Umbilical Cord Grafts Shown To Heal Foot Ulcers
25 September 2018. Results from a clinical trial show skin grafts made from dehydrated human umbilical cord tissue heal more diabetic foot ulcers than alginate dressings, a common treatment for the condition. Findings from the trial sponsored by MiMedx Group Inc. developer of EpiCord, the treatment tested in the study appear in yesterdays issue of International Wound Journal.
People with diabetes often develop slow-healing skin ulcers on their feet, a common complication of the disease. In people with diabetes, blood flow is reduced to the legs and feet, leading to nerve damage and reduced feeling in those regions, as well as slower healing of wounds. Centers for Disease Control and Prevention says in 2010, some 73,000 Americans required amputation of a leg or foot because of complications from diabetes. While malnutrition and immune deficiencies can also cause chronic wounds, CDC says people with diabetes are 8 times more likely to lose a leg or foot than people without diabetes.
EpiCord uses tissue from human umbilical cords for wound healing. The umbilical cord provides blood and nutrients from the mother to the fetus and is usually discarded after birth. But the cord is made from layers of amniotic membrane and a substance called Whartons Jelly that is also a source of stem cells and growth factors, thus increasingly studied as a source of regenerative medical solutions.
More from Science & Enterprise:
Outcomes In Rheumatoid Ulcers
CLUs are frequent in patients suffering from rheumatoid arthritis , with an approximate prevalence of 9% , . The aetiology of chronic ulcerations in such patients is multifactorial but is often associated with venous insufficiency, systemic rheumatoid vasculitis or both. Rheumatoid ulcerations particularly caused by systemic vasculitis are noted to be more painful and more resistant to treatment if compared to the other types of ulcers.
Ãien et al. described the effect of pinch grafting on pain and healing of RUs caused by both venous insufficiency and systemic vasculitis as an alternative to conservative treatment. They found a remarkable reduction in pain and an increased healing rate of RUs after pinch grafting. However, grafting success and then ulcer healing mostly depends on two primary predictive factors, ulcer size and ulcer duration. So, the best outcomes have been observed in smaller and recent ulcerations.
Although pinch grafting is found to be an excellent tool to treat RUs, in the last few years, many studies established the effectiveness of pharmacological therapies in the treatment of such ulcers. With respect of this, Hellmann et al. reported the successful treatment of rheumatoid vasculitis-associated cutaneous ulcers using rituximab in two patients with RA. Even in the case of RUs, the literature is poor in results concerning the healing rate of such ulcers.
Research Design And Methods
We searched the Cochrane Controlled Trials Register , MEDLINE , EMBASE , and CINAHL using a combination of text and keywords in addition to a filter for controlled clinical trials. The last update of searches was performed on 30 September 2007. We included trials if the allocation of participants was described as randomized, with participants of any age and in any care setting having diabetic leg or foot ulceration. We included studies that compared the following types of grafts with any other intervention: 1) autografts , 2) allografts , 3) xerografts, and 4) bioengineered skin.
Two reviewers independently evaluated reports for eligibility and assessed methodological details and results of the studies. Disagreements were resolved by discussion.
The prespecified primary end point was complete healing rate at the end of the trial. Results are presented as odds ratios . We used standard fixed-effects meta-analysis and Cochran’s Q test for heterogeneity . Analyses were performed using Stata .
Don’t Miss: What Does Asacol Do For Ulcerative Colitis
How Is A Skin Graft Procedure Done
Your plastic surgeon will choose the type of skin graft and the donor site . Donor sites are usually places that are easily concealed, like the thigh or scalp. Surgeons may also take skin from the buttocks, back, and arm.
The wound site is thoroughly prepared. This includes removing any damaged skin in the area a process called debridement and ensuring that the area is sufficiently free of bacteria. If necessary, the area will be treated with antibiotics. This process is particularly important as improper wound preparation can lead to hematoma and wound infection, two common causes of skin graft failure. Finally, the area is cleaned using saline, and any bleeding is stopped.
Healthy skin is typically harvested using a dermatome, a handheld device that strips away an even layer of skin for later application. Smaller areas that need a more refined touch may be harvested by hand or by a drum dermatome.
After the skin is removed, the donor site is dressed and treated according to whether it was a split or full thickness graft. Full thickness graft donor sites will be sutured closed. Split-thickness skin graft donor sites will be dressed and left to heal via reepithelialization .
What Does Current Guidance Say On This Issue
NICEs 2015 guidance on Diabetic foot problems: prevention and management recommends that usual care includes one or more of the following treatments: offloading , control of foot infection, control of ischaemia and wound dressings.
