 seconds, and altered skin characteristics.
Desired Outcomes:
- The patient will demonstrate improved tissue perfusion as evidenced by adequate peripheral pulses, absence of edema, and normal skin color and temperature.
- The patient will employ behaviors that will enhance tissue perfusion.
- The patient will demonstrate increased tolerance to activity.
Choosing More Effective Dressings And Medical Adhesives
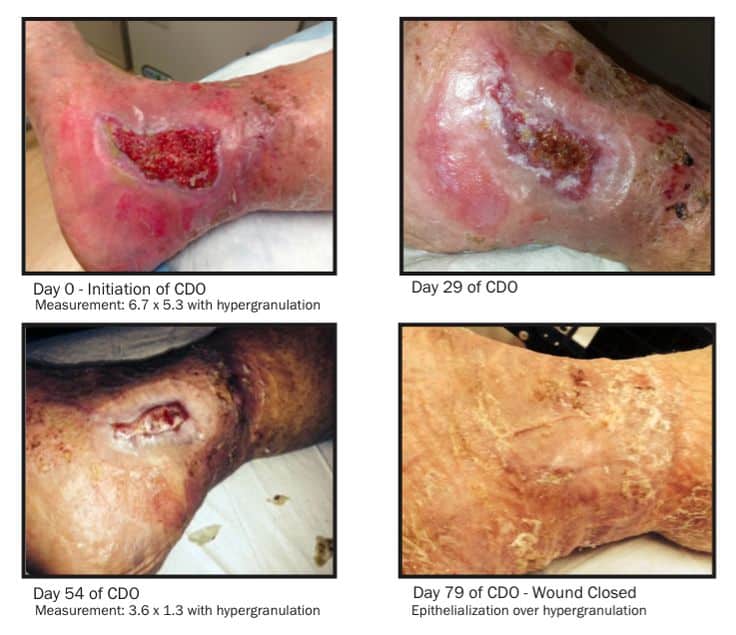
Wound dressings are key components of effective venous leg ulcer treatment. Using the right dressing and using a secure, gentle medical adhesive can help the patient be more comfortable, promote rapid healing, and reduce costs.1 Important considerations when choosing a dressing and medical adhesive for a venous leg ulcer include:
With best practice wound management, it is possible to reduce the impact of venous leg ulcers, even in the most vulnerable populations. Secure wound dressings are essential in the management of exudate to support an optimal healing environment and contain exudate from moderately to heavily draining venous leg ulcers. Use of a strong, moisture-resistant medical tape plays a key role in the effective securement of wound dressings when managing venous leg ulcers. By choosing appropriate dressings based on the level of wound exudate, clinicians can support an optimal healing and can provide the best possible care while reducing costs and time spent changing dressings.
Industry Voices is brought to you by health care industry sponsors. All content is developed and paid for by the sponsoring company. Kestrel Health Information, Inc. is not involved in the creation of this content. The views and opinions expressed in this blog are solely those of the author and do not represent the views of WoundSource, Kestrel Health Information, Inc., its affiliates, or subsidiary companies.
Also Check: Ulcerative Colitis And Lung Disease
Read Also: What Are The Symptoms Of An Ulcer In The Esophagus