What Are The Complications Of Ulcerative Colitis
Ulcerative colitis may lead to complications that develop over time, such as
- anemia, a condition in which you have fewer red blood cells than normal. Ulcerative colitis may lead to more than one type of anemia, including iron-deficiency anemia and anemia of inflammation or chronic disease.
- bone problems, because ulcerative colitis and corticosteroids used to treat the disease can affect the bones. Bone problems include low bone mass, such as osteopenia or osteoporosis.
- problems with growth and development in children, such as gaining less weight than normal, slowed growth, short stature, or delayed puberty.
- colorectal cancer, because patients with long-standing ulcerative colitis that involves a third or more of the colon are at increased risk and require closer screening.
In some cases, ulcerative colitis may lead to serious complications that develop quickly and can be life-threatening. These complications require treatment at a hospital or emergency surgery. Serious complications include
Severe ulcerative colitis or serious complications may lead to additional problems, such as severe anemia and dehydration. These problems may require treatment at a hospital with blood transfusions or intravenous fluids and electrolytes.
It Doesnt Have To Be Chronic
The latest research shows that combining herbal compounds like curcumin and qing-dai with standard medication can quickly induce remission in patients, including those who were non-responsive to drug therapies.
The European Crohns and Colitis Organization lists Curcumin as an effective add-on therapy to 5-ASA in inducing remission in mild-to-moderately active ulcerative colitis
A systematic review published in the Journal of Complementary Therapies in Medicine found that curcumin reduced inflammatory markers and disease activity in patients with Crohns disease. They also indicated curcumin reduces the level of an inflammatory molecule called IL-1, which is believed to be involved- at least partly in loss of response to biological agents. The researchers, coming from Grand Valley University in Michigan, suggested that adding curcumin may prove to be beneficial, and concluded that Curcumin, even by itself, was found to be a cheap and safe way to reduce Crohns disease symptoms and inflammatory markers.
Curcumin add-on treatment maintains remission 4X better than pharmaceutical treatment alone
Gut Directed Curcumin add-on treatment induces over 10X more clinical remission than placebo within 4 WK
Outlook For People With Ulcerative Colitis
If you have UC, a doctor will need to monitor your condition, and youll need to carefully follow your treatment plan throughout your life.
The only true cure for UC is removal of the entire colon and rectum. Your doctor will usually begin with medical therapy unless you have a severe complication that requires surgery. Some people will eventually require surgery, but most do well with nonsurgical therapy and care.
Also Check: Vitamin E And Ulcerative Colitis
Ulcerative Colitis Risk Factors
Most people with UC dont have a family history of the condition. However, about 12 percent of people with UC do have a family member with IBD, according to research from 2014.
UC can develop in a person of any race, but its more common in white people. If youre of Ashkenazi Jewish descent, you have a greater chance of developing the condition than most other groups.
Young people with IBD may also be dealing with acne at the same time. Some older studies have suggested a possible link between the use of the cystic acne medication isotretinoin and UC. However, newer research has yet to find a definitive causal relationship.
Theres no solid evidence indicating that your diet affects whether you develop UC. You may find that certain foods and drinks aggravate your symptoms when you have a flare-up, though.
Practices that may help include:
- drinking small amounts of water throughout the day
- eating smaller meals throughout the day
- limiting your intake of high fiber foods
- avoiding fatty foods
- lowering your intake of milk if youre lactose intolerant
Also, ask a doctor if you should take a multivitamin.
Reduce Stress To Combat Uc Flare

While stress doesnât cause ulcerative colitis, it can trigger flare-ups and make your symptoms worse. Try the following for lowering your stress levels:
- Exercise. Youâve probably heard it a lot, but itâs true â even mild exercise is important for combating stress and inflammatory disease. It can also give you a boost in fighting depression, and it can help keep you more regular.
- Biofeedback. This is a technique that uses a device to help you reduce tension in your muscles and slow your heart rate. There are lots of types of biofeedback machines out there. They give you information about how your body is functioning by measuring different things using sensors. These include brain waves, your breathing or heart rate, muscle contractions, sweat glands, and temperature. Talk with your doctor about what device might be best for you.
- Relaxation and breathing exercises. This could include trying things like yoga and meditation. There are many options depending on your needs, from in-person classes to videos online.
- Get enough sleep. This can help you better cope with stress and prevent flare-ups.
- Talk to a mental health pro. A therapist, counselor, or psychiatrist can help you navigate all of these strategies. They can also help you talk through the negative and sometimes embarrassing effects that UC can have on your life.
