Getting A Specialist Vascular Referral
If you have venous hypertension, intervention to your veins from a vascular specialist might help with healing and stop your wound or sore from coming back. Sometimes varicose veins can be treated by laser therapy. If you have peripheral arterial disease, you may require further investigations and the vascular team will be able to assess the need to improve the blood supply to your leg or whether your ulcer can be managed in other ways such as reduced/modified compression. Ask your nurse or doctor for a referral to your local vascular team to talk about how their input might help you.
Bread And Baking Soda
I have a new leg uler which developed after a bleed. It is on my interior ankle. Extremely painful. Can feel the swelling where the damage was done. I was told of a method using bread, bicarbonate of soda on the bread and water which makes the paste bubble. Does anyone know of this method. Surelly there is some native bush remedy out there. Indigenous people have cures for all their needs which they have used for years. Modern wound clinics just put on a bandage and say see you nexst week. One year later you are still doing the same thing.
Some years ago I was given a radical idea to try. At the time I didn’t take any notes etc but it worked! I had 5 cellulitis ulcers on one leg and I was told to drink 1/4 cup of Colloidal Silver every 5 hours and spray my leg frequently with same. To do it over a 24 hour period. I did it and within 10 days I had only had the original ulcer left. Which hasn’t been oozy for years.
So in that time frame, I lost 4 ulcers that have never returned. In 2017, one of my 2 specialists told me to use potassium permanganate to wash my legs daily and use the amount of crystals that would barely fit on the edge of a matchstick… He told me it kills sepsis and pseudomonas. Other Dr was delighted and told me that before the arrival of penicillin, doctors used Condy’s Crystals as a wash for ulcers.
HoneyHoney
What Type Of Healthcare Provider Helps With Ulcers How Do They Diagnose An Ulcer
Your healthcare provider can tell what type of ulcer you have based on four observations:
- Appearance of the ulcer.
- Appearance of the borders.
- Appearance of the surrounding skin.
Your primary healthcare provider can diagnose an ulcer, but they may send you to a specialist for treatment. You may see a podiatrist, a provider who works with feet, or a wound specialist. To find out how deep the ulcer goes, and to see if it caused an infection in a nearby bone, they may order an X-ray, MRI or CT scan.
For more complicated cases that require surgery, you may also see a plastic surgeon, anesthesiologist, orthopedic surgeon and/or vascular surgeon.
Recommended Reading: Best Ulcerative Colitis Diet Book
Can Emuaid Help Relieve Diabetic Ulcers Naturally
Yes! Before we show you how EMUAID® works, there’s something you must know.
Your skin is a barrier designed to keep bacteria and infections out. Most medications cannot penetrate deep into the skin to efficiently deliver the active ingredients to where they are needed the most.
No matter how effective the medication is, there’s no use if it can’t penetrate the skins barrier to treat your your diabetic ulcers.
EMUAID® is different.
EMUAID® is specially designed to penetrate skin. It has a unique delivery system that helps carry powerful healing ingredients deep into your skin.
When To Call A Healthcare Provider
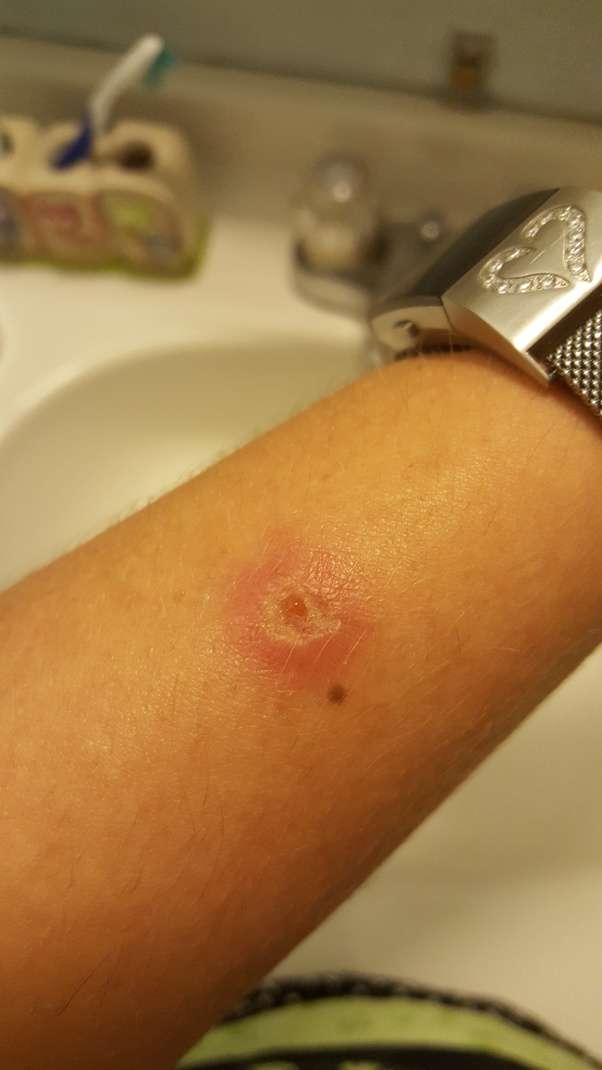
If the ulcer is large or deep, growing in size, incredibly painful, or if you have any signs of infection , you notice a bad smell coming from your ulcer, or you’re running a fever, call your healthcare provider right away.
