Getting To A Diagnosis
Theres no doubt that IBD can significantly decrease quality of life, between uncomfortable symptoms and frequent bathroom visits. IBD can even lead to scar tissue and increase the risk of colon cancer.
If you experience any unusual symptoms, its important to call your doctor. You may be referred to a gastroenterologist for IBD testing, such as a colonoscopy, sigmoidoscopy, or a CT scan. Your doctor may also order blood and fecal testing. Diagnosing the specific form of IBD will lead to more effective therapies.
Commitment to daily treatment and lifestyle changes can help minimize symptoms, achieve remission, and avoid complications.
Regardless of your diagnosis, Healthlines free app, IBD Healthline, can connect you with people who understand. Meet others living with Crohns and ulcerative colitis through one-on-one messaging and live group discussions. Plus, youll have expert-approved information on managing IBD at your fingertips. Download the app for iPhone or Android.
Last medically reviewed on November 12, 2021
How To Begin Including Smoothies In Your Diet
Start simple. You might be excited to eat these nutritious foods, but be careful to add only one new ingredient at a time. For example, if you tolerate bananas and almond milk then make a banana almond milk smoothie. From there, add blueberries. Did that work well? Great! Now add a handful of spinach. You get the gist.
While its tempting to become a creature of habit and eat your same favorite smoothie every day, I encourage you to mix things up. A key part of healthy eating is variety so youll want to incorporate all the colors of the rainbow. Plus, eating the same food every day when the gut is unwell can increase your risk of becoming sensitive to it.
Also Check: Ulcerative Colitis Caused By Alcohol
May Have Similar Symptoms
Because all three of these inflammatory bowel diseases involve inflammation of your digestive tract, Crohns disease symptoms, ulcerative colitis symptoms, and celiac disease symptoms have a significant amount of overlap and include:2,3
- Diarrhea and/or constipation
- Canker sores in the mouth
While these inflammatory bowel conditions may be hard to differentiate at first glance, there are actually some important and distinct differences between them.
Recommended Reading: Boost Vs Ensure Ulcerative Colitis
One Syllable Describing Words
To diagnose ulcerative colitis, doctors review medical and family history, perform a physical exam, and order medical tests. Doctors order tests to. confirm the diagnosis of ulcerative colitis. find out how severe ulcerative colitis is and how much of the large intestine is affected. rule out other health problemssuch as infections.
The ongoing coronavirus disease 2019 pandemic, caused by severe acute respiratory syndrome coronavirus 2, represents a potentially major challenge to patients with immune-mediated inflammatory diseases who are treated with immunomodulatory therapies. We report the case of an 18-year-old ulcerative colitis patient in sustained clinical remission who 4 days.
Ulcerative colitis is an inflammatory bowel disease that causes long-lasting inflammation and ulcers in your digestive tract. Ulcerative colitis affects the innermost.
COVID-19 Resource Center. Review the latest information on visitor policies, safety procedures, Ulcerative colitis is an autoimmune disease and inflammatory bowel disorder that affects the large intestine and rectum. Although it can begin at any age, it often starts in young adulthood. Monitoring diet to limit foods that cause.
Treatment Options For Ulcerative Colitis
Ulcerative colitis involves more than just medications and symptoms. It is a life changing condition that you are learning to manage, and it represents only part of your story. As you continue your journey with ulcerative colitis while in college, there may be many questions that you will have to navigate in order to help make your experience rewarding. This Campus Connection website will cover some helpful tips and information that you should know before, and during college, and offers a way for you to potentially connect with others like you.
Read our Living with Ulcerative Colitis brochure to learn more about the disease, treatment and daily living.
- Campus Connection
Recommended Reading: Simponi Dose For Ulcerative Colitis
Differences Between Ulcerative Colitis And Crohns Disease
The differences between ulcerative colitis and Crohnâs disease are:
- In Crohnâs disease, there are healthy parts of the intestine mixed in between inflamed areas. Ulcerative colitis, on the other hand, is continuous inflammation of the colon
- Ulcerative colitis only affects the inner most lining of the colon while Crohnâs disease can occur in all the layers of the bowel walls
Dont Miss: How To Heal Venous Ulcers
What Are The Risk Factors Of Ulcerative Colitis Vs Crohns Disease
In general, the risk factors for ulcerative colitis vs. Crohns disease are largely the same, save for one caveat. According to the Mayo Clinic, they include:
- Unintended weight loss
The severity of these symptoms varies widely, but none of them are exactly pleasant. The good thing about bloody diarrhea is that it can be alarming enough that it forces a trip to the doctor. And it should, says Dr. Balzora. Blood in the stool is never normal, she warns. That really should prompt a visit and discussion with your physician.