Also Check: New Biologic Drugs For Ulcerative Colitis
What Can I Expect If I Have A Diagnosis Of Ulcerative Colitis
Ulcerative colitis is a lifelong condition that can have mild to severe symptoms. For most people, the symptoms come and go. Some people have just one episode and recover. A few others develop a nonstop form that rapidly advances. In up to 30% of people, the disease spreads from the rectum to the colon. When both the rectum and colon are affected, ulcerative symptoms can be worse and happen more often.
You may be able to manage the disease with medications. But surgery to remove your colon and rectum is the only cure. About 30% of people with ulcerative colitis need surgery.
Get Regular Exercise To Reduce Uc Inflammation
Snider says exercise is useful in managing many of the complications associated with ulcerative colitis, including decreased bone density, a weakened immune system, emotional health problems, stress, and weight gain.
Try to engage in a moderate-intensity exercise like swimming or biking, three or four days per week, he says. A review published in August 2016 in Pharmacological Reports noted that moderate exercise releases protective myokines such as irisin from working skeletal muscles, which promotes healing and helps with inflammatory bowel disease inflammation.
Snider also strongly recommends yoga as a natural treatment for ulcerative colitis, as it promotes relaxation and targets the digestive system, flooding the area with oxygen and nutrition for healing. Find what type and frequency of exercise works for you and take it slow: Too much exercise can cause mild systemic inflammation.
Research indicates that stress plays a role in inflammatory bowel diseases such as ulcerative colitis. Researchers analyzed data on 2,007 adults in a Swiss IBD study and found a relationship between depression and anxiety and disease symptoms. The results were published in June 2016 in Clinical Gastroenterology and Hepatology.
Counteract stress with relaxation techniques such as meditation, deep breathing, and progressive muscle relaxation to help your body relax.
You May Like: Can A Heating Pad Help Ulcerative Colitis
Look For Ways To Ward Off A Flare
Your loved ones symptoms may be in remission now, but you can help ward off a future flare by being on the lookout for potential triggers. For example, help them avoid certain foods, such as:
- Nuts and seeds, which can irritate the GI tract
- Carbonated drinks, which can increase gas
- Popcorn, since kernels can be hard on the digestive tract
- Dairy, if theyre lactose intolerant
Encourage your loved one to keep a diary of what they eat and drink, noting the foods that are especially problematic. Dont want to keep a physical record? Theres an app available.
Also Check: What To Do For Ulcerative Colitis Flare Up
What Role Does Diet And Nutrition Play In Ulcerative Colitis
Diet does not cause the development of ulcerative colitis nor can any special diet cure the disease. However, the foods you or your child eat may play a role in managing symptoms and lengthening the time between flareups.
Some foods may make symptoms worse and should be avoided, especially during flareups. Foods that trigger symptoms are different from person to person. To narrow down what foods affect you, keep track of what you eat each day and how you feel afterward .
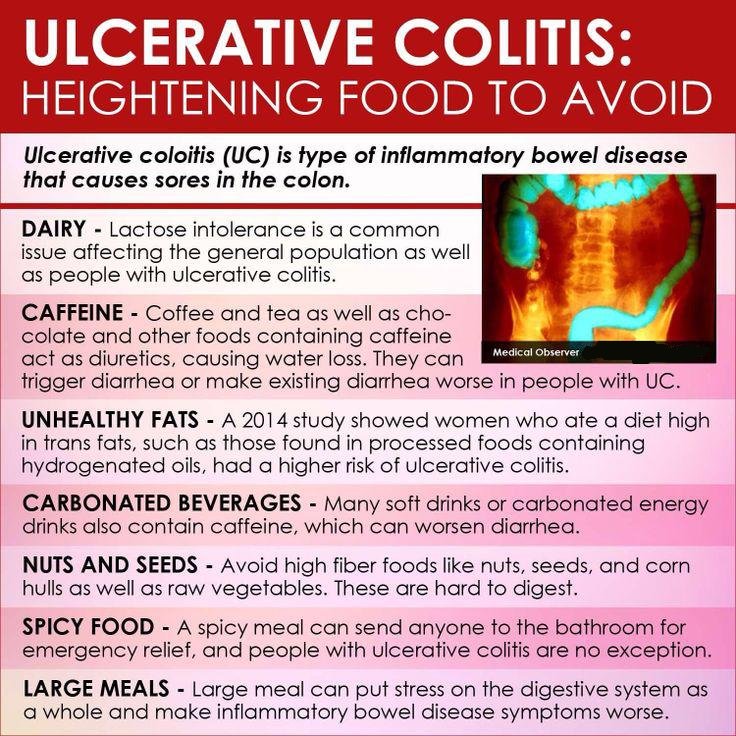
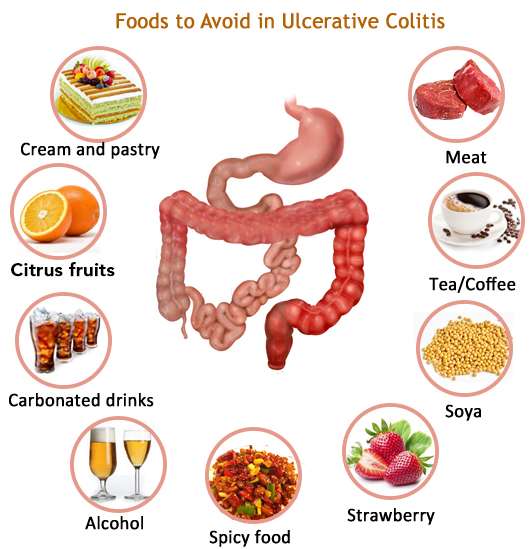
Problem foods often include:
- High sugar foods and drinks.
- Carbonated beverages.
- High-fiber foods.