It also recommends considering skin grafts or skin substitutes in addition to usual care for diabetic foot ulcers only when healing has not progressed and on the advice of the multidisciplinary foot care service.
Recommended Reading: How Long Does Prednisolone Take To Work For Ulcerative Colitis
Skin Grafting In Diabetic Foot Ulcers
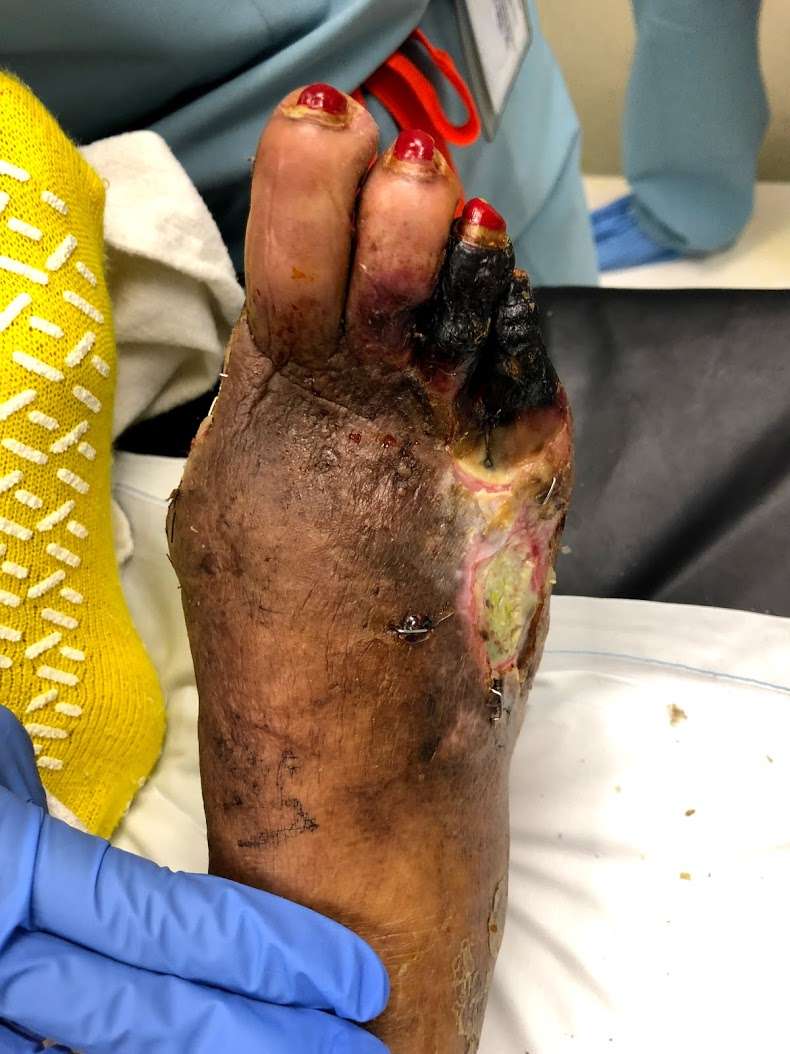
Skin grafting is advocated by many centers in Diabetic Foot Ulcers. However in my experience of more than 20 Years split skin grafting leads to contractures and recurrent ulceration in diabetic foot wounds, especially on the plantar surface. Because of this I do not advocate skin grafting in diabetic ulcers. However recently available skin substitutes may have a role to play in faster skin cover of such ulcers as well as having reduced incidence of contractures.