It might also help to open dialogue with your family, she says. Youll need to assess your medical history with your family. Thats a very taboo topic for certain cultures, but it can prompt earlier, more aggressive treatment that would otherwise be missed.
Also Check: How To Prevent Pressure Ulcers On Heels
What Are Surgical Treatments For Crohns Disease
As many as 7 in 10 people with Crohns disease eventually need surgery when medications no longer provide symptom relief. During a bowel resection, a surgeon:
- Removes the diseased bowel segment.
- Connects the two ends of the healthy bowel together .
After surgery, the remaining part of the bowel adapts and functions as it did before. Approximately 6 in 10 people who undergo surgery for Crohns disease will have a recurrence within 10 years. Another bowel resection may be a good option for you.
Types Of Ulcerative Colitis
Ulcerative colitis can be categorized into different types, depending on its location. The following types of ulcerative colitis include:
- Pancolitis: a type that affects the entire colon and causes bloody diarrhea, abdominal pain, fatigue, and significant weight loss.
- Ulcerative proctitis: a type that causes inflammation to the rectum which can result in rectal bleeding.
- Left-sided colitis: is a type that causes inflammation from the rectum, through the sigmoid and down to the colon. Common symptoms include pain and cramping on the left side, bloody diarrhea, and an urgency to have a bowel movement.
- Proctosigmoiditis: is a type that causes inflammation in the rectum and sigmoid colon. Bloody diarrhea, abdominal pain, and constipation are common signs of this type.
Don’t Miss: How Long Does Prednisone Take To Work For Ulcerative Colitis
Follow Up With Your Doctor
You may only need at-home or short-term care for some kinds of colitis. But UC is a condition youâll have for the rest of your life. And it affects everyone in a different way. Youâll need to work with your doctor to find a treatment plan that works for you.
No matter whatâs causing your symptoms, get medical care right away if you have:
- Watery diarrhea for more than a few days
- Heavy, ongoing diarrhea
Layers Of The Bowel Wall
The walls of your bowel have layers. The inner layers take in nutrients from food. The outer layers help move food through the gut and waste out of the body.
In Colitis, theres inflammation and swelling of the inner layer of the bowel wall. This can cause bleeding. More mucus may be produced by the inner layer of the bowel wall. Ulcers develop on the inner layer as the condition gets worse, but they can also go as the condition gets better.
The inflammation in Colitis affects how your body digests food, absorbs nutrients and gets rid of waste.
Everyone experiences Colitis differently. When youre having symptoms, its known as active disease, a flare-up or relapse. Symptoms may be mild or severe and are likely to change over time.
Your symptoms may vary depending on where Colitis is active in your bowel and how severe it is. Find out more in the section Types of Colitis.
The most common symptoms are:
Andy
Living with Colitis
Also Check: Managing Ulcerative Colitis Flare Ups
Are You Struggling With Crohns Disease Ulcerative Colitis Or Celiac Disease
Are you or a loved one struggling with an inflammatory bowel condition? If so, the good news is, youre not at the mercy of your diagnosis. While we may not be able to cure these conditions, you have so much power over your own health. I cant overemphasize the importance and influence your diet, supplements, and lifestyle factors can have on your inflammation levels and symptoms.
So if youre ready to take your power and health back from one of these inflammatory bowel conditions, I recommend starting with the steps outlined in this article and seeking out the guidance of an experienced Integrative and Functional Medicine Practitioner. Theyll help you identify the root cause of your condition and come up with a personalized plan of action to begin healing.
And if youre hungry for more practical and research-backed tips on optimizing your health, you can head over to my blog and catch up on hundreds of articles that simplify healthy living.