You’ll also want to call your healthcare provider if your ulcer, no matter how minor, isn’t showing signs healing after a week to 10 days.
In most cases, the ulcer will be dressed to protect the wound. However, if your ulcer is draining considerably, your healthcare provider may recommend leaving the wound uncovered. Dressing the ulcer if it’s draining considerably can impede healing.
If your ulcer is painful, pain medication can be prescribed. Antibiotics may also be prescribed either prophylactically to prevent infection or to treat an already infected wound.
Debridement is done to remove dead tissue from more serious ulcers. For deep ulcers or those that aren’t healing after a long period of time, skin grafts may be needed. In the most severe cases, part of the foot, leg, or other appendage may have to be amputated.
Restoring good circulation is key in treating and preventing ulcers. This includes elevating the legs, wearing compression stockings, reducing pressure on ulcer-prone areas, superficial vein surgery. Leg ulcers, in particular, are incredibly likely to reoccur, so compression stockings are often needed to be worn for life.
Also Check: How To Treat An Eye Ulcer
Should Leg Ulcers Be Kept Dry
Low oxygen tension leads to high levels of oxygen at the capillaries and low levels of oxygen at the wound edges. This provides the ideal environment for wound healing because granulation and wound healing is stimulated. a wound, nurses should remember: If theres no blood supply keep it dry and seek expert advice.
Swelling In The Legs And Ankles
Venous leg ulcers are often accompanied by swelling of your feet and ankles , which is caused by fluid. This can be controlled by compression bandages.
Keeping your leg elevated whenever possible, ideally with your toes above your hips, will also help ease swelling.
You should put a suitcase, sofa cushion or foam wedge under the bottom of your mattress to help keep your legs raised while you sleep.
You should also keep as active as possible and aim to continue with your normal activities.
Regular exercise, such as a daily walk, will help reduce leg swelling.
But you should avoid sitting or standing still with your feet down. You should elevate your feet at least every hour.
You May Like: Wound Vac For Pressure Ulcers
Why It Is Important To Do This Review
Venous leg ulcers are a relatively common type of complex wound that have a negative impact on peoples lives and incur high costs for health services and society. Leg ulcers are painful, sometimes malodorous, prone to infection, and may severely affect people’s mobility and quality of life, and in severe cases, there is a risk of limb amputation. There are a number of treatments for venous leg ulcers, but many ulcers prove hard to heal, although healing is a key outcome for patients.
We conducted an open consultation with consumers to ask them which treatments for treating venous leg ulcers they would like to see considered. Respondents selfselected through their response to a short questionnaire posted on the Cochrane Wounds website and Facebook page. Although some identified compression as the main consideration, others mentioned specific types of dressings. These included many of the dressing types listed in , including charcoalcontaining dressings, dressings designed to reduce formation and presence of biofilms and dressings with antimicrobial properties and debriding actions. Also specifically identified as being of interest was Unna’s boot a specialised dressing which consists of gauze wraps impregnated with zinc oxide and calamine, sometimes in combination with other agents.
A glossary of NMA terms is given in .
What To Look Our For When Applying Compression Bandaging Wrap Systems Or Hosiery
If youre using a wrap system, wear supportive stockings or tights or use compression bandaging (compression bandaging is normally only applied by your nurse or healthcare professional, here are some things to look out for:
- Does your footwear still fit the same if your footwear is tight it may mean that the swelling has increased?
- Does the bandaging, wrap or hosiery feel firm and supportive?
- Is your skin red and inflamed?
- Is your skin dry and flaky?
- Is your skin white and soggy like youve just come out of the bath?
- Do you have eczema or another skin condition that requires specific creams or ointments?
If you have concerns with any of the above, please get in touch with your healthcare professional for advice.
You May Like: Does Ulcer Pain Come And Go
Cleaning And Dressing The Ulcer
The first step is to remove any debris or dead tissue from the ulcer and apply an appropriate dressing. This provides the best conditions for the ulcer to heal.
A simple non-sticky dressing will be used to dress your ulcer. This usually needs to be changed once a week.
Many people find they can manage cleaning and dressing their own ulcer under the supervision of a nurse.
Who Gets Foot And Toe Ulcers
You’re at higher risk for foot and toe ulcers if you are:
- Native American.
- Male.
- Elderly.
If you have an eye, kidney or heart disease related to diabetes, youre also at a higher risk. About 15% of people with diabetes will get an ulcer, typically on the bottom of their foot. Around 6% of that 15% will have to be hospitalized because of complications.
Youre also at a higher risk of getting foot and toe ulcers if you have any of the following:
- Problems with circulation.
- A foot deformity like a bunion or hammertoe.
- Kidney disease.
- Use alcohol.
Don’t Miss: Signs Of Ulcers In Humans
What Treatment Might I Be Offered
Compression therapy if your wound isnt healing because of venous hypertension and there are no problems with the arterial blood supply to your legs, then you should be offered compression therapy. Compression therapy usually works very effectively and helps wounds to heal fast. It is thus essential to find a compression regime that is comfortable, provides the level of support you need and works. If this is inconsistently used or applied, this must be dealt with so that healing is not delayed
Compression therapy improves blood supply by applying pressure to the leg. This can be done by bandaging the lower leg or by wearing supportive socks, stockings or tights. To begin with it can be a little uncomfortable when you first start treatment but should not cause you any pain it should feel supportive to your leg. Any discomfort should reduce as the swelling goes down. If you do experience discomfort, talk to your nurse or doctor about it and they will advise you on ways of alleviating this.
Data Collection And Analysis
Two review authors independently performed study selection, ‘Risk of bias’ assessment and data extraction. We conducted this NMA using frequentist metaregression methods for the efficacy outcome the probability of complete healing. We assumed that treatment effects were similar within dressings classes . We present estimates of effect with their 95% confidence intervals for individual treatments focusing on comparisons with widely used dressing classes, and we report ranking probabilities for each intervention . We assessed the certainty of the body of evidence using GRADE for each network comparison and for the network as whole.
Don’t Miss: How Do You Treat Mouth Ulcers
Venous Leg Ulcers: 6 Things To Know When Treating Venous Disease
Lower extremity venous disease affects millions of Americans and may ultimately lead to open, draining wounds that adversely affect quality of life. However, there are exciting developments in early diagnosis, prevention and treatment of venous leg ulcers . On the treatment side, there are more choices now than ever before in compression products, which is greatly improving the patient experience. But proper treatment also comes from a better understanding of venous leg ulcers, and better understanding comes from more education. Luckily, were here to help provide education and support for you and your team, so here are six things to know when treating VLUs.
Diabetes And Leg Wounds
Although diabetic leg ulcers and peripheral vascular disease wounds are different, they may share some of the same causes and risk factors. According to Science Directs study, It is reported that diabetes is associated with a two to four-fold increase in the incidence of peripheral arterial disease compared to non-diabetic subjects.
Diabetes and PAD go hand-in-hand because the lining in your blood vessels becomes less flexible allowing plaque to build up even easier. When blood isnt able to move freely, blockages tend to occur. Not only does diabetes irritate and inflame the lining of your blood vessels, but it can also compromise your ability to fight infections which could cause open wounds to not heal properly.
Lastly, high blood pressure, increased cholesterol levels, family history of vascular disease, and diabetes are all linked as causal factors for peripheral vascular disease wounds. That said, if youre at an increased risk, you should be monitoring any slow-healing wounds or diabetic leg ulcers so you can notify your doctor.