Large diabetic foot wound on both dorsum and plantar surfaces
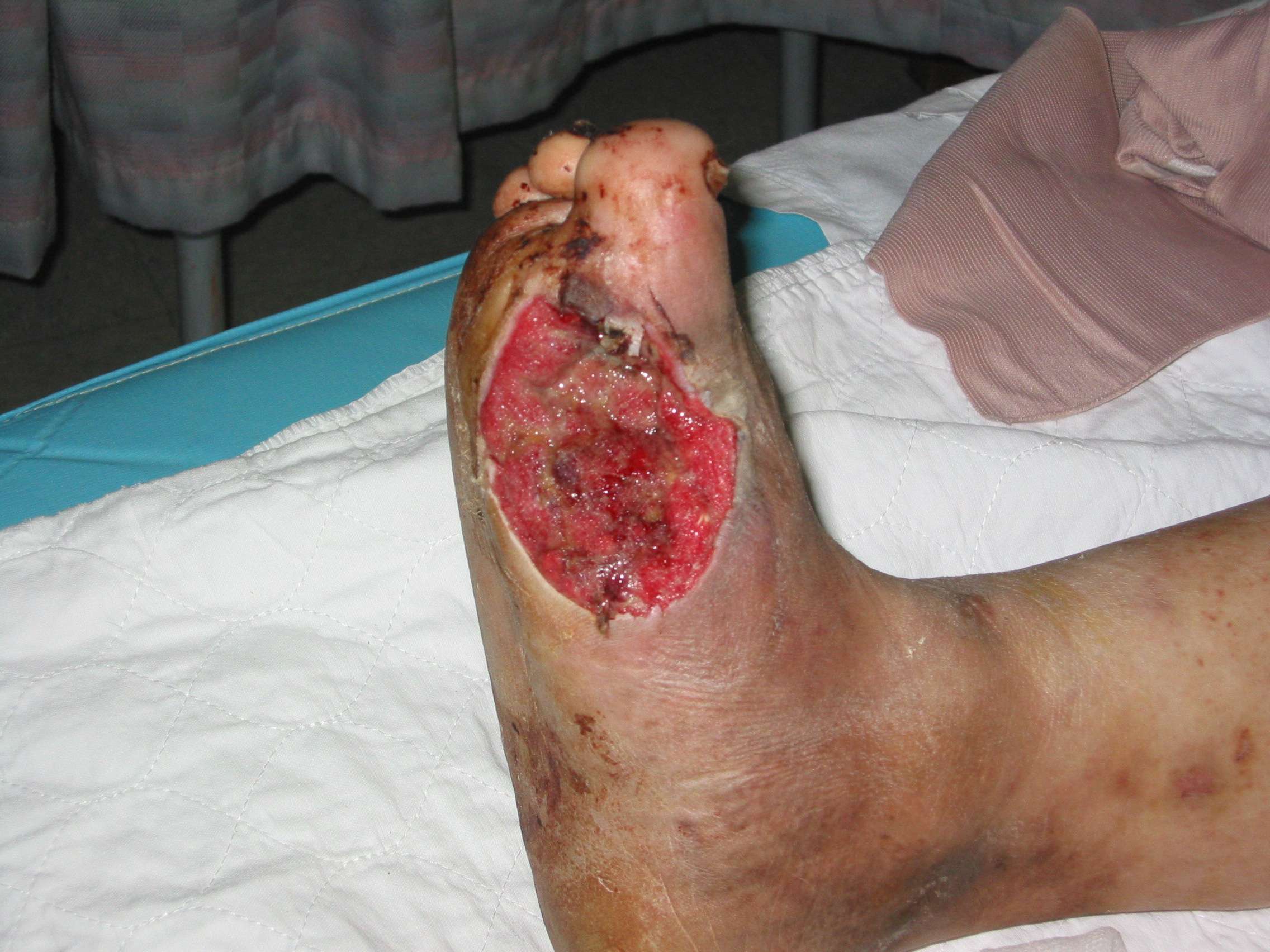
Complete closure of the wound without skin grafting
What To Expect From A Skin Graft Procedure
A skin graft procedure is sometimes needed in order to remove and transplant healthy skin from one part of your body to another in order to replace damaged skin due to a wound or another problem. The areas from which grafts are taken include the buttocks, thigh and upper arm. Here is some information on why this procedure is needed and what to expect during the surgery and afterward.
Read Also: Aloe Vera Gel For Horses Ulcers
What Did It Find
- Fourteen trials found that skin grafts and tissue replacement products use in the trials increased the healing rate for people with diabetes by approximately 55% compared to usual care . Complete ulcer healing at 6 to 16 weeks was 423 per 1,000 people using skin grafts or tissue replacement, significantly more than the 273 per 1,000 achieved in standard care. Despite this improvement, fewer than half of all ulcers were healed by 16 weeks.
- Four trials directly comparing skin graft or tissue replacement products with one another found no specific type was more effective than another.
- Two trials looking at the rate of lower limb amputations found around half the rate of amputations in the skin graft or tissue replacement groups compared with usual care . There was imprecision in reporting of amputations rates.
- No trials reported significant differences in adverse events between skin graft or tissue replacement products compared to usual care, based on 16 trials.
- No trials reported on quality of life or compared the cost benefits of skin grafts or tissue replacement compared with usual care.
Management Of Systemic And Local Factors
Treatment of diabetic foot ulcers requires management of a number of systemic and local factors.