What Are The Main Types Of Ibd
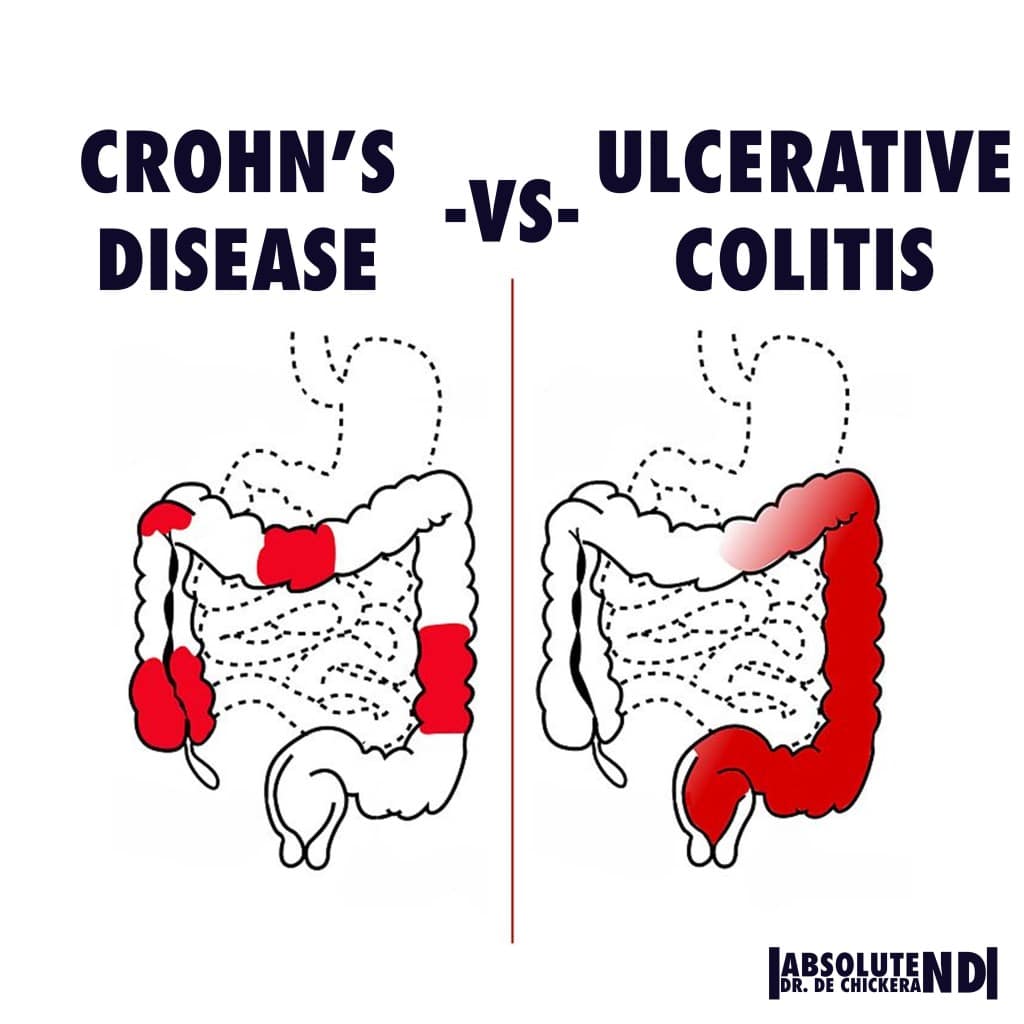
| Crohns Disease | Ulcerative Colitis | |
|---|---|---|
| Affected Location | Can affect any part of the GI tract Most often it affects the portion of the small intestine before the large intestine/colon. | Occurs in the large intestine and the rectum. |
| Damaged Areas | Damaged areas appear in patches that are next to areas of healthy tissue. | Damaged areas are continuous usually starting at the rectum and spreading further into the colon. |
| Inflammation | Inflammation may reach through the multiple layers of the walls of the GI tract. | Inflammation is present only in the innermost layer of the lining of the colon. |
Don’t Miss: Best Cranberry Juice For Ulcers
Key Differences: The Symptoms
While the two diseases are similar, there are also a few notable differences that set them apart including some of their symptoms and where the inflammation develops. Only a health professional will be able to determine which type of IBD you have, so its important to explain all your symptoms to your doctor or GI specialist.
While their symptoms may seem similar on the surface, Everyday Health points out that ulcerative colitis is mostly characterized by blood stool with mucus and frequent diarrhea, whereas Crohns disease is often marked by nausea, weight loss, and vomiting, with only occasional rectal bleeding, and diarrhea. Crohns can also cause mouth sores, or inflammation of the skin, joints, and eyes which are not symptoms of ulcerative colitis.
Ulcerative Colitis And Crohns Disease
Inflammatory bowel disease includes a number of conditions in which the immune system mistakenly attacks the intestines and triggers inflammation of the tissues. There are two main kinds of IBD: ulcerative colitis and Crohns disease. Today many medications are available to successfully treat IBD. These therapies work to calm inflammation, reduce and even alleviate symptoms, decrease flare-ups, and help you better cope with your condition. This report provides insight into the possible causes and complications of IBD, how you are diagnosed, and the steps you can take for better care so you can live your best life.