You May Like: Icd 10 Stage 4 Sacral Ulcer
Leg Ulcers: How To Relieve The Pain At Home
Patients most often present with either of the two main types of leg ulcers: venous or arterial. Less frequently, people suffering from diabetes can develop neuropathic ulcers as a result of unstable blood sugar.
Most often associated with varicose veins, venous ulcers make up the lionâs share of leg ulcers with 85% of diagnoses. These ulcers take a long time to heal, and it is a painful process. Worse still, 75% of these painful ulcers will reoccur. Home treatment and surgical intervention can help ease the pain associated with these types of wounds.
A Note From Cleveland Clinic
Foot and toe ulcers take longer to heal the longer theyre ignored. If you dont get treatment for your ulcer, it may get bigger and deeper, get infected or cause you to be unable to use your feet correctly. Remember that ulcers can return after treatment. In fact, you have a 50% chance of getting another one within three years of the first. See a podiatrist for your ulcer as soon as possible.
Don’t Miss: How Do Doctors Test For Ulcerative Colitis
Can Venous Leg Ulcers Be Prevented
There are several ways to help prevent a venous leg ulcer in people at risk, such as:
- wearing compression stockings
- losing weight if you’re overweight
- exercising regularly
- elevating your leg when possible
This is particularly important if you’ve previously had a leg ulcer once a leg has suffered a venous ulcer, you’re at risk of further ulcers developing within months or years.
Read more about preventing venous leg ulcers.
Criteria For Considering Studies For This Review
Types of studies
We included published and unpublished randomised controlled trials , irrespective of language of report. We only included crossover trials that reported outcome data at the end of the first treatment period and prior to crossover. We excluded studies using quasirandom methods of allocation . We highlighted trials in which three or more interventions were randomised and included all relevant arms.
Types of participants
We included trials recruiting adults described as having venous leg ulcers, managed in any setting. We accepted study authors’ definitions of venous leg ulcers. Where wounds were described only as “leg ulcers” without information as to aetiology, we assumed that they were venous in origin. Trials in which a minority of leg ulcers are described as having a mixed or arterial pathology were included provided that these were fewer than 25% of participants. Trials including other types of mixed wound populations were not included. We included participants at any stage of their treatment process for example, participants with or without ulcers described as being hard to heal or clinically infected.
Types of interventions
* ‘combination dressings’ means two or more dressings applied sequentially over time , or a product containing two or more types of dressing material .
Some of the interventions we considered are as follows we used the categories listed below as the basis for grouping the treatments used in individual studies:
Data synthesis
Read Also: What Foods Should I Avoid With A Stomach Ulcer
Caring For Venous Ulcers
Venous ulcers need proper care and treatment to prevent infection and to heal. It’s important to have any venous ulcers checked right away by your healthcare provider.
Treatment may require focusing on the circulatory or vein problems that are causing the ulcers. Or it may mean removing some tissue around the wound. You may be asked to:
-
Clean the wound regularly
-
Apply a dressing to the ulcer
-
Avoid products that cause skin sensitivity
-
Wear compression stockings to prevent blood from pooling in the legs and to speed healing
-
Apply an antibacterial ointment or another topical medicine to prevent or treat an infection
-
Take oral antibiotic medicines to prevent or treat an infection
-
Have allergy testing done
Wearing a compression wrap to keep blood flowing back up to your heart can also help ulcers heal more quickly. In some cases, surgery or a skin graft is needed to close up the opening in the skin.
Dressings And Topical Agents
Dressings are usually applied to open ulcers. As well as offering protection, dressings may be chosen for other reasons, such as antimicrobial properties or absorption of exudate. As well as a wide range of types of dressings available, there are a number of topical products, used to reduce infection risk, aid exudate absorption or promote wound healing by other means, as well as topical painkilling agents. Having reliable evidence to guide choices is important, and not only for healthcare professionals. Patients responding to Cochrane Wounds online open consultation on research priorities, conducted between May and November 2016, asked in particular for evidence relating to specific dressings.
There are high quality, recent evidence syntheses, including a number of Cochrane Reviews, on particular dressing types and topical agents, but the evidence is low quality and does not provide robust support for any specific dressing or treatment. What is needed is a network meta-analysis , a simultaneous comparison of linked, multiple, competing treatments in a single statistical regression model. This is being done in a new Cochrane Review for the outcome of venous leg ulcer healing, for alternative dressings and topical agents .
Also Check: Is Milk Good For Ulcers