In addition to the problem foods listed above, infants, children and teenagers can also experience issues with:
- Dairy products.
Keep a careful eye on your childs diet and nutrition. Their appetite may decrease during a flareup and they might not eat enough to stay healthy, and grow. Also, the inflammation caused by ulcerative colitis may keep their digestive tract from absorbing enough nutrients. This can also affect your childs health. For these reasons, you may have to increase the amount of calories your child consumes.
Its best to work with your provider and nutritionist to come up with a personalized diet plan if you or your child has ulcerative colitis.
Also Check: Holistic Treatment For Stomach Ulcer
Engage In Regular Physical Activity
According to the Mayo Clinic, exercise may normalize bowel function. And a 2015 study that looked at the relationship between constipation and lifestyle factors found that people who regularly exercise had a lower risk of constipation.
Increase your level of physical activity to see if constipation improves. Start with low- to moderate-intensity workouts, and then gradually increase intensity as your endurance improves.
Go for a walk or swim, ride your bike, or participate in enjoyable sports. The
Youre Ignoring How Stressed You Really Are
Drs. Bloomfeld and Yun agree: When asked, people with UC often report experiencing stress before a flare. A study published in March 2019 in the Journal of Crohns and Colitis followed 417 people with IBD, which includes UC, and found that experiencing a stressful life event or new stressors in the previous three months was commonly linked to a flare-up.
Stress can trigger inflammation in the gut, worsening the symptoms of UC, according to a study published in 2019 in Frontiers in Pediatrics. Plus, stress can interfere with your usual routine, leading to poor sleep and medication and eating habits.
At Yuns clinic, a psychologist teaches relaxation exercises to people with UC. Learning techniques such as meditation or yoga may help you manage stress.
Recommended Reading: How To Reduce Ulcerative Colitis
Key Points About Ulcerative Colitis
Drugs That Target Inflammation
Most people with UC take prescription drugs called aminosalicylates that tame inflammation in the gut. These include balsalazide , mesalamine , olsalazine , and sulfasalazine . Which one you take, and whether it is taken by mouth or as an enema or suppository, depend on the area of your colon that’s affected. As long as you avoid your triggers, these may be enough if your disease is mild to moderate.
You may need something else if your condition is more severe or if those standard treatments stop working. Your doctor may consider other medicines. Some people may also need surgery.
Also Check: Best Bone Broth For Ulcerative Colitis
Treatment Of Ulcerative Colitis
Vedolizumab is a drug for people who have moderate to severe ulcerative colitis that has not responded to TNF inhibitors or other immunomodulating drugs or who are unable to tolerate these drugs. The most serious side effect it causes is increased susceptibility to infection. Vedolizumab has a theoretical risk of a serious brain infection called progressive multifocal leukoencephalopathy Progressive Multifocal Leukoencephalopathy Progressive multifocal leukoencephalopathy is a rare infection of the brain that is caused by the JC virus. People with a weakened immune system are most likely to get the read more because this infection has been reported with the use of a related drug called natalizumab.