Recommended Reading: Ulcers In The Legs Or Feet
Diagnosis Criteria & Disease Severity Assessment
To assess disease activity and severity of UC, we used Mayo disease activity score, which is a combined endoscopic and clinical score .
The Crohns Disease Activity Index was used to assess disease severity in patients with CD consisting of 8 factors of patients symptoms during previous seven days and clinical data that are adjusted with a weighting factor and then summed. The score ranges from 0 to 600 .
The disease was considered clinically active if the CDAI score was higher than 150 and Mayo Score was higher than 3 . All patients with UC had active disease, while only 86.7% of patients with CD had Active disease.
You May Like: Is Nausea A Symptom Of Ulcer
What To Eat On A Crohns Diet During Remission:
What you should eat on a crohns diet plan is very individual but lets get acquainted with what it takes to be on a Crohns diet plan when your disease is not active:
-
Eat a variety of vegetables and fruits
-
Get enough calcium
-
Drink plenty of fluids
Your Crohns diet plan can even be more liberal when your symptoms subside but remember to:
-
Go slowly Gradually add more foods back into your diet. Shift to whole grains and those colorful veggies and fruits. Start with small amounts of these foods. If your symptoms act up, add that item to your potential list of trigger foods. You can try eating that food at a later time.
-
Eat 5 or 6 small meals per day Go easy on your GI tract. Large meals can flare your symptoms and make you feel bloated.
-
Stay well hydrated Sip on water throughout the day. As you add back in fiber, getting enough to drink is important. Fiber without adequate fluid intake can lead to constipation.
-
Avoid your trigger foods. Focus on the foods you can eat and enjoy. Create a list of substitutions for your trigger foods.
Recommended Reading: Ulcerative Colitis Remission Without Medication
Vitamin And Mineral Supplements For Ibd
A person with IBD who eats a healthy, varied diet does not usually need to take vitamin supplements. But if they have a dietary deficiency, they may need tablets or occasional vitamin B12 injections. For example, a person on a low-fibre diet may need extra vitamin C and folic acid because they dont eat enough fruit and vegetables.A person with Crohns disease who experiences steatorrhoea may need calcium and magnesium supplements. Most children with IBD should take supplements to help them grow and develop normally.
What Does Ulcerative Colitis Look Like
With UC there is a wide variation in the amount of inflammation from person to person, so that in mild cases the bowel can look almost normal but, when the inflammation is bad, the bowel can look very red and ulcerated. Ulcerative colitis usually affects the rectum, but occasionally there is no inflammation . Sometimes the inflammation is limited just to the rectum . However, the inflammation can involve varying lengths of the colon. When the whole large bowel is affected, this is called pan-colitis .
Also Check: Do Probiotics Help With Stomach Ulcers
You May Like: How Do You Cure Ulcerative Colitis
Rule Number 3 Eliminate Gluten And Dairy Generally
Gluten, or more specifically gliadin, stimulates zonulin production that in turn increases intestinal permeability, AKA Leaky Gut.
This increased gut permeability makes us more susceptible to an autoimmune response.
This post isnt meant to be a science lesson, but you can check this study out if you want to learn a little more about the process itself.
Noteworthily, several studies have also found that the casein protein in dairy behaves similarly to gluten / gliadin in our guts, and may also promote leaky gut.
This would explain why coeliacs often show cross-reactivity to many dairy products.
And to be very plain for a second, pretty much everyone whos been diagnosed with ulcerative colitis or Crohns disease has experienced gluten and/or casein being problematic at least on occasion.
^ That very basic fact is important.
Its important to add though, that not all dairy is created equal.
In fact, certain types of fermented dairy have actually been shown to improve serum zonulin levels and may help to improve leaky gut. See here.
And we could also muddy the water even more and say that other lectins and lectin-like proteins can also cause issues..
But, Im here to give you the broad brush strokes and attempt to simplify things.
So to keep it basic
Stay away from dairy and gluten and youll be off to a good start.