Precise diabetic control is, of course, vital, not only in achieving resolution of the current wound, but also in minimizing the risk of recurrence. Management of contributing systemic factors, such as hypertension, hyperlipidemia, atherosclerotic heart disease, obesity, or renal insufficiency, is crucial. Management of arterial insufficiency, treatment of infection with appropriate antibiotics, offloading the area of the ulcer, and wound care are also essential.
References
Amin N, Doupis J. Diabetic foot disease: From the evaluation of the “foot at risk” to the novel diabetic ulcer treatment modalities. World J Diabetes. 2016 Apr 10. 7 :153-64. . .
Naves CC. The Diabetic Foot: A Historical Overview and Gaps in Current Treatment. Adv Wound Care . 2016 May 1. 5 :191-197. . .
Rice JB, Desai U, Cummings AK, Birnbaum HG, Skornicki M, Parsons NB. Burden of diabetic foot ulcers for Medicare and private insurers. Diabetes Care. 2014. 37 :651-8. .
Gentile AT, Berman SS, Reinke KR, Demas CP, Ihnat DH, Hughes JD, et al. A regional pedal ischemia scoring system for decision analysis in patients with heel ulceration. Am J Surg. 1998 Aug. 176:109-14. .
Mills JL Sr, Conte MS, Armstrong DG, et al. The Society for Vascular Surgery Lower Extremity Threatened Limb Classification System: risk stratification based on wound, ischemia, and foot infection . J Vasc Surg. 2014 Jan. 59 :220-34.e1-2. . .
Recommended Reading: What Causes Ulcers To Flare Up
Basic Consideration And Indication For Grafting
Wounds with skin loss close through two main mechanisms: epithelial migration and wound contraction. Both processes occur from the edges of the wound and aim to fill the lesion and to shrink the wound edges. When these natural mechanisms are insufficient, skin grafts or flaps can be considered a suitable solution, especially after 6 weeks of non-healing wounds despite appropriate treatment , . Skin grafts are commonly and frequently used in a variety of clinical situations, such as traumatic wounds, CLUs , burn reconstruction, scar contracture release, defects after oncological resection, congenital skin deficiencies, hair restoration, vitiligo and nipple-areola reconstruction , . Obviously, different types of wounds require different treatments and different typologies of grafts that must be selected individually for each defect in order to restore the functional integrity of the skin with the best possible cosmetic outcome .
Outcomes In Diabetic Ulcers
Diabetic ulcers represent a common complication of diabetes and are responsible for more hospitalisations than any other complication of diabetes in fact, about 15% of diabetic patients develop DUs, and from 12 to 24% of individuals diagnosed with such ulcers will require amputation .
The use of skin grafting for chronic lower-limb ulcerations has been controversial for a long time and has been considered not suitable for such ulcers because of the concrete risk of failure, especially in patients with plantar diabetic foot wounds. However, a study by Rose et al. has shown that the application of STSGs to chronic lower-limb ulcerations is an effective method for the promotion of wound healing regardless of wound location and presence of diabetes .
Recommended Reading: Removing Colon Due To Ulcerative Colitis
Split Thickness Skin Grafts
Split thickness skin grafting is a technique that has been around for a long time because it works! With a skin graft, the surgeon will take a partial thickness piece of skin and transplant it to the wound bed. This procedure is done in the operating room. There will be a new wound on the thigh that will need to heal. If successful, the skin graft will take and can lead to wound healing in as little as two weeks.
Understanding Stem Cell Therapy
Stem cell therapy is a type of treatment that uses your bodys own natural healing abilities as part of the recovery process. Using stem cells speeds up your healing process and can be used to treat a variety of foot conditions, including diabetic foot ulcers.
Your stem cell treatment is noninvasive and takes place right in the Podiatry Hotline Foot & Ankle office. To complete the procedure, our podiatrists use highly effective and ethically sound placental tissues.
After getting stem cell therapy, your body not only heals your area of concern more quickly, it also decreases inflammation and reduces your pain. Youll also regrow fresh, new tissues in the area, often resolving the problem permanently.
Recommended Reading: How Is Ulcerative Colitis Caused
Recipient Site Care And Frequent Complications
Postoperative immobilisation is essential during a period of 5â10 days in the position of maximal graft stretching. This will help to improve graft take and minimise graft shrinkage. After 7 or 10 days of immobilisation, physiotherapy can be started, with care taken to avoid shear forces. It is also important to prevent the drying of the skin graft by applying fat cream and lotion for 6â12 weeks. Scar treatment with massage or silicon sheets might be necessary in order to prevent the formation of hypertrophic scar , .
Poor or inadequate management of the recipient site can lead to a number of complications that can be divided into early complications and late complications.
Early complications are responsible for failure of graft take. Haematoma, seroma and infections are the most frequent early complications leading to graft failure. Infections can be prevented by the use of preoperative and perioperative antibiotics and leg elevation , .
Skin Grafting In Venous Ulcers
I personally do not believe in skin grafting in venous ulcers and have never carried it out. After treating the root cause, i.e. the increased venous pressure which leads to the ulcer, I find that the ulcers have healed.
Also many series report a failure of the skin graft if the primary cause which is the venous pressure , is not treated. Most patients who come to us have undergone skin grafting and then after failure of graft they come to us.
So grafting of a leg ulcer without vascular assessment as to cause of
ulcer, should be avoided.
The wound above healed without grafting as did the venous wound below
This was a long standing ulcer, extending around the leg.
Six months after surgery and treatment of the underlying venous hypertension, the ulcer completely closed, without skin grafting.
As you can see from these cases, venous ulcers of any size, can heal without skin grafting. This is not to say that skin grafting is not to be done but mainly till you treat the underlying cause the ulcer is not going to heal. In case of very large ulcers, grafting may be carried out for faster cover of the ulcer, however in my personal opinion and experience, it is better not to graft a venous ulcer.
Read Also: Natural Way To Cure Ulcer
Why Was This Study Needed
Foot complications are common in people with diabetes with around 10 to15% experiencing a diabetic foot ulcer at some point in their lives. NICE also estimate that around 50% of people die within five years of developing a diabetic foot ulcer and ulcers precede more than 80% of diabetes-related amputations.
They are also costly. A 2012 NHS Diabetes report estimated that around £650 million is spent on foot ulcers or amputations each year.
Despite the variety of current treatments for diabetic foot ulcers – including control of foot infection and wound dressings – up to 60% of ulcers fail to heal completely.
This review looked to see whether treatments involving skin grafts and tissue replacement would improve ulcer healing rates compared to usual care.
Outcomes In Chronic Venous Leg Ulcers
CVLUs amount to 70% of all CLUs and consist of excavation located in lower leg skin because of the loss of inflammatory necrotic tissue as a result of insufficient venous blood circulation because of structural abnormalities of the vein draining the legs. These abnormalities can be detected in the superficial veins, the communicating veins or the deep veins and mostly consist of faulty valves unable to ensure forward progression of blood. This alteration leads to an increased venous pressure with progressive dilation of the veins and egress of proteins, such as fibrinogen. The resulting fibrin complexes compromise the microcirculation and cause the phlogosis onset. Finally, cell death and necrotic tissue evolve into venous ulcerations. CVLUs consist of irregular, shallow and painful lesions usually located over bony prominences such as medial malleolus, with granulation tissue and fibrin present in the ulcer base. Other important findings may be oedema, varicosities, hyperpigmentation and lipodermatosclerosis with thickening and fibrosis of the adipose layer under the skin .
Furthermore, Salomè et al. showed how split-thickness skin grafting resulted in better health-related quality of life and self-esteem in patients with venous leg ulcers than did different treatments.
Also Check: What Is Best Medicine For Ulcer
What Did This Study Do
This Cochrane systematic review included 17 randomised controlled trials involving 1,655 adults with type 1 or 2 diabetes. Fourteen trials compared skin grafts / tissue replacement with usual care, four compared tissue products against each other.
Skin grafts came from the person themselves, a different person engineered or artificial skin or from animals. Follow-up to assess ulcer healing ranged from six weeks to 14 months, but most were 12 weeks. In the 15 trials that described patients characteristics in detail, all studied people who had sufficient blood flow to their feet.
We can be confident the review identified the most relevant trials, but they were rated in the review as low-quality due to a lack of blinding of the outcomes assessors. Blinding is not feasible for these studies as the treatments are visible. There were links with manufacturers of skin products in 15 of the trials. No studies came from England and most were from the US, so applicability to the UK may be an issue.
Excision And Split Skin Grafting
Skin grafts may be used as a primary procedure at the time of excision, or they may be placed on an excision site that is granulating satisfactorily. Primary grafting in an attempt to ablate recurrent disease may be appropriate for large defects. Results of secondary grafting are rather disappointing, as split skin may not take on rapidly contracting granulation tissue. In many cases, the defect will probably heal more quickly at this stage without grafting.
Primary skin grafting has been used by a few enthusiasts, usually for recurrent disease, with good results . Guyuron et al reported a median hospital stay of 10 days, a period off work of only 5 weeks, and only five recurrences in 58 patients .
Read Also: Ulcerative Colitis Caused By Alcohol