Ustekinumab is another kind of biologic agent given to people who have moderate to severe ulcerative colitis that has not responded to TNF inhibitors or other immunomodulating drugs or who are unable to tolerate these drugs. The first dose is given by vein and then by injections under the skin every 8 weeks. Side effects include injection site reactions , cold-like symptoms, chills, and headache.
Stress Less To Keep Things Moving
Research indicates that stress plays a role in inflammatory bowel diseases such as ulcerative colitis. According to a research review published in October 2019 in Frontiers in Pediatrics, stress leads to inflammation and changes in the gut, which can exacerbate UC symptoms.
Counteract stress with relaxation techniques such as meditation, deep breathing, and progressive muscle relaxation to help your body relax.
These modalities shift the nervous system away from fight or flight and into a rest and digest mode, Snider says. In addition to heart rate, blood pressure, and respiration rate changing, blood and nutrients move into the core to support digestive function.
Don’t Miss: Is Olive Oil Good For Ulcerative Colitis
Oral Vs Rectal Treatments
Most physicians prescribe ulcerative colitis patients oral versions of 5-ASAs or corticosteroids, since this is a patient-preferred delivery method of medication. However, even if they have a specially designed release mechanism, they might not reach and treat the area where the disease is most active.
For example, when you apply sunscreen to your skin, you need to make sure that you cover every exposed part to protect it from the sun. Similarly, when applying these treatments to your rectum and lower colon, you need to make sure that the product covers all of the inflamed areas.
Oral tablets might not be the optimal way to reach the end of the colon, where stool and the fact that ulcerative colitis patients have diarrhea, might interfere with its effectiveness. Unfortunately, this is also the area in the colon where a flare usually starts. The best way to reach this particular area is by inserting the drug directly into the rectum.
Rectal preparations are particularly good at treating urgency and bleeding, symptoms that often are very bothersome. A positive response often occurs within days of treatment.
Ulcerative Colitis Treatment Options
The primary goal in treating ulcerative colitis is to help patients regulate their immune system better. While there is no known cure for ulcerative colitis and flare ups may recur, a combination of treatment options can help you stay in control of your disease and lead a full and rewarding life.
Treatment for ulcerative colitis is multifaceted and includes the use of medication, alterations in diet and nutrition, and sometimes surgical procedures to repair or remove affected portions of your GI tract.
Don’t Miss: What Is The Best Thing To Put On Leg Ulcers
Youre Eating Large Meals
When UC symptoms are active, you can ease your bodys burden by eating frequent, smaller meals so the volume of food and fluid is stable and limited. Consider having five or six fist-sized meals every three to four hours instead of three large meals a day.
On top of helping reduce discomfort from UC symptoms, this strategy is also a way to cope with nausea or loss of appetite that might accompany your flare.
Why Do I Need To Take The Assessment
The reason many supplements fail is a lack of vital information, both on the side of patients and the side of providers. Supplement providers require the history, specifics, and state of your condition in order to recommend the most efficient recovery strategy. This data helps us provide the correct product, dosage & combinations for you.
Also Check: Treating Leg Ulcers With Sugar
How Ulcerative Colitis Is Treated
If you’ve been diagnosed with ulcerative colitis, your treatment plan will take into consideration your specific symptoms and how long you have had the disease. A variety of over-the-counter and prescription medications, from antidiarrheals to antibiotics to anti-inflammatories, may be considered along with lifestyle modifications. Probiotics may also be recommended to help restore healthy gut bacteria. In more severe cases, surgical procedures to remove diseased parts of the colon can provide relief and reduce the risk of developing colon cancer.
What Causes Ulcerative Colitis
Researchers think the cause of ulcerative colitis is complex and involves many factors. They think its probably the result of an overactive immune response. The immune systems job is to protect the body from germs and other dangerous substances. But, sometimes your immune system mistakenly attacks your body, which causes inflammation and tissue damage.
Don’t Miss: How To Treat An Eye Ulcer
How To Treat An Ulcerative Colitis Flare
The great thing about the internet is that you have constant access to information on any topic you want to learn about. The bad thing about the internet is that it can be difficult to determine a credible source from a phony one. When it comes to finding information on how to best manage GI conditions like Ulcerative Colitis , online information can often be contradicting and confusing. Thankfully, were up to date on the current research and recommendations to help you best manage your Ulcerative Colitis symptoms.
The tough part about ulcerative colitis management is that our recommendations are specifically tailored to your stage of ulcerative colitis- active or dormant .