Recommended Reading: Signs You Have A Stomach Ulcer
Diagnosis And Assessment Of Disease Activity
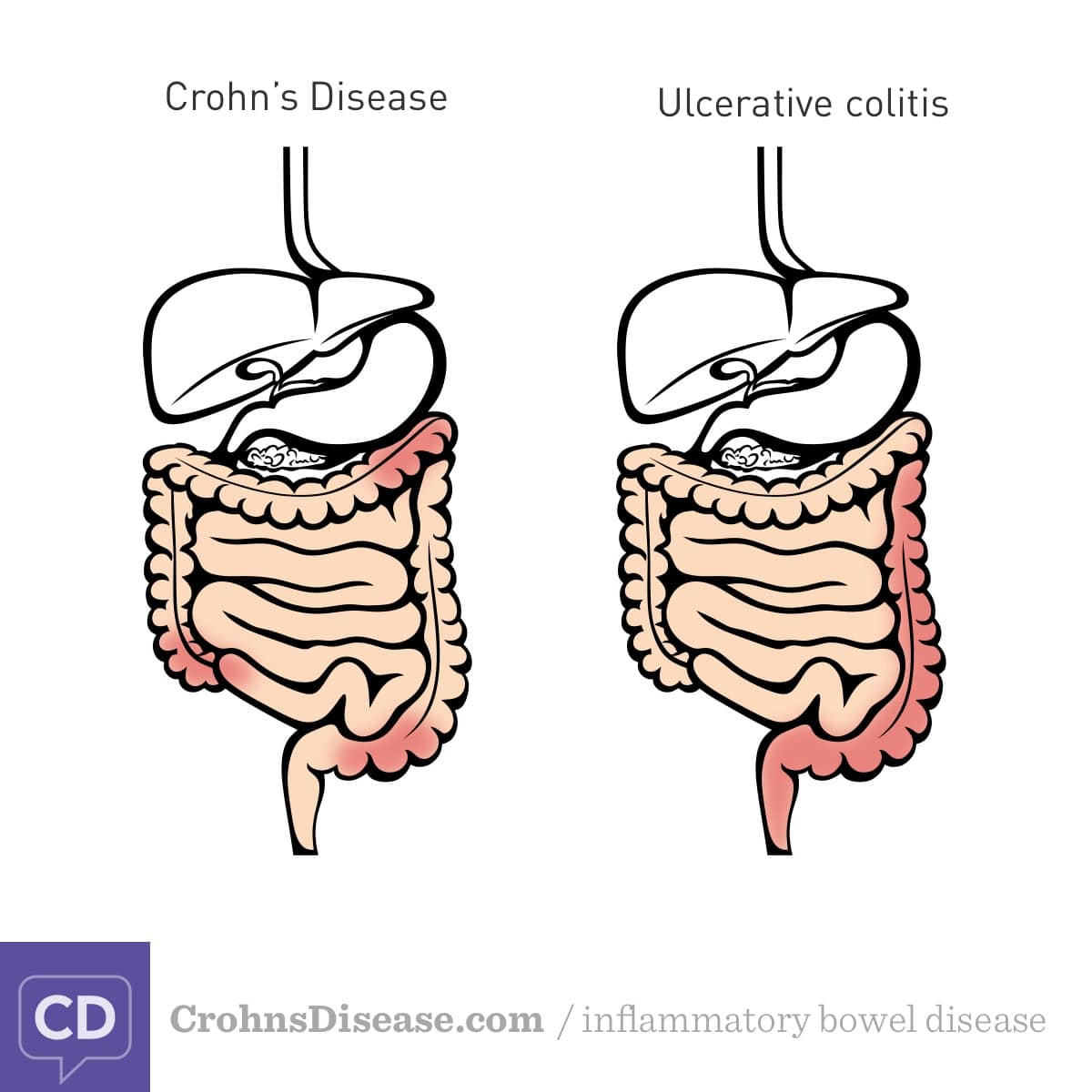
The diagnoses of Crohns disease and ulcerative colitis are made on clinical grounds supplemented with objective findings of radiological, endoscopic, and histological examination. In some cases, the diagnostic evaluation must be repeated after a certain period of time has passed. There is no gold standard for diagnosis . When establishing the diagnosis, one must exclude other inflammatory, toxic, vascular, neoplastic, and infectious etiologies of enteritis and/or colitis .
Don’t Miss: Ulcers On Legs From Diabetes
Daily Life For People With Ibd
People with IBD lead useful and productive lives, even though they need to take medications. When they are not experiencing a flare-up of their disease, they feel quite well and are often free of symptoms.People with IBD can marry, enjoy sexual activity and have children. They can hold down jobs, care for families and enjoy sport and recreational activities.Even though there is currently no cure for IBD, medical therapy has improved the health and quality of life of most people with Crohns disease and ulcerative colitis. Research underway today may lead to further improvements in medical and surgical treatment, and even a